Abstract
Purpose
To examine the effect of high-intensity interval work (HIIW) and moderate-intensity continuous work (MICW) on markers of acute kidney injury (AKI) and kidney function in a hot environment.
Methods
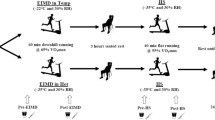
Nine males completed 2 h of work (2 × 60 min with 10 min passive rest) in a hot environment (40 °C and 15% relative humidity) as either HIIW [2 min at 80% peak oxygen consumption (VO2peak) and 3 min at 30% VO2peak] or MICW (matched for total work of HIIW). Blood and urine samples were collected immediately before (Pre), after (Post), 1 h (1 h Post), and 24 h after (24 h Post) the trials. Urine flow rate (UFR), creatinine clearance, insulin-like growth factor binding protein 7 (IGFBP7), urinary neutrophil gelatinase-associated lipocalin (uNGAL), and urinary kidney injury marker 1 (uKIM-1) were measured to assess kidney function and injury.
Results
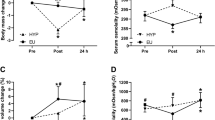
Log IGFBP7 (p < 0.01), log uNGAL (p < 0.01), and log uKIM-1 (p = 0.01) all displayed a main effect for time after both HIIW and MICW. IGFBP7 (p = 0.01) and uKIM-1 (p < 0.01), corrected for Uosm, were higher after HIIW compared to MICW at Post, while IGFBP7 was also higher 1 h Post after HIIW compared to MICW (p = 0.02). UFR significantly decreasing from Pre to Post (p < 0.01) and 1 h Post (p < 0.01), but no main effect for condition (p = 0.53).
Conclusion
Both HIIW and MICW in a hot environment caused an increase in biomarkers of kidney injury (IGFBP7, KIM-1, and NGAL), but HIIW may have a greater impact on biomarkers related to AKI.






Similar content being viewed by others

Abbreviations
- ηp 2 :
-
Partial eta-squared
- AKI:
-
Acute kidney injury
- eGFR:
-
Estimated glomerular filtration rate
- GFR:
-
Glomerular filtration rate
- Hct:
-
Hematocrit
- HR:
-
Heart rate
- IGFBP7:
-
Insulin-like growth factor binding protein 7
- KIM-1:
-
Kidney injury marker 1
- NGAL:
-
Neutrophil gelatinase-associated lipocalin
- Posm:
-
Plasma osmolality
- PV:
-
Plasma volume
- RH:
-
Relative humidity
- RPE:
-
Rating of perceived exertion
- Tc:
-
Core temperature
- TS:
-
Thermal stress
- UFR:
-
Urine flow rate
- Uosm:
-
Urine osmolality
References
American College of Sports Medicine (2018) ACSM’s for exercise guidelines testing and prescription, 10th edn. Lippincott Williams & Wilkins, Philadelphia, PA
American College of Sports Medicine, Sawka MN, Burke LM et al (2007) American college of sports Medicine position stand. Exercise and fluid replacement. Med Sci Sports Exerc 39:377–390. https://doi.org/10.1249/mss.0b013e31802ca597
Barclay J, Cooke W, Kenney R, Nutt ME (1947) The effects of water diuresis and exercise on the volume and composition of the urine. Am J Physiol 148(2):327–337
Bie P (1980) Osmoreceptors, vasopressin, and control of renal water excretion. Physiol Rev 60:961–1048. https://doi.org/10.1152/physrev.1980.60.4.961
Bongers CCWG, Alsady M, Nijenhuis T et al (2018) Impact of acute versus prolonged exercise and dehydration on kidney function and injury. Physiol Rep 6:e13734. https://doi.org/10.14814/phy2.13734
Borg GA (1982) Psychophysical bases of perceived exertion. Med Sci Sports Exerc 14:377–381
Chapman CL, Johnson BD, Sackett JR et al (2019) Soft drink consumption during and following exercise in the heat elevates biomarkers of acute kidney injury. Am J Physiol Regul Integr Comp Physiol 316:R189–R198. https://doi.org/10.1152/ajpregu.00351.2018
Chapman CL, Johnson BD, Parker MD et al (2020a) Kidney physiology and pathophysiology during heat stress and the modification by exercise, dehydration, heat acclimation and aging. Temperature 8:108–159. https://doi.org/10.1080/23328940.2020.1826841
Chapman CL, Johnson BD, Vargas NT et al (2020b) Both hyperthermia and dehydration during physical work in the heat contribute to the risk of acute kidney injury. J Appl Physiol 128:715–728. https://doi.org/10.1152/japplphysiol.00787.2019
Chatauret N, Badet L, Barrou B, Hauet T (2014) Ischemia-reperfusion: from cell biology to acute kidney injury. Prog Urol 24:S4–S12. https://doi.org/10.1016/S1166-7087(14)70057-0
