Abstract
Introduction
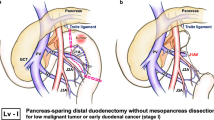
Pancreatoduodenectomy is the standard procedure for duodenal carcinoma of the third or fourth portion. As an alternative option, we developed a novel segmental resection (SR) with partial mesopancreatic and mesojejunal excision (pMME) that enhances radicality. In this report, the surgical technique with video and outcomes are described.
Method
We performed SR with pMME on seven consecutive patients with third or fourth duodenal carcinoma between 2009 and 2021. We divided the procedure into four sections, including (1) wide Kocher’s maneuver, (2) supracolic anterior artery-first approach, (3) dissection of the mesopancreas and mesojejunum, and (4) devascularization of the uncinate process and dissection of duodenum.
Result
Median operative time was 348 min (range, 222–391 min), and median blood loss was 100 mL (range, 30–580 mL). Major complications of Clavien-Dindo classification grade 3a or more occurred in one patient. All patients achieved R0 resections with 10 mm or more proximal margin. Six cases (85%) were alive without recurrence.
Conclusion
We developed a radical and safe procedure of SR with pMME as an alternative and less invasive approach for duodenal carcinoma of the third or fourth portion.




Similar content being viewed by others
Abbreviations
- PD:
-
Pancreatoduodenectomy
- SR:
-
Segmental resection
- pMME:
-
Partial mesopancreatic and mesojejunal excision
- SMV:
-
Superior mesenteric vein
- SMA:
-
Superior mesenteric artery
- IPDA:
-
Inferior pancreatoduodenal artery
- JA:
-
Jejunal artery
References
Overman MJ, Hu CY, Kopetz S, Abbruzzese JL, Wolff RA, Chang GJ (2012) A population-based comparison of adenocarcinoma of the large and small intestine: insights into a rare disease. Ann Surg Oncol 19(5):1439–1445. https://doi.org/10.1245/s10434-011-2173-6
Sakamoto T, Saiura A, Ono Y, Mise Y, Inoue Y, Ishizawa T et al (2017) Optimal lymphadenectomy for duodenal adenocarcinoma: does the number alone matter? Ann Surg Oncol 24(11):3368–3375. https://doi.org/10.1245/s10434-017-6044-7
Cloyd JM, George E, Visser BC (2016) Duodenal adenocarcinoma: advances in diagnosis and surgical management. World J Gastrointestinal Surg 8(3):212–221. https://doi.org/10.4240/wjgs.v8.i3.212
Tocchi A, Mazzoni G, Puma F, Miccini M, Cassini D, Bettelli E et al (1960) 2003 Adenocarcinoma of the third and fourth portions of the duodenum: results of surgical treatment. Archives Surg (Chicago, Ill) 138(1):80–5. https://doi.org/10.1001/archsurg.138.1.80
Poultsides GA, Huang LC, Cameron JL, Tuli R, Lan L, Hruban RH et al (2012) Duodenal adenocarcinoma: clinicopathologic analysis and implications for treatment. Ann Surg Oncol 19(6):1928–1935. https://doi.org/10.1245/s10434-011-2168-3
Lee SY, Lee JH, Hwang DW, Kim SC, Park KM, Lee YJ (2014) Long-term outcomes in patients with duodenal adenocarcinoma. ANZ J Surg 84(12):970–975. https://doi.org/10.1111/ans.12112
Solaini L, Jamieson NB, Metcalfe M, Abu Hilal M, Soonawalla Z, Davidson BR et al (2015) Outcome after surgical resection for duodenal adenocarcinoma in the UK. Br J Surg 102(6):676–681. https://doi.org/10.1002/bjs.9791
Sugiyama M, Suzuki Y, Nakazato T, Yokoyama M, Kogure M, Matsuki R et al (2020) Vascular anatomy of mesopancreas in pancreatoduodenectomy using an intestinal derotation procedure. World J Surg 44(10):3441–3448. https://doi.org/10.1007/s00268-020-05605-z
Inoue Y, Saiura A, Yoshioka R, Ono Y, Takahashi M, Arita J et al (2015) Pancreatoduodenectomy with systematic mesopancreas dissection using a supracolic anterior artery-first approach. Ann Surg 262(6):1092–1101. https://doi.org/10.1097/sla.0000000000001065
Inoue Y, Saiura A, Tanaka M, Matsumura M, Takeda Y, Mise Y et al (2016) Technical details of an anterior approach to the superior mesenteric artery during pancreaticoduodenectomy. J Gastrointestinal Surg : Official J Soci Surg Alimentary Tract 20(10):1769–1777. https://doi.org/10.1007/s11605-016-3214-z
West NP, Hohenberger W, Weber K, Perrakis A, Finan PJ, Quirke P (2010) Complete mesocolic excision with central vascular ligation produces an oncologically superior specimen compared with standard surgery for carcinoma of the colon. J Clin Oncol : Official J American Soc Clin Oncol 28(2):272–278. https://doi.org/10.1200/jco.2009.24.1448
Popescu I, Dumitrascu T (2011) Total meso-pancreas excision: key point of resection in pancreatic head adenocarcinoma. Hepatogastroenterology 58(105):202–207
