Abstract
Purpose
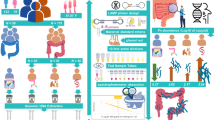
Neo-adjuvant radiotherapy (NART) is a widely used pre-surgery radiotherapy for rectal cancer patients. Although NART is effective in reducing tumor burden before surgery, it may cause dysbiosis of intestinal microbiota. The intestinal microbiota shapes tumor inflammatory environment and influences cancer progression. However, how NART remodels the microbiota and how the microbiota affects therapeutic efficacy has been largely elusive. This study aimed to reveal the details of how NART affects the intestinal microbiota in patients with rectal cancer.
Methods
Rectal cancer patients who received NART were recruited into the study, and their healthy family members on the same diet served as controls. Stool samples from five rectal cancer patients (28 in total) and five healthy individuals (16 in total) were collected for intestinal microbiota analysis by 16S rRNA gene amplicon sequencing. Samples from patients were divided into earlier- and later-NART according to the number of NART.
Results
NART did not significantly affect the α diversity of intestinal microbiota. However, the abundance of bacterial genera associated with cancer progression tended to decrease in later-NART patients. More importantly, a variety of oral pathogenic bacteria were enriched in the intestine of later-NART patients. NART also affected functional pathways associated with the microbiota in DNA repair, metabolism, and bacterial infection.
Conclusion
NART significantly altered the microbiota composition and function in rectal cancer patients, and some oral pathogens were found to translocate to the intestine. This is the first report to study the effect of NART on intestinal microbiota in patients with rectal cancer, exploring the importance of intestinal microbiota during the process of NART.





Similar content being viewed by others
Data availability
Contact the corresponding author for the raw sequencing reads.
References
Abdulamir AS, Hafidh RR, Abu BF (2011) The association of Streptococcus bovis/gallolyticus with colorectal tumors: the nature and the underlying mechanisms of its etiological role. J Exp Clin Cancer Res 30:11
Abed J, Maalouf N, Manson AL, Earl AM, Parhi L, Emgård JEM et al (2020) Colon cancer-associated Fusobacterium nucleatum may originate from the oral cavity and reach colon tumors via the circulatory system. Front Cell Infect Microbiol 10:400
Agnes A, Biondi A, Belia F, Di Giambenedetto S, Addolorato G, Antonelli M et al (2021) Association between colorectal cancer and Streptococcus gallolyticus subsp. pasteuranus (former S. bovis) endocarditis: clinical relevance and cues for microbiota science. Case report and review of the literature. Eur Rev Med Pharmacol Sci 25:480–486
Amoroso C, Perillo F, Strati F, Fantini MC, Caprioli F, Facciotti F (2020) The role of gut microbiota biomodulators on mucosal immunity and intestinal inflammation. Cells 9:1234
Apetoh L, Ghiringhelli F, Tesniere A, Obeid M, Ortiz C, Criollo A et al (2007) Toll-like receptor 4-dependent contribution of the immune system to anticancer chemotherapy and radiotherapy. Nat Med 13:1050–1059
Are A, Aronsson L, Wang S, Greicius G, Lee YK, Gustafsson JA et al (2008) Enterococcus faecalis from newborn babies regulate endogenous PPARgamma activity and IL-10 levels in colonic epithelial cells. Proc Natl Acad Sci USA 105:1943–1948
Arthur JC, Gharaibeh RZ, Mühlbauer M, Perez-Chanona E, Uronis JM, McCafferty J et al (2014) Microbial genomic analysis reveals the essential role of inflammation in bacteria-induced colorectal cancer. Nat Commun 5:4724
Asadollahi P, Ghanavati R, Rohani M, Razavi S, Esghaei M, Talebi M (2020) Anti-cancer effects of Bifidobacterium species in colon cancer cells and a mouse model of carcinogenesis. PLoS One 15:e0232930
Barker HE, Paget JT, Khan AA, Harrington KJ (2015) The tumour microenvironment after radiotherapy: mechanisms of resistance and recurrence. Nat Rev Cancer 15:409–425
