Abstract
Introduction
Approximately 80 % of patients with pancreatic cancer are not candidates for curative resection at the time of diagnosis. The objective of this study is to show that although endoscopic treatment is the standard palliation, surgical laparoscopic treatment is both feasible and effective for these patients.
Materials and methods
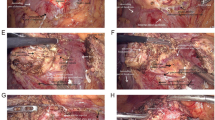
Preoperative resectability was evaluated by dynamic contrast-enhanced computed tomography scans. Endoscopic palliation was the first choice for patients with metastatic disease and for patients with locally advanced pancreatic cancer with bad performance status. Laparoscopic surgical palliation was indicated for patients with jaundice and locally advanced pancreatic cancer (elective palliation) and for patients with jaundice with metastatic disease and failure in the endoscopic/percutaneous treatment (necessary palliation). Elective palliation consisted of Roux-en-Y hepaticojejunostomy and gastrojejunostomy and necessary palliation consisted of laparoscopic hepaticojejunostomy alone.
Results
A total of 48 patients received laparoscopic surgical palliation. Morbidity rate was 33.3 % and mortality was 2.08 %. There was no need for late surgeries in any of the patients.
Conclusion
Surgical laparoscopic palliation is a feasible treatment option for locally advanced pancreatic cancer. Even though metallic stents are still the best palliation method for patients with systemic disease, if stents fail, the laparoscopic approach is a viable treatment.




Similar content being viewed by others
References
Siegel R, Naishadham D, Jemal A (2013) Cancer statistics, 2013. CA Cancer J Clin 63(1):11–30
Hidalgo M (2010) Pancreatic Cancer. N Engl J Med 362:1605–1617
Lloyd S, Chang BW (2013) A comparison of three treatment strategies for locally advanced and borderline resectable pancreatic cancer. J Gastrointest Oncol 4(2):123–130
Lillemoe K, Cameron J, Hardacre J et al (1999) Is prophylactic gastrojejunostomy indicated for unresectable periampullary cancer? A prospective randomized trial. Ann Surg 230(3):322–328; discussion 328–30
Elwir S, Sharzehi K, Veith J et al (2013) Biliary stenting in patients with malignant biliary obstruction: comparison of double layer, plastic and metal stents. Dig Dis Sci 58:2088–2092
Scott E, Garcea G, Doucas H et al (2009) Surgical bypass vs. endoscopic stenting for pancreatic ductal adenocarcinoma. HPB 11:118–124
Kneuertz P, Cunningham S, Cameron J et al (2012) Palliative surgical management of patients with unresectable pancreatic adenocarcinoma: trends and lessons learned from a large, single institution experience. J Gastrointest Surg 15(11):1917–1927
Buchs N, Addeo P, Bianco F et al (2011) Robotic palliation for unresectable pancreatic cancer and distal cholangiocarcinoma. Int J Med Robotics Comput Assist Surg 7:60–65
Conroy T, Mitry E (2011) Chimiothérapie de l´adénocarcinome du pancréas métastatique: défis et espoirs (chemotherapy of metastatic pancreatic adenocarcinoma: challenges and encouraging results). Bull Cancer 98(12):1439–1446
Chauffert B et al (2008) Phase III trial comparing intensive induction chemoradiotherapy (60 Gy, infusional 5-FU and intermittent cisplatin) followed by maintenance gemcitabine with gemcitabine alone for locally advanced unresectable pancreatic cancer. Definitive results of the 2000–01 FFCD/SFRO study. Ann Oncol 19(9):1592–1599
Disclosures
This is an observational study. There are no possible conflicts of interest declared. Authors Gustavo Kohan, Carlos G. Ocampo, Hugo I. Zandalazini, Roberto Klappenbach, Federico Yazyi, Ornella Ditulio, Carlos Canullán, Juan Alvarez Rodriguez, and Adelina Coturel declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kohan, G., Ocampo, C.G., Zandalazini, H.I. et al. Laparoscopic hepaticojejunostomy and gastrojejunostomy for palliative treatment of pancreatic head cancer in 48 patients. Surg Endosc 29, 1970–1975 (2015). https://doi.org/10.1007/s00464-014-3894-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3894-y