Abstract
Background
The aim of the present study was to explore incidence and severity of parastomal hernia (PSH) formation during the first 2 years after open/laparoscopic abdominoperineal resection (APR).
Methods
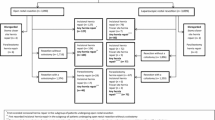
This was a retrospective cohort study conducted in a single institution. All patients who underwent laparoscopic/open APR for low rectal cancer within a 10-year study period were assessed for study eligibility.
Results
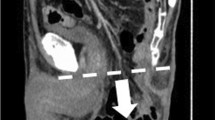
In total, 148 patients were included in the study (97 patients after laparoscopic APR; 51 patients after open APR). There were no statistically significant differences between study subgroups regarding demographic and clinical features. The incidence of PSH detected by physical examination was significantly higher in patients after laparoscopic APR 1 year after the surgery (50.5% vs. 19.6%, p < 0.001) and 2 years after the surgery (57.7% vs. 29.4%, p = 0.001). The incidence of radiologically detected PSH was significantly higher in laparoscopically operated patients after 1 year (58.7% vs. 35.3%, p = 0.007) and after 2 years (61.8% vs. 37.2%, p = 0.004). The mean diameter of PSH was similar in both study subgroups. The incidence of incisional hernia was significantly higher in patients who underwent open APR after 1 year (25.5% vs. 7.2%, p = 0.002) and after 2 years (31.3% vs. 7.2%, p < 0.001).
Conclusions
The risk of PSH development after laparoscopic APR appears to be significantly higher in comparison with patients undergoing open APR. Higher incidence of PSH should be considered a potential disadvantage of minimally invasive approach to patients with low rectal cancer.
Similar content being viewed by others
References
Londono-Schimmer EE, Leaong AP, Phillips RK (1994) Life table analysis of stomal complications following colostomy. Dis Colon Rectum 37(9):916–920
Gillern S, Bleier JI (2014) Parastomal hernia repair and reinforcement: the role of biologic and synthetic materials. Clin Colon Rectal Surg 27:162–171
Hansson BME, Morales-Conde S, Mussack T, Valdes J, Muysoms FE, Bleichrodt RP (2013) The laparoscopic modified Sugarbaker technique is safe and has a low recurrence rate: a multicenter cohort study. Surg Endosc 27:494–500
Carne PW, Robertson GM, Frizelle FA (2003) Parastomal hernia. Br J Surg 90(7):784–793
O’Neill CH, Borrazzo EC, Hyman NH (2015) Parastomal hernia repair. J Gastrointest Surg 19:766–769
Cheung MT, Chia NH, Chiu WY (2001) Surgical treatment of parastomal hernia complicating sigmoid colostomies. Dis Colon Rectum 44:266–271
Ripoche J, Basurko C, Fabbro-Perray P, Prudhomme M (2011) Parastomal hernia. A study of the French federation of ostomy patients. J Visc Surg 148:e435–e441
Asif A, Ruiz M. Yetasook A, Denham W, Linn J, Carbray J, Ujiki MB (2012) Laparoscopic modified Sugerbaker technique results in superior recurrence rate. Surg Endosc 26:3430–3434
Kald A, Juul KN, Hjortsvang H, Sjodahl RI (2008) Quality of life is impaired in patients with peristomal bulging of a sigmoid colostomy. Scand J Gastroenterol 43:627–633
Ihnát P, Guňková P, Peteja M, Vávra P, Pelikán A, Zonča P (2016) Diverting ileostomy in laparoscopic rectal cancer surgery: high price of protection. Surg Endosc 30(11):4809–4816
Funahashi K, Suzuki R, Nagashima Y, Matsuda S, Koike J, Shiokawa H, Ushigome M, Arai K, Kaneko T, Kurihara A, Kaneko H (2014) Risk factors for parastomal hernia in Japanese patients with permanent colostomy. Surg Today 44:1465–1469
Vennix S, Pelzers L, Bouvy N, Beets GL, Pierie JP, Wiggers T, Breukink S (2014) Laparoscopic versus open total mesorectal excision for rectal cancer. Cochrane Database Syst Rev 4:CD005200
Tan WJ, Chew MH, Dharmawan AR, Singh M, Acharyya S, Loi CT, Tanq CL (2016) Critical appraisal of laparoscopic vs open rectal cancer surgery. World J Gastrointest Surg 8(6):452
Ng SS, Lee JF, Yiu RY, Li JC, Hon SS, Mak TW, Leung WW, Leunq KL (2014) Long-term oncologic outcomes of laparoscopic versus open surgery for rectal cancer: a pooled analysis of 3 randomized controlled trials. Ann Surg 259(1):139–147
