Abstract
Purpose
Immunonutritional status is a known prognostic correlate in the context of gastric cancer (GC). In the present study, we investigated the prognostic relevance of a lipid profile-based immunonutritional score in patients with GC.
Methods
Data pertaining to 224 patients with stage II and III GC who underwent curative gastrectomy were retrospectively analyzed. The total cholesterol-lymphocyte score (TL score) was defined as follows: patients with both low total cholesterol (TC) and total lymphocyte count were allocated a score of 2; patients with only one or none of these biochemical abnormalities were allocated a score of 1 or 0, respectively.
Results
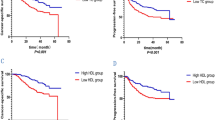
Among the serum lipid indices, low TC was the strongest predictor of cancer-specific survival (CSS; p = 0.001). On multivariate analysis, both low prognostic nutritional index (PNI) (p < 0.001) and high TL score (p = 0.003) were independent prognostic factors. PNI was significantly associated with peritoneal recurrence (p = 0.047), while TL score was significantly associated with locoregional and distant metastasis (p = 0.004 and p = 0.003, respectively).
Conclusions
TL score may facilitate risk stratification of patients based on CSS. TL score plus PNI may help predict the recurrence pattern in patients with stage II and III GC.




Similar content being viewed by others
References
Ferlay J, Soerjomataram I, Dikshit R, Eser S et al (2015) Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 136:E359–E386
Heys SD, Park KG, Garlick PJ et al (1992) Nutrition and malignant disease: implications for surgical practice. Br J Surg 79:614–623
Miyata H, Yano M, Yasuda T et al (2012) Randomized study of clinical effect of enteral nutrition support during neoadjuvant chemotherapy on chemotherapy-related toxicity in patients with esophageal cancer. Clin Nutr 31:330–336
Heys SD, Park KG, Garlick PJ et al (1992) Nutrition and malignant disease: implications for surgical practice. Br J Surg 79(7):614–623
Ogino S, Galon J, Fuchs CS et al (2011) Cancer immunology--analysis of host and tumor factors for personalized medicine. Nat Rev Clin Oncol 9;8(12):711–719. https://doi.org/10.1038/nrclinonc.2011.122
Pinato DJ, North BV, Sharma R et al (2012) A novel, externally validated inflammation-based prognostic algorithm in hepatocellular carcinoma: the prognostic nutritional index (PNI). Br J Cancer 106:1439–1445
Yang Y, Gao P, Song Y et al (2016) The prognostic nutritional index is a predictive indicator of prognosis and postoperative complications in gastric cancer: A meta-analysis. Eur J Surg Oncol 42(8):1176–1182. https://doi.org/10.1016/j.ejso.2016.05.029 Epub 2016 Jun 1
Jiang SS, Weng DS, Jiang L et al (2016) The clinical significance of preoperative serum cholesterol and high-density lipoprotein-cholesterol levels in hepatocellular carcinoma. J Cancer 20;7(6):626–632. https://doi.org/10.7150/jca.13837 eCollection 2016
Hao B, Bi B, Sang C et al (2019) Systematic review and meta-analysis of the prognostic value of serum high-density lipoprotein cholesterol levels for solid tumors. Nutr Cancer 15:1–10. https://doi.org/10.1080/01635581.2019.1577983
Wettstein MS, Saba K, Umbehr MH et al (2017) Prognostic role of preoperative serum lipid levels in patients undergoing radical prostatectomy for clinically localized prostate cancer. Prostate. 77(5):549–556. https://doi.org/10.1002/pros.23296 Epub 2017 Jan 17
Liu BZ, Tao L, Chen YZ et al (2016) Preoperative body mass index, blood albumin and triglycerides predict survival for patients with gastric cancer. PLoS One 16;11(6):e0157401. https://doi.org/10.1371/journal.pone.0157401 eCollection 2016
Toyokawa T, Kubo N, Tamura T et al (2016) The pretreatment Controlling Nutritional Status (CONUT) score is an independent prognostic factor in patients with resectable thoracic esophageal squamous cell carcinoma: results from a retrospective study. BMC Cancer 6(16):722. https://doi.org/10.1186/s12885-016-2696-0