Butt J, Romero-Hernández B, Pérez-Gómez B, Willhauck-Fleckenstein M, Holzinger D, Martin V et al (2016) Association of Streptococcus gallolyticus subspecies gallolyticus with colorectal cancer:serological evidence. Int J Cancer 138:1670–1679
Cedermark B, Dahlberg M, Glimelius B, Påhlman L, Rutqvist LE, Wilking N (1997) Improved survival with preoperative radiotherapy in resectable rectal cancer. N Engl J Med 336:980–987
Chalmers NI, Oh K, Hughes CV, Pradhan N, Kanasi E, Ehrlich Y et al (2015) Pulp and plaque microbiotas of children with severe early childhood caries. J Oral Microbiol 7:25951
Chen S, Zhou Y, Chen Y, Gu J (2018) Fastp: an ultra-fast all-in-one FASTQ preprocessor. Bioinformatics 34:i884–i890
Chen BD, Jia XM, Xu JY, Zhao LD, Ji JY, Wu BX et al (2021) An autoimmunogenic and proinflammatory profile defined by the gut microbiota of patients with untreated systemic lupus erythematosus. Arthritis Rheumatol 73:232–243
Cogdill AP, Gaudreau PO, Arora R, Gopalakrishnan V, Wargo JA (2018) The impact of intratumoral and gastrointestinal microbiota on systemic cancer therapy. Trends Immunol 39:900–920
de Almeida CV, Taddei A, Amedei A (2018) The controversial role of Enterococcus faecalis in colorectal cancer. Therap Adv Gastroenterol 11:1756284818783606
Demaria S, Coleman CN, Formenti SC (2016) Radiotherapy: changing the game in immunotherapy. Trends Cancer 2:286–294
Deng Q, Wang C, Yu K, Wang Y, Yang Q, Zhang J et al (2020) Streptococcus bovis contributes to the development of colorectal cancer via recruiting CD11b+TLR-4+ cells. Med Sci Monit 26:e921886
Dong J, Li Y, Xiao H, Zhang S, Wang B, Wang H et al (2021) Oral microbiota affects the efficacy and prognosis of radiotherapy for colorectal cancer in mouse models. Cell Rep 37:109886
Dove WF, Clipson L, Gould KA, Luongo C, Marshall DJ, Moser AR et al (1997) Intestinal neoplasia in the ApcMin mouse: independence from the microbial and natural killer (beige locus) status. Cancer Res 57:812–814
Downes J, Munson MA, Radford DR, Spratt DA, Wade WG (2002) Shuttleworthia satelles gen. nov., sp. nov., isolated from the human oral cavity. Int J Syst Evol Microbiol 52:1469–1475
Dzutsev A, Goldszmid RS, Viaud S, Zitvogel L, Trinchieri G (2015) The role of the microbiota in inflammation, carcinogenesis, and cancer therapy. Eur J Immunol 45:17–31
Edgar RC (2013) UPARSE: highly accurate OTU sequences from microbial amplicon reads. Nat Methods 10:996–998
Elinav E, Garrett WS, Trinchieri G, Wargo J (2019) The cancer microbiome. Nat Rev Cancer 19:371–376
Fahmy CA, Gamal-Eldeen AM, El-Hussieny EA, Raafat BM, Mehanna NS, Talaat RM et al (2019) Bifidobacterium longum suppresses murine colorectal cancer through the modulation of oncomiRs and tumor suppressor miRNAs. Nutr Cancer 71:688–700
Fung TC, Olson CA, Hsiao EY (2017) Interactions between the microbiota, immune and nervous systems in health and disease. Nat Neurosci 20:145–155
Hasan R, Bose S, Roy R, Paul D, Rawat S, Nilwe P et al (2022) Tumor tissue-specific bacterial biomarker panel for colorectal cancer: Bacteroides massiliensis, Alistipes species, Alistipes onderdonkii, Bifidobacterium pseudocatenulatum, Corynebacterium appendicis. Arch Microbiol 204:348
Herrera FG, Bourhis J, Coukos G (2017) Radiotherapy combination opportunities leveraging immunity for the next oncology practice. CA Cancer J Clin 67:65–85
Huo RX, Wang YJ, Hou SB, Wang W, Zhang CZ, Wan XH (2022) Gut mucosal microbiota profiles linked to colorectal cancer recurrence. World J Gastroenterol 28:1946–1964
Ida Y, Okuyama T, Araki K, Sekiguchi K, Watanabe T, Ohnishi H (2022) First description of Lachnoanaerobaculum orale as a possible cause of human bacteremia. Anaerobe 73:102506
Ivanov II, Tuganbaev T, Skelly AN, Honda K (2022) T cell responses to the microbiota. Annu Rev Immunol 40:559–587
Jaffray DA (2012) Image-guided radiotherapy: from current concept to future perspectives. Nat Rev Clin Oncol 9:688–699
