Abstract
Oxygen sensing is of paramount importance for maintaining cellular and systemic homeostasis. In response to diminished oxygen levels, the hypoxia-inducible factors (HIFs) orchestrate various biological processes. These pivotal transcription factors have been identified as key regulators of several biological events. Notably, extensive research from our group and others has demonstrated that HIF1α exerts an inverse regulatory effect on steroidogenesis, leading to the suppression of crucial steroidogenic enzyme expression and a subsequent decrease in steroid levels. These steroid hormones occupy pivotal roles in governing a myriad of physiological processes. Substantial or prolonged fluctuations in steroid levels carry detrimental consequences across multiple organ systems and underlie various pathological conditions, including metabolic and immune disorders. MicroRNAs serve as potent mediators of multifaceted gene regulatory mechanisms, acting as influential epigenetic regulators that modulate a broad spectrum of gene expressions. Concomitantly, phosphodiesterases (PDEs) play a crucial role in governing signal transduction. PDEs meticulously manage intracellular levels of both cAMP and cGMP, along with their respective signaling pathways and downstream targets. Intriguingly, an intricate interplay seems to exist between hypoxia signaling, microRNAs, and PDEs in the regulation of steroidogenesis. This review highlights recent advances in our understanding of the role of microRNAs during hypoxia-driven processes, including steroidogenesis, as well as the possibilities that exist in the application of HIF prolyl hydroxylase (PHD) inhibitors for the modulation of steroidogenesis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Hypoxia pathway proteins
Oxygen plays a central role in the complex world of cellular survival, serving as an essential molecule for all cells and tissues in our body. Its importance extends far beyond respiration, as oxygen is not only a critical component in the generation of cellular energy, but also serves as a key cofactor and substrate for a wide range of enzymes. The lack of sufficient oxygen, a condition known as hypoxia, can have profound effects on cellular function. However, it is important to realize that the concept of hypoxia is far from absolute, as what constitutes normal oxygen levels varies widely between different tissues. At a molecular level, the cellular adaptation to hypoxia is governed by a remarkable set of transcription factors known as hypoxia-inducible factors (HIFs). These hypoxia pathway proteins, including HIF1α and HIF2α, oversee the orchestration of hundreds of genes involved in adaptation processes, the preservation of cell viability, and interconnection to an enormous variety of biological functions [72, 89, 95, 120].
The structural backbone of these functional HIF transcription factors is a heterodimer composed of two subunits: an oxygen-sensitive HIFα subunit and a constitutively expressed HIF1β subunit [7, 111]. Under conditions of ample oxygen, HIF prolyl hydroxylase domain proteins (PHD1-3), known as oxygen sensors, step into the scene, hydroxylating the HIFα subunit at two specific proline residues within its oxygen-dependent degradation domain [6, 32]. Subsequently, hydroxylated HIFs are recognized and bound by the von Hippel-Lindau tumor suppressor protein (VHL). VHL recruits components of the E3-ubiquitin ligase complex and facilitates the ubiquitination and proteasomal degradation of hydroxylated HIFs (see Fig. 1). These PHD enzymes belong to the 2-oxoglutarate-dependent oxygenase superfamily and rely on oxygen, iron, and ascorbate for their enzymatic activity. However, in the oxygen-starved realm of hypoxic cells, PHDs remain inactive, allowing HIF1α or HIF2α to accumulate within the cell. These accumulated HIFs then partner with the HIF1β subunit in the nucleus, forming the functional HIF heterodimer accompanied by its co-activators (e.g., p300 and CBP). This nuclear engagement culminates in the formation of a transcriptional complex, with the HIF transcription factor binding to hypoxia-responsive elements (HRE) within gene promoters, which exerts regulatory control over numerous cellular processes, including erythropoiesis, angiogenesis, metabolism, and cellular proliferation and differentiation (see Fig. 1) [96].
Hypoxia signaling pathway. Under normal oxygen levels (normoxia), hypoxia-inducible factor (HIF)-α subunits are hydroxylated by HIF prolyl hydroxylase domain proteins (PHDs). PHDs require oxygen (O2), ferrous iron (Fe2+), and 2-oxoglutarate (2-OG) for their activity. Hydroxylated HIFs are recognized and bound by the von Hippel-Lindau tumor suppressor protein (VHL). VHL recruits components of the E3-ubiquitin ligase complex and facilitates the ubiquitination and proteasomal degradation of hydroxylated HIFs. HIF is also regulated in a VHL-independent manner by the activity of factor inhibiting HIF1 (FIH), an asparaginyl hydroxylase. The conserved asparaginyl (Asn) residue within the C-terminal activation domain in HIFα is hydroxylated under normoxia or mild hypoxia, thereby suppressing HIF transcriptional activity by preventing interaction with the transcriptional coactivators p300/CBP. Conversely, under conditions of relatively low oxygen levels (hypoxia), PHD activity and the degradation of HIFα subunits as well as FIH activity are inhibited. Therefore, HIFα subunits are stabilized and are able to dimerize with the HIFβ subunit. In the nucleus, active HIFα/β dimer in complex with other cofactors promote the transcription of target genes with hypoxia response elements (HREs) such as transferrin (Tf), erythropoietin (Epo), numerous microRNAs, and other genes involved in metabolism, angiogenesis, erythropoiesis, steroidogenesis, and other hypoxia regulated processes
Another oxygen-dependent mechanism of HIF regulation involves factor inhibiting HIF1 (FIH1), an asparaginyl hydroxylase, which hydroxylates the HIFα subunit at the asparagine in the C-terminal activation domain under normoxia and mild hypoxia. Such hydroxylation prevents the activation of HIF as it inhibits interactions between HIF1α and its p300/CBP co-activators [19]. FIH1 also acts as a safety net because it is less sensitive to a reduction in oxygen pressure compared to PHDs and remains active even under mild hypoxia to block HIFα activation that has escaped PHD-mediated degradation [49].
MicroRNAs
MicroRNAs (miRNAs) are a class of endogenous, small, noncoding, single-stranded ribonucleic acids (RNAs) that are usually about 21–24 nucleotides in length and function in gene regulation. They repress the expression of their target genes post-transcriptionally and act as potent epigenetic regulators of a vast array of gene expressions [5]. Although still at its infancy state, microRNAs are implicated in myriads of biological processes as they underlie the regulation of processes such as metabolism, apoptosis, embryonic development, proliferation and differentiation, inflammation, and homeostasis amongst other physiological processes [105]. Furthermore, the aberrant expressions of miRNAs play critical roles in the pathogenesis of several diseases such as cancer, cardiovascular diseases, hepatitis, and many metabolic diseases. Amongst other types of noncoding RNAs (ncRNAs), miRNAs have emerged as key regulators of gene expression [2, 5, 26].
The biogenesis of miRNAs has been extensively described [81, 84, 129]. MiRNAs functionally regulate gene expression by base pairing partially or completely with complementary sites in their target messenger RNAs (mRNAs). The binding of miRNAs to their target mRNAs, usually in the 3′-untranslated region (3′UTR), triggers various mechanisms of miRNA gene regulation, such as alteration of mRNA stability, mRNA de-adenylation, translational repression, 5′-to-3′ mRNA degradation, and de-capping [5, 84]. MicroRNAs are dynamic in their regulatory activities. A single miRNA has the ability to bind to and regulate the expression of sometimes even hundreds of mRNAs. Similarly, multiple miRNA types can bind to a single mRNA target in the 3′UTR and regulate its expression in concert or individually. Computational studies have predicted that more than 50% of human protein–coding genes are regulated by miRNAs [5, 23, 129].
Several studies have described the important role of miRNAs, and deregulation of miRNAs has been implicated to underlie many different pathological conditions [98]. MiR-26a, miR-197, and miR-210 have been characterized as high-risk factors for patients with colorectal cancer (CRC), whereas miR-375 has served as a protective factor [125]. Vascular endothelial cells (VECs) highly express miR125a-5p and miR-125b-5p. Deregulation in the expression of these miRNAs may contribute to vascular dysfunction [64]. MiR-146a is thought to negatively regulate the innate immune response [90]. Diabetes patients with or without diabetic retinopathy (DR) can be differentiated based on the expression levels of miR-93 and miR-152. Both miRNAs showed good diagnostic performance for diabetes and DR [93]. MiR-10 acts as an endogenous inhibitor of the NLRP3 inflammasome. It is able to suppress the activation of NLRP3 (NOD-, LRR, and pyrin domain–containing protein 3) inflammasome and prevent inflammation in a diabetic kidney. In fact, miRNAs play a pivotal role in mediating the regulation of many physiological and pathophysiological processes [22].
Hypoxia-microRNA crosstalk
Hypoxia signaling influences miRNA expression and activity, and those that respond to hypoxia have been termed hypoxamiRs [28]. However, a bidirectional crosstalk has also been described in which microRNAs can target HIFs and thereby modulate their expression and signaling [10, 97]. Several miRNAs such as miR-6789-5p, miR-98-3p, miR-139-5p, miR-520d-3p and miR-4745-5p [75], miR-210-3p [41, 70, 75], miR-687 [8], miR-155 [10], miR363 [122], miR-19a [1], and miR-146a [101] have been identified as HIF-dependent miRNAs. Except for miR-6789-5p, which was a HIF1-specific miRNA, all of these miRNAs were also identified to be regulated by HIF2. Other HIF2-specific miRNAs have also been described: miR-7-5p, miR-503-5p, miR-503-3p, miR-424-3p, miR-495-3p, and miR-543 [75].
Many of these hypoxia-related miRNAs play critical roles in the regulation of various biological processes. MiR-210 has been widely described in the field of hypoxia signaling and is predominantly upregulated under hypoxic conditions [117]. It regulates mitochondrial function, proliferation, DNA repair, apoptosis, cell migration, and cell cycle [42]. Hypoxia-related miRNAs are of great prognostic value for identifying high-risk patients with various types of cancer, including colorectal cancer (CRC) [125]. Moreover, patients with pancreatic ductal adenocarcinoma (PDAC) have increased expression levels of total miR-30b-5p and peripheral blood plasma exosomal miR-30b-5p compared to healthy individuals. MiR-30b-5p is enriched in hypoxic pancreatic cancer cells and it directly targets and inhibits GJA1 expression in endothelial cells thereby facilitating angiogenesis [13].
Hypoxia can alter the expression levels of microRNAs depending on the cellular and physiological context. MiR-140-3p expression is induced under hypoxia, and its overexpression has been shown to enhance osteo/odontogenic differentiation of hypoxia-treated dental pulp stem cells (DPSCs) by negatively regulating lysine methyltransferase 5B (KMT5B) [131]. MiR-34a expression is induced under hypoxia. MiR-34a targets and represses the expression of Klotho in ARPE-19 cells [121]. PHDs, which target HIFs, may also be targeted by miRNAs. MiR-122, an HIF1-regulated miRNA, was identified to target and repress PHD1 upon hypoxia induction and facilitate liver protection by attenuating liver injury during liver transplantations [48]. Similarly, hypoxia-elevated miR-182-5p has been described to regulate contractile vascular smooth muscle cells (VSMCs). MiR-182-5p acts as a negative regulator of RhoA signaling in VSMCs by repressing RGS5 expression under hypoxia [113].
