Abstract
Purpose
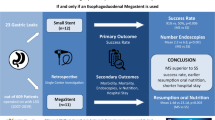
Presentation of results of non-stenting treatment versus endoscopic stenting placement in gastric staple leaks after laparoscopic sleeve gastrectomy (LSG).
Methods
Between January 2007 and August 2020, 1371 eligible patients underwent LSG. After gastric leak detection, patients were classified into treatment groups A (endoscopic stent placement) and B (non-stenting management). Overall hospital stay, the time to complete gastric leak resolution and the incidence of further operative management constituted the main outcome measures. Statistical analysis included descriptive statistics and linear regression tests as needed.
Results
A total of 27 patients (19 F/8 M, median age: 44.8 years (range: 36–58) with median preoperative BMI: 43.5 kg/m2 (range: 37.0–48.7)) presented with gastric staple line leak (1.9%) — mean detection day 5.8 postop (range: 1–12). Eight patients enrolled in group A and 19 patients in group B. The mean hospital stay for group A was 41.2 days (range: 24–60) versus 15 days (range: 12–18) for group B (p < 0.001). Complete leakage resolution was observed at mean 42.4 days (range 25–60) for group A and 34.5 days (range: 28–40) for group B patients, (p = 0.025). Only 2 group A patients accomplished complete leak resolution without additional intervention. Five group A patients (62.5%) versus 4 group B patients (21.1%) needed operative intervention during the treatment course (p = 0.037).
Conclusions
Conservative, non-stenting treatment of staple line leaks after LSG is feasible and is associated with superior results in terms of hospital say and leak resolution in comparison to endoscopic stenting.
Similar content being viewed by others
Introduction
During the last decade, laparoscopic sleeve gastrectomy (LSG) has become the most common bariatric procedure performed worldwide [1]. Technically, the procedure involves the creation of a small gastric reservoir based on the lesser curvature of the stomach preserving the antrum and pylorus together with its vagal innervation. Medically, its classic indication as a multi-purpose procedure for morbid obesity through gastric volume restriction to induce satiety and resection of the fundal ghrelin-producing cells to decrease appetite [2, 3] has been expanded to include an emerging role for the treatment of metabolic syndrome and type 2 diabetes mellitus [4, 5].
Perioperative major and minor complications do occur, with a reported incidence of approximately 5% and 11%, respectively [5, 6]. Staple-line complications, such as bleeding or gastric content leak presenting with an estimated mean incidence between 2.2 and 2.4%, rank among the most feared, as both may lead to significant morbidity and even patient death [6]. Efforts to reduce these rates, such as staple line suture or use of reinforcement material, have been met with unclear results [7, 8]. Additionally, since gastric leaks pose serious therapeutic challenges, much interest has been given as to better define their severity based on their location, the clinical presentation and the time of onset, to standardize the management approach [9,10,11].
The aim of this study is to present for gastric staple line leaks after LSG during the last 13 years in our Academic Bariatric Centre.
Materials and methods
This study is a retrospective analysis of our database in patients who:
-
i.
Were eligible for LSG exhibiting Body Mass Index (BMI) > 40 kg/m2 or > 35 kg/m2 with relevant comorbidities and have undergone LSG at the 1st Clinic, Division of Morbid Obesity and Metabolic Surgery, “Ippokrateion” Hospital, National and Kapodistrian University of Athens School of Medicine
-
ii.
Had a radiographically proven staple line leak after LSG
All patients received preoperative psychological, endoscopic upper GI, cardiologic, anesthesiologic and nutritional assessment and each one of them signed an informed consent. Exclusion criteria for the study were as follows: patient’s age greater than 60 years and patient’s inability to undergo general anaesthesia. The authors obtained the data through retrospective chart review of the hospital database. Institutional Review Board approval was also obtained for the research study. All operations were performed by a single surgeon.
Patient data
Patients’ demographic data, operative and perioperative data, and the presence of leak were recorded and analysed. More specifically, the interventional means used to manage the gastric leaks, the interval between LSG and gastric leak detection and the interval between diagnosis and leak closure were recorded. Main outcome measures of the study were the overall hospital stay, the time to complete gastric leak resolution and the incidence of operative management needed after the application of endoscopic stenting or conservative management. Moreover, we analysed and presented the adverse events associated with both treatment options and provide our treatment algorithm of gastric staple line leaks.
