Abstract
Purpose
The study aims to review the efficacy, safety, and technique of Nd:YAG laser vitreolysis for the management of malignant glaucoma (MG).
Methods
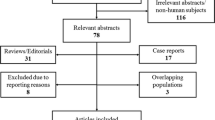
We performed a search of electronic databases for all published studies which included technical specifications of Nd:YAG laser application for MG. Individual patient data was extracted and evaluated in a weighted pooled analysis.
Results
Thirty eyes were reported on from seven studies worldwide. Age of affected patients ranged between 37 and 82 years. Nd:YAG vitreolysis was performed either through an iritodomy (66.7%, 18/27 eyes), transpupillary (18.5%, 5/27 eyes), or through both simultaneously (14.8%, 4/27 eyes). Treatment intensity ranged between 1.0 and 11.00 mJ with 75.9% (22/29 eyes) of treatments being 3.0 mJ or lower. Between 1 and 41 pulses per session were applied. Rates of both anatomical and intraocular pressure resolution were examined. Overall, in a pooled analysis, 77% of eyes demonstrated MG resolution with no further treatment required after Nd:YAG vitreolysis (95% CI: 58.1 to 91.4%). A trend for lower need of additional interventions was seen with transpupillary application (11.1% versus 42.1%). No complications were reported.
Conclusions
Nd:YAG laser vitreolysis is a safe procedure, associated with MG resolution in the majority of reported cases, regardless of treatment intensity. Transpupillary treatment may be associated with lower risk of re-intervention.






Similar content being viewed by others
Availability of data and material
Uploaded as tables.
Code availability
Not applicable.
References
Grzybowski A, Kanclerz P (2018) Acute and chronic fluid misdirection syndrome: pathophysiology and treatment. Graefes Arch Clin Exp Ophthalmol 256:135–154. https://doi.org/10.1007/s00417-017-3837-0
Foreman-Larkin J, Netland PA, Salim S (2015) Clinical management of malignant glaucoma. J Ophthalmol 2015:283707. https://doi.org/10.1155/2015/283707
Sharma A, Sii F, Shah P, Kirkby GR (2006) Vitrectomy-phacoemulsification-vitrectomy for the management of aqueous misdirection syndromes in phakic eyes. Ophthalmology 113:1968–1973. https://doi.org/10.1016/j.ophtha.2006.04.031
Varma DK, Belovay GW, Tam DY, Ahmed II (2014) Malignant glaucoma after cataract surgery. J Cataract Refract Surg 40:1843–1849. https://doi.org/10.1016/j.jcrs.2014.02.045
Debrouwere V, Stalmans P, Van Calster J, Spileers W, Zeyen T, Stalmans I (2012) Outcomes of different management options for malignant glaucoma: a retrospective study. Graefes Arch Clin Exp Ophthalmol 250:131–141. https://doi.org/10.1007/s00417-011-1763-0
Lynch MG, Brown RH, Michels