Hypoxia can also lead to miRNA downregulation. MiR-873-5p is significantly downregulated under hypoxic conditions [24]. HIF1α has been shown to directly bind the tumor suppressor miR-326 promoter and suppress its expression under hypoxic conditions. MiR-326 targets and suppresses ITGA5 levels thereby ameliorating resistance to chemotherapy in triple-negative breast cancer (TNBC) [4]. There is also a bidirectional crosstalk between HIFs and microRNAs. MiR-196b-5p has been reported to target high-mobility group AT-hook 2 (HMGA2) mRNA, thereby inhibiting angiogenic function. Simultaneously, miR-196b-5p is downregulated in endothelial cells as a result of HIF1α regulation. However, by targeting HMGA2, miR-196b-5p may also reduce the expression levels of HIF1α [86]. The tumor suppressor protein P53 inhibits tumor angiogenesis by inducing microRNA-107 expression in human colon cancer cells. MiR-107 targets HIF1β in these cells, reducing its expression and hypoxia signaling [123].Treatment of metastatic clear cell renal cell carcinoma (m-ccRCC)-bearing patients with EGFR tyrosine kinase inhibitors (VEGFR TKIs) as first-line therapy has identified three miRNAs (miR-3529-3p, miR-185-5p, and miR-223-3p) that target HIF-2α and are associated with reduced expression and tumor reduction [51]. These studies represent a growing catalog of possible interactions between HIFs and microRNAs. Such a catalog can be used as part of the effort to establish specific HIF inhibitor regimens. Further investigation of the biological and therapeutic relevance of these associations is warranted.
MicroRNAs regulate steroidogenesis
Steroid hormones play a critical role in many physiological events [38]. Steroids are essential for immune cell function, cell metabolism, reproduction, salt and water balance, pregnancy, and the body’s response to stress signals. The biochemistry of steroid synthesis has been described in detail [5, 12]. Steroidogenesis involves the concerted activity of steroidogenic enzymes in catalyzing the conversion of cholesterol and the production of different types of steroids depending on the cell type, tissue type, or species. The steroidogenic acute regulatory protein (StAR) facilitates the mobilization of free cholesterol from the cytoplasm into the mitochondria. The enzyme “cytochrome P450scc” (also known as CYP11A1) cleaves the cholesterol side chain to produce pregnenolone, which is then converted to other steroids via oxidation by a series of oxidative enzymes present in both the mitochondria and the endoplasmic reticulum [12].
Five classes of steroid hormones include (1) glucocorticoids (with cortisol being the main glucocorticoid in humans and corticosterone in rodents, reptiles, and birds), (2) mineralocorticoids (with aldosterone being the main mineralocorticoids in humans) (3) estrogens such as estrone and estradiol, (4) progestins such as progesterone, and (5) androgens such as dihydrotestosterone and testosterone [5]. In addition to the canonical tissue-specific trophic hormone regulation of steroid hormone biosynthesis and the transcriptional and translational events underlying the regulation of chronic steroidogenesis [38], there are several other mechanisms of regulation of the steroidogenic pathway that are currently under investigation. These include post-transcriptional and post-translational regulatory mechanisms such as phosphorylation/dephosphorylation, as well as miRNA and protein–protein interactions [5].
MiRNAs play a critical role in the regulation of steroidogenesis. Using computational studies, several miRNAs have been identified that bind to specific sequences in the 3′UTR of various target mRNAs of steroidogenic enzymes and thus modulate their expression. These miRNAs are currently being validated in various experimental conditions and models [10, 119]. MiRNAs regulate different steps of corticosteroid biosynthesis. Downregulation of miRNA levels by Dicer1 knockdown induced the expression of several corticosteroidogenic genes, including CYP11A1, CYP11B1, CYP11B2, CYP17A1, and CYP21A. Increased expression of these genes was associated with increased levels of steroids such as corticosterone, aldosterone, and 18-hydroxycorticosterone. In this study, miR-125a-5p and miR-125b-5p were shown to directly suppress CYP11B2 expression levels in vitro [88]. MiR-132 has been shown to modulate steroidogenesis. It represses StAR protein expression while inducing 20α-HSD enzyme mRNA levels, leading to the production of biologically inactive steroids [40]. Together with collaborators, we have previously described the dysregulation of adrenal miRNAs in different forms of Cushing’s syndrome (CS). Analysis of human adrenal tissue revealed that miR-1247-5p and miR-379-5p are significantly associated with different CS subtypes [106]. Moreover, even circulating miRNAs are possible hypercortisolism biomarkers in different CS subtypes [105, 106]. MiR-150 negatively modulates steroidogenesis of Leydig cells in mice by targeting and repressing the expression of StAR [27]. Taken together, repression of steroidogenic enzyme expression and consequently steroid hormone synthesis by the action of miRNAs may prove critical in disrupting the reproductive system and normal physiological processes, as well as other developmental processes in which optimal steroid levels are essential. The effect of miRNAs on steroidogenesis may be crucial for ameliorating disorders associated with impaired steroid production. Understanding the role of miRNAs in the regulation of steroidogenesis is therefore of paramount importance.
Hypoxia regulates steroidogenesis via a crosstalk with microRNA
A number of studies with zebra fish, mouse, and different cell lines revealed the activity of hypoxia/HIF on steroidogenesis with a resultant disruption of aldosterone and glucocorticoid biosynthesis [53, 68, 114, 124]. Our group has recently described the effect of hypoxia pathway proteins on steroidogenesis. We reported that cell-specific overexpression of HIF1α in mouse adrenal cortical cells resulted in the impaired expression of essential steroidogenic enzymes and, consequently, steroids [118].
Steroidogenesis thrives on cholesterol availability, and although several reports have suggested a disruptive action on normal cholesterol biosynthesis and lipid accumulation as a result of HIF pathway activity, findings from our mouse model revealed a reduction in the size of lipid droplets in the adrenal glands associated with increased steroid production [118]. Such a perceived contradiction in the differential activity of the HIF pathway in regulating cholesterol metabolism and steroidogenesis may point to the presence of other HIF-independent regulators under conditions of complete hypoxia, which are absent in our mouse model. Sterol regulatory element binding protein 2 (SREBP2) has recently been described as a central transcription factor underlying mammalian sterol production. SREBP2 is degraded under hypoxia in a HIF-independent manner, ultimately distorting normal sterol production [21].
Mechanistically, the effect of HIF on steroidogenesis is possible through different mechanisms. HIFs can directly bind to the promoters of steroidogenic enzyme genes and regulate their transcription. For example, HIF1α has been reported to directly repress the expression of the mitochondrial cholesterol transporter StAR by directly binding to 3 different HREs in the StAR promoter [114] (see Fig. 2). Admittedly, this study represents one of the very few and unusual examples of direct HIF-mediated suppression of gene expression. Other possible mechanisms such as the displacement of other important transcriptional activators, HIF interaction with specific epigenetic factors, and the recruitment of co-repressors to HIF may therefore be involved in mediating the HIF1 negative regulation of StAR expression and other gene expressions in general [74, 95].
Hypoxia pathway proteins-microRNA-phosphodiesterase crosstalk in steroidogenesis regulation. Hypoxia regulates steroid production through either direct binding of HIFs to the HREs in the promoter of steroidogenic enzymes or by a crosstalk of HIFs with other regulators such as microRNAs (miRNAs) and phosphodiesterases (PDE) (see further). The expression and activity of steroidogenic enzymes as well as steroidogenesis are regulated by miRNAs and PDE. MiRNAs and PDE are also regulated by each other, which ultimately impacts steroidogenesis either positively or negatively. MiRNAs may also target Hif1α. Hypoxia is able to alter the expression and activity of miRNAs and PDE, which ultimately affects steroid production
MiRNAs are potent epigenetic regulators of gene expression [26, 81, 129]. As described in other established reports where HIF negatively regulates different biological processes, HIF may also mechanistically regulate steroidogenesis through its established crosstalk with miRNAs [37, 48, 113, 131]. Using in silico algorithms such as PicTar (http://pictar.bio.nyu.edu/), TargetScan (http://www.targetscan.org/), and Sanger microRNA target (http://microrna.sanger.ac.uk/), potential miRNAs of steroidogenic enzymes can be identified. In this way, the upregulation of miRNAs targeting mRNAs of steroidogenic enzymes can potentially elucidate the paradox of the negative regulation of steroidogenesis upon hypoxia/HIF1α upregulation [57, 80].
Recent studies have investigated the effect of hypoxia on the activity of miRNAs in the regulation of steroidogenesis. Hypoxia-inducible miR-10 was reported to be a negative regulator of two important steroidogenic enzymes, namely CYP11B1 and CYP11B2, repressing their expression in H295R, a human adrenocortical carcinoma cell line [80]. CYP19A1 (Aromatase) was reported to be downregulated as a result of the induction of a HIF1-inducible miRNA, miR-98 [127].
Hitherto, most hypoxia-microRNA–related studies on steroidogenesis have been investigated across in vitro experimental models [80]. It would be of great interest to conduct studies in models that closely reflect real physiological conditions, such as in steroidogenic tissues and in vivo experimental models, to corroborate the first few existing findings on the impact of hypoxia-microRNA crosstalk and steroidogenesis regulation. To further elucidate the exact molecular mechanisms by which hypoxia regulates steroidogenesis, under hypoxia, the experimental validation of other unexplored miRNAs that have already been predicted to target steroidogenic enzymes and regulate steroidogenesis is worth pursuing in future studies.
Hypoxia-inducible factor prolyl hydroxylase inhibitors (PHDi) and steroidogenesis
Given the critical role of hypoxia/HIFs in steroid production as described in the previous sections, it is important and appropriate to highlight some of the currently available opportunities to stabilize HIFs and thereby modulate steroid production. Several HIF stabilizers with potential clinical relevance have been approved in the past and/or are currently under clinical trials [62, 116, 130]. Although most of these drugs are primarily designed to treat conditions such as anemia of various etiologies, ischemia, and inflammation, not much is known about their effects on steroid production. Most of the drugs currently available to inhibit the activity of PHD include the HIF competitors, iron chelators, iron displacers, and α-ketoglutarate mimetics. Drugs such as roxadustat, dimethyloxalylglycine (DMOG), enarodustat, daprodustat, desidustat or ZYAN1 (Zydus), and vadadustat belong to the group of α-ketoglutarate mimetics. Deferoxamine (DFO) and ciclopirox are metal chelators. Metal ions such as cobalt, manganese, nickel, and zinc are iron displacers [82]. The most clinically advanced of these drugs are the 2-OG derivatives, which compete with 2-oxoglutarate (2-OG) for binding sites in PHDs, rendering them inactive [116].