Agha A, Benseler V, Hornung M, Gerken M, Iesalnieks I, Fürst A, Anthuber M, Jauch KW, Schlitt HJ (2014) Long-term oncologic outcome after laparoscopic surgery for rectal cancer. Surg Endosc 28(4):1119–1125
Ihnát P, Martínek L, Mitták M, Vávra P, Ihnát Rudinská L, Zonča P (2014) Quality of life after laparoscopic and open resection of colorectal cancer. Dig Surg 31(3):161–168
Randall J, Lord B, Fulham J, Soin B (2012) Parastomal hernias as the predominant stoma complication after laparoscopic colorectal surgery. Surg Laparosc Endosc Percutan Tech 22(5):420–423
Carne PW, Frye JN, Robertson GM, Frizelle FA (2003) Parastomal hernia following minimally invasive stoma formation. ANZ J Surg 73(10):843–845
Heald RJ, Husband EM, Ryall RD (1982) The mesorectum in rectal cancer surgery—the clue to pelvic recurrence? Br J Surg 69:613–616
Moreno-Matias J, Serra-Aracil X, Darnell-Martin A, Bombardo-Junca J, Mora-Lopez L, Alcantara-Moral M, Rebasa P, Ayguavives-Garnica I, Navarro-Soto S (2009) The prevalence of parastomal hernia after formation of an end colostomy. A new clinico-radiological classification. Colorectal Dis 11:173–177
Hotouras A, Murphy J, Thaha M, Chan CL (2013) The persistent challenge of parastomal herniation: a review of the literature and future developments. Colorectal Dis 15(5):e202–e214
Malik T, Lee MJ, Harikrishnan AB (2018) The incidence of soma related morbidity—a systematic review of randomised controlled trials. Ann R Coll Surg Engl 100(7):501–508. https://doi.org/10.1308/rcsann.2018.0126 [Epub ahead of print]
Petersson J, Koedam TW, Bonjer HJ, Andersson J, Angenete E, Bock D, Cuesta MA, Deijen CL, Furst A, Lacz AM, Rosenberg J, Haglind E, COlorectal cancer Laparoscopic or Open Resection (COLOR) II Study Group (2018) Bowel obstruction and ventral hernia after laparoscopic versus open surgery for rectal cancer in a randomized trial (COLOR II). Ann Surg. https://doi.org/10.1097/SLA.0000000000002790 [Epub ahead of print]
Aguina CT, Iannuzzi JC, Probst CP, Kelly KN, Noyes K, Fleming FJ, Monson JRT (2014) Parastomal hernia: a growing problem with new solutions. Dig Surg 31:366–376
Ihnát P, Ihnát Rudinská L, Zonča P (2014) Radiofrequency energy in surgery: state of the art. Surg Today 44(6):985–991
Hansson BM, Slater NJ, van der Velden AS, Groenewoud HM, Buyne OR, de Hingh IH, Bleichrodt RP (2012) Surgical techniques for parastomal hernia repair: a systematic review of the literature. Ann Surg 255:685–695
Slater NJ, hansson BME, Buyne OR, Hendriks T, Bleichrodt RP (2011) Repair of parastomal hernias with biological grafts: a systematic review of the literature. J Gastrointest Surg 15:1252–1258
Hansson BME (2013) Parastomal hernia: treatment and prevention 2013; where do we go from here? Colorectal Dis 15:1467–1470
Cingi A, Carik T, Sever A, Aktan AO (2006) Enterostomy site hernias: a clinical and computerized tomographic evaluation. Dis Colon Rectum 49:1559–1563
Janson AR, Janes A, Israelsson LA (2010) Laparoscopic stoma formation with a prophylactic prosthetic mesh. Hernia 14:495–498
Jones HG, Rees M, Aboumarzouk OM, Brown J, Cragg J, Billings P, Carter B, Chandran P (2018) Prosthetic mesh placement for the prevention of parastomal herniation. Cochrane Database Syst Rev 7:CD008905
Findlay JM, Wood CPJ, Cunninham C (2018) Prophylactic mesh reinforcement of stomas: a cost-effectiveness meta-analysis of randomised controlled trials. Tech Coloproctol. https://doi.org/10.1007/s10151-018-1774-5 [Epub ahead of print]
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Peter Ihnát, Lubomír Tulinský, Tomáš Jonszta, Pavel Koscielnik, Lucia Ihnát Rudinská, and Igor Penka have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Ihnát, P., Tulinský, L., Jonszta, T. et al. Parastomal and incisional hernia following laparoscopic/open abdominoperineal resection: is there a real difference?. Surg Endosc 33, 1789–1794 (2019). https://doi.org/10.1007/s00464-018-6453-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-6453-0