Laparoscopic sleeve gastrectomy operative technique — immediate postoperative management
The same operative technique was applied to all patients. The technical details of the procedure in brief are as follows: Peritoneal cavity entrance is accomplished with the Opti-view trocar (Ethicon Endo-Surgery, Inc.). After the identification of the pylorus, omental dissection commences 5–7 cm cephalad and is performed with the LCSC5 Coagulating Shears (Ethicon Endo-Surgery, Inc.). Then follows the ligation of all branches of the gastroepiploic vessels at their point of entrance to the greater curvature and the complete mobilization of the gastric body and fundus from any posterior attachments. A 38-Fr boogie is then placed to transect the stomach along the lesser curvature applying multiple firings of Echelon Compact Linear Cutter, 60 mm (Ethicon Endo-Surgery, Inc.). A combination of green reloads (4.1 mm) for the first two firings and blue reloads (3.5 mm) for the upper stomach was used. All patients were operated using the same cartridge size. Intraoperative gastric leak test is routinely performed with methylene blue instillation (80–100 ml) through a nasogastric tube placed right above the gastroesophageal junction. Presence of blue dye at the operating field confirms a positive intra-operative leak test. A penrose drain is left adjacent to the staple line depending on surgeon preference at the time of operation completion. Routinely, on the second postoperative day, a gastrographin swallow test is performed and if negative, the patient is discharged, and the drain is kept in place for the next 8–10 days. Removal of the drain is accomplished when there is no discharge from the drain and the patient exhibits neither signs nor symptoms of gastric staple line leakage.
Gastric leak management principles — patient groups
After the radiographic confirmation of gastric staple-line leak using abdominal CT scan in all patients presenting with tachycardia, fever or abdominal pain, either laparoscopic or endoscopic drain placement near the leak site was readily accomplished. Thereafter, as soon as the patient was deemed clinically and hemodynamically stable, the management proceeded to either:
-
i.
Endoscopic stent placement at the gastroesophageal junction region (group A) or
-
ii.
Non-stenting treatment with total parenteral nutrition (TPN), intravenous fluids and broad-spectrum antibiotics institution (group B). TPN was given through a central line placed at the right or left subclavian vein with the total amount of calories administered per day calculated by the Harris-Benedict equation.
Parameters that may affect the choice of the treatment plan such as the size of the extraluminal collection and the type and size of stent used were assessed. Moreover, a clinical score called quick SOFA (Sequential Organ Failure Assessment) was recorded at patient admission. This score includes respiratory rate of 22/min or greater, altered mentation or systolic blood pressure of 100 mm Hg or less. Using this score in out-of-hospital, emergency department or general hospital ward settings, adult patients with suspected infection can be rapidly identified as being more likely to have poor outcomes typical of sepsis, if they have at least 2 of the above clinical criteria [12, 13]. APACHE II scores were not calculated.
Definition and classification of gastric staple line leak
Leakage was defined as:
-
i.
extravasation of dye or gastrointestinal secretions through the abdominal drain and/or
-
ii.
positive clinical signs and laboratory markers of inflammation and sepsis and
-
iii.
radiological evidence of contrast extravasation and/or surgical site collection.
Diagnosis of all leaks was accomplished with abdominal computed tomography scanning in a standard multi-slice technique after liquid contrast media ingestion and/or upper gastrointestinal series (GI) with water-soluble ingested contrast material.
Based on clinical relevance and extent of dissemination [10, 11, 14], gastric leaks were classified as:
-
Type I (subclinical): Presence of leakage without early septic complications corresponding to drainage through a fistulous track and/or without generalized dissemination to the pleural or abdominal cavity with or without the appearance of contrast medium in any of the abdominal drains.
-
Type II (clinical): Presence of leakage with early septic complications corresponding to drainage by an irregular pathway (no well-formed fistulous tract) and a more generalized dissemination into the pleural or abdominal cavity with or without appearance of contrast medium in any of the abdominal drains.
Based on the detection time [10, 11], leaks were classified as:
-
i.
Early (leaks detected 1–3 days after LSG)
-
ii.
Intermediate (leaks detected 4–7 days after LSG)
-
iii.
Late (leaks detected ≥ 8 days after LSG)
Endoscopic stent placement technique
Endoscopic stent placement was performed by two experienced gastroenterologists which were qualified by the Hospital Institutional Board to undertake such interventional procedures. No differences in clinical experience of both practitioners could be identified and both performed a variety of other interventional endoscopic procedures.
