Abstract
Introduction
Reductions in fibrinolytic potential occur with both aging and physical inactivity and are associated with an increased cardiovascular disease risk. Plasmin, the enzyme responsible for the enzymatic degradation of fibrin clots, is activated by tissue plasminogen activator (tPA), while plasminogen activator inhibitor-1 (PAI-1) inhibits its activation. Currently, fibrinolysis research focuses almost exclusively on changes within the plasma. However, tPA and PAI-1 are expressed by human skeletal muscle (SM). Currently, no studies have focused on changes in SM fibrinolytic activity with regard to aging and aerobic fitness.
Purpose
The purpose of this study was to cross-sectionally evaluate effects of age and aerobic fitness on tPA and PAI-1 expressions and activity in SM.
Methods
Twenty-six male subjects were categorized into the following groups: (1) young aerobically trained (n = 8); (2) older aerobically trained (n = 6); (3) young aerobically untrained (n = 7); and (4) older aerobically untrained (n = 5). Muscle biopsies were obtained from each subject. SM tPA activity was assessed using gel zymography and SM tPA and PAI-1 expressions were assessed using RT-PCR.
Results
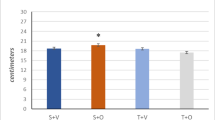
Trained subjects had higher SM tPA activity compared to untrained (25.3 ± 2.4 × 103 vs. 21.5 ± 5.6 × 103 pixels, respectively; p = 0.03) with no effect observed for age. VO2 max and SM tPA activity were also significantly correlated (r = 0.42; p < 0.04). SM tPA expression was higher in older participants, but no effect of fitness level was observed. No differences were observed for PAI-1 expression in SM.
Conclusions
Higher levels of aerobic fitness are associated with increased fibrinolytic activity in SM.

Similar content being viewed by others
Abbreviations
- CVD:
-
Cardiovascular disease
- OT:
-
Older trained
- OU:
-
Older untrained
- PAI-1:
-
Plasminogen activator inhibitor-1
- PCR:
-
Polymerase chain reaction
- RCF:
-
Relative centrifugal force
- RNA:
-
Ribonucleic acid
- RT:
-
Reverse transcription
- SM:
-
Skeletal muscle
- tPA:
-
Tissue plasminogen activator
- uPA:
-
Urokinase plasminogen activator
- VO2 max :
-
Maximal oxygen consumption
- wt:
-
Weight
- YT:
-
Young trained
- YU:
-
Young untrained
References
Abbate R, Prisco D, Rostagno C, Boddi M, Gensini GF (1993) Age-related changes in the hemostatic system. Int J Clin Lab Res 23(1):1–3
Angleton P, Chandler WL, Schmer G (1989) Diurnal variation of tissue-type plasminogen activator and its rapid inhibitor (PAI-1). Circulation 79(1):101–106
Barani AE, Durieux AC, Sabido O, Freyssenet D (2003) Age-related changes in the mitotic and metabolic characteristics of muscle-derived cells. J Appl Physiol 95(5):2089–2098
Bassett DR Jr (1994) Skeletal muscle characteristics: relationships to cardiovascular risk factors. Med Sci Sports Exerc 26(8):957–966
Carpenter RL, Lemmer JT, Francis RM, Knous JL, Sarzynski MA, Womack CJ (2010) Tissue plasminogen activator and plasminogen activator inhibitor-1 gene expression in muscle after maximal acute aerobic exercise. J Exerc Physiol 13(6):35–44
Chandler WL, Levy WC, Stratton JR (1995) The circulatory regulation of TPA and UPA secretion, clearance, and inhibition during exercise and during the infusion of isoproterenol and phenylephrine. Circulation 92(10):2984–2994
Daussin FN, Zoll J, Dufour SP, Ponsot E, Lonsdorfer-Wolf E, Doutreleau S, Mettauer B, Piquard F, Geny B, Richard R (2008) Effect of interval versus continuous training on cardiorespiratory and mitochondrial functions: relationship to aerobic performance improvements in sedentary subjects. Am J Physiol Regul Integr Comp Physiol 295(1):R264–R272
DeSouza CA, Jones PP, Seals DR (1998) Physical activity status and adverse age-related differences in coagulation and fibrinolytic factors in women. Arterioscler Thromb Vasc Biol 18(3):362–368
El-Sayed MS, El-Sayed Ali Z, Ahmadizad S (2004) Exercise and training effects on blood haemostasis in health and disease: an update. Sports Med 34(3):181–200