Devarajan P (2006) Update on mechanisms of ischemic acute kidney injury. J Am Soc Nephrol 17:1503–1520. https://doi.org/10.1681/ASN.2006010017
Dill DB, Costill DL (1974) Calculation of percentage changes in volumes of blood, plasma, and red cells in dehydration. J Appl Physiol 37:247–248. https://doi.org/10.1152/jappl.1974.37.2.247
Emlet DR, Pastor-Soler N, Marciszyn A, Wen X, Gomez H, Humphries WH, Morrisroe S, Volpe JK, Kellum JA (2017) Insulin-like growth factor binding protein 7 and tissue inhibitor of metalloproteinases-2: differential expression and secretion in human kidney tubule cells. Am J Physiol Renal Physiol 312(2):F284–F296. https://doi.org/10.1152/ajprenal.00271.2016
Freund BJ, Shizuru EM, Hashiro GM, Claybaugh JR (1991) Hormonal, electrolyte, and renal responses to exercise are intensity dependent. J Appl Physiol 70:900–906. https://doi.org/10.1152/jappl.1991.70.2.900
Grimby G (1965) Renal clearances during prolonged supine exercise at different loads. J Appl Physiol 20:1294–1298. https://doi.org/10.1152/jappl.1965.20.6.1294
Hall C, Figueroa A, Fernhall B, Kanaley JA (2004) Energy expenditure of walking and running: comparison with prediction equations. Med Sci Sports Exerc 36:2128–2134. https://doi.org/10.1249/01.mss.0000147584.87788.0e
Ichimura T, Bonventre JV, Bailly V et al (1998) Kidney injury molecule-1 (KIM-1), a putative epithelial cell adhesion molecule containing a novel immunoglobulin domain, is up-regulated in renal cells after injury. J Biol Chem 273:4135–4142. https://doi.org/10.1074/jbc.273.7.4135
Jackson AS, Pollock ML (1978) Generalized equations for predicting body density of men. Br J Nutr 40:497–504. https://doi.org/10.1079/BJN19780152
Junglee NA, Lemmey AB, Burton M et al (2012) Does proteinuria-inducing physical activity increase biomarkers of acute kidney injury? Kidney Blood Press Res 36:278–289. https://doi.org/10.1159/000343417
Junglee NA, Di Felice U, Dolci A et al (2013) Exercising in a hot environment with muscle damage: effects on acute kidney injury biomarkers and kidney function. Am J Physiol Renal Physiol 305:F813–F820. https://doi.org/10.1152/ajprenal.00091.2013
Kawakami S, Yasuno T, Matsuda T et al (2018) Association between exercise intensity and renal blood flow evaluated using ultrasound echo. Clin Exp Nephrol 22:1061–1068. https://doi.org/10.1007/s10157-018-1559-1
Lipman GS, Krabak BJ, Rundell SD et al (2016) Incidence and prevalence of acute kidney injury during multistage ultramarathons. Clin J Sport Med 26:314–319. https://doi.org/10.1097/JSM.0000000000000253
Lipman GS, Shea K, Christensen M et al (2017) Ibuprofen versus placebo effect on acute kidney injury in ultramarathons: a randomised controlled trial. Emerg Med J 34:637–642. https://doi.org/10.1136/emermed-2016-206353
Mack GW, Nadel ER (2010) Body fluid balance during heat stress in humans. Handbook of physiology section 4, environmental physiology, vol 1. Oxford University Press for the American Physiological Society, New York, pp 187–214
Madero M, García-Arroyo FE, Sánchez-Lozada L-G (2017) Pathophysiologic insight into MesoAmerican nephropathy. Curr Opin Nephrol Hypertens 26:296–302. https://doi.org/10.1097/MNH.0000000000000331
Mansour SG, Martin TG, Obeid W et al (2019) The role of volume regulation and thermoregulation in AKI during marathon running. Clin J Am Soc Nephrol 14:1297–1305. https://doi.org/10.2215/CJN.01400219
Mehta RL, Kellum JA, Shah SV et al (2007) Acute kidney injury network: report of an initiative to improve outcomes in acute kidney injury. Crit Care 11:R31. https://doi.org/10.1186/cc5713
Moyce S, Mitchell D, Armitage T et al (2017) Heat strain, volume depletion and kidney function in California agricultural workers. Occup Environ Med 74:402–409. https://doi.org/10.1136/oemed-2016-103848
Moyce S, Armitage T, Mitchell D, Schenker M (2020) Acute kidney injury and workload in a sample of California agricultural workers. Am J Ind Med 63:258–268. https://doi.org/10.1002/ajim.23076
National Institute for Occupational Safety and Health (2016) NIOSH criteria for a recommended standard: occupational exposure to heat and hot environments. Cincinnati, OH.
