Abstract
Background
The laparoscopic magnified visual effects and evolution of the laparoscopic camera system have recently enabled us to observe details in the deep pelvic floor. Indications of laparoscopic surgery for colorectal cancer have been expanded, and laparoscopic (Lap) lateral pelvic node dissection (LLND) has been introduced in some institutions. We investigated the feasibility of Lap LLND in patients with locally advanced rectal cancer (LARC).
Methods
Lap LLND was performed in 38 patients diagnosed with cT3-4 or cN1-2 cancer during 2014–2018. We retrospectively analyzed their surgical and short-term outcomes.
Results
Laparoscopic surgery was performed in all patients. cStages II/III/IV were found in 6/31/1 patients, respectively. Among them, 25 patients underwent neoadjuvant chemotherapy without radiotherapy. Lap unilateral LLND was performed in 6 patients and Lap bilateral LLND was performed 32 patients. The number of harvested lymph nodes (LNs) were 4 in the unilateral group and 15 in the bilateral group. Operation time was 531 min, and blood loss was 105 ml. Oral intake has started on postoperative day (POD) 3, and pelvic drain was removed on POD 7. Hospital stay was 18.5 days. Seven patients developed a neurogenic bladder (all Clavien–Dindo grade (CD) II and all occured in the bilateral LLND group), one patient developed abdominal bleeding (CD IIIb) and one patient developed anastomotic leakage (CD IIIb). Pathological results revealed 2/5/16/14/1 patients with pStages 0/I/II/III/IV, respectively. Four patients had histopathologically verified lateral pelvic lymph node metastases. There were no local recurrences after curative surgery (median follow-up 24.2 months).
Conclusion
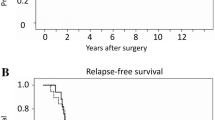
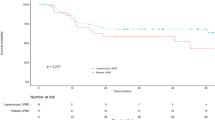
Although the median follow-up period is relatively short and further follow-up is necessary, oncologically, especially in the point of local control rate, Lap LLND appears to have acceptable in the treatment of LARC without radiotherapy in experienced centers. Further investigations focusing on indications and the Lap LLND procedural technique are required.


Similar content being viewed by others
References
National Cancer Center Japan (2018) Projected Cancer Statistics. Research Center for Cancer Control and Information Services, Cancer Information Service. https://ganjoho.jp/en/index.html. Accessed 20 April 2019
Bosset JF, Collette L, Calais G, Mineur L, Maingon P, Radosevic-Jelic L, Daban A, Bardet E, Beny A, Ollier JC (2006) Chemotherapy with preoperative radiotherapy in rectal cancer. N Engl J Med 355:1114–1123
Sauer R, Becker H, Hohenberger W, Rödel C, Wittekind C, Fietkau R, Martus P, Tschmelitsch J, Hager E, Hess CF, Karstens JH, Liersch T, Schmidberger H, Raab R (2004) Preoperative versus postoperative chemoradiotherapy for rectal cancer. N Engl J Med. 351:1731–1740
Fleming FJ, Påhlman L, Monson JR (2011) Neoadjuvant therapy in rectal cancer. Dis Colon Rectum 54:901–912
National Comprehensive Cancer Network, Inc. (US). https://www.nccn.org/patients/guidelines/rectal/42/. Accessed 20 April 2019
Fujita S, Mizusawa J, Kanemitsu Y, Ito M, Kinugasa Y, Komori K, Ohue M, Ota M, Akazai Y, Shiozawa M, Yamaguchi T, Bandou H, Katsumata K, Murata K, Akagi Y, Takiguchi N, Saida Y, Nakamura K, Fukuda H, Akasu T, Moriya Y (2017) Mesorectal excision with or without lateral lymph node dissection for clinical stage II/III lower rectal cancer (JCOG0212): a multicenter, randomized controlled, noninferiority trial. Ann Surg 266:201–207
Fleshman J, Sargent DJ, Green E, Anvari M, Stryker SJ, Beart RW Jr, Hellinger M, Flanagan R Jr, Peters W, Nelson H (2007) Laparoscopic colectomy for cancer is not inferior to open surgery based on 5-year data from the COST Study Group trial. Ann Surg 246:655–664