It is worth noting that some of the hypoxia-inducible factor prolyl hydroxylase inhibitors (HIF-PHIs) may affect cholesterol levels, probably directly related to the fact that HIF has been shown to reduce cholesterol synthesis [43]. Roxadustat treatment has been shown to result in lower LDL cholesterol levels [14, 62, 83]. Conversely, no clear correlations were observed for the effect of the oral hypoxia–inducible factor prolyl hydroxylase inhibitor vadadustat on cholesterol levels after use in phase 2 clinical trials [77]. The explanations for the observed ambivalence in the role of different HIF-PHIs on cholesterol levels remain poorly understood and require further investigation [61]. The extent to which non-erythropoietic pathways are targeted in patients receiving these treatments remains a puzzle, and the use of these interventions is not without potential risks [54]. The lack of mechanistic specificity in the action of these drugs may interfere with normal steroid production even after HIFs have been stabilized. Future studies delineating the full effects of these drugs on steroidogenesis and cholesterol metabolism are warranted.
The effect of clinically approved roxadustat on steroidogenesis in immortalized murine KK1 granulosa cells has been reported. Treatment of these cells with roxadustat resulted in a biphasic StAR protein expression response. Specifically, at lower roxadustat concentrations, the expression of the StAR protein was upregulated; however, with increased doses of roxadustat and consequent enhancement in HIF1α stabilization, StAR expression levels were significantly reduced indicating an inverse relationship between HIF1α and StAR expression levels [29]. The role of cobalt chloride (CoCl2)-induced hypoxia on steroid production in Leydig cell–derived MA-10 cells has been reported, with CoCl2 treatment leading to the inhibition of progesterone production as well as direct inhibition of P450scc mRNA levels, which could be attributed to the resultant increased HIF1α activity [55]. Karimi and colleagues also examined how melatonin treatment affects steroidogenesis following hypoxia induction in TM3 Leydig cells. Treatment of these cells with CoCl2 resulted in decreased Hsd3b1 and StAR mRNA/protein expression [50]. In contrast, administration of dimethyloxalylglycine (DMOG) led to an increase in plasma corticosterone as early as 5 min after airpuff startle (APS), an acute stressor, which was abolished by 2 h [31].
However, the use of these drugs is not without limitations due to unspecific PHD binding and possible off-target effects of α-ketoglutarate mimetics, as there are more than 50 α-ketoglutarate-dependent oxygenases in the human genome. Also, the toxicity of cobalt and the involvement of iron in many cellular processes and its displacement or chelation can have dire consequences. A great concern has also been directed to their use, as the prolonged stabilization of HIFs may result in modulations in the expression of arrays of HIF target genes and may be implicated in the etiology of pathologies such as increased risk of hyperkalemia and iron deficiency development. Consequently, further research aimed at modifying the activities and specificities of these drugs, as well as reducing their side effects, is of paramount importance in order to maximize their therapeutic efficacy and maybe even steroidogenesis regulatory potential [116].
The regulation of PHDs by microRNAs has been suggested and also requires further investigation to better understand the possibilities around the miR-PHD axis as a mechanism for steroidogenesis regulation. In this regard, Chen and colleagues have already shown that miR-17 is able to target prolyl hydroxylases 2 (PHD2) in its 3′-UTR and that overexpression of miR-17 in pulmonary artery smooth muscle cells (PASMC) leads to the decreased expression of PHD2 and induction of HIF1α protein levels [15]. Further research on the repressive potential of microRNAs on PHD expression, which would ultimately promote HIF1 activity, as well as the implications for steroidogenesis is warranted.
Phosphodiesterases regulate adrenal cAMP-dependent steroidogenesis
Steroidogenesis is also induced by the cAMP signaling pathway downstream of the ACTH receptor in the adrenal gland. Stimulation of the G-protein-coupled ACTH receptor leads to activation of adenylate cyclases (ACs), which generate the intracellular second messenger cAMP. Further activation of cAMP-dependent protein kinase A (PKA) promotes steroidogenesis by both acute and chronic mechanisms [103]. The acute mechanism involves the phosphorylation of StAR, which facilitates the transport of cholesterol into the mitochondria for steroid hormone synthesis [67]. The chronic mechanism involves the transcriptional regulation of steroidogenic enzymes, which is mediated by the phosphorylation of transcription factors by cAMP-dependent PKA [46].
The spatial and temporal concentration of cellular cAMP is controlled by the interplay between its production by ACs and its hydrolysis by phosphodiesterases (PDE). In mammalian species, 11 families of PDE have been described, each characterized by distinct kinetics, regulatory partners, and tissue distribution [109]. PDE play a pivotal role in governing the intracellular levels of both cAMP and cGMP, as well as the respective signaling pathways and downstream targets. The adrenal cortex expresses several isoforms of PDEs [58]. Here, we will focus on PDEs which are associated with adrenal gland–related diseases. Current research projects in our organization are focused on investigating a potential link between PDE-HIF and steroidogenesis (see further).
PDE2
The predominant PDE isoform in adrenal tissue is PDE2A, which is a dual-substrate phosphodiesterase capable of degrading both cAMP and cGMP with similar affinities (35 µM for cAMP and 11 µM for cGMP). PDE2A can be stimulated via cGMP-binding to the regulatory GAF-B domain thereby enhancing the cAMP hydrolyses up to 30-fold [69]. Thus, PDE2 induces a so-called negative cGMP/cAMP crosstalk, which has been described in several cell types, including cardiomyocytes and adrenal zona glomerulosa cells [91, 110]. In the heart, the cGMP-dependent PDE2 activation as well as PDE2 overexpression resulted in reduced catecholamine-induced arrhythmia after myocardial infarction [11, 71, 108]. In situ hybridization showed a strong expression of PDE2 in the zona glomerulosa cells of the adrenal gland [102]. PDE2 was the first cAMP degrading enzyme that was described to directly regulate steroid synthesis. In zona glomerulosa cells, the A-type natriuretic peptide (ANP) induced cGMP generation upon NPRA receptor stimulation. The following cGMP-dependent activation of PDE2 resulted in dose-dependent cAMP hydrolysis and attenuation of aldosterone secretion [65]. The ANP effect in human glomerulosa cells was prevented by PDE2 inhibition with EHNA (erythron-9-[2-hydroxo-3-nonyl] adenine) [17]. The influence of the simultaneous activation of the cGMP-dependent protein kinase G (PKG) on aldosterone secretion is controversially discussed. In rat glomerulosa cells, the direct PKG stimulation with the cGMP analog 8-pCPT-cGMP promoted aldosterone synthesis [100], whereas the injection of ANP reduced serum aldosterone levels in WT mice but not in mice with genetic PKGII deletion [25]. The consequences of cGMP-dependent PDE2 stimulation are cell specific, but mediate beneficial effects in cardiomyocytes and adrenal glomerulosa cells [11, 107]
PDE8
The PDE8 family also plays a role in adrenal steroidogenesis. The two isoforms PDE8A and PDE8B, encoded by different genes, specifically degrade cAMP with high affinity (Km = 0.15 µM) without affecting cGMP. While PDE8A is expressed only at low levels in a subpopulation of adrenal zona fasciculata cells, transcripts of PDE8B are highly abundant throughout the fasciculata layers [34, 104]. Using isoform-specific knockout mice, PDE8B was shown to control the corticosterone production in the adrenal gland by regulating the activity of cAMP-dependent PKA and the expression of StAR protein [103, 104]. PDE8B knockout mice showed elevated urinary corticosterone levels due to adrenal hypersensitivity to ACTH with enhanced steroid production. Specific PDE8 inhibition increases acute adrenal steroid production in adrenal Y-1 cells in vitro as well as basal adrenal steroidogenesis in vivo [104]. A point mutation of PDE8B was identified in patients with adrenal hyperplasia [35]. Heterogeneous expression of the mutant in HEK cells increased cellular cAMP levels, suggesting that impaired PDE8B function, amongst other factors, may contribute to the development of adrenal hyperplasia.
PDE11
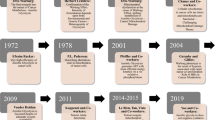
PDE11 was the last identified enzyme of the PDE family and is encoded by one single gene PDE11A with four transcriptional splicing variants (PDE11A1 to PDE11A4) [66]. Like PDE2, PDE11A is a dual-specificity phosphodiesterase that catalyzes the hydrolysis of both cAMP and cGMP with similar affinities. The function of its regulatory GAF-domains remains unclear. PDE11A is expressed in several endocrine tissues, including the adrenal gland [18]. Mice with global genetic PDE11A deletion showed only a reduced enzyme expression but displayed adrenal subcapsular hyperplasia with preserved fetal-like proteins in the inner adrenal cortex [60]. In contrast to WT mice, PDE11A KO mice were not responsive to a low dose dexamethasone treatment followed by the suppression of corticosterone secretion. In tissue lysates from adrenal glands, PDE11B deletion resulted in enhanced cAMP concentrations and increased PKA activity [60]. Human PDE11A defects are associated to adrenal diseases, after a genome-wide study identified the chromosome 2q31.2 PDE11A gene locus in 2006 [33]. Three PDE11A mutations have been reported in Cushing syndrome patients with primary pigmented nodular or isolated micronodular adrenocortical disease. Furthermore, single-nucleotide polymorphisms, truncation mutations, and missense substitutions in the PDE11A sequence have been linked to adrenocortical tumors [52].
PDE3
PDE3 is a family of phosphodiesterases that hydrolyze both second messengers, but with significantly higher catalytic rates for cAMP than for cGMP. At the same time, PDE3 has similar high affinities for cAMP and cGMP, resulting in competitive inhibition of cAMP hydrolysis in the presence of cGMP. Therefore, PDE3 is often referred to as the cGMP-inhibited PDE [76]. Within the PDE3 family, two genes—PDE3A and PDE3B—have been identified, including three transcriptional isoforms of PDE3A that differ in the length of the N-terminal sequence. PDE3 is mainly expressed in the myocardium with minor transcripts in other tissues, such as the adrenal gland [58], but few studies have reported the influence of PDE3 on steroidogenesis. In human adrenocortical H295R cells, specific PDE3 inhibition with cilostamide decreased angiotensin II–stimulated aldosterone levels, suggesting the idea of targeting PDE3 in the treatment of hypertension [16]. Another study demonstrated the inhibition of ACTH-induced cortisol secretion by leptin in human adrenocortical carcinoma cells (NCI-H295). The leptin effect was downstream mediated by PDE3-induced cAMP degradation, since selective PDE3 inhibition abrogated the reduction of cortisol synthesis [36]. Two rare germline variants in the PDE3B gene were identified in patients with primary aldosteronism and bilateral adrenal hyperplasia. The PDE3B mutants mediated a significant reduction in PDE3B expression levels in transfected HEK cells. Another germline nonsense variant of PDE3B was discovered in a child with an adrenocortical tumor [85].
Phosphodiesterases are regulated by miRNA
There is evidence that microRNAs play a role in the regulation of phosphodiesterases, which are also expressed in the adrenal gland. Previous studies have shown that PDE2 is the host gene for miR-139, which is in the second intron of the PDE2A gene sequence. Accordingly, a strong correlation was observed between miR-139 and PDE2A expression levels, as well as DNA methylation in the PDE2A promoter [94, 115]. In human glioblastoma tissues, miR-139 expression was associated with PDE2A transcription and shared correlation of expression levels. However, the overexpression of miR-139 increased the mRNA levels of PDE2A and pre-miR-139 in glioblastoma cell lines. In addition to the dependency of expression, both miR-139 and PDE2A act synergistically in glioblastoma cells by repressing detrimental Wnt/β-catenin signaling and reducing the tumorigenesis of gliomas [63].