Group A patients underwent an upper GI endoscopy in order to evaluate the location and the size of the leak. Radiopaque markers were then placed under fluoroscopic control to outline the proximal and distal extension of the stent. An ultra-stiff guide wire was subsequently placed into the gastric antrum and then a 30-mm diameter/24 or 21 cm in length, silicone coated, self-expanding metal stent (HANAROSTENT® BARIATRIC SURGERY CCC, MI Tech. Co. Ltd., Kr) was deployed over this, positioned between the radiopaque markers. The choice of the stent type was based on the attending endoscopists’ choice. Subsequently, at the completion endoscopy, the endoscopist decided on the correct placement of the stent.
Finally, either laparoscopic or percutaneous drainage of the abdominal fluid collections completed the treatment plan. All endoscopically treated patients proceeded to early feeding with liquids on the 3rd postprocedural day as soon as the nausea and possible vomiting has substantially subsided. Adverse events of endoscopic stenting were analysed and classified according to the American Society of Gastrointestinal Endoscopy definitions as follows:
-
i.
Mild—The procedure was aborted due to an adverse event.
-
Events requiring medical consultation after the procedure or extended hospital admission (≤ 3 nights).
-
-
ii.
Moderate—Unplanned ventilatory support.
-
Extended ward (4–10 nights) or ICU (1 night) admission.
-
Need for blood transfusion.
-
Events mandating interventional radiology or repeat endoscopy.
-
-
iii.
Severe—Extended ward (> 10 nights) or ICU (> 1 night) admission. Events requiring surgical intervention.
-
Residual permanent disability.
-
-
iv.
Fatal—Death
Definition of success/failure management
Success of management was defined as complete resolution of clinical and laboratory manifestations of sepsis with radiological evidence of localized, sealed, or absent extravasation of dye outside the digestive tract on imaging. The management was deemed a failure when there is persistence of:
-
i.
positive clinical signs (fever, tachycardia, abdominal pain, hemodynamic instability) and
-
ii.
laboratory markers of inflammation.
Statistical analysis
Statistical analysis was performed using descriptive statistics, independent samples t-test for comparison of variables between groups and crosstabs for comparison of groups with categorical variables. Chi-square test with the Yate’s correction or the Fisher’s exact test and Mann–Whitney U test were also used, whenever appropriate. Linear regression analysis was used for intragroup variables. The cut-off for statistical significance was defined as p < 0.05. The statistical package used was IBM SPSS Statistics for Windows, version 25.0 (IBM Corp., Armonk, NY, USA).
Results
From January 2007 to August 2020, 1371 morbidly obese patients were treated with laparoscopic sleeve gastrectomy in a tertiary care Academic Bariatric Centre in Athens, Greece.
Gastric staple line leak was detected in 27 patients: 19 females (70.4%) and 8 males (29.6%) with median age 44.78 years (range: 36–58 years) and median preoperative BMI 43.5 kg/m2 (range: 37.0–48.7 kg/m2). The overall leak rate was 1.9%. Most leaks were clinically significant (25 patients — 92.6%: type II — clinical leaks) versus two cases, which were detected remotely (postoperative days: 180 and 710 respectively: type I — subclinical leaks). From those 25 patients with clinically significant leaks, the detection day occurred at mean 5.8 days postoperatively (range: 1–12) (Fig. 1). Grouping of leak detection days revealed that, early leaks (leaks detected between days 1 and 3 postop) occurred in 8 patients, intermediate leaks (leaks detected between days 4 and 7) in 9 patients and late leaks (leaks detected after the 8th postoperative day) in 10 patients, including 2 patients with subclinical leaks (Fig. 2). Eight patients were treated by endoscopic stent placement (group A), whereas 19 patients (group B) were treated without stents (Table 1).
Clinical presentation
Most patients (8 out of 8 patients from group A and 18 out of 19 from group B) presented with abdominal pain. Similarly, the majority (17/19 from group A and 7/9 from group B) exhibited tachycardia > 90 pulses/min. However, only 3 patients of group A and 6 patients from group B had systolic blood pressure < 10 mmHg. Overall qSOFA scores for both treatment groups at admission are presented in Table 2. Interestingly, only one patient of group B was found to have qSOFA score 2, whereas most patients of the series exhibited low scores and no mental alteration status. All patients from both groups had leukocutosis (WBC > 12,000/ mm3, whereas fever > 38.2 °C was found in 2 patients of group A and 6 patients of group B. No mortalities were encountered in this series.