Kharrat N, Assidi M, Abu-Elmagd M, Pushparaj PN, Alkhaldy A, Arfaoui L et al (2019) Data mining analysis of human gut microbiota links Fusobacterium spp. with colorectal cancer onset. Bioinformation 15:372–379
Komiya Y, Shimomura Y, Higurashi T, Sugi Y, Arimoto J, Umezawa S et al (2019) Patients with colorectal cancer have identical strains of Fusobacterium nucleatum in their colorectal cancer and oral cavity. Gut 68:1335–1337
Li Y, Dong J, Xiao H, Zhang S, Wang B, Cui M et al (2020) Gut commensal derived-valeric acid protects against radiation injuries. Gut Microbes 11:789–806
Lim YK, Park SN, Jo E, Shin JH, Chang YH, Shin Y et al (2019) Lachnoanaerobaculum gingivalis sp. nov., isolated from human subgingival dental plaque of a gingivitis lesion. Curr Microbiol 76:1147–1151
Liu YK, Chen V, He JZ, Zheng X, Xu X, Zhou XD (2021) A salivary microbiome-based auxiliary diagnostic model for type 2 diabetes mellitus. Arch Oral Biol 126:105118
Magoč T, Salzberg SL (2011) FLASH: fast length adjustment of short reads to improve genome assemblies. Bioinformatics 27:2957–2963
O’Keefe SJ (2016) Diet, microorganisms and their metabolites, and colon cancer. Nat Rev Gastroenterol Hepatol 13:691–706
Périchon B, Lichtl-Häfele J, Bergsten E, Delage V, Trieu-Cuot P, Sansonetti P et al (2022) Detection of Streptococcus gallolyticus and four other CRC-associated bacteria in patient stools reveals a potential “driver” role for enterotoxigenic Bacteroides fragilis. Front Cell Infect Microbiol 12:794391
Pons BJ, Vignard J, Mirey G (2019) Cytolethal distending toxin subunit b: a review of structure-function relationship. Toxins (Basel) 11:595
Rubinstein MR, Wang X, Liu W, Hao Y, Cai G, Han YW (2013) Fusobacterium nucleatum promotes colorectal carcinogenesis by modulating E-cadherin/β-catenin signaling via its FadA adhesin. Cell Host Microbe 14:195–206
Scanlan PD, Shanahan F, Clune Y, Collins JK, O’Sullivan GC, O’Riordan M et al (2008) Culture-independent analysis of the gut microbiota in colorectal cancer and polyposis. Environ Microbiol 10:789–798
Schloss PD, Westcott SL, Ryabin T, Hall JR, Hartmann M, Hollister EB et al (2009) Introducing mothur: open-source, platform-independent, community-supported software for describing and comparing microbial communities. Appl Environ Microbiol 75:7537–7541
Segata N, Izard J, Waldron L, Gevers D, Miropolsky L, Garrett WS et al (2011) Metagenomic biomarker discovery and explanation. Genome Biol 12:R60
Sheng Q, Du H, Cheng X, Cheng X, Tang Y, Pan L et al (2019) Characteristics of fecal gut microbiota in patients with colorectal cancer at different stages and different sites. Oncol Lett 18:4834–4844
Steck N, Hoffmann M, Sava IG, Kim SC, Hahne H, Tonkonogy SL et al (2011) Enterococcus faecalis metalloprotease compromises epithelial barrier and contributes to intestinal inflammation. Gastroenterology 141:959–971
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71:209–249
Taghinezhad SS, Mohseni AH, Fu X (2021) Intervention on gut microbiota may change the strategy for management of colorectal cancer. J Gastroenterol Hepatol 36:1508–1517
Thomas AM, Jesus EC, Lopes A, Aguiar S, Begnami MD, Rocha RM et al (2016) Tissue-associated bacterial alterations in rectal carcinoma patients revealed by 16S rRNA community profiling. Front Cell Infect Microbiol 6:179
Viaud S, Saccheri F, Mignot G, Yamazaki T, Daillère R, Hannani D et al (2013) The intestinal microbiota modulates the anticancer immune effects of cyclophosphamide. Science 342:971–976
Wang Q, Garrity GM, Tiedje JM, Cole JR (2007) Naive Bayesian classifier for rapid assignment of rRNA sequences into the new bacterial taxonomy. Appl Environ Microbiol 73:5261–5267
Wang S, Hibberd ML, Pettersson S, Lee YK (2014) Enterococcus faecalis from healthy infants modulates inflammation through MAPK signaling pathways. PLoS One 9:e97523