Estelles A, Aznar J, Tormo G, Sapena P, Tormo V, Espana F (1989) Influence of a rehabilitation sports programme on the fibrinolytic activity of patients after myocardial infarction. Thromb Res 55(2):203–212
Evans WJ, Phinney SD, Young VR (1982) Suction applied to a muscle biopsy maximizes sample size. Med Sci Sports Exerc 14(1):101–102
Fibbi G, Barletta E, Dini G, Del Rosso A, Pucci M, Cerletti M, Del Rosso M (2001) Cell invasion is affected by differential expression of the urokinase plasminogen activator/urokinase plasminogen activator receptor system in muscle satellite cells from normal and dystrophic patients. Lab Invest 81(1):27–39
Fibbi G, D’Alessio S, Pucci M, Cerletti M, Del Rosso M (2002) Growth factor-dependent proliferation and invasion of muscle satellite cells require the cell-associated fibrinolytic system. Biol Chem 383(1):127–136
Folsom AR, Aleksic N, Park E, Salomaa V, Juneja H, Wu KK (2001) Prospective study of fibrinolytic factors and incident coronary heart disease: the Atherosclerosis Risk in Communities (ARIC) Study. Arterioscler Thromb Vasc Biol 21(4):611–617
Francis JL (1988) Fibrinogen, fibrin stabilisation, and fibrinolysis: clinical, biochemical, and laboratory aspects. Ellis Horwood series in biomedicine. VCH, New York
Gardner AW, Killewich LA (2002) Association between physical activity and endogenous fibrinolysis in peripheral arterial disease: a cross-sectional study. Angiology 53(4):367–374
Giri S, Thompson PD, Kiernan FJ, Clive J, Fram DB, Mitchel JF, Hirst JA, McKay RG, Waters DD (1999) Clinical and angiographic characteristics of exertion-related acute myocardial infarction. JAMA 282(18):1731–1736
Gleerup G, Winther K (1995) The effect of ageing on platelet function and fibrinolytic activity. Angiology 46(8):715–718
Hashimoto Y, Kobayashi A, Yamazaki N, Sugawara Y, Takada Y, Takada A (1987) Relationship between age and plasma t-PA, PA-inhibitor, and PA activity. Thromb Res 46(5):625–633
Hepple RT, Mackinnon SL, Goodman JM, Thomas SG, Plyley MJ (1997) Resistance and aerobic training in older men: effects on VO2peak and the capillary supply to skeletal muscle. J Appl Physiol 82(4):1305–1310
Hittel DS, Kraus WE, Hoffman EP (2003) Skeletal muscle dictates the fibrinolytic state after exercise training in overweight men with characteristics of metabolic syndrome. J Physiol 548(Pt 2):401–410
Huber D, Cramer EM, Kaufmann JE, Meda P, Masse JM, Kruithof EK, Vischer UM (2002) Tissue-type plasminogen activator (t-PA) is stored in Weibel–Palade bodies in human endothelial cells both in vitro and in vivo. Blood 99(10):3637–3645
Killewich LA, Macko RF, Montgomery PS, Wiley LA, Gardner AW (2004) Exercise training enhances endogenous fibrinolysis in peripheral arterial disease. J Vasc Surg 40(4):741–745
Koh TJ, Bryer SC, Pucci AM, Sisson TH (2005) Mice deficient in plasminogen activator inhibitor-1 have improved skeletal muscle regeneration. Am J Physiol Cell Physiol 289(1):C217–C223
Kraus WE, Torgan CE, Duscha BD, Norris J, Brown SA, Cobb FR, Bales CW, Annex BH, Samsa GP, Houmard JA, Slentz CA (2001) Studies of a targeted risk reduction intervention through defined exercise (STRRIDE). Med Sci Sports Exerc 33(10):1774–1784
Lash JM, Bohlen HG (1992) Functional adaptations of rat skeletal muscle arterioles to aerobic exercise training. J Appl Physiol 72(6):2052–2062
Leber TM, Balkwill FR (1997) Zymography: a single-step staining method for quantitation of proteolytic activity on substrate gels. Anal Biochem 249(1):24–28
Lemmer JT, Francis RM, Hackney KJ, Carpenter RL, Womack CJ (2007) Single muscle fiber gene expression of tPA, uPA, and PAI-1. Med Sci Sports Exerc 39(5):S469–S470
Lisman T, de Groot PG, Meijers JC, Rosendaal FR (2005) Reduced plasma fibrinolytic potential is a risk factor for venous thrombosis. Blood 105(3):1102–1105
Lluis F, Roma J, Suelves M, Parra M, Aniorte G, Gallardo E, Illa I, Rodriguez L, Hughes SM, Carmeliet P, Roig M, Munoz-Canoves P (2001) Urokinase-dependent plasminogen activation is required for efficient skeletal muscle regeneration in vivo. Blood 97(6):1703–1711
Miles LA, Ellis V (2003) Alpha-enolase comes muscling in on plasminogen activation. Thromb Haemost 90(4):564–566