Imaging studies
Detailed imaging findings at patient presentation are shown in Table 3. Six patients (75%) of the stenting group and 16 patients (84.2%) of the non-stenting group presented with peri-gastric fluid collection, which comprised the most common imaging feature of gastric leak in this series (p = 1.04). Interestingly, 3 patients of the former group (37.5%) and 6 patients of the latter (31.5%) exhibited oral contrast leak (p = 0.98), whereas only one patient of the non-stenting group had gas-only leak.
Leak location and size
All leaks of both groups occurred in the upper part of the staple line and near the oesophagogastric junction. Leak size was measured only for group A patients (Table 3), since upper endoscopy was performed as a part of the stenting approach and was not included in the non-stenting treatment protocol. However, data retrieval allowed for leak size estimation in only 2 patients of this group.
Group A (endoscopic stent placement) — treatment results
None of these patients had previous bariatric operation. Eight silicone coated, self-expanding metal stents (HANAROSTENT® BARIATRIC SURGERY CCC, MI Tech. Co. Ltd, Kr) were placed in this group of patients. These were specifically designed metallic stents suitable for use in bariatric surgery and had 30-mm diameter and 24 or 21 cm in length. The placement protocol included a completion endoscopy to verify the full coverage of the gastric leak defect. Overall, the mean hospital stay for this group was 41.2 days (range: 24–60, SD: 4.8) and the mean time of leakage resolution as per definition was 42.4 days (range 25–60, SD: 13.7). Two patients (25%) exhibited complete resolution of the leak without any other intervention (Fig. 3). Three patients showed hemodynamic instability due to signs of ongoing sepsis at 5, 5- and 4-day poststent placement and at 15, 19- and 24-day postLSG accordingly. All of them underwent completion gastrectomy. In the rest 3 patients of this group, stent removal was eventually deemed necessary for all and a conservative treatment was instituted with drains left in place and kept until drainage of fluid finally ceased. More analytically, in one patient, a gastro-cutaneous fistula occurred, which was treated by endoscopic application of Histo-Acryl glue 45-day poststent placement and percutaneous drainage. Another patient was treated with gastrostomy and percutaneous drains placement, whereas in the last patient, two attempts of stent placement were done, the second one performed due to stent migration, consisting a case of stent migration encountered in this series. However, due to ongoing leakage and concurrent signs of sepsis, a laparoscopic peritoneal lavage and drainage was eventually attained.
Group B (non-stenting treatment) — treatment results
Nineteen patients were treated according to a non-stenting protocol. This included drains placement, administration of intravenous fluids and broad-spectrum antibiotics as well as total parenteral nutrition institution. Four of them had previous bariatric operation: two had gastric band and the other two had gastric plication in the past. The overall mean hospital stay for this group was 15 days (range: 12–18, SD: 0.43) and the mean time for leak resolution 34.5 days (range: 28–40, SD: 3.77) (Table 4). Four patients needed reoperation; one patient with early type leak was brought to the operating room on the 1st postoperative day, whereas in the rest 3 patients whom failed to respond to the conservative measures as per protocol, an operative approach was ultimately deemed necessary.
Comparison between treatment groups
Comparison between treatment groups revealed statistically significant differences in all primary outcome measures in favour of patients treated with non-stenting measures: the overall hospital stay (p < 0.001), the overall leakage resolution time (p = 0.025) and the incidence of operative interventions (p = 0.037).
More specifically, the mean hospital stay for group A was 41.2 days (range: 24–60) versus 15 days (range: 12–18) for group B (p < 0.001). Accordingly, complete leakage resolution was observed at mean 42.4 days (range 25–60) for group A and 34.5 days (range: 28–40) for group B patients (p = 0.025).
Overall, 5 patients (62.5%) of the stenting group A ultimately needed operative intervention versus 4 patients of group B (21.1%). In the same stent placement group, only 2 out of 8 patients eventually managed to accomplish complete leak resolution without any other intervention (p = 0.037). Furthermore, one patient of this group presented stent migration that needed further treatment modification with endoscopic and ultimately laparoscopic intervention. Running a univariate analysis within the group B patients that showed the best treatment outcomes, no significant correlation of the main outcome measures with the descriptive characteristics of the patients was found, especially with age or BMI stratification (p = 0.681 and p = 0.682 respectively).