In silico prediction identified 67 PDE3A-related miRNAs, including miR-27a-3p and miR-222-3p. Expression of these miRNAs in a human endothelial cell line resulted in a significant reduction of PDE3A expression [126]. In suppressive regulatory T cells (Treg), it was shown that miR-142-5p directly targets the PDE3B mRNA, limiting PDE3B protein levels. Thereby, miR-142-5p regulated intracellular cAMP levels and controlled Treg suppressive functions [3]. Interestingly, the Treg-specific deletion of miR-142 in mice led to enhanced PDE3 expression in Treg cells, impaired suppressive Treg function and lethal multisystem autoimmunity while PDE3 inhibition with cilostamide restored Treg function and prevents autoimmune disease [3].
The influence of miRNAs on PDE8A was investigated in immune and cancer cells. Thus, miR-145-5p was shown to regulate PDE8 expression levels by targeting the 3′UTR of the PDE8A mRNA transcript. Accordingly, PDE8A expression negatively correlates with miR-145-5p levels during the differentiation of monocytes into macrophages [9]. Another study showed the association of PDE8A with miR-33a in glioma cells. In vivo inhibition of miR-33a using a locked nucleic acid (LNA) enhanced the PDE8A expression and reduced tumor growth in mice [112].
Using computational-driven methods, intronic regions of the oncogene musashi RNA binding protein 1 (MSI1) were analyzed for potential precursor miRNAs. The study identified the new precursor miRNA MSM-3, which is expressed in several cancerous cell lines as well as human breast cancer tissue. PDE11 was confirmed to be a direct target of MSM3-3p addressing the 3′UTR region of PDE11A. Cancer cell lines with high miR MSM3-3p expression displayed reduced PDE11 levels [56]. In microarray analysis of miRNA and related genes in colorectal cancer stromal tissue, PDE11A was found to be highly inversely correlated with two other miRNAs, namely miR-18a and miR-19a [79].
Hypoxia-phosphodiesterase crosstalk, a possible mechanism in the regulation of steroidogenesis?
The role of some PDE isoforms in steroidogenesis has been described in earlier sections of this review, and several isoforms are expressed in the adrenal gland, including the ubiquitous phosphodiesterase 5 [45]. Other PDE isoforms have been identified in normal adrenal glands, cortisol-producing adenomas, and macro-nodular adrenocortical hyperplasia, such as PDE11A, PDE2A, PDE8E, and PDE8B [30, 34].
Hypoxia pathway proteins modulate phosphodiesterase expression and activity, while modulation of the PDE activity by hypoxia affects downstream signaling pathways. At the molecular level, HIF2α has been shown to induce the expression of cAMP-specific phosphodiesterases, which was confirmed by the inhibition of HIF prolyl hydroxylases [87]. It was shown that the induction of cAMP-specific phosphodiesterase expression and activity (including PDE4 and 7) in a HIF2α-dependent manner ultimately leads to glucagon signaling and sensitivity blockade in mouse and human hepatocytes. These findings suggest a PHD-dependent regulation of PDE via HIF2α [87] (see Fig. 2).
Hypoxia has been described to activate the cAMP/PKA pathway by inducing the expression of the adenylyl cyclase system of enzymes that facilitate the production of cAMP. The cAMP/PKA pathway is important for cells to adapt to hypoxia. Studies have shown that HIF regulation of adenylyl cyclases 6 and 7 led to the induction of cancer-associated cAMP and PKA signaling despite increased activity of PDEs that control cAMP degradation [99]. In human pulmonary artery smooth muscle cells (hPASM cells), hypoxia was shown to mediate a brief induction of PDE4B2 expression, which later peaked after day 7, with concomitant upregulation of both intracellular cAMP levels without altering total cAMP PDE3 or cAMP PDE4 activity. However, in this study, hypoxia also upregulated PDE4D5 and PDE4A10/11 levels over a 14-day period [73]. The effects of PDE-selective inhibitors in the treatment of various physiological and pathological conditions, including steroidogenesis, have been described. Vardenafil, a phosphodiesterase 5 inhibitor, has been shown to promote angiogenesis via a protein kinase G-dependent HIF1/VEGF pathway [92]. Tadalafil, a type 5 phosphodiesterase inhibitor, increases salivary cortisol levels in response to stress [20].
Hypoxia appears to upregulate both cAMP levels and PDE expression depending on the cellular context or tissue type. In addition, severe hypoxia has been reported to negatively affect protein kinase A phosphorylation [47]. The cAMP/PKA pathway, which can be regulated by PDE, is critical for StAR expression and activity [53]. Given that both hypoxia and PDE affect steroidogenesis as described in the previous discussion, and that hypoxia can affect PDE activity, we propose that there is a crosstalk between PDE and hypoxia in the regulation of steroidogenesis. Hypoxia induction of PDE may result in the modulation of cAMP levels required to regulate certain aspects of steroidogenesis. Studies elucidating such a relationship are scarce and warranted. Elucidation of such crosstalk may provide great insight into further delineation of other molecular mechanisms by which hypoxia may regulate steroidogenesis in steroid-producing cells. Findings from such studies may potentially point to novel therapeutic avenues.
Modulation of miRNA expression by second messengers and steroid hormones
Interestingly, some studies have also reported the modulation of miRNA expression in response to hormonal treatment and second messenger activity. Several miRNAs expressed in the adrenal gland and other steroidogenic cells are regulated by various hormones and the second messenger cAMP. This regulation ultimately affects the steroid output of these cells/tissues. The miRNA-132 expression level is increased in undisturbed adrenal glands following adrenocorticotropic hormone (ACTH) treatment and in Y1 adrenocortical cells following cAMP treatment [40]. MiRNA-455, miRNA-125a, and miRNA-125b expression levels are reduced in rat adrenals treated with ACTH in vivo as well as in MLTC-1 cells and primary rat granulosa cells treated with cyclic AMP (cAMP) [39]. Treatment of rats with ACTH, dexamethasone, or 17α-E2 affects the expression of several miRNAs. Specifically in the adrenal glands, miRNA-182, miRNA-212, miRNA-132, miRNA-183, and miRNA-96 expression levels are upregulated while miRNA-214, miRNA-27a, miRNA-503, and miRNA-466b expression levels are downregulated upon ACTH treatment. In response to treatment with 17α-E2, the expression levels of miRNA-200b, miRNA27a, miR-125b, miR-122, miRNA-214, miR-138, miRNA-466b, and miRNA-503 are downregulated, whereas the expression levels of miRNA-370, miR-212, miRNA-377, miRNA-183, miRNA-96, miRNA-370, and miRNA-132 are upregulated. Treatment with dexamethasone only led to an increased miRNA-183 expression level and a decrease in the expression levels of miR-19a, miRNA-200b, miRNA27a, miR-122, and miRNA-466b [38].
There is an interaction between pituitary-adrenal axis hormones and circulating microRNAs associated with the adrenal cortex. Hormonal treatment of 10 individuals with either dexamethasone or tetracosactide (adrenocorticotropin) altered the expression profile of miRNAs in human plasma samples. Hsa-miR-27a expression was suppressed by adrenocorticotropin, whereas dexamethasone induced its expression. This effect was also recapitulated in NCI-H295R cells treated with dexamethasone. Since adrenal mass dexamethasone suppression and ACTH stimulation assays are very important functional endocrine diagnostic tests, knowledge of microRNA expression patterns as a result of these assays may be particularly useful in screening for adrenal malignancies that would ultimately affect normal adrenocortical hormone production. [44]. Sex steroid hormones also regulate microRNA expression. Treatment of EEC cell lines with estrogen-induced miR-196a-5p expression and increased the viability of these cells by targeting Forkhead box protein O1 (FOXO1) [132]. Progesterone induces miR-145/143 expression leading to the inhibition of cyclin D2 expression and proliferation of endometrial epithelial cells [128].
These studies reveal a complex interplay between hormones, second messengers, microRNAs and steroidogenesis. MicroRNAs under the control of various hormones are important in mediating the regulatory control of these hormones on steroidogenesis. Increased steroid levels may be attenuated by a possible feedback mechanism that induces the expression of microRNAs to negatively control the expression of steroid biosynthetic enzymes. Future studies are needed to decipher the precise molecular mechanisms underlying the interaction between microRNAs and these different hormones, the role of specific hormone-regulated miRNAs in adrenal cells, the consequences for the regulation of steroidogenesis, and their biological relevance.
Conclusions and perspectives
Pathophysiological hypoxia can occur in a variety of environmental and pathological conditions and may well adversely affect systemic processes including the nervous, cardiovascular, and endocrine systems [78]; the latter encompassing the adrenal, pancreatic, thyroid, and ovarian glands, which play central roles in maintaining the body’s homeostasis [59]. Hypoxia/HIF has been widely considered systemically undruggable due to its critical role in regulating myriad physiological processes. Therefore, the focus is now shifting to targeting downstream effectors of HIF as a means to generate novel and less complicated therapies [59]. Since miRNAs and PDE may be such downstream effectors, and there is bidirectional crosstalk between both, pharmacological targeting of hypoxia-inducible miRNAs may provide potential interventions for ameliorating several diseases [48]. Conversely, since the hypoxia pathway proteins play a vital role in the adrenal gland, uncontrolled deregulation of their expression or related machinery may negatively affect normal adrenal function and lead to various adrenal-related disorders. In addition, the therapeutic use of HIF prolyl hydroxylase inhibitors (PHDi) must be carefully controlled and their effects on steroidogenesis well considered. Further research is therefore warranted to better understand these diverse effects, including potential links between HIF-PDE and steroidogenesis, and to translate them into new potential therapies.
Data availability
No datasets were generated or analyzed during the current study.