Ryo S, Kanda M, Ito S et al (2019) The Controlling Nutritional Status score serves as a predictor of short- and long-term outcomes for patients with stage 2 or 3 gastric cancer: analysis of a multi-institutional data set. Ann Surg Oncol 26(2):456–464. https://doi.org/10.1245/s10434-018-07121-w Epub 2018 Dec 18
Kuroda D, Sawayama H, Kurashige J et al (2018) Controlling Nutritional Status (CONUT) score is a prognostic marker for gastric cancer patients after curative resection. Gastric Cancer 21(2):204–212. https://doi.org/10.1007/s10120-017-0744-3 Epub 2017 Jun 27
Japanese Gastric Cancer Association 2014. Japanese Gastric Cancer Treatment Guidelines 2014 (version 4). Tokyo
Brierley JD, Gospodarowicz MK, Wittekind C (2017) editors. Union for International Cancer Control. TNM Classification of Malignant Tumors. 8th ed. Wiley, New York
Japanese Gastric Cancer Association (2011) Japanese classification of gastric carcinoma: 3rd English edition. Gastric Cancer 14:101–112 [PMID: 21573743. https://doi.org/10.1007/s10120-011-0041-5
Onodera T, Goseki N, Kosaki G (1984) Prognostic nutritional index in gastrointestinal surgery of malnourished cancer patients [in Japanese]. Nippon Geka Gakkai Zasshi 85:1001–1005
Ignacio de Ulíbarri J, González-Madroño A, de Villar NG et al (2005) CONUT: a tool for controlling nutritional status. First validation in a hospital population. Nutr Hosp Jan-Feb 20(1):38–45
Altman DG, Lausen B, Sauerbrei W et al (1994) Dangers of using “optimal” cutpoints in the evaluation of prognostic factors. J Natl Cancer Inst 86:829–835
Gadgil MD, Anderson CA, Kandula NR et al (2015) Dietary patterns are associated with metabolic risk factors in South Asians living in the United States. J Nutr. Jun 145(6):1211–1217. https://doi.org/10.3945/jn.114.207753 Epub 2015 Apr 22
Calleros L, Lasa M, Toro MJ et al (2006) Low cell cholesterol levels increase NFkappaB activity through a p38 MAPK-dependent mechanism. Cell Signal 18(12):2292–2301 Epub 2006 Jun 27
Wang Y, Sun XQ, Lin HC et al (2019) Correlation between immune signature and high-density lipoprotein cholesterol level in stage II/III colorectal cancer. Cancer Med 8(3):1209–1217. https://doi.org/10.1002/cam4.1987 Epub 2019 Feb 7
Chen P, Han L, Wang C et al (2017) Preoperative serum lipids as prognostic predictors in esophageal squamous cell carcinoma patients with esophagectomy. Oncotarget 20;8(25):41605–41619. https://doi.org/10.18632/oncotarget.15651
Zhou P, Li B, Liu B et al (2018) Prognostic role of serum total cholesterol and high-density lipoprotein cholesterol in cancer survivors: A systematic review and meta-analysis. Clin Chim Acta 477:94–104. https://doi.org/10.1016/j.cca.2017.11.039 Epub 2017 Dec 6
Li X, Tang H, Wang J et al (2017) The effect of preoperative serum triglycerides and high-density lipoprotein-cholesterol levels on the prognosis of breast cancer. Breast 32:1–6. https://doi.org/10.1016/j.breast.2016.11.024 Epub 2016 Dec 8
Liao F, He W, Jiang C et al (2015) A high LDL-C to HDL-C ratio predicts poor prognosis for initially metastatic colorectal cancer patients with elevations in LDL-C. Onco Targets Ther 27;8:3135–3142. https://doi.org/10.2147/OTT.S90479 eCollection 2015
Zhou T, Zhan J, Fang W et al (2017) Serum low-density lipoprotein and low-density lipoprotein expression level at diagnosis are favorable prognostic factors in patients with small-cell lung cancer (SCLC). BMC Cancer 14;17(1):269. https://doi.org/10.1186/s12885-017-3239-z
Lofterød T, Mortensen ES, Nalwoga H et al (2018) Impact of pre-diagnostic triglycerides and HDL-cholesterol on breast cancer recurrence and survival by breast cancer subtypes. BMC Cancer 15;18(1):654. https://doi.org/10.1186/s12885-018-4568-2
