Abstract
Background
Postoperative intraabdominal abscess (IAA) is the most feared complication after laparoscopic appendectomy (LA). We aimed to evaluate the management of this complication in a large cohort of patients undergoing LA in order to design a treatment algorithm.
Methods
We included a consecutive series of patients undergoing LA for acute appendicitis from January 2008 to December 2018. The cohort of patients with postoperative IAA was divided into three groups based on the implemented treatments: G1: antibiotics only, G2: CT-guided drainage, and G3: laparoscopic lavage. Characteristics of the fluid collections and outcomes were analyzed in the three groups.
Results
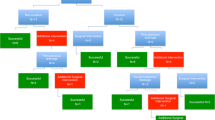
A total of 1668 LA were performed; the rate of IAA was 2.2% (36 patients). There were 12 (33%) patients who received antibiotics only (G1), 8 (22%) underwent CT-guided percutaneous drainage (G2), and 16 (45%) underwent laparoscopic lavage (G3). The median size of the abscesses was 2.7 (1.2–4) cm in G1, 6.2 (4.5–8) cm in G2, and 9.6 (8–11.4) cm in G3 (p < 0.04). Patients with two or more fluid collections underwent a laparoscopic lavage in all cases. Treatment failure occurred in 16% (2/12), 12.5% (1/8) and 12.5% (2/16) of the patients in G1, G2, and G3, respectively. None of the patients in the entire cohort required open surgery to resolve the postoperative IAA.
Conclusions
A minimally invasive step-up approach based on the size and number of fluid collections is associated with excellent outcomes. A treatment algorithm for post-appendectomy IAA is proposed.

Similar content being viewed by others
References
Weiss AJ, Elixhauser A, Andrews RM (2006) Characteristics of operating room procedures in U.S. Hospitals, 2011: statistical brief #170. Agency for healthcare research and quality. https://www.hcup-us.ahrq.gov/reports/statbriefs/sb170-Operating-Room-Procedures-United-States-2011.jsp. Accessed 22 May 2019.
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Semm K (1983) Endoscopic appendectomy. Endoscopy 15:59–64
Masoomi H, Nguyen NT, Dolich MO et al (2014) Laparoscopic appendectomy trends and outcomes in the united states: data from the nationwide inpatient sample (NIS), 2004–2011. Am Surg 80:1074–1077
Schlottmann F, Sadava EE, Peña ME et al (2017) Laparoscopic appendectomy: risk factors for postoperative intraabdominal abscess. World J Surg 41(5):1254–1258
Reid RI, Dobbs BR, Frizelle FA (1999) Risk factors for post-appendicectomy intra-abdominal abscess. Aust N Z J Surg 69:373–374
Dhaou MB, Ghorbel S, Chouikh T et al (2010) Conservative management of post-appendicectomy intra-abdominal abscesses. Ital J Pediatr 2010(36):68
Alvarado A et al (1986) A practical score for the early diagnosis of acute appendicitis. Ann Emerg Med 15(5):557–564
Clara L et al (2018) Infecciones intraabdominales. puesta al día y recomendaciones de la sociedad argentina de infectología. Medicina (Buenos Aires) 78:417–426
Masoomi H, Nguyen NT, Dolich MO et al (2011) Comparison of laparoscopic versus open appendectomy for acute nonperforated and perforated appendicitis in the obese population. Am J Surg 202:733–739
Athanasiou C, Lockwood S, Markides GA (2017) Systematic review and meta-analysis of laparoscopic versus open appendicectomy in adults with complicated appendicitis: an update of the literature. World J Surg 41(12):3083–3099
Feld R, Eschelman DJ, Sagerman JE et al (1994) Treatment of pelvic abscesses and other fluid collections: efficacy of transvaginal sonographically guided aspiration and drainage. AJR Am J Roentgenol 163:1141–1145
Pereira JK, Chait PG, Miller SF (1996) Deep pelvic abscesses in children: transrectal drainage under radiologic guidance. Radiology 198:393–396
Okoye BO, Rampersad B, Marantos A (1998) Abscess after appendectomy in children: the role of conservative management. Br J Surg 85:1111–1113
Blot S, De Waele JJ, Vogelaers D (2012) Essentials for selecting antimicrobial therapy for intra-abdominal infections. Drugs 72:17–32
Forgues D, Habbig S, Diallo AF et al (2007) Post-appendectomy intra-abdominal abscesses—can they successfully be managed with the sole use of antibiotic therapy? Eur J Pediatr Surg 17(2):104–109
Dobremez E, Lavrand F, Lefevre Y et al (2003) Treatment of post-appendectomy intra-abdominal deep abscesses. Eur J Pediatr Surg 13:393
Betsch A, Wiskirchen J, Trübenbach J et al (2002) CT-guided percutaneous drainage of intra-abdominal abscesses: APACHE III score stratification of 1-year results. Acute physiology, age, chronic health evaluation. Eur Radiol 12:2883–2889
Gronvall J, Gronvall S, Hegedüs V (1977) Ultrasound-guided drainage of fluid-containing masses using angiographic catheterization techniques. Am J Roentgenol 129:997–1002
Gervais DA, Brown SD, Connolly SA et al (2004) Percutaneous imaging guided abdominal and pelvic abscess drainage in children. Radiographics 24:737–754
Gregersen R, Mortensen LQ, Burcharth J, Pommergaard H-C, Rosenberg J (2016) Treatment of patients with acute colonic diverticulitis complicated by abscess formation: a systematic review. Int J Surg 35:201–208
Jaffe TA, Nelson RC, DeLong DM, Paulson EK (2004) Practice patterns in percutaneous image-guided intraabdominal abscess drainage: survey of academic and private practice centers. Radiology 233(3):750–756
Durmishi Y, Gervaz P, Brandt D et al (2006) Results from percutaneous drainage of Hinchey stage II diverticulitis guided by computed tomography scan. Surg Endosc 20:1129–1133
Clark JJ, Johnson SM (2011) Laparoscopic drainage of intraabdominal abscess after appendectomy: an alternative to laparotomy in cases not amenable to percutaneous drainage. J Pediatr Surg 46:1385–1389
Kok K, Yapp S (2000) Laparoscopic drainage of postoperative complicated intra-abdominal abscess. Surg Lap Endo Perc Tech 10:311–313
Gorter RR, Eker HH, Gorter-Stam MAW et al (2016) Diagnosis and management of acute appendicitis. EAES consensus development conference 2015. Surg Endosc 30:4668–4690
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Francisco Laxague MD, Francisco Schlottmann MD, MPH, José M. Piatti MD and Emmanuel E. Sadava MD, have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Laxague, F., Schlottmann, F., Piatti, J.M. et al. Minimally invasive step-up approach for the management of postoperative intraabdominal abscess after laparoscopic appendectomy. Surg Endosc 35, 787–791 (2021). https://doi.org/10.1007/s00464-020-07448-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07448-0