References
Akhtar S, Hartmann P, Karshovska E, Rinderknecht FA, Subramanian P, Gremse F, Grommes J, Jacobs M, Kiessling F, Weber C, Steffens S, Schober A (2015) Endothelial hypoxia-inducible factor-1 alpha promotes atherosclerosis and monocyte recruitment by upregulating microRNA-19a. Hypertension 66:1220–1226. https://doi.org/10.1161/HYPERTENSIONAHA.115.05886
Alfar EA, El-Armouche A, Guan K (2018) MicroRNAs in cardiomyocyte differentiation and maturation. Cardiovasc Res 114:779–781. https://doi.org/10.1093/cvr/cvy065
Anandagoda N, Willis JC, Hertweck A, Roberts LB, Jackson I, Gokmen MR, Jenner RG, Howard JK, Lord GM (2019) MicroRNA-142-mediated repression of phosphodiesterase 3B critically regulates peripheral immune tolerance. J Clin Invest 129:1257–1271. https://doi.org/10.1172/JCI124725
Assidicky R, Tokat UM, Tarman IO, Saatci O, Ersan PG, Raza U, Ogul H, Riazalhosseini Y, Can T, Sahin O (2022) Targeting HIF1-alpha/miR-326/ITGA5 axis potentiates chemotherapy response in triple-negative breast cancer. Breast Cancer Res Treat 193:331–348. https://doi.org/10.1007/s10549-022-06569-5
Azhar S, Dong DC, Shen WJ, Hu ZG, Kraemer FB (2020) The role of miRNAs in regulating adrenal and gonadal steroidogenesis. J Mol Endocrinol 64:R21–R43. https://doi.org/10.1530/Jme-19-0105
Berra E, Benizri E, Ginouvès A, Volmat V, Roux D, Pouysségur J (2003) HIF prolyl-hydroxylase 2 is the key oxygen sensor setting low steady-state levels of HIF-1alpha in normoxia. Embo j 22:4082–4090. https://doi.org/10.1093/emboj/cdg392
Bersten DC, Sullivan AE, Peet DJ, Whitelaw ML (2013) bHLH-PAS proteins in cancer. Nat Rev Cancer 13:827–841. https://doi.org/10.1038/nrc3621
Bhatt K, Wei QQ, Pabla N, Dong GE, Mi QS, Liang MY, Mei CL, Dong Z (2015) MicroRNA-687 induced by hypoxia-inducible factor-1 targets phosphatase and tensin homolog in renal ischemia-reperfusion injury. J Am Soc Nephrol 26:1588–1596. https://doi.org/10.1681/Asn.2014050463
Booiman T, Cobos Jimenez V, van Dort KA, van’tWout AB, Kootstra NA (2014) Phosphodiesterase 8a supports HIV-1 replication in macrophages at the level of reverse transcription. PLoS One 9:e109673. https://doi.org/10.1371/journal.pone.0109673
Bruning U, Cerone L, Neufeld Z, Fitzpatrick SF, Cheong A, Scholz CC, Simpson DA, Leonard MO, Tambuwala MM, Cummins EP, Taylor CT (2011) MicroRNA-155 promotes resolution of hypoxia-inducible factor 1alpha activity during prolonged hypoxia. Mol Cell Biol 31:4087–4096. https://doi.org/10.1128/MCB.01276-10
Cachorro E, Gunscht M, Schubert M, Sadek MS, Siegert J, Dutt F, Bauermeister C, Quickert S, Berning H, Nowakowski F, Lammle S, Firneburg R, Luo X, Kunzel SR, Klapproth E, Mirtschink P, Mayr M, Dewenter M, Vettel C, Heijman J, Lorenz K, Guan K, El-Armouche A, Wagner M, Kammerer S (2023) CNP promotes antiarrhythmic effects via phosphodiesterase 2. Circ Res 132:400–414. https://doi.org/10.1161/CIRCRESAHA.122.322031
Chakraborty S, Pramanik J, Mahata B (2021) Revisiting steroidogenesis and its role in immune regulation with the advanced tools and technologies. Genes Immun 22:125–140. https://doi.org/10.1038/s41435-021-00139-3
Chen K, Wang Q, Liu X, Wang F, Yang Y, Tian X (2022) Hypoxic pancreatic cancer derived exosomal miR-30b-5p promotes tumor angiogenesis by inhibiting GJA1 expression. Int J Biol Sci 18:1220–1237. https://doi.org/10.7150/ijbs.67675
Chen N, Hao C, Peng X, Lin H, Yin A, Hao L, Tao Y, Liang X, Liu Z, Xing C, Chen J, Luo L, Zuo L, Liao Y, Liu BC, Leong R, Wang C, Liu C, Neff T, Szczech L, Yu KP (2019) Roxadustat for anemia in patients with kidney disease not receiving dialysis. N Engl J Med 381:1001–1010. https://doi.org/10.1056/NEJMoa1813599
Chen TJ, Zhou QY, Tang HY, Bozkanat M, Yuan JXJ, Raj JU, Zhou GF (2016) miR-17/20 controls prolyl hydroxylase 2 (PHD2)/hypoxia-inducible factor 1 (HIF1) to regulate pulmonary artery smooth muscle cell proliferation. J Am Heart Assoc 5. ARTN e004510. https://doi.org/10.1161/JAHA.116.004510
Chen Y, Iyer SR, Nikolaev VO, Naro F, Pellegrini M, Cardarelli S, Ma X, Lee HC, Burnett JC Jr (2022) MANP activation of the cGMP inhibits aldosterone via PDE2 and CYP11B2 in H295R cells and in mice. Hypertension 79:1702–1712. https://doi.org/10.1161/HYPERTENSIONAHA.121.18906
Cote M, Payet MD, Rousseau E, Guillon G, Gallo-Payet N (1999) Comparative involvement of cyclic nucleotide phosphodiesterases and adenylyl cyclase on adrenocorticotropin-induced increase of cyclic adenosine monophosphate in rat and human glomerulosa cells. Endocrinology 140:3594–3601. https://doi.org/10.1210/endo.140.8.6889
D’Andrea MR, Qiu Y, Haynes-Johnson D, Bhattacharjee S, Kraft P, Lundeen S (2005) Expression of PDE11A in normal and malignant human tissues. J Histochem Cytochem 53:895–903. https://doi.org/10.1369/jhc.5A6625.2005
Dayan F, Roux D, Brahimi-Horn MC, Pouyssegur J, Mazure NM (2006) The oxygen sensor factor-inhibiting hypoxia-inducible factor-1 controls expression of distinct genes through the bifunctional transcriptional character of hypoxia-inducible factor-1alpha. Cancer Res 66:3688–3698
Di Luigi L, Baldari C, Sgrò P, Emerenziani GP, Gallotta MC, Bianchini S, Romanelli F, Pigozzi F, Lenzi A, Guidetti L (2008) The type 5 phosphodiesterase inhibitor tadalafil influences salivary cortisol, testosterone, and dehydroepiandrosterone sulphate responses to maximal exercise in healthy men. J Clin Endocr Metab 93:3510–3514. https://doi.org/10.1210/jc.2008-0847
Dickson AS, Pauzaite T, Arnaiz E, Ortmann BM, West JA, Volkmar N, Martinelli AW, Li ZQ, Wit N, Vitkup D, Kaser A, Lehner PJ, Nathan JA (2023) A HIF independent oxygen-sensitive pathway for controlling cholesterol synthesis. Nat Commun 14. ARTN 4816. https://doi.org/10.1038/s41467-023-40541-1
Ding H, Li J, Li Y, Yang M, Nie S, Zhou M, Zhou Z, Yang X, Liu Y, Hou FF (2021) MicroRNA-10 negatively regulates inflammation in diabetic kidney via targeting activation of the NLRP3 inflammasome. Mol Ther 29:2308–2320. https://doi.org/10.1016/j.ymthe.2021.03.012
Dong HF, Lei JP, Ding L, Wen YQ, Ju HX, Zhang XJ (2013) MicroRNA: function, detection, and bioanalysis. Chem Rev 113:6207–6233. https://doi.org/10.1021/cr300362f
Duan YB, Bai X, Yang JX, Zhou Y, Gu WQ, Liu GQ, Wang Q, Zhu JB, La LL, Li XY (2022) Exposure to high-altitude environment is associated with drug transporters change: microRNA-873-5p-mediated alteration of function and expression levels of drug transporters under hypoxia. Drug Metab Dispos 50:174–186. https://doi.org/10.1124/dmd.121.000681
Gambaryan S, Butt E, Marcus K, Glazova M, Palmetshofer A, Guillon G, Smolenski A (2003) cGMP-dependent protein kinase type II regulates basal level of aldosterone production by zona glomerulosa cells without increasing expression of the steroidogenic acute regulatory protein gene. J Biol Chem 278:29640–29648. https://doi.org/10.1074/jbc.M302143200
Gebert LFR, MacRae IJ (2019) Regulation of microRNA function in animals. Nat Rev Mol Cell Bio 20:21–37. https://doi.org/10.1038/s41580-018-0045-7
Geng XJ, Zhao DM, Mao GH, Tan L (2017) MicroRNA-150 regulates steroidogenesis of mouse testicular Leydig cells by targeting STAR. Reproduction 154:229–236. https://doi.org/10.1530/Rep-17-0234
Greco S, Gaetano C, Martelli F (2014) HypoxamiR regulation and function in ischemic cardiovascular diseases. Antioxid Redox Sign 21:1202–1219. https://doi.org/10.1089/ars.2013.5403
Gysin T, Kowalewski MP (2021) The involvement of hypoxia-inducible factor 1alpha (HIF1alpha)-stabilising factors in steroidogenic acute regulatory (STAR) protein-dependent steroidogenesis in murine KK1 granulosa cells in vitro. Reprod Fertil Dev 33:865–880. https://doi.org/10.1071/RD21170
Hannah-Shmouni F, Faucz FR, Stratakis CA (2016) Alterations of phosphodiesterases in adrenocortical tumors. Front Endocrinol (Lausanne) 7:111. https://doi.org/10.3389/fendo.2016.00111
Harrell CS, Rowson SA, Neigh GN (2015) Pharmacological stimulation of hypoxia inducible factor-1α facilitates the corticosterone response to a mild acute stressor. Neurosci Lett 600:75–79. https://doi.org/10.1016/j.neulet.2015.05.051
Hirsila M, Koivunen P, Gunzler V, Kivirikko KI, Myllyharju J (2003) Characterization of the human prolyl 4-hydroxylases that modify the hypoxia-inducible factor. J Biol Chem 278:30772–30780. https://doi.org/10.1074/jbc.M304982200
Horvath A, Boikos S, Giatzakis C, Robinson-White A, Groussin L, Griffin KJ, Stein E, Levine E, Delimpasi G, Hsiao HP, Keil M, Heyerdahl S, Matyakhina L, Libe R, Fratticci A, Kirschner LS, Cramer K, Gaillard RC, Bertagna X, Carney JA, Bertherat J, Bossis I, Stratakis CA (2006) A genome-wide scan identifies mutations in the gene encoding phosphodiesterase 11A4 (PDE11A) in individuals with adrenocortical hyperplasia. Nat Genet 38:794–800. https://doi.org/10.1038/ng1809
Horvath A, Giatzakis C, Tsang K, Greene E, Osorio P, Boikos S, Libe R, Patronas Y, Robinson-White A, Remmers E, Bertherat J, Nesterova M, Stratakis CA (2008) A cAMP-specific phosphodiesterase (PDE8B) that is mutated in adrenal hyperplasia is expressed widely in human and mouse tissues: a novel PDE8B isoform in human adrenal cortex. Eur J Hum Genet 16:1245–1253. https://doi.org/10.1038/ejhg.2008.85
