Abstract
Propose
Poly (ADP-ribose) polymerase 1 inhibitors were originally investigated as anti-cancer therapeutics with BRCA1/2 genes mutation. Here, we investigate the effectiveness of a novel PARP1 inhibitor fluzoparib, for enhancing the radiation sensitivity of NSCLC cells lacking BRCA1/2 mutation.
Methods
We used MTS assays, western blotting, colony formation assays, immunofluorescence staining, and flow cytometry to evaluate the radiosensitization of NSCLC cells to fluzoparib and explore the underlying mechanisms in vitro. Through BRCA1 and RAD50 genes knockdown, we established dysfunctional homologous recombination (HR) DNA repair pathway models in NSCLC cells. We next investigated the radiosensitization effect of fluzoparib in vivo using human NSCLC xenograft models in mice. The expression of PARP1 and BRCA1 in human NSCLC tumor samples was measured by immunohistochemistry. Furthermore, we sequenced HR-related gene mutations and analyzed their frequencies in advanced NSCLC.
Results
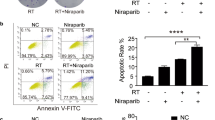
In vitro experiments in NSCLC cell lines along with in vivo experiments using an NSCLC xenograft mouse model demonstrated the radiosensitization effect of fluzoparib. The underlying mechanisms involved increased apoptosis, cell-cycle arrest, enhanced irradiation-induced DNA damage, and delayed DNA-damage repair. Immunohistochemical staining showed no correlation between the expression of PARP1 and BRCA1. Moreover, our sequencing results revealed high mutation frequencies for the BRCA1/2, CHEK2, ATR, and RAD50 genes.
Conclusion
The potential therapeutic value of fluzoparib for increasing the radiation sensitivity of NSCLC is well confirmed. Moreover, our findings of high mutation frequencies among HR genes suggest that PARP1 inhibition may be an effective treatment strategy for advanced non-small cell lung cancer patients.








Similar content being viewed by others
References
BRCA2 mutation linked to lung cancer risk (2014) Cancer Discov 4:OF1 https://doi.org/10.1158/2159-8290.cd-nb2014-096
Bryant HE et al (2009) PARP is activated at stalled forks to mediate Mre11-dependent replication restart and recombination. EMBO J 28:2601–2615. https://doi.org/10.1038/emboj.2009.206
Chen J, Peng H, He J, Huan X, Miao Z, Yang C (2014) Synthesis of isoquinolinone-based tricycles as novel poly(ADP-ribose) polymerase-1 (PARP-1) inhibitors. Bioorg Med Chem Lett 24:2669–2673. https://doi.org/10.1016/j.bmcl.2014.04.061
Chevanne M et al (2010) Inhibition of PARP activity by PJ-34 leads to growth impairment and cell death associated with aberrant mitotic pattern and nucleolar actin accumulation in M14 melanoma cell line. J Cell Physiol 222:401–410. https://doi.org/10.1002/jcp.21964
Coleman RL et al (2017) Rucaparib maintenance treatment for recurrent ovarian carcinoma after response to platinum therapy (ARIEL3): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet 390:1949–1961. https://doi.org/10.1016/s0140-6736(17)32440-6
Cseh AM et al (2019) PARP Inhibitor PJ34 Protects mitochondria and induces DNA-damage mediated apoptosis in combination with cisplatin or temozolomide in B16F10 melanoma. Cells Front Physiol 10:538. https://doi.org/10.3389/fphys.2019.00538
Engert F, Kovac M, Baumhoer D, Nathrath M, Fulda S (2017) Osteosarcoma cells with genetic signatures of BRCAness are susceptible to the PARP inhibitor talazoparib alone or in combination with chemotherapeutics. Oncotarget 8:48794–48806. https://doi.org/10.18632/oncotarget.10720
