Abstract
Background
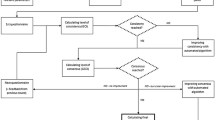
Virtual reality (VR) simulators have been demonstrated to improve basic psychomotor skills in endoscopic surgery. The exercise configuration settings used for validation in studies published so far are default settings or are based on the personal choice of the tutors. The purpose of this study was to establish consensus on exercise configurations and on a validated training program for a virtual reality simulator, based on the experience of international experts to set criterion levels to construct a proficiency-based training program.
Methods
A consensus meeting was held with eight European teams, all extensively experienced in using the VR simulator. Construct validity of the training program was tested by 20 experts and 60 novices. The data were analyzed by using the t test for equality of means.
Results
Consensus was achieved on training designs, exercise configuration, and examination. Almost all exercises (7/8) showed construct validity. In total, 50 of 94 parameters (53%) showed significant difference.
Conclusions
A European, multicenter, validated, training program was constructed according to the general consensus of a large international team with extended experience in virtual reality simulation. Therefore, a proficiency-based training program can be offered to training centers that use this simulator for training in basic psychomotor skills in endoscopic surgery.
Similar content being viewed by others
References
Aggarwal R, Ward J, Balasundaram I, Sains P, Athanasiou T, Darzi A (2007) Proving the effectiveness of virtual reality simulation for training in laparoscopic surgery. Ann Surg 5:771–779
Ahlberg G, Heikkinen T, Iselius L, Leijonmarck CE, Rutqvist J, Arvidsson D (2002) Does training in a virtual reality simulator improve surgical performance? Surg Endosc 1:126–129
Ahlberg G, Enochsson L, Gallagher AG, Hedman L, Hogman C, McClusky DA III, Ramel S, Smith CD, Arvidsson D (2007) Proficiency-based virtual reality training significantly reduces the error rate for residents during their first 10 laparoscopic cholecystectomies. Am J Surg 6:797–804
Grantcharov TP, Kristiansen VB, Bendix J, Bardram L, Rosenberg J, Funch-Jensen P (2004) Randomized clinical trial of virtual reality simulation for laparoscopic skills training. Br J Surg 2:146–150
Gurusamy K, Aggarwal R, Palanivelu L, Davidson BR (2008) Systematic review of randomized controlled trials on the effectiveness of virtual reality training for laparoscopic surgery. Br J Surg 9:1088–1097
Hyltander A, Liljegren E, Rhodin PH, Lonroth H (2002) The transfer of basic skills learned in a laparoscopic simulator to the operating room. Surg Endosc 9:1324–1328
Kundhal PS, Grantcharov TP (2009) Psychomotor performance measured in a virtual environment correlates with technical skills in the operating room. Surg Endosc 3:645–649
Larsen CR, Soerensen JL, Grantcharov TP, Dalsgaard T, Schouenborg L, Ottosen C, Schroeder TV, Ottesen BS (2009) Effect of virtual reality training on laparoscopic surgery: randomised controlled trial. BMJ 14:b1802
Schijven MP, Jakimowicz JJ, Broeders IA, Tseng LN (2005) The Eindhoven laparoscopic cholecystectomy training course-improving operating room performance using virtual reality training: results from the first E.A.E.S. accredited virtual reality trainings curriculum. Surg Endosc 9:1220–1226
Seymour NE, Gallagher AG, Roman SA, O’Brien MK, Bansal VK, Andersen DK, Satava RM (2002) Virtual reality training improves operating room performance: results of a randomized, double-blinded study. Ann Surg 4:458–463
Aggarwal R, Grantcharov TP, Eriksen JR, Blirup D, Kristiansen VB, Funch-Jensen P, Darzi A (2006) An evidence-based virtual reality training program for novice laparoscopic surgeons. Ann Surg 2:310–314
Duffy AJ, Hogle NJ, McCarthy H, Lew JI, Egan A, Christos P, Fowler DL (2005) Construct validity for the LAPSIM laparoscopic surgical simulator. Surg Endosc 3:401–405
Eriksen JR, Grantcharov T (2005) Objective assessment of laparoscopic skills using a virtual reality stimulator. Surg Endosc 9:1216–1219
Grantcharov TP, Bardram L, Funch-Jensen P, Rosenberg J (2003) Learning curves and impact of previous operative experience on performance on a virtual reality simulator to test laparoscopic surgical skills. Am J Surg 2:146–149
Sherman V, Feldman LS, Stanbridge D, Kazmi R, Fried GM (2005) Assessing the learning curve for the acquisition of laparoscopic skills on a virtual reality simulator. Surg Endosc 5:678–682
van Dongen KW, Tournoij E, van der Zee, Schijven MP, Broeders IA (2007) Construct validity of the LapSim: can the LapSim virtual reality simulator distinguish between novices and experts? Surg Endosc 21(8):1413–1417
Panait L, Bell RL, Roberts KE, Duffy AJ (2008) Designing and validating a customized virtual reality-based laparoscopic skills curriculum. J Surg Educ 6:413–417
Aggarwal R, Crochet P, Dias A, Misra A, Ziprin P, Darzi A (2009) Development of a virtual reality training curriculum for laparoscopic cholecystectomy. Br J Surg 9:1086–1093
Verdaasdonk EG, Dankelman J, Lange JF, Stassen LP (2008) Incorporation of proficiency criteria for basic laparoscopic skills training: how does it work? Surg Endosc 12:2609–2615
Verdaasdonk EG, Stassen LP, van Wijk RP, Dankelman J (2007) The influence of different training schedules on the learning of psychomotor skills for endoscopic surgery. Surg Endosc 2:214–219
Mackay S, Morgan P, Datta V, Chang A, Darzi A (2002) Practice distribution in procedural skills training: a randomized controlled trial. Surg Endosc 6:957–961
Munz Y, Almoudaris AM, Moorthy K, Dosis A, Liddle AD, Darzi AW (2007) Curriculum-based solo virtual reality training for laparoscopic intracorporeal knot tying: objective assessment of the transfer of skill from virtual reality to reality. Am J Surg 6:774–783
Schijven MP, Jakimowicz J (2004) The learning curve on the Xitact LS 500 laparoscopy simulator: profiles of performance. Surg Endosc 1:121–127
Aggarwal R, Grantcharov T, Moorthy K, Hance J, Darzi A (2006) A competency-based virtual reality training curriculum for the acquisition of laparoscopic psychomotor skill. Am J Surg 1:128–133
Acknowledgment
The authors thank R. Aggarwal of the Imperial College of London for sharing his knowledge and for his collaboration during the consensus meeting.
Disclosures
Drs. Koen van Dongen, Dr. Gunnar Ahlberg, Prof. Dr. Luigi Bonavina, Dr. Fiona Carter, Dr. Teodor Grantcharov, Dr. Marlies Schijven, Dr. Alessandro Stefani, Prof. Dr. David van der Zee, and Prof. Dr. Ivo Broeders have no conflicts of interest or financial ties to disclose. Dr. Anders Hyltander was founder and director of Surgical Science, Sweden, from 1999 until 2004. At this moment he is senior advisor to this company.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
van Dongen, K.W., Ahlberg, G., Bonavina, L. et al. European consensus on a competency-based virtual reality training program for basic endoscopic surgical psychomotor skills. Surg Endosc 25, 166–171 (2011). https://doi.org/10.1007/s00464-010-1151-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-010-1151-6