Horvath A, Mericq V, Stratakis CA (2008) Mutation in PDE8B, a cyclic AMP-specific phosphodiesterase in adrenal hyperplasia. N Engl J Med 358:750–752. https://doi.org/10.1056/NEJMc0706182
Hsu HT, Chang YC, Chiu YN, Liu CL, Chang KJ, Guo IC (2006) Leptin interferes with adrenocorticotropin/3’,5’-cyclic adenosine monophosphate (cAMP) signaling, possibly through a Janus kinase 2-phosphatidylinositol 3-kinase/Akt-phosphodiesterase 3-cAMP pathway, to down-regulate cholesterol side-chain cleavage cytochrome P450 enzyme in human adrenocortical NCI-H295 cell line. J Clin Endocrinol Metab 91:2761–2769. https://doi.org/10.1210/jc.2005-2383
Hu XQ, Dasgupta C, Song R, Romero M, Wilson SM, Zhang LB (2021) MicroRNA-210 mediates hypoxia-induced repression of spontaneous transient outward currents in sheep uterine arteries during gestation. Hypertension 77:1412–1427. https://doi.org/10.1161/Hypertensionaha.120.16831
Hu Z, Shen WJ, Cortez Y, Tang X, Liu LF, Kraemer FB, Azhar S (2013) Hormonal regulation of microRNA expression in steroid producing cells of the ovary, testis and adrenal gland. PLoS ONE 8:e78040. https://doi.org/10.1371/journal.pone.0078040
Hu Z, Shen WJ, Kraemer FB, Azhar S (2012) MicroRNAs 125a and 455 repress lipoprotein-supported steroidogenesis by targeting scavenger receptor class B type I in steroidogenic cells. Mol Cell Biol 32:5035–5045. https://doi.org/10.1128/MCB.01002-12
Hu ZG, Shen WJ, Kraemer FB, Azhar S (2017) Regulation of adrenal and ovarian steroidogenesis by miR-132. J Mol Endocrinol 59:269–283. https://doi.org/10.1530/Jme-17-0011
Huang X, Ding LH, Bennewith KL, Tong RT, Welford SM, Ang KK, Story M, Le QT, Giaccia AJ (2009) Hypoxia-inducible miR-210 regulates normoxic gene expression involved in tumor initiation. Mol Cell 35:856–867. https://doi.org/10.1016/j.molcel.2009.09.006
Hui X, Al-Ward H, Shaher F, Liu CY, Liu N (2020) The role of miR-210 in the biological system: a current overview. Hum Hered 84:233–239. https://doi.org/10.1159/000509280
Hwang S, Nguyen AD, Jo Y, Engelking LJ, Brugarolas J, DeBose-Boyd RA (2017) Hypoxia-inducible factor 1alpha activates insulin-induced gene 2 (Insig-2) transcription for degradation of 3-hydroxy-3-methylglutaryl (HMG)-CoA reductase in the liver. J Biol Chem 292:9382–9393. https://doi.org/10.1074/jbc.M117.788562
Igaz I, Nyiro G, Nagy Z, Butz H, Nagy Z, Perge P, Sahin P, Toth M, Racz K, Igaz P, Patocs A (2015) Analysis of circulating microRNAs in vivo following administration of dexamethasone and adrenocorticotropin. Int J Endocrinol 2015:589230. https://doi.org/10.1155/2015/589230
Ilias I, Zabuliene L (2019) Phosphodiesterase 5 inhibitors and adrenal incidentalomas. Med Hypotheses 130:109288. https://doi.org/10.1016/j.mehy.2019.109288
Jefferi NES, Shamhari A, Hamid ZA, Budin SB, Zulkifly AMZ, Roslan FN, Taib IS (2022) Knowledge gap in understanding the steroidogenic acute regulatory protein regulation in steroidogenesis following exposure to bisphenol A and its analogues. Biomedicines 10. https://doi.org/10.3390/biomedicines10061281
Jiang YF, Tsui KH, Wang PH, Lin CW, Wang JY, Hsu MC, Chen YC, Chiu CH (2011) Hypoxia regulates cell proliferation and steroidogenesis through protein kinase A signaling in bovine corpus luteum. Anim Reprod Sci 129:152–161. https://doi.org/10.1016/j.anireprosci.2011.12.004
Ju C, Wang M, Tak E, Kim B, Emontzpohl C, Yang Y, Yuan X, Kutay H, Liang Y, Hall DR, Dar WA, Bynon JS, Carmeliet P, Ghoshal K, Eltzschig HK (2021) Hypoxia-inducible factor-1alpha-dependent induction of miR122 enhances hepatic ischemia tolerance. J Clin Invest 131. https://doi.org/10.1172/JCI140300
Kaelin WG Jr, Ratcliffe PJ (2008) Oxygen sensing by metazoans: the central role of the HIF hydroxylase pathway. Mol Cell 30:393–402. https://doi.org/10.1016/j.molcel.2008.04.009
Karimi S, Jalili C, Mansouri K, Bahremand F, Gholami MR (2023) Effect of melatonin on steroidogenesis-related enzymes expression and testosterone synthesis following CoCl-induced hypoxia in TM3 Leydig cells. Iran J Basic Med Sci 26:1041–1046. https://doi.org/10.22038/Ijbms.2023.69570.15152
Kinget L, Roussel E, Verbiest A, Albersen M, Rodríguez-Antona C, Graña-Castro O, Inglada-Pérez L, Zucman-Rossi J, Couchy G, Job S, de Reyniès A, Laenen A, Baldewijns M, Beuselinck B (2021) MicroRNAs targeting HIF-2α, VEGFR1 and/or VEGFR2 as potential predictive biomarkers for VEGFR tyrosine kinase and HIF-2α inhibitors in metastatic clear-cell renal cell carcinoma. Cancers 13. ARTN 3099 https://doi.org/10.3390/cancers13123099
Kong G, Lee H, Vo TT, Juang U, Kwon SH, Park J, Park J, Kim SH (2022) Functional characteristics and research trends of PDE11A in human diseases (review). Mol Med Rep 26. https://doi.org/10.3892/mmr.2022.12814
Kowalewski MP, Gram A, Boos A (2015) The role of hypoxia and HIF1alpha in the regulation of STAR-mediated steroidogenesis in granulosa cells. Mol Cell Endocrinol 401:35–44. https://doi.org/10.1016/j.mce.2014.11.023
Ku E, Del Vecchio L, Eckardt KU, Haase VH, Johansen KL, Nangaku M, Tangri N, Waikar SS, Wiecek A, Cheung M, Jadoul M, Winkelmayer WC, Wheeler DC (2023) Novel anemia therapies in chronic kidney disease: conclusions from a Kidney Disease: Improving Global Outcomes (KDIGO) controversies conference. Kidney Int 104:655–680. https://doi.org/10.1016/j.kint.2023.05.009
Kumar A, Rani L, Dhole B (2014) Role of oxygen in the regulation of Leydig tumor derived MA-10 cell steroid production: the effect of cobalt chloride. Syst Biol Reprod Med 60:112–118. https://doi.org/10.3109/19396368.2013.861034
Lachinani L, Forouzanfar M, Dormiani K, Soltani BM, Dolatshahi K, Hakimian SM, Dokanehiifard S, Nasr-Esfahani MH (2023) The oncogene Musashi1 encodes novel miRNAs in breast cancer. Sci Rep 13:13710. https://doi.org/10.1038/s41598-023-40666-9
Lai KP, Li JW, Tse ACK, Chan TF, Wu RSS (2016) Hypoxia alters steroidogenesis in female marine medaka through miRNAs regulation. Aquat Toxicol 172:1–8. https://doi.org/10.1016/j.aquatox.2015.12.012
Lakics V, Karran EH, Boess FG (2010) Quantitative comparison of phosphodiesterase mRNA distribution in human brain and peripheral tissues. Neuropharmacology 59:367–374. https://doi.org/10.1016/j.neuropharm.2010.05.004
Lee HC, Tsai SJ (2017) Endocrine targets of hypoxia-inducible factors. J Endocrinol 234:R53–R65. https://doi.org/10.1530/JOE-16-0653
Levy I, Szarek E, Maria AG, Starrost M, De La Luz SM, Faucz FR, Stratakis CA (2021) A phosphodiesterase 11 (Pde11a) knockout mouse expressed functional but reduced Pde11a: phenotype and impact on adrenocortical function. Mol Cell Endocrinol 520:111071. https://doi.org/10.1016/j.mce.2020.111071
Li J, Haase VH, Hao CM (2023) Updates on hypoxia-inducible factor-prolyl hydroxylase inhibitors in the treatment of renal anemia. Kidney Dis-Basel 9:1–11. https://doi.org/10.1159/000527835
Li J, Haase VH, Hao CM (2023) Updates on hypoxia-inducible factor prolyl hydroxylase inhibitors in the treatment of renal anemia. Kidney Dis (Basel) 9:1–11. https://doi.org/10.1159/000527835
Li SZ, Ren KX, Zhao J, Wu S, Li J, Zang J, Fei Z, Zhao JL (2021) miR-139/PDE2A-Notch1 feedback circuit represses stemness of gliomas by inhibiting Wnt/beta-catenin signaling. Int J Biol Sci 17:3508–3521. https://doi.org/10.7150/ijbs.62858
Lia D, Yang PY, Xiong QH, Song XH, Yang XQ, Liu L, Yuan WJ, Rui YC (2010) MicroRNA-125a/b-5p inhibits endothelin-1 expression in vascular endothelial cells. J Hypertens 28:1646–1654. https://doi.org/10.1097/HJH.0b013e32833a4922
MacFarland RT, Zelus BD, Beavo JA (1991) High concentrations of a cGMP-stimulated phosphodiesterase mediate ANP-induced decreases in cAMP and steroidogenesis in adrenal glomerulosa cells. J Biol Chem 266:136–142
Makhlouf A, Kshirsagar A, Niederberger C (2006) Phosphodiesterase 11: a brief review of structure, expression and function. Int J Impot Res 18:501–509. https://doi.org/10.1038/sj.ijir.3901441
Manna PR, Dyson MT, Stocco DM (2009) Regulation of the steroidogenic acute regulatory protein gene expression: present and future perspectives. Mol Hum Reprod 15:321–333. https://doi.org/10.1093/molehr/gap025
Marchi D, Santhakumar K, Markham E, Li N, Storbeck KH, Krone N, Cunliffe VT, van Eeden FJM (2020) Bidirectional crosstalk between hypoxia-inducible factor and glucocorticoid signalling in zebrafish larvae. Plos Genet 16. ARTN e1008757. https://doi.org/10.1371/journal.pgen.1008757
Martinez SE, Wu AY, Glavas NA, Tang XB, Turley S, Hol WG, Beavo JA (2002) The two GAF domains in phosphodiesterase 2A have distinct roles in dimerization and in cGMP binding. Proc Natl Acad Sci U S A 99:13260–13265. https://doi.org/10.1073/pnas.192374899
McCormick RI, Blick C, Ragoussis J, Schoedel J, Mole DR, Young AC, Selby PJ, Banks RE, Harris AL (2013) miR-210 is a target of hypoxia-inducible factors 1 and 2 in renal cancer, regulates ISCU and correlates with good prognosis. Brit J Cancer 108:1133–1142. https://doi.org/10.1038/bjc.2013.56