Discussion
The optimal management approach to treat staple line leaks has been a subject of intense research in the current bariatric literature. Attempts to standardize the management approach for staple line leaks have implicated the time of onset and the clinical presentation of the leak as serious predictors [10, 11]. For early leaks with hemodynamic instability, surgical intervention seems appropriate to provide adequate drainage and source control, whereas in intermediate and late leaks, there is uncertainty concerning the best management algorithm. In this study, the superiority of the non-stenting versus the endoscopic stenting for the management of gastric staple line leaks after laparoscopic sleeve gastrectomy has been a key finding.
The incidence of gastric leak in this series was found to be 1.9%, ranking within literature rates, which vary between < 1 and 5.7% [15, 16]. Interestingly, more recent data have shown that gastric leak incidence has declined to 0.28%, which is in stark contrast from data that date back to the beginning of the past decade [17]. Endoscopic stent placement extrapolated from the treatment of foregut strictures and malignant perforations to the management of leaks after bariatric surgery, has been instituted during the middle of the previous decade and gained increased popularity thereafter [18, 19]. We applied this new treatment option early on; however, treatment outcomes were hampered by several moderate and severe adverse events and admittedly gradually fell out of preference. This justifies the marked discrepancy in size of the two groups presented at this study. Even though this may potentially be a source of bias, the superiority of the non-stenting approach was obvious for every primary outcome of this study. Only two out of 8 patients with stent placement (25%) accomplished complete resolution of the leak without any additional intervention, whereas the rest presented moderate or severe adverse events. Consequently, the overall hospital stay and time to complete leak resolution differ in a significantly statistical way in favour of the non-stenting treatment; patients of this group had shorter hospital stay, because stent placement patients needed various additional endoscopic or operative procedures during the treatment course. More specifically, stent placement was associated with high incidence of operative management later, as 5 out of 8 patients (62.5%) of this group ultimately resorted to an operative intervention (Fig. 3).
Of significant note, all group A patients had LSG as the index operation, whereas the non-stenting group included 4 patients with prior bariatric operations (gastric banding in 2 and gastric plication in the other two patients). Conversion of a gastric band to LSG has been described as a contributing factor to gastric leak development [20]. Interestingly, despite using long (24 cm in two patients and 21 cm in one patient) and wide stents (30-mm diameter), one patient presented with stent migration distally into the antrum requiring further invasive treatment. Stent migration has been the most frequent poststenting complication and recent efforts have concentrated into the design of stents able to accommodate the bariatric anatomy with wider diameter, longer shafts, coverage of the metal component and anti-migration flanges with variable degrees of flexibility [21]. However, stent migration remains a serious adverse event that requires further interventional measures.
Non-stenting management in this series led to leak closure in all patients at mean 34 days. Therefore, our treatment algorithm initially includes intense efforts for adequate source control which is accomplished with ample drainage of the leak using drains placed either by radiology interventional or laparoscopic means. Thereafter, the patient follows a strict protocol including iv fluids, antibiotics and total parenteral nutrition administration. Further patient management focuses on monitoring patient’s vital signs (fever, tachycardia and blood pressure) and leakage output. Antibiotics are stopped as soon as the patient is afebrile and clinically stable. Thereafter, antibiotic discontinuation as soon as the patient remains afebrile for 3 days is followed by gradual oral feeding institution and subsequently patient discharge after 3 more days of uneventful course. The patient can be safely discharged home carrying the drain/s, which are monitored until complete drainage resolution. The patient is then followed up closely for 1 year to establish the definitive leak closure.
The limitations of this study arise from its non-randomized, retrospective/observational methodology. Accordingly, patients’ assignment between the two different treatment groups was based on surgeon’s preference. Using several stent types in the same cohort may be another source of bias. Additionally, various other endoscopic techniques do exist, such as the double pig tail, the endovacuum system or over-the scope clips (OTCS’s) which may have a more favourable adverse event profile [22,23,24]. However, the stenting method attained in this series was the only one offered in our Institution and consists a valid and extensively described option in the literature. This clinical study, also, encompasses a large sample of patients treated with LSG in an Academic Bariatric Centre over a 13-year period with a standardized operative technique and demographically comparable treatment groups after gastric leak detection.
Conclusion
Non-stenting approach has become the mainstay of treatment for patients with gastric staple line leak after LSG in our Institution. Endoscopic stent placement after a 13-year application timeline was associated with moderate and severe adverse events that gradually questioned its real value in this setting.