Buunen M, Veldkamp R, Hop WC, Kuhry E, Jeekel J, Haglind E, Påhlman L, Cuesta MA, Msika S, Morino M, Lacy A, Bonjer HJ (2009) Survival after laparoscopic surgery versus open surgery for colon cancer: long-term outcome of a randomized clinical trial. Lancet Oncol 10:44–52
Jayne DG, Thorpe HC, Copeland J, Quirke P, Brown JM, Guillou PJ (2010) Five-year follow-up of the Medical Research Council CLASICC trial of laparoscopically assisted versus open surgery for colorectal cancer. Br J Surg 97:1638–1645
Kim MJ, Oh JH (2018) Lateral lymph node dissection with the focus on indications, functional outcomes, and minimally invasive surgery. Ann Coloproctol 34:229–233
Konishi T, Kuroyanagi H, Oya M, Ueno M, Fujimoto Y, Akiyoshi T, Yoshimatsu H, Watanabe T, Yamaguchi T, Muto T (2011) Multio-media article. Lateral lymph node dissection with preoperative chemoradiation for locally advanced lower rectal cancer through a laparoscopic approach. Surg Endosc 25:2358–2359
Park JS, Choi GS, Lim KH, Jang YS, Kim HJ, Park SY, Jun SH (2011) Laparoscopic extended lateral pelvic node dissection following total mesorectal excision for advanced rectal cancer: initial clinical experience. Surg Endosc 25:3322–3329
Liang JT (2011) Technical feasibility of laparoscopic lateral pelvic lymph node dissection for patients with low rectal cancer after concurrent chemoradiation therapy. Ann Surg Oncol 18:153–159
Furuhata T, Okita K, Nishidate T, Ito T, Yamaguchi H, Ueki T, Akizuki E, Meguro M, Ogawa T, Kukita K, Kimura Y, Mizuguchi T, Hirata K (2015) Clinical feasibility of laparoscopic lateral pelvic lymph node dissection following total mesorectal excision for advanced rectal cancer. Surg Today 45:310–314
Sugihara K, Ajioka Y, Ishiguro S, Isomoto H, Iwashita A, Iwama T (2018) Japanese classification of colorectal, appendiceal, and anal carcinoma, 9th edn. Japanese Society for Cancer of the Colon and Rectum, Kanehara Shuppan, Tokyo
Tokuhara K, Ueyama Y, Nakatani K, Yoshioka K, Kon M (2016) Outcomes of neoadjuvant chemoradiotherapy in Japanese locally advanced rectal carcinoma patients. World J Surg Oncol 14:136
Hashiguchi Y, Muro K, Saito Y, Ito Y, Ajioka Y, Ishiguro M (2019) Japanese Society for Cancer of Colon and Rectum Guidelines 2019 for the Treatment of Colorectal Cancer. Japanese Society for Cancer of Colon and Rectum. Kanehara Shuppan, Tokyo
Akasu T, Sugihara K, Moriya Y (2009) Male urinary and sexual functions after mesorectal excision alone or in combination with extended lateral pelvic lymph node dissection for rectal cancer. Ann Surg Oncol 16:2779–2786
Deng Y, Chi P, Lan P, Wang L, Chen W, Cui L, Chen D, Cao J, Wei H, Peng X, Huang Z, Cai G, Zhao R, Huang Z, Xu L, Zhou H, Wei Y, Zhang H, Zheng J, Huang Y, Zhou Z, Cai Y, Kang L, Huang M, Peng J, Ren D, Wang J (2016) Modified FOLFOX6 with or without radiation versus fluorouracil and leucovorin with radiation in neoadjuvant treatment of locally advanced rectal cancer: initial results of the Chinese FOWARC multicenter, open-label, randomized three-arm phase III trial. J Clin Oncol 34:3300–3307
ClinicalTrials.gov. PROSPECT: chemotherapy alone or chemotherapy plus radiation therapy in treating patients with locally advanced rectal cancer undergoing surgery. https://clinicaltrials.gov/ct2/show/NCT01515787/. Accessed 30 April 2019
Funding
There was no funding source for this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Katsuji Tokuhara, Hidehiko Hishikawa, Terufumi Yoshida, Yosuke Ueyama, Kazuhiko Yoshioka, and Mitsugu Sekimoto have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tokuhara, K., Hishikawa, H., Yoshida, T. et al. Short-term outcomes of laparoscopic lateral pelvic node dissection for advanced lower rectal cancer. Surg Endosc 35, 1572–1578 (2021). https://doi.org/10.1007/s00464-020-07534-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07534-3