Mehel H, Emons J, Vettel C, Wittköpper K, Seppelt D, Dewenter M, Lutz S, Sossalla S, Maier LS, Lechêne P, Leroy J, Lefebvre F, Varin A, Eschenhagen T, Nattel S, Dobrev D, Zimmermann WH, Nikolaev VO, Vandecasteele G, Fischmeister R, El-Armouche A (2013) Phosphodiesterase-2 is up-regulated in human failing hearts and blunts β-adrenergic responses in cardiomyocytes. J Am Coll Cardiol 62:1596–1606. https://doi.org/10.1016/j.jacc.2013.05.057
Meneses AM, Wielockx B (2016) PHD2: from hypoxia regulation to disease progression. Hypoxia (Auckl) 4:53–67. https://doi.org/10.2147/HP.S53576
Millen J, MacLean MR, Houslay MD (2006) Hypoxia-induced remodelling of PDE4 isoform expression and cAMP handling in human pulmonary artery smooth muscle cells. Eur J Cell Biol 85:679–691. https://doi.org/10.1016/j.ejcb.2006.01.006
Mole DR, Blancher C, Copley RR, Pollard PJ, Gleadle JM, Ragoussis J, Ratcliffe PJ (2009) Genome-wide association of hypoxia-inducible factor (HIF)-1alpha and HIF-2alpha DNA binding with expression profiling of hypoxia-inducible transcripts. J Biol Chem 284:16767–16775. https://doi.org/10.1074/jbc.M901790200
Moszynska A, Jaskiewicz M, Serocki M, Cabaj A, Crossman DK, Bartoszewska S, Gebert M, Dabrowski M, Collawn JF, Bartoszewski R (2022) The hypoxia-induced changes in miRNA-mRNA in RNA-induced silencing complexes and HIF-2 induced miRNAs in human endothelial cells. FASEB J 36:e22412. https://doi.org/10.1096/fj.202101987R
Movsesian M (2016) Novel approaches to targeting PDE3 in cardiovascular disease. Pharmacol Ther 163:74–81. https://doi.org/10.1016/j.pharmthera.2016.03.014
Nangaku M, Farag YMK, DeGoma E, Luo WL, Vargo D, Khawaja Z (2021) Vadadustat, an oral hypoxia-inducible factor prolyl hydroxylase inhibitor, for treatment of anemia of chronic kidney disease: two randomized phase 2 trials in Japanese patients. Nephrol Dial Transpl 36:1244–1252. https://doi.org/10.1093/ndt/gfaa060
Netzer N, Strohl K, Faulhaber M, Gatterer H, Burtscher M (2013) Hypoxia-related altitude illnesses. J Travel Med 20:247–255. https://doi.org/10.1111/jtm.12017
Nishida N, Nagahara M, Sato T, Mimori K, Sudo T, Tanaka F, Shibata K, Ishii H, Sugihara K, Doki Y, Mori M (2012) Microarray analysis of colorectal cancer stromal tissue reveals upregulation of two oncogenic miRNA clusters. Clin Cancer Res 18:3054–3070. https://doi.org/10.1158/1078-0432.CCR-11-1078
Nusrin S, Tong SKH, Chaturvedi G, Wu RSS, Giesy JP, Kong RYC (2014) Regulation of CYP11B1 and CYP11B2 steroidogenic genes by hypoxia-inducible miR-10b in H295R cells. Mar Pollut Bull 85:344–351. https://doi.org/10.1016/j.marpolbul.2014.04.002
O'Brien J, Hayder H, Zayed Y, Peng C (2018) Overview of microRNA biogenesis, mechanisms of actions, and circulation. Front Endocrinol 9. ARTN 402 https://doi.org/10.3389/fendo.2018.00402
Poloznikov AA, Nersisyan SA, Hushpulian DM, Kazakov EH, Tonevitsky AG, Kazakov SV, Vechorko VI, Nikulin SV, Makarova JA, Gazaryan IG (2020) HIF prolyl hydroxylase inhibitors for COVID-19 treatment: pros and cons. Front Pharmacol 11:621054. https://doi.org/10.3389/fphar.2020.621054
Provenzano R, Shutov E, Eremeeva L, Korneyeva S, Poole L, Saha G, Bradley C, Eyassu M, Besarab A, Leong R, Liu CS, Neff TB, Szczech L, Yu KHP (2021) Roxadustat for anemia in patients with end-stage renal disease incident to dialysis. Nephrol Dial Transpl 36:1717–1730. https://doi.org/10.1093/ndt/gfab051
Rani V, Sengar RS (2022) Biogenesis and mechanisms of microRNA-mediated gene regulation. Biotechnol Bioeng 119:685–692. https://doi.org/10.1002/bit.28029
Rassi-Cruz M, Maria AG, Faucz FR, London E, Vilela LAP, Santana LS, Benedetti AFF, Goldbaum TS, Tanno FY, Srougi V, Chambo JL, Pereira MAA, Cavalcante A, Carnevale FC, Pilan B, Bortolotto LA, Drager LF, Lerario AM, Latronico AC, Fragoso M, Mendonca BB, Zerbini MCN, Stratakis CA, Almeida MQ (2021) Phosphodiesterase 2A and 3B variants are associated with primary aldosteronism. Endocr Relat Cancer 28:1–13. https://doi.org/10.1530/ERC-20-0384
Ren R, Ma K, Jiang Y, Chen J, Kou Y, Ge Z, Chen Z, Wei X, Yu L (2023) Endothelial miR-196b-5p regulates angiogenesis via the hypoxia/miR-196b-5p/HMGA2/HIF1alpha loop. Am J Physiol Cell Physiol 324:C407–C419. https://doi.org/10.1152/ajpcell.00309.2022
Riopel M, Moon JS, Bandyopadhyay GK, You S, Lam K, Liu X, Kisseleva T, Brenner D, Lee YS (2020) Inhibition of prolyl hydroxylases increases hepatic insulin and decreases glucagon sensitivity by an HIF-2alpha-dependent mechanism. Mol Metab 41:101039. https://doi.org/10.1016/j.molmet.2020.101039
Robertson S, Diver LA, Alvarez-Madrazo S, Livie C, Ejaz A, Fraser R, Connell JM, MacKenzie SM, Davies E (2017) Regulation of corticosteroidogenic genes by microRNAs. Int J Endocrinol 2017. Artn 2021903. https://doi.org/10.1155/2017/2021903
Rodriguez D, Watts D, Gaete D, Sormendi S, Wielockx B (2021) Hypoxia pathway proteins and their impact on the blood vasculature. Int J Mol Sci 22. https://doi.org/10.3390/ijms22179191
Roganovic J (2021) Downregulation of microRNA-146a in diabetes, obesity and hypertension may contribute to severe COVID-19. Med Hypotheses 146:110448. https://doi.org/10.1016/j.mehy.2020.110448
Sadek MS, Cachorro E, El-Armouche A, Kammerer S (2020) Therapeutic implications for PDE2 and cGMP/cAMP mediated crosstalk in cardiovascular diseases. Int J Mol Sci 21. https://doi.org/10.3390/ijms21207462
Sahara M, Sata M, Morita T, Nakajima T, Hirata Y, Nagai R (2010) A phosphodiesterase-5 inhibitor vardenafil enhances angiogenesis through a protein kinase G-dependent hypoxia-inducible factor-1/vascular endothelial growth factor pathway. Arterioscl Throm Vas 30:1315-U1389. https://doi.org/10.1161/Atvbaha.109.201327
Saleh AA, El-Hefnawy SM, Kasemy ZA, Alhagaa AA, Nooh MZ, Arafat ES (2022) Mi-RNA-93 and Mi-RNA-152 in the diagnosis of type 2 diabetes and diabetic retinopathy. Br J Biomed Sci 79:10192. https://doi.org/10.3389/bjbs.2021.10192
Sannigrahi MK, Sharma R, Singh V, Panda NK, Rattan V, Khullar M (2017) Role of host miRNA Hsa-miR-139-3p in HPV-16-induced carcinomas. Clin Cancer Res 23:3884–3895. https://doi.org/10.1158/1078-0432.CCR-16-2936
Schodel J, Oikonomopoulos S, Ragoussis J, Pugh CW, Ratcliffe PJ, Mole DR (2011) High-resolution genome-wide mapping of HIF-binding sites by ChIP-seq. Blood 117:E207–E217. https://doi.org/10.1182/blood-2010-10-314427
Schofield CJ, Ratcliffe PJ (2004) Oxygen sensing by HIF hydroxylases. Nat Rev Mol Cell Biol 5:343–354. https://doi.org/10.1038/nrm1366
Serocki M, Bartoszewska S, Janaszak-Jasiecka A, Ochocka RJ, Collawn JF, Bartoszewski R (2018) miRNAs regulate the HIF switch during hypoxia: a novel therapeutic target. Angiogenesis 21:183–202. https://doi.org/10.1007/s10456-018-9600-2
Seyhan AA (2023) Circulating microRNAs as potential biomarkers in pancreatic cancer-advances and challenges. International Journal of Molecular Sciences 24. ARTN 13340. https://doi.org/10.3390/ijms241713340
Simko V, Iuliano F, Sevcikova A, Labudova M, Barathova M, Radvak P, Pastorekova S, Pastorek J, Csaderova L (2017) Hypoxia induces cancer-associated cAMP/PKA signalling through HIF-mediated transcriptional control of adenylyl cyclases VI and VII. Sci Rep-Uk 7. ARTN 10121. https://doi.org/10.1038/s41598-017-09549-8
Spiessberger B, Bernhard D, Herrmann S, Feil S, Werner C, Luppa PB, Hofmann F (2009) cGMP-dependent protein kinase II and aldosterone secretion. FEBS J 276:1007–1013. https://doi.org/10.1111/j.1742-4658.2008.06839.x
Spinello I, Quaranta MT, Paolillo R, Pelosi E, Cerio AM, Saulle E, Lo Coco F, Testa U, Labbaye C (2015) Differential hypoxic regulation of the microRNA-146a/CXCR4 pathway in normal and leukemic monocytic cells: impact on response to chemotherapy. Haematologica 100:1160–1171. https://doi.org/10.3324/haematol.2014.120295
Stephenson DT, Coskran TM, Wilhelms MB, Adamowicz WO, O’Donnell MM, Muravnick KB, Menniti FS, Kleiman RJ, Morton D (2009) Immunohistochemical localization of phosphodiesterase 2A in multiple mammalian species. J Histochem Cytochem 57:933–949. https://doi.org/10.1369/jhc.2009.953471
Tsai LC, Beavo JA (2011) The roles of cyclic nucleotide phosphodiesterases (PDEs) in steroidogenesis. Curr Opin Pharmacol 11:670–675. https://doi.org/10.1016/j.coph.2011.09.003
Tsai LC, Shimizu-Albergine M, Beavo JA (2011) The high-affinity cAMP-specific phosphodiesterase 8B controls steroidogenesis in the mouse adrenal gland. Mol Pharmacol 79:639–648. https://doi.org/10.1124/mol.110.069104
Vetrivel S, Zhang R, Engel M, Altieri B, Braun L, Osswald A, Bidlingmaier M, Fassnacht M, Beuschlein F, Reincke M, Chen A, Sbiera S, Riester A (2021) Circulating microRNA expression in Cushing’s syndrome. Front Endocrinol (Lausanne) 12:620012. https://doi.org/10.3389/fendo.2021.620012
Vetrivel S, Zhang R, Engel M, Osswald A, Watts D, Chen A, Wielockx B, Sbiera S, Reincke M, Riester A (2022) Characterization of adrenal miRNA-based dysregulations in Cushing’s syndrome. Int J Mol Sci 23. https://doi.org/10.3390/ijms23147676