Salomaa V, Stinson V, Kark JD, Folsom AR, Davis CE, Wu KK (1995) Association of fibrinolytic parameters with early atherosclerosis. The ARIC Study. Atherosclerosis Risk in Communities Study. Circulation 91(2):284–290
Shono N, Urata H, Saltin B, Mizuno M, Harada T, Shindo M, Tanaka H (2002) Effects of low intensity aerobic training on skeletal muscle capillary and blood lipoprotein profiles. J Atheroscler Thromb 9(1):78–85
Silverstein MD, Heit JA, Mohr DN, Petterson TM, O’Fallon WM, Melton LJ 3rd (1998) Trends in the incidence of deep vein thrombosis and pulmonary embolism: a 25-year population-based study. Arch Intern Med 158(6):585–593
Smith FB, Lee AJ, Rumley A, Fowkes FG, Lowe GD (1995) Tissue-plasminogen activator, plasminogen activator inhibitor and risk of peripheral arterial disease. Atherosclerosis 115(1):35–43
Smith FB, Lee AJ, Fowkes FG, Price JF, Rumley A, Lowe GD (1997) Hemostatic factors as predictors of ischemic heart disease and stroke in the Edinburgh Artery Study. Arterioscler Thromb Vasc Biol 17(11):3321–3325
Smith DT, Hoetzer GL, Greiner JJ, Stauffer BL, DeSouza CA (2003) Effects of ageing and regular aerobic exercise on endothelial fibrinolytic capacity in humans. J Physiol 546(Pt 1):289–298
Stratton JR, Chandler WL, Schwartz RS, Cerqueira MD, Levy WC, Kahn SE, Larson VG, Cain KC, Beard JC, Abrass IB (1991) Effects of physical conditioning on fibrinolytic variables and fibrinogen in young and old healthy adults. Circulation 83(5):1692–1697
Suelves M, Lopez-Alemany R, Lluis F, Aniorte G, Serrano E, Parra M, Carmeliet P, Munoz-Canoves P (2002) Plasmin activity is required for myogenesis in vitro and skeletal muscle regeneration in vivo. Blood 99(8):2835–2844
Suelves M, Vidal B, Serrano AL, Tjwa M, Roma J, Lopez-Alemany R, Luttun A, de Lagran MM, Diaz-Ramos A, Jardi M, Roig M, Dierssen M, Dewerchin M, Carmeliet P, Munoz-Canoves P (2007) uPA deficiency exacerbates muscular dystrophy in MDX mice. J Cell Biol 178(6):1039–1051. doi:10.1083/jcb.200705127
van den Burg PJ, Hospers JE, van Vliet M, Mosterd WL, Bouma BN, Huisveld IA (1997) Effect of endurance training and seasonal fluctuation on coagulation and fibrinolysis in young sedentary men. J Appl Physiol 82(2):613–620
Wilkerson WR, Sane DC (2002) Aging and thrombosis. Semin Thromb Hemost 28(6):555–568
Winther K, Hillegass W, Tofler GH, Jimenez A, Brezinski DA, Schafer AI, Loscalzo J, Williams GH, Muller JE (1992) Effects on platelet aggregation and fibrinolytic activity during upright posture and exercise in healthy men. Am J Cardiol 70(11):1051–1055
Yamamoto K, Takeshita K, Kojima T, Takamatsu J, Saito H (2005) Aging and plasminogen activator inhibitor-1 (PAI-1) regulation: implication in the pathogenesis of thrombotic disorders in the elderly. Cardiovasc Res 66(2):276–285
Zhang C, Meng X, Zhu Z, Yang X, Deng A (2004) Role of connective tissue growth factor in renal tubular epithelial-myofibroblast transdifferentiation and extracellular matrix accumulation in vitro. Life Sci 75(3):367–379
Acknowledgments
This study was supported by a research grant from the Michigan State University Intramural Research Grant Program and the College of Education. We would like to thank Dr. Mukta Webber and Erik Tokar for their helping with teaching us gel zymography. We would like to thank the Research Technology Support Facility at Michigan State University for their consultation and expertise on the microarray analyses.
Conflict of interest
There are no companies, manufacturers or outside organizations that will benefit from the results of the present study.
Author information
Authors and Affiliations
Corresponding author
Additional information
Communicated by Fabio Fischetti.
Rights and permissions
About this article
Cite this article
Francis, R.M., Romeyn, C.L., Coughlin, A.M. et al. Age and aerobic training status effects on plasma and skeletal muscle tPA and PAI-1. Eur J Appl Physiol 114, 1229–1238 (2014). https://doi.org/10.1007/s00421-014-2857-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-014-2857-2