Availability of data and material
Authors, Andreas Kiriakopoulos MD, Nefeli Kounatidis MS, Menenakos Ilias, Kostrova Maria MD, Zografos Konstantinos MD, Evangelos Menenakos MD, declare that the data of the study are available upon reasonable request.
Code availability
Authors, Andreas Kiriakopoulos MD, Nefeli Kounatidis MS, Menenakos Ilias, Kostrova Maria MD, Zografos Konstantinos MD, Evangelos Menenakos MD, declare that all software applications are available upon reasonable request.
References
Angrisani L, Santonicola A, Iovino P et al (2018) IFSO worldwide survey 2016: primary, endoluminal, and revisional procedures. Obes Surg 28:3783–3794. https://doi.org/10.1007/s11695-018-3450-2
Salman MA, El-Ghobary M, Soliman A et al (2020) Long-term changes in leptin, chemerin, and ghrelin levels following Roux-en-Y gastric bypass and laparoscopic sleeve gastrectomy. Obes Surg 30(3):1052–1060. https://doi.org/10.1007/s11695-019-04254-z
Kalinowski P, Paluszkiewicz R, Wróblewski T, Remiszewski P, Grodzicki M, Bartoszewicz Z, Krawczyk M (2017) Ghrelin, leptin, and glycemic control after sleeve gastrectomy versus Roux-en-Y gastric bypass-results of a randomized clinical trial. Surg Obes Relat Dis 13(2):181–188. https://doi.org/10.1016/j.soard.2016.08.025201618
Gagner M, Hutchinson C, Rosenthal R (2016) Fifth International Consensus Conference: current status of sleeve gastrectomy. Surg Obes Relat Dis 12(4):750–756. https://doi.org/10.1016/j.soard.2016.01.022
McTigue KM, Wellman R, Nauman E, Anau J, Coley RY, Odor A et al (2020) Comparing the 5-year diabetes outcomes of sleeve gastrectomy and gastric bypass: the National Patient-Centered Clinical Research Network (PCORNet) Bariatric Study. JAMA Surg 155(5):e200087. https://doi.org/10.1001/jamasurg.2020.0087
Kichler K, Rosenthal RJ, DeMaria E, Higa K (2019) Reoperative surgery for non-responders and complicated sleeve gastrectomy operations in patients with severe obesity. An international expert panel consensus statement to define best practice guidelines. Surg Obes Relat Dis 15(2):173–186. https://doi.org/10.1016/j.soard.2018.11.006
Gagner M, Buchwald JN (2014) Comparison of laparoscopic sleeve gastrectomy leak rates in four staple-line reinforcement options: a systematic review. Surg Obes Relat Dis 10(4):713–723. https://doi.org/10.1016/j.soard.2014.01.016
Chen B, Kiriakopoulos A, Tsakayannis D, Wachtel MS, Linos D, Frezza EE (2009) Reinforcement does not necessarily reduce the rate of staple line leaks after sleeve gastrectomy. A review of the literature and clinical experiences. Obes Surg 19(2):166–172. https://doi.org/10.1007/s11695-008-9668-7
Nedelcu M, Skalli M, Delhom E, Fabre J, Nocca D (2013) New CT scan classification of leak after sleeve gastrectomy. Obes Surg 23(8):1341–1343
Csendes A, Burdiles P, Burgos AM, Maluenda F, Diaz JC (2005) Conservative management of anastomotic leaks after 557 open gastric bypasses. Obes Surg 15:1252–1256
Burgos AM, Braghetto I, Csendes A, Maluenda F, Korn O, Yarmuch J et al (2009) Gastric leak after laparoscopic-sleeve gastrectomy for obesity. Obes Surg 19:1672–7
Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M, Bellomo R, Bernard GR, Chiche JD, Coopersmith CM, Hotchkiss RS, Levy MM, Marshall JC, Martin GS, Opal SM, Rubenfeld GD, van der Poll T, Vincent JL, Angus DC (2016) The third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA 315(8):801–810. https://doi.org/10.1001/jama.2016.0287
Bhattacharjee P, Edelson DP, Churpek MM (2017) Identifying patients with sepsis on the hospital wards. Chest 151(4):898–907. https://doi.org/10.1016/j.chest.2016.06.020
Abou Rached A, Basile M, El Masri H (2014) Gastric leaks post sleeve gastrectomy: review of its prevention and management. World J Gastroenterol 20(38):13904–13910. https://doi.org/10.3748/wjg.v20.i38.13904