Vettel C, Lämmle S, Ewens S, Cervirgen C, Emons J, Ongherth A, Dewenter M, Lindner D, Westermann D, Nikolaev VO, Lutz S, Zimmermann WH, El-Armouche A (2014) PDE2-mediated cAMP hydrolysis accelerates cardiac fibroblast to myofibroblast conversion and is antagonized by exogenous activation of cGMP signaling pathways. Am J Physiol-Heart C 306:H1246–H1252. https://doi.org/10.1152/ajpheart.00852.2013
Vettel C, Lindner M, Dewenter M, Lorenz K, Schanbacher C, Riedel M, Lammle S, Meinecke S, Mason FE, Sossalla S, Geerts A, Hoffmann M, Wunder F, Brunner FJ, Wieland T, Mehel H, Karam S, Lechene P, Leroy J, Vandecasteele G, Wagner M, Fischmeister R, El-Armouche A (2017) Phosphodiesterase 2 protects against catecholamine-induced arrhythmia and preserves contractile function after myocardial infarction. Circ Res 120:120–132. https://doi.org/10.1161/CIRCRESAHA.116.310069
Vezzosi D, Bertherat J (2011) Phosphodiesterases in endocrine physiology and disease. Eur J Endocrinol 165:177–188. https://doi.org/10.1530/EJE-10-1123
Wagner M, Sadek MS, Dybkova N, Mason FE, Klehr J, Firneburg R, Cachorro E, Richter K, Klapproth E, Kuenzel SR, Lorenz K, Heijman J, Dobrev D, El-Armouche A, Sossalla S, Kammerer S (2021) Cellular mechanisms of the anti-arrhythmic effect of cardiac PDE2 overexpression. Int J Mol Sci 22. https://doi.org/10.3390/ijms22094816
Wang GL, Jiang BH, Rue EA, Semenza GL (1995) Hypoxia-inducible factor 1 is a basic-helix-loop-helix-PAS heterodimer regulated by cellular O2 tension. Proc Natl Acad Sci U S A 92:5510–5514. https://doi.org/10.1073/pnas.92.12.5510
Wang H, Sun T, Hu J, Zhang R, Rao Y, Wang S, Chen R, McLendon RE, Friedman AH, Keir ST, Bigner DD, Li QJ, Wang H, Wang XF (2014) miR-33a promotes glioma-initiating cell self-renewal via PKA and NOTCH pathways. J Clin Invest 124:4489–4502. https://doi.org/10.1172/JCI75284
Wang X, Xu X, Zhu Q, Han Y, Zhang W (2022) Hypoxia-induced miR-182-5p regulates vascular smooth muscle cell phenotypic switch by targeting RGS5. Cell Biol Int 46:1864–1875. https://doi.org/10.1002/cbin.11883
Wang X, Zou Z, Yang Z, Jiang S, Lu Y, Wang D, Dong Z, Xu S, Zhu L (2018) HIF 1 inhibits StAR transcription and testosterone synthesis in murine Leydig cells. J Mol Endocrinol. https://doi.org/10.1530/JME-18-0148
Watanabe K, Amano Y, Ishikawa R, Sunohara M, Kage H, Ichinose J, Sano A, Nakajima J, Fukayama M, Yatomi Y, Nagase T, Ohishi N, Takai D (2015) Histone methylation-mediated silencing of miR-139 enhances invasion of non-small-cell lung cancer. Cancer Med 4:1573–1582. https://doi.org/10.1002/cam4.505
Watts D, Gaete D, Rodriguez D, Hoogewijs D, Rauner M, Sormendi S, Wielockx B (2020) Hypoxia pathway proteins are master regulators of erythropoiesis. Int J Mol Sci 21. https://doi.org/10.3390/ijms21218131
Watts D, Jaykar MT, Bechmann N, Wielockx B (2022) Hypoxia signaling pathway: a central mediator in endocrine tumors. Front Endocrinol (Lausanne) 13:1103075. https://doi.org/10.3389/fendo.2022.1103075
Watts D, Stein J, Meneses A, Bechmann N, Neuwirth A, Kaden D, Kruger A, Sinha A, Alexaki VI, Perez-Rivas LG, Kircher S, Martinez A, Theodoropoulou M, Eisenhofer G, Peitzsch M, El-Armouche A, Chavakis T, Wielockx B (2021) HIF1 alpha is a direct regulator of steroidogenesis in the adrenal gland. Cell Mol Life Sci 78:3577–3590. https://doi.org/10.1007/s00018-020-03750-1
Witkos TM, Koscianska E, Krzyzosiak WJ (2011) Practical aspects of microRNA target prediction. Curr Mol Med 11:93–109. https://doi.org/10.2174/156652411794859250
Xia X, Lemieux ME, Li W, Carroll JS, Brown M, Liu XS, Kung AL (2009) Integrative analysis of HIF binding and transactivation reveals its role in maintaining histone methylation homeostasis. Proc Natl Acad Sci U S A 106:4260–4265. https://doi.org/10.1073/pnas.0810067106
Xie L, Wang Y, Li Q, Ji X, Tu Y, Du S, Lou H, Zeng X, Zhu L, Zhang J, Zhu M (2021) The HIF-1alpha/p53/miRNA-34a/Klotho axis in retinal pigment epithelial cells promotes subretinal fibrosis and exacerbates choroidal neovascularization. J Cell Mol Med 25:1700–1711. https://doi.org/10.1111/jcmm.16272
Xie Y, Li W, Feng J, Wu T, Li J (2016) MicroRNA-363 and GATA-1 are regulated by HIF-1alpha in K562 cells under hypoxia. Mol Med Rep 14:2503–2510. https://doi.org/10.3892/mmr.2016.5578
Yamakuchi M, Lotterman CD, Bao C, Hruban RH, Karim B, Mendell JT, Huso D, Lowenstein CJ (2010) P53-induced microRNA-107 inhibits HIF-1 and tumor angiogenesis. Proc Natl Acad Sci U S A 107:6334–6339. https://doi.org/10.1073/pnas.0911082107
Yamashita K, Ito K, Endo J, Matsuhashi T, Katsumata Y, Yamamoto T, Shirakawa K, Isobe S, Kataoka M, Yoshida N, Goto S, Moriyama H, Kitakata H, Mitani F, Fukuda K, Goda N, Ichihara A, Sano M (2020) Adrenal cortex hypoxia modulates aldosterone production in heart failure. Biochem Biophys Res Commun 524:184–189. https://doi.org/10.1016/j.bbrc.2020.01.088
Yang YM, Qu AL, Wu Q, Zhang X, Wang LL, Li C, Dong ZG, Du LT, Wang CX (2020) Prognostic value of a hypoxia-related microRNA signature in patients with colorectal cancer. Aging-Us 12:35–52
Yasmeen S, Kaur S, Mirza AH, Brodin B, Pociot F, Kruuse C (2019) miRNA-27a-3p and miRNA-222-3p as novel modulators of phosphodiesterase 3a (PDE3A) in cerebral microvascular endothelial cells. Mol Neurobiol 56:5304–5314. https://doi.org/10.1007/s12035-018-1446-5
Yu RM, Chaturvedi G, Tong SK, Nusrin S, Giesy JP, Wu RS, Kong RY (2015) Evidence for microRNA-mediated regulation of steroidogenesis by hypoxia. Environ Sci Technol 49:1138–1147. https://doi.org/10.1021/es504676s
Yuan DZ, Lei Y, Zhao D, Pan JL, Zhao YB, Nie L, Liu M, Long Y, Zhang JH, Yue LM (2019) Progesterone-induced miR-145/miR-143 inhibits the proliferation of endometrial epithelial cells. Reprod Sci 26:233–243. https://doi.org/10.1177/1933719118768687
Zaporozhchenko IA, Rykova EY, Laktionov PP (2020) The fundamentals of miRNA biology: structure, biogenesis, and regulatory functions. Russ J Bioorg Chem+ 46:1–13. https://doi.org/10.1134/S106816202001015x
Zhao H, Li P, Zhang HL, Jia L (2023) An updated meta-analysis on the efficacy and safety of hypoxia-inducible factor prolyl hydroxylase inhibitor treatment of anemia in nondialysis-dependent chronic kidney disease. Ren Fail 45:2258986. https://doi.org/10.1080/0886022X.2023.2258986
Zheng H, Wang N, Li L, Ge L, Jia H, Fan Z (2021) miR-140-3p enhanced the osteo/odontogenic differentiation of DPSCs via inhibiting KMT5B under hypoxia condition. Int J Oral Sci 13:41. https://doi.org/10.1038/s41368-021-00148-y
Zhu Y, Tang Y, Fan Y, Wu D (2023) MiR-196a-5p facilitates progression of estrogen-dependent endometrial cancer by regulating FOXO1. Histol Histopathol 38:1157–1168. https://doi.org/10.14670/HH-18-5
Acknowledgements
This work was supported by grants from the DFG (German Research Foundation) within the CRC/Transregio 205/1, Project No. 314061271—TRR205, “The Adrenal: Central Relay in Health and Disease” (A02) to B.W. and A.E.-A.; DFG grants WI3291/12-1 and 13-1 to B.W., EL 270/7-3 to A.E.-A., KA 4194/3-3 to S.K. This work was also supported by a grant from the DFG priority program µBONE 2084 and a cancer research grant from the Wilhelm Sander foundation to B.W.; project no. 288034826—International Research Training Group (IRTG) 2251 to A.E.A. and S.K.
Figures were created with BioRender.com.
Funding
Open Access funding enabled and organized by Projekt DEAL. This work was supported by grants from the DFG (German Research Foundation) within the CRC/Transregio 205/1, Project No. 314061271—TRR205, “The Adrenal: Central Relay in Health and Disease “ (A02) to B.W. and A.E.-A.; DFG grants WI3291/12–1 and 13–1 to B.W., EL 270/7–3 to A.E.-A., KA 4194/3–3 to S.K. This work was also supported by a grant from the DFG priority program µBONE 2084 and a cancer research grant from the Wilhelm Sander foundation to B.W.; project no. 288034826—International Research Training Group (IRTG) 2251 to A.E.A. and S.K.
Author information
Authors and Affiliations
Contributions
S.A., S.K., and B.W. wrote the manuscript. E.K. and A.E.-A. contributed to the discussion.
Corresponding authors
Ethics declarations
Ethical approval
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Stephen Ariyeloye and Susanne Kämmerer equally contributed as first authors, and Ben Wielockx and Ali El-Armouche equally contributed as last authors.
This article is part of the special issue on Oxygen Sensors – HIF-Hydroxylases in Physiology, Pathophysiology and Pharmacology in Pflügers Archiv—European Journal of Physiology.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ariyeloye, S., Kämmerer, S., Klapproth, E. et al. Intertwined regulators: hypoxia pathway proteins, microRNAs, and phosphodiesterases in the control of steroidogenesis. Pflugers Arch - Eur J Physiol (2024). https://doi.org/10.1007/s00424-024-02921-4
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00424-024-02921-4