Abstract
Background
Because choledochoscopy often is a challenging maneuver, it would be advantageous to define the real utility of its use. This study aimed to compare blind exploration of the common bile duct (CBD) with choledochoscopy-assisted CBD stone removal in terms of patient outcome and complication rate.
Methods
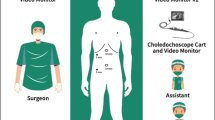
Two groups of patients were prospectively evaluated in a 4-year period. The study participants were 36 men and 27 women randomized to group A (n = 32) for a blind basket procedure or group B (n = 31) for a choledochoscopy-assisted procedure as the first step of laparoscopic CBD stone removal. Patients with preoperatively suspected CBD stones (n = 51) and those with unsuspected stones (n = 12) were included. The two groups did not differ significantly in terms of anagraphics, American Society of Anesthesiology (ASA) score, or previous surgery. All the procedures were performed by surgeons skilled in this surgical field. Choledochoscopy, when used, was always performed with the instrument connected to a camera monitor that had a wide vision, whether in a single-monitor, in a picture-in-picture manner, or with the use of an additional monitor.
Results
From March 2004 to April 2008, 63 patients undergoing CBD exploration for stone removal were enrolled in the study. Five of these patients had undergone previous endoscopic retrograde cholangiopancreatography (ERCP)/endoscopic sphincterotomy (ES). The mean operative time was 107 min for group A and 122 min for group B. The mean hospital stay was 3 days for group A and 3.6 days for group B. Clearance of CBD stones was achieved laparoscopically in 62 cases. One patient required open combined transduodenal papilloplasty and transcholedochotomy. In seven cases, blind basket exploration was unable to remove the stones according to the cholangiogram, so choledochoscopy was required. Six patients underwent a transversal coledocothomy for stone removal. A Kehr T-tube was placed in four of these patients. In four group A cases, the papilla was inadvertently passed during the procedure. In six group A cases, including the four aforementioned cases, a high level of amylases was found on postoperative day 1. At this writing, no late complications or stone recurrences have been observed in either group.
Conclusions
The laparoscopic basket blind technique and choledochoscopy are safe and effective for CBD stone removal. However, the latter seems to be better in terms of a higher stone removal rate and fewer minor complications despite its longer operation time. In the authors’ opinion, it may be preferable to reserve ERCP for very high-risk patients, taking into account that in addition to the related complications, it results in an approximate 10% rate of recurrent or persistent stones.



Similar content being viewed by others
References
Muhe E (1992) Long-term follow-up after laparoscopic cholecystectomy. Endoscopy 24(9):754–758
Pierce RA, Jonnalagadda S, Spitler JA, Tessier DJ, Liaw JM, Lall SC, Melman LM, Frisella MM, Todt LM, Brunt LM, Halpin VJ, Eagon JC, Edmundowicz SA, Matthews BD (2008) Incidence of residual choledocholithiasis detected by intraoperative cholangiography at the time of laparoscopic cholecystectomy in patients having undergone preoperative ERCP. Surg Endosc 22:2365–2372
Hekimoglu K, Ustundag Y, Dusak A, Erdem Z, Karademir B, Aydemir S, Gundogdu S (2008) MRCP vs. ERCP in the evaluation of biliary pathologies: review of current literature. J Dig Dis 9:162–169
Petelin J (1991) Laparoscopic approach to common bile duct pathology. Surg Laparosc Endosc 12:23–29
Paganini AM, Guerrieri M, Sarnari J, De Sanctis A, D’Amb G, Lezoche G, Perretta S, Lezoche E (2007) Thirteen years’ experience with laparoscopic transcystic common bile duct exploration for stone. Surg Endosc 21:34–40
Schreurs WH, Juttmann JR, Stuifbergen WN, Oostvogel HJ, van Vroonhoven TJ (2002) Management of common bile duct stones: selective retrograde cholangiography and endoscopic sphincterotomy: short- and long-term results. Surg Endosc 16:1068–1072
Campbell S, Mee A, Thompson MH (2004) Common bile duct calculi-ERCP versus laparoscopic exploration. Ann R Coll Surg Engl 86:470–473
Macadam RCA, Goodal RJR (2004) Long-term symptoms following endoscopic sphincterotomy for common bile duct stones. Surg Endosc 18:363–366
Waage A, Stromberg C, Leijonmarck CE, Arvidsson D (2003) Long-term results from laparoscopic common bile duct exploration. Surg Endosc 17:1181–1185
JCh Berthou, Dron B, Charbonneau P, Moussalier K, Pellissier L (2007) Evaluation of laparoscopic treatment of common bile duct stones in a prospective series of 505 patients: indications and results. Surg Endosc 21:1970–1974
Hamouda AH, Goh W, Mahmud S, Khan M, Nassar AH (2007) Intraoperative cholangiography facilitates simple transcystic clearance of ductal stones in units without expertise for laparoscopic bile duct surgery. Surg Endosc 21:955–959
Paganini AM, Guerrieri M, Sarnari J, De Sanctis A, D’Ambrosio G, Lezoche G, Lezoche E (2005) Long-term results after laparoscopic transverse choledochotomy for common bile duct stones. Surg Endosc 19:705–709
Lezoche E, Paganini AM (1995) Single-stage laparoscopic treatment of gallstones and common bile duct stones in 120 unselected consecutive patients. Surg Endosc 9:1070–1075
Yang MH, Chen TH, Wang SE, Tsai YF, Su CH, Wu CW, Lui WY, Shyr YM (2008) Biochemical predictors for absence of CBD stones in patients undergoing laparoscopic cholecystectomy. Surg Endosc 22:1620–1624
Tranter SE, Thompson MH (2002) Comparison of endoscopic sphincterotomy and laparoscopic exploration of the common bile duct. Br J Surg 89:1495–1504
Morino M, Baracchi F, Miglietta C, Ragona R, Garbarini A (2006) Preoperative endoscopic sphincterotomy versus laparoendoscopic rendezvous in patients with gallbladder and common bile duct stones. Ann Surg 244:889–896
Kharbutli B, Velanovich V (2008) Management of preoperative suspected choledocholithiasis: a decision analysis. J Gastrointest Surg 12:1973–1980
Phillips EH, Toouli J, Pitt HA, Soper NJ (2008) Treatment of common bile duct stones discovered during cholecystectomy. J Gastrointest Surg 12:624–628
Kullman E, Borch K, Lindström E, Svanvik J, Anderberg B (1996) Management of bile duct stones in the era of laparoscopic cholecystectomy: appraisal of routine operative cholangiography and endoscopic treatment. Eur J Surg 162:873–880
NIH state-of-the-science statement on endoscopic retrograde cholangiopancreatography (ERCP) for diagnosis and therapy (2002) NIH Consens State Sci Statements 19:1–26
Rhodes M, Sussman L, Cohen L, Lewis MP (1998) Randomised trial of laparoscopic exploration of the common bile duct versus postoperative endoscopic retrograde cholangiography for common bile duct stones. Lancet 351:159–161
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Campagnacci, R., Baldoni, A., Baldarelli, M. et al. Is laparoscopic fiberoptic choledochoscopy for common bile duct stones a fine option or a mandatory step?. Surg Endosc 24, 547–553 (2010). https://doi.org/10.1007/s00464-009-0599-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-009-0599-8