Ferlay J, Parkin DM, Steliarova-Foucher E (2010) Estimates of cancer incidence and mortality in Europe in 2008. Eur J Cancer 46:765–781. https://doi.org/10.1016/j.ejca.2009.12.014
Fong PC et al (2009) Inhibition of poly(ADP-ribose) polymerase in tumors from BRCA mutation carriers. N Engl J Med 361:123–134. https://doi.org/10.1056/nejmoa0900212
Hastak K, Bhutra S, Parry R, Ford JM (2017) Poly (ADP-ribose) polymerase inhibitor, an effective radiosensitizer in lung and pancreatic cancers. Oncotarget 8:26344–26355. https://doi.org/10.18632/oncotarget.15464
Hirai T, Saito S, Fujimori H, Matsushita K, Nishio T, Okayasu R, Masutani M (2016) Radiosensitization by PARP inhibition to proton beam irradiation in cancer cells. Biochem Biophys Res Commun 478:234–240. https://doi.org/10.1016/j.bbrc.2016.07.062
Hjortkjaer M, Waldstrom M, Jakobsen A, Kanstrup H, Sogaard-Andersen E, Dahl Steffensen K (2017) The prognostic value of BRCA1 and PARP expression in epithelial ovarian carcinoma: immunohistochemical detection. Int J Gynecol Pathol 36:180–189. https://doi.org/10.1097/pgp.0000000000000310
Horton JK, Wilson SH (2013) Predicting enhanced cell killing through PARP inhibition. Mol Cancer Res 11:13–18. https://doi.org/10.1158/1541-7786.MCR-12-0512
Hu C et al (2018a) Association between inherited germline mutations in cancer predisposition genes and risk of pancreatic cancer. JAMA 319:2401–2409. https://doi.org/10.1001/jama.2018.6228
Hu Y et al (2018b) False-positive plasma genotyping due to clonal hematopoiesis. Clin Cancer Res 24:4437–4443. https://doi.org/10.1158/1078-0432.CCR-18-0143
Inbar-Rozensal D, Castiel A, Visochek L, Castel D, Dantzer F, Izraeli S, Cohen-Armon M (2009) A selective eradication of human nonhereditary breast cancer cells by phenanthridine-derived polyADP-ribose polymerase inhibitors. Breast Cancer Res 11:R78. https://doi.org/10.1186/bcr2445
Jiang Y et al (2016) Hypoxia potentiates the radiation-sensitizing effect of olaparib in human non-small cell lung cancer xenografts by contextual synthetic lethality. Int J Radiat Oncol Biol Phys 95:772–781. https://doi.org/10.1016/j.ijrobp.2016.01.035
Karanam NK, Srinivasan K, Ding L, Sishc B, Saha D, Story MD (2017) Tumor-treating fields elicit a conditional vulnerability to ionizing radiation via the downregulation of BRCA1 signaling and reduced DNA double-strand break repair capacity in non-small cell lung cancer cell lines. Cell Death Dis 8:e2711. https://doi.org/10.1038/cddis.2017.136
Kim G et al (2015) FDA approval summary: olaparib monotherapy in patients with deleterious germline BRCA-mutated advanced ovarian cancer treated with three or more lines of chemotherapy. Clin Cancer Res 21:4257–4261. https://doi.org/10.1158/1078-0432.CCR-15-0887
Klein C et al (2017) Overcoming hypoxia-induced tumor radioresistance in non-small cell lung cancer by targeting DNA-dependent protein kinase in combination with carbon ion irradiation. Radiat Oncol 12:208. https://doi.org/10.1186/s13014-017-0939-0
Kocher S et al (2019) A functional ex vivo assay to detect PARP1-EJ repair and radiosensitization by PARP-inhibitor in prostate cancer. Int J Cancer 144:1685–1696. https://doi.org/10.1002/ijc.32018
Koeppel F et al (2017) Whole exome sequencing for determination of tumor mutation load in liquid biopsy from advanced cancer patients. PLoS One 12:e0188174. https://doi.org/10.1371/journal.pone.0188174
Lawrence TS (1988) Ouabain sensitizes tumor cells but not normal cells to radiation. Int J Radiat Oncol Biol Phys 15:953–958
Li L et al (2017) Androgen receptor inhibitor-induced “BRCAness” and PARP inhibition are synthetically lethal for castration-resistant prostate cancer. Sci Signal. https://doi.org/10.1126/scisignal.aam7479