Berger ER, Clements RH, Morton JM, Huffman KM, Wolfe BM, Nguyen NT et al (2016) The impact of different surgical techniques on outcomes in laparoscopic sleeve gastrectomies: the first report from the metabolic and bariatric surgery accreditation and quality improvement program (MBSAQIP). Ann Surg 264:464–73
Stroh C, Köckerling F, Volker L, Frank B, Stefanie W, Christian K et al (2016) Results of more than 11,800 sleeve gastrectomies: data analysis of the German Bariatric Surgery Registry. Ann Surg 263:949–955
Yolsuriyanwong K, Ingviya T, Kongkamol C, Marcotte E, Chand B (2019) Effects of intraoperative leak testing on postoperative leak-related outcomes after primary bariatric surgery: an analysis of the MBSAQIP database. Surg Obes Relat Dis 15(9):1530–1540. https://doi.org/10.1016/j.soard.2019.06.008
Mumtaz H, BaroneGW KBL et al (2002) Successful management of a non-malignant esophageal perforation with a coated stent. Ann Thorac Surg 74:1233–1235
Salinas A, Baptista A, Santiago E et al (2006) Self-expandable metal stents to treat gastric leaks. Surg Obes Relat Dis 2:570–572
Iannelli A, Schneck AS, Ragot E, Liagre A, Anduze Y, Msika S et al (2009) Laparoscopic sleeve gastrectomy as revisional procedure for failed gastric banding and vertical banded gastroplasty. Obes Surg 19:1216–1220
Shehab H (2018) Enteral stents in the management of post-bariatric surgery leaks. Surg Obes Relat Dis 14(3):393–403
Swinnen J, Eisendrath P, Rigaux J, Kahegeshe L, Lemmers A, Le Moine O, Devière J (2011) Self-expandable metal stents for the treatment of benign upper GI leaks and perforations. Gastrointest Endosc 73(5):890–899. https://doi.org/10.1016/j.gie.2010.12.019
Schiesser M, Kressig P, Bueter M, Nocito A, Bauerfeind P, Gubler C (2014) Successful endoscopic management of gastrointestinal leakages after laparoscopic Roux-en-Y gastric bypass surgery. Dig Surg 31(1):67–70. https://doi.org/10.1159/000358849
Morell B, Murray F, Vetter D et al (2019) Endoscopic vacuum therapy (EVT) for early infradiaphragmal leakage after bariatric surgery—outcomes of six consecutive cases in a single institution. Langenbecks Arch Surg 404:115–121. https://doi.org/10.1007/s00423-019-01750-9
Acknowledgements
We, authors: Andreas Kiriakopoulos MD, Nefeli Kounatidis MS, Menenakos Ilias, Kostrova Maria MD, Zografos Konstantinos MD, Evangelos Menenakos MD, declare that no other personal assistance has taken place in creating this work.
Author information
Authors and Affiliations
Contributions
Andreas Kiriakopoulos: study conception and design, analysis and interpretation of data, drafting of manuscript, critical revision of manuscript. Nefeli Kounatidis: acquisition of data, drafting of manuscript. Menenakos Ilias: study conception and design, acquisition of data, analysis and interpretation of data. Kostrova Maria: study conception and design, acquisition of data, drafting of manuscript. Zografos Konstantinos: acquisition of data, drafting of manuscript, critical revision of manuscript. Menenakos Evangelos: study conception and design, acquisition of data, analysis and interpretation of data, drafting of manuscript, critical revision of manuscript.
Corresponding author
Ethics declarations
Consent to participate
Authors, Andreas Kiriakopoulos MD, Nefeli Kounatidis MS, Menenakos Ilias, Kostrova Maria MD, Zografos Konstantinos MD, Evangelos Menenakos MD, declare that all participants have consent to this research study.
Consent to publication
Authors, Andreas Kiriakopoulos MD, Nefeli Kounatidis MS, Menenakos Ilias, Kostrova Maria MD, Zografos Konstantinos MD, Evangelos Menenakos MD, declare that we consent to the publication of our research study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kiriakopoulos, A., Kounatidis, N., Menenakos, I. et al. Non-stenting treatment versus endoscopic stent placement in staple line leaks after laparoscopic sleeve gastrectomy. Langenbecks Arch Surg 407, 1863–1872 (2022). https://doi.org/10.1007/s00423-022-02498-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-022-02498-5