Gockel I, Domeyer M, Wolloscheck T, Konerding MA, Junginger T (2007) Resection of the mesopancreas (RMP): a new surgical classification of a known anatomical space. World J Surgical Oncol 5:44. https://doi.org/10.1186/1477-7819-5-44
Gaedcke J, Gunawan B, Grade M, Szöke R, Liersch T, Becker H et al (2010) The mesopancreas is the primary site for R1 resection in pancreatic head cancer: relevance for clinical trials. Langenbeck’s Arch Surg 395(4):451–458. https://doi.org/10.1007/s00423-009-0494-8
Zaheer S, Pemberton JH, Farouk R, Dozois RR, Wolff BG, Ilstrup D (1998) Surgical treatment of adenocarcinoma of the rectum. Ann Surg 227(6):800–811. https://doi.org/10.1097/00000658-199806000-00003
Sharma D, Isaji S (2016) Mesopancreas is a misnomer: time to correct the nomenclature. J Hepatobiliary Pancreat Sci 23(12):745–749. https://doi.org/10.1002/jhbp.402
Cloyd JM, Norton JA, Visser BC, Poultsides GA (2015) Does the extent of resection impact survival for duodenal adenocarcinoma? Analysis of 1,611 cases. Ann Surg Oncol 22(2):573–580. https://doi.org/10.1245/s10434-014-4020-z
Nitta N, Ohgi K, Sugiura T, Okamura Y, Ito T, Yamamoto Y et al (2020) Prognostic impact of pancreatic invasion in duodenal carcinoma: a single-center experience. Ann Surg Oncol 27(11):4553–4560. https://doi.org/10.1245/s10434-020-08512-8
Mann K, Gilbert T, Cicconi S, Jackson R, Whelan P, Campbell F et al (2019) Tumour stage and resection margin status are independent survival factors following partial pancreatoduodenectomy for duodenal adenocarcinoma. Langenbecks Arch Surg 404(4):439–449. https://doi.org/10.1007/s00423-019-01779-w
Cecchini S, Correa-Gallego C, Desphande V, Ligorio M, Dursun A, Wargo J et al. 2012 Superior prognostic importance of perineural invasion vs. lymph node involvement after curative resection of duodenal adenocarcinoma. J Gastrointestinal Surger : Official J Soc Surg Alimentary Tract 16 1 113–20 discussion 20. https://doi.org/10.1007/s11605-011-1704-6
Sohn TA, Lillemoe KD, Cameron JL, Pitt HA, Kaufman HS, Hruban RH et al (1998) Adenocarcinoma of the duodenum: factors influencing long-term survival. J Gastrointestinal Surg : Official J Soc Surg Alimentary Tract 2(1):79–87. https://doi.org/10.1016/s1091-255x(98)80107-8
Bracale U, Pontecorvi E, Silvestri V, Cuccurullo D, D’Ambra M, Lionetti R et al (2021) Laparoscopic segmental resection for tumours of the Angle of Treitz: a challenging but feasible surgical option. Results Retrospective Case-Series Anal Updates Surg 73(1):179–86. https://doi.org/10.1007/s13304-020-00910-7
Fuks D, Piessen G, Huet E, Tavernier M, Zerbib P, Michot F et al (2009) Life-threatening postoperative pancreatic fistula (grade C) after pancreaticoduodenectomy: incidence, prognosis, and risk factors. Am J Surg 197(6):702–709. https://doi.org/10.1016/j.amjsurg.2008.03.004
Kuroki N, Ono Y, Sato T, Inoue Y, Oba A, Ito H et al (2022) Long-term outcome of patients with postoperative refractory diarrhea after tailored nerve plexus dissection around the major visceral arteries during pancreatoduodenectomy for pancreatic cancer. World J Surg. https://doi.org/10.1007/s00268-022-06457-5
Burasakarn P, Higuchi R, Nunobe S, Kanaji S, Eguchi H, Okada KI et al (2021) Limited resection vs. pancreaticoduodenectomy for primary duodenal adenocarcinoma: a systematic review and meta-analysis. Int J Clin Oncol 26(3):450–60. https://doi.org/10.1007/s10147-020-01840-510.1007/s10147-020-01840-5
Author information
Authors and Affiliations
Contributions
Study conception and design: R.I, M.Y, Y.T, Y.I, A.S. Acquisition of data: R.I. Analysis and interpretation of data: R.I, M.Y, A.S. Drafting of manuscript: R.I, M.Y. Critical revision of manuscript: Y.T, Y.I, A.S.
Corresponding author
Ethics declarations
Conflict of interest
Our institutional review board approved this retrospective study with waived informed consent. All authors have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 64459 KB)
Rights and permissions
About this article
Cite this article
Ito, R., Mise, Y., Takahashi, Y. et al. Segmental resection with partial mesopancreatic and mesojejunal excision (pMME) for duodenal carcinoma of the third or fourth portion. Langenbecks Arch Surg 407, 2143–2150 (2022). https://doi.org/10.1007/s00423-022-02569-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-022-02569-7