Liu L et al (2014) TGFbeta induces “BRCAness” and sensitivity to PARP inhibition in breast cancer by regulating DNA-repair genes. Mol Cancer Res 12:1597–1609. https://doi.org/10.1158/1541-7786.mcr-14-0201
Liu G et al (2015) Augmentation of response to chemotherapy by microRNA-506 through regulation of RAD51 in serous ovarian cancers. J Natl Cancer Inst. https://doi.org/10.1093/jnci/djv108
Lord CJ, McDonald S, Swift S, Turner NC, Ashworth A (2008) A high-throughput RNA interference screen for DNA repair determinants of PARP inhibitor sensitivity. DNA Repair (Amst) 7:2010–2019. https://doi.org/10.1016/j.dnarep.2008.08.014
M IJ et al (2018) Enhancement of radiation effectiveness in cervical cancer cells by combining ionizing radiation with hyperthermia and molecular targeting agents. Int J Mol Sci. https://doi.org/10.3390/ijms19082420
Madison DL, Stauffer D, Lundblad JR (2011) The PARP inhibitor PJ34 causes a PARP1-independent, p21 dependent mitotic arrest. DNA Repair (Amst) 10:1003–1013. https://doi.org/10.1016/j.dnarep.2011.07.006
Mangoni M et al (2018) Enhancement of soft tissue sarcoma cell radiosensitivity by poly(ADP-ribose) polymerase-1 inhibitors. Radiat Res 190:464–472. https://doi.org/10.1667/rr15035.1
Martinez P, Martinez-Marti A, Navarro A, Cedres S, Felip E (2014) Molecular targeted therapy for early-stage non-small-cell lung cancer: will it increase the cure rate? Lung Cancer 84:97–100. https://doi.org/10.1016/j.lungcan.2014.01.018
Mateo J et al (2015) DNA-repair defects and olaparib in metastatic prostate cancer. N Engl J Med 373:1697–1708. https://doi.org/10.1056/NEJMoa1506859
Mirza MR et al (2016) Niraparib maintenance therapy in platinum-sensitive, recurrent ovarian cancer. N Engl J Med 375:2154–2164. https://doi.org/10.1056/NEJMoa1611310
Oei AL et al (2017a) Enhancing synthetic lethality of PARP-inhibitor and cisplatin in BRCA-proficient tumour cells with hyperthermia. Oncotarget 8:28116–28124. https://doi.org/10.18632/oncotarget.15922
Oei AL, Vriend LEM, Krawczyk PM, Horsman MR, Franken NAP, Crezee J (2017b) Targeting therapy-resistant cancer stem cells by hyperthermia. Int J Hyperthermia 33:419–427. https://doi.org/10.1080/02656736.2017.1279757
Pant S, Maitra A, Yap TA (2019) PARP inhibition—opportunities in pancreatic cancer. Nat Rev Clin Oncol. https://doi.org/10.1038/s41571-019-0257-6
Park ES et al (2017) Cardioprotective effect of KR-33889, a novel PARP inhibitor, against oxidative stress-induced apoptosis in H9c2 cells and isolated rat hearts. Arch Pharm Res 40:640–654. https://doi.org/10.1007/s12272-017-0912-3
Podszywalow-Bartnicka P et al (2014) Downregulation of BRCA1 protein in BCR-ABL1 leukemia cells depends on stress-triggered TIAR-mediated suppression of translation. Cell Cycle 13:3727–3741. https://doi.org/10.4161/15384101.2014.965013
Rouleau M, Patel A, Hendzel MJ, Kaufmann SH, Poirier GG (2010) PARP inhibition: PARP1 and beyond. Nat Rev Cancer 10:293–301. https://doi.org/10.1038/nrc2812
Schoonen PM et al (2017) Progression through mitosis promotes PARP inhibitor-induced cytotoxicity in homologous recombination-deficient cancer cells. Nat Commun 8:15981. https://doi.org/10.1038/ncomms15981
Shen J et al (2019) PARPi triggers the STING-dependent immune response and enhances the therapeutic efficacy of immune checkpoint blockade independent of BRCAness. Cancer Res 79:311–319. https://doi.org/10.1158/0008-5472.CAN-18-1003