Wang Q, Wang K, Wu W, Lv L, Bian X, Yang L et al (2020) Administration of Bifidobacterium bifidum CGMCC 15068 modulates gut microbiota and metabolome in azoxymethane (AOM)/dextran sulphate sodium (DSS)-induced colitis-associated colon cancer (CAC) in mice. Appl Microbiol Biotechnol 104:5915–5928
Wong SH, Zhao L, Zhang X, Nakatsu G, Han J, Xu W et al (2017) Gavage of fecal samples from patients with colorectal cancer promotes intestinal carcinogenesis in germ-free and conventional mice. Gastroenterology 153:1621-1633.e1626
Xu S, Yin W, Zhang Y, Lv Q, Yang Y, He J (2020) Foes or friends? bacteria enriched in the tumor microenvironment of colorectal cancer. Cancers (Basel) 12:372
Zhang H, Chang Y, Zheng Q, Zhang R, Hu C, Jia W (2019a) Altered intestinal microbiota associated with colorectal cancer. Front Med 13:461–470
Zhang S, Wang Q, Zhou C, Chen K, Chang H, Xiao W et al (2019b) Colorectal cancer, radiotherapy and gut microbiota. Chin J Cancer Res 31:212–222
Zhao Z, Wang H, Zhang D, Guan Y, Siddiqui SA, Feng-Shan X et al (2022) Oral vaccination with recombinant Lactobacillus casei expressing Aeromonas hydrophila Aha1 against A. hydrophila infections in common carps. Virulence 13:794–807
Zhiqin W, Palaniappan S, Raja Ali RA (2014) Inflammatory bowel disease-related colorectal cancer in the Asia-Pacific region: past, present, and future. Intest Res 12:194–204
Zorron Cheng Tao PuL, Yamamoto K, Honda T, Nakamura M, Yamamura T, Hattori S et al (2020) Microbiota profile is different for early and invasive colorectal cancer and is consistent throughout the colon. J Gastroenterol Hepatol 35:433–437
Acknowledgements
This research was funded by the Health Commission of Hubei Province (WJ2021M193), the Biomedical Center of Hubei Cancer Hospital (2022SWZX13), Natural Science Foundation of Hubei Province (2016CFB405), Health and Family Planning Commission of Hubei Province (WJ2017M144), and the Fundamental Research Funds for the Central Universities (2662017PY112).
Funding
This research was funded by the Health Commission of Hubei Province (WJ2021M193), the Biomedical Center of Hubei Cancer Hospital (2022SWZX13), Natural Science Foundation of Hubei Province (2016CFB405), Health and Family Planning Commission of Hubei Province (WJ2017M144), and the Fundamental Research Funds for the Central Universities (2662017PY112).
Author information
Authors and Affiliations
Contributions
SX: data curation; formal analysis; investigation; methodology; visualization; roles/writing—original draft. QL: data curation; formal analysis; investigation; methodology; resources; writing—review and editing. NZ: conceptualization; formal analysis; funding acquisition; resources; writing—review and editing. YZ: investigation; methodology; writing—review and editing. JZ: conceptualization; funding acquisition; project administration; resources; writing—review and editing. QT: conceptualization; data curation; formal analysis; project administration; writing—review and editing. S-HC: writing—review and editing. LL: funding acquisition; formal analysis; project administration; writing—review and editing. JH: conceptualization; formal analysis; funding acquisition; project administration; writing—review & editing. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Institutional review board statement
This is certify that the design and methods of the research are in accordance with the requirements of related regulations and procedures as well as the ethical principles, and approved by the Institutional Review Board of Hubei Cancer Hospital, project associated code LLHBCH2022YN-044.
Informed consent
Informed consent was obtained from all subjects involved in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xu, S., Lv, Q., Zou, N. et al. Influence of neo-adjuvant radiotherapy on the intestinal microbiota of rectal cancer patients. J Cancer Res Clin Oncol 149, 6085–6096 (2023). https://doi.org/10.1007/s00432-022-04553-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-022-04553-6