Neugarten J, Golestaneh L (2022) Sex differences in acute kidney injury. Semin Nephrol 42:208–218. https://doi.org/10.1016/j.semnephrol.2022.04.010
Otani H, Kaya M, Tsujita J (2013) Effect of the volume of fluid ingested on urine concentrating ability during prolonged heavy exercise in a hot environment. J Sports Sci Med 12:197–204
Parikh CR, Coca SG (2010) Defining prerenal azotemia in clinical practice and research. Nat Rev Nephrol 6:641–642. https://doi.org/10.1038/nrneph.2010.128
Philippou A, Bogdanis G, Maridaki M et al (2009) Systemic cytokine response following exercise-induced muscle damage in humans. Clin Chem Lab Med 47:777–782. https://doi.org/10.1515/CCLM.2009.163
Pundee R, Kongtip P, Nankongnab N et al (2020) Cross-shift change of acute kidney injury biomarkers in sugarcane farmers and cutters. Hum Ecol Risk Assess Int J 27:1170–1187. https://doi.org/10.1080/10807039.2020.1812049
Radigan LR, Robinson S (1949) Effects of environmental heat stress and exercise on renal blood flow and filtration rate. J Appl Physiol 4:185–191
Schlader Z, Chapman C, Sarker S et al (2017) Firefighter work duration influences the extent of acute kidney injury. Med Sci Sports Exerc 49:1745–1753. https://doi.org/10.1249/mss.0000000000001254
Schlader ZJ, Hostler D, Parker MD et al (2019) The potential for renal injury elicited by physical work in the heat. Nutrients 11:2087. https://doi.org/10.3390/nu11092087
Schneider DA, McLellan TM, Gass GC (2000) Plasma catecholamine and blood lactate responses to incremental arm and leg exercise. Med Sci Sports Exerc 32:608–613. https://doi.org/10.1097/00005768-200003000-00009
Schrezenmeier EV, Barasch J, Budde K et al (2017) Biomarkers in acute kidney injury – pathophysiological basis and clinical performance. Acta Physiol 219:556–574. https://doi.org/10.1111/apha.12764
Smith J, Robinson S, Pearcy M (1952) Renal responses to exercise, heat and dehydration. J Appl Physiol 8:659–665
Tidgren B, Hjemdahl P, Theodorsson E, Nussberger J (1991) Renal neurohormonal and vascular responses to dynamic exercise in humans. J Appl Physiol 70:2279–2286. https://doi.org/10.1152/jappl.1991.70.5.2279
Virvidakis C, Loukas A, Mayopoulou-Symvoulidou D, Mountokalakis T (1986) Renal responses to bicycle exercise in trained athletes: influence of exercise intensity. Int J Sports Med 7:86–88. https://doi.org/10.1055/s-2008-1025739
Waikar SS, Sabbisetti VS, Bonventre JV (2010) Normalization of urinary biomarkers to creatinine during changes in glomerular filtration rate. Kidney Int 78:486–494. https://doi.org/10.1038/ki.2010.165
Funding
Partial funding for this study was provided by the Graduate and Professional Student Association and the Exercise Physiology Laboratory at the University of New Mexico.
Author information
Authors and Affiliations
Contributions
JH and FA conceived the experiment design. JH, ZM, ZF, JD, AW, and FA collected data. JH, ZM, FA, and JS analyzed the data. JH drafted the manuscript. All authors contributed to the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
None declared.
Ethical approval
This study was approved by the University of New Mexico Main Campus Institutional Review Board (protocol #1690849–3).
Additional information
Communicated by George Havenith.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Houck, J., McKenna, Z., Fennel, Z. et al. The effect of interval and continuous work on markers of acute kidney injury in a hot environment. Eur J Appl Physiol 122, 2437–2450 (2022). https://doi.org/10.1007/s00421-022-05030-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-022-05030-1