Sonnenblick A, de Azambuja E, Azim HA Jr, Piccart M (2015) An update on PARP inhibitors–moving to the adjuvant setting. Nat Rev Clin Oncol 12:27–41. https://doi.org/10.1038/nrclinonc.2014.163
Sulkowski PL et al (2017) 2-Hydroxyglutarate produced by neomorphic IDH mutations suppresses homologous recombination and induces PARP inhibitor sensitivity. Sci Transl Med. https://doi.org/10.1126/scitranslmed.aal2463
Tyldesley S, Boyd C, Schulze K, Walker H, Mackillop WJ (2001) Estimating the need for radiotherapy for lung cancer: an evidence-based, epidemiologic approach. Int J Radiat Oncol Biol Phys 49:973–985
Wang YQ, Wang PY, Wang YT, Yang GF, Zhang A, Miao ZH (2016) An update on poly(ADP-ribose)polymerase-1 (PARP-1) inhibitors: opportunities and challenges in cancer therapy. J Med Chem 59:9575–9598. https://doi.org/10.1021/acs.jmedchem.6b00055
Wang L et al (2019) Pharmacologic characterization of fluzoparib, a novel poly(ADP-ribose) polymerase inhibitor undergoing clinical trials. Cancer Sci 110:1064–1075. https://doi.org/10.1111/cas.13947
Waqar SN et al (2014) BRCAness in non-small cell lung cancer (NSCLC). J Clin Oncol 32:11033. https://doi.org/10.1200/jco.2014.32.15_suppl.11033
Wu M et al (2018) Olaparib nanoparticles potentiated radiosensitization effects on lung cancer. Int J Nanomedicine 13:8461–8472. https://doi.org/10.2147/IJN.S181546
Yi JM, Huan XJ, Song SS, Zhou H, Wang YQ, Miao ZH (2016) Triptolide induces cell killing in multidrug-resistant tumor cells via CDK7/RPB1 rather than XPB or p44. Mol Cancer Ther 15:1495–1503. https://doi.org/10.1158/1535-7163.mct-15-0753
Ying S, Hamdy FC, Helleday T (2012) Mre11-dependent degradation of stalled DNA replication forks is prevented by BRCA2 and PARP1. Cancer Res 72:2814–2821. https://doi.org/10.1158/0008-5472.can-11-3417
Zhang K, Zhang M, Zhu J, Hong W (2016a) Screening of gene mutations associated with bone metastasis in nonsmall cell lung cancer. J Cancer Res Ther 12:C186–C190. https://doi.org/10.4103/0973-1482.200597
Zhang M, Liu G, Xue F, Edwards R, Sood AK, Zhang W, Yang D (2016b) Copy number deletion of RAD50 as predictive marker of BRCAness and PARP inhibitor response in BRCA wild type ovarian cancer. Gynecol Oncol 141:57–64. https://doi.org/10.1016/j.ygyno.2016.01.004
Acknowledgements
We wish to thank the timely help given by Dr. Qinghua Wang and Dr. Shuai Ma in data analysis and plotting.
Funding
This research was supported by a Grant from Tianjin Natural Science Foundation (16jcybjc25300).
Author information
Authors and Affiliations
Contributions
Conception and design: NBL, GGY, LJZ, and PW. Development of methodology: NBL, GGY, LJZ, and CYY. Acquisition of data (provided animals, acquired and managed patients, provided facilities, etc.): JL, HH, XCD, LMZ, JC, JFS, QW, YX, and SLX. Analysis and interpretation of data (e.g., statistical analysis, biostatistics, and computational analysis): JL, HH, XCD, and NBL. Writing, review, and/or revision of the manuscript: JL and NBL. Administrative, technical, or material support (i.e., reporting or organizing data, constructing databases): YX, SLX, and GGY. Study supervision: NBL and GGY.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (include name of committee + reference number) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Luo, J., Dai, X., Hu, H. et al. Fluzoparib increases radiation sensitivity of non-small cell lung cancer (NSCLC) cells without BRCA1/2 mutation, a novel PARP1 inhibitor undergoing clinical trials. J Cancer Res Clin Oncol 146, 721–737 (2020). https://doi.org/10.1007/s00432-019-03097-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-019-03097-6