Guillaumond F, Bidaut G, Ouaissi M et al (2015) Cholesterol uptake disruption, in association with chemotherapy, is a promising combined metabolic therapy for pancreatic adenocarcinoma. Proc Natl Acad Sci U S A 24;112(8):2473–2478. https://doi.org/10.1073/pnas.1421601112 Epub 2015 Feb 9
Gallagher EJ, Zelenko Z, Neel BA et al (2017) Elevated tumor LDLR expression accelerates LDL cholesterol-mediated breast cancer growth in mouse models of hyperlipidemia. Oncogene 16;36(46):6462–6471. https://doi.org/10.1038/onc.2017.247 Epub 2017 Jul 31
Wang C, Li P, Xuan J et al (2017) Cholesterol enhances colorectal cancer progression via ROS elevation and MAPK signaling pathway activation. Cell Physiol Biochem 42(2):729–742. https://doi.org/10.1159/000477890 Epub 2017 Jun 15
Mantovani A, Allavena P, Sica A et al (2008) Cancer-related inflammation. Nature 24;454(7203):436–444. https://doi.org/10.1038/nature07205
Feng JF, Liu JS, Huang Y (2014) Lymphopenia predicts poor prognosis in patients with esophageal squamous cell carcinoma. Medicine (Baltimore) 93(27):e257. https://doi.org/10.1097/MD.0000000000000257
Ray-Coquard I, Cropet C, Van Glabbeke M et al (2009) Lymphopenia as a prognostic factor for overall survival in advanced carcinomas, sarcomas, and lymphomas. Cancer Res 1;69(13):5383–5391. https://doi.org/10.1158/0008-5472.CAN-08-3845 Epub 2009 Jun 23
Toyokawa T, Muguruma K, Tamura T et al (2018) Comparison of the prognostic impact and combination of preoperative inflammation-based and/or nutritional markers in patients with stage II gastric cancer. Oncotarget 29;9(50):29351–29364. https://doi.org/10.18632/oncotarget.25486 eCollection 2018 Jun 29
Saito H, Kono Y, Murakami Y, Kuroda H, Matsunaga T, Fukumoto Y, Osaki T (2017) Influence of prognostic nutritional index and tumor markers on survival in gastric cancer surgery patients. Langenbecks Arch Surg 402(3):501–507
Nam DH, Lee H, Park JC et al (2014) Long-term statin therapy improves oncological outcome after radical gastrectomy for stage II and III gastric cancer. Anticancer Res 34(1):355–361
Hatao F, Chen KY, Wu JM, Wang MY, Aikou S, Onoyama H, Shimizu N, Fukatsu K, Seto Y, Lin MT (2017) Randomized controlled clinical trial assessing the effects of oral nutritional supplements in postoperative gastric cancer patients. Langenbecks Arch Surg 402(2):203–211
Adiamah A, Skořepa P, Weimann A, Lobo DN (2019) The impact of preoperative immune modulating nutrition on outcomes in patients undergoing surgery for gastrointestinal cancer: a systematic review and meta-analysis. Ann Surg doi. https://doi.org/10.1097/SLA.0000000000003256
Giger U, Büchler M, Farhadi J, Berger D, Hüsler J, Schneider H, Krähenbühl S, Krähenbühl L (2007) Preoperative immunonutrition suppresses perioperative inflammatory response in patients with major abdominal surgery-a randomized controlled pilot study. Ann Surg Oncol 14(10):2798–2806 Epub 2007 Jul 15
Ding D, Feng Y, Song B, Gao S, Zhao J (2015) Effects of preoperative and postoperative enteral nutrition on postoperative nutritional status and immune function of gastric cancer patients. Turk J Gastroenterol 26(2):181–185. https://doi.org/10.5152/tjg.2
Author information
Authors and Affiliations
Contributions
This study was designed by D.M., K.S., T.K., and E.O.; D.M. and K.S. performed statistical analyses. The clinical information and materials were collected and kept by K.S., T.K., T.K., H.K., A.S., H.F., K.O., T.A., M.K., R.M., Y.M., H.I., Y.K., and M.N.; D.M. and K.S. drafted the manuscript. T.K. edited and revised the manuscript. E.O. approved the final version of manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 16.7 kb)
Rights and permissions
About this article
Cite this article
Matsubara, D., Shoda, K., Kubota, T. et al. Preoperative total cholesterol-lymphocyte score as a novel immunonutritional predictor of survival in gastric cancer. Langenbecks Arch Surg 404, 743–752 (2019). https://doi.org/10.1007/s00423-019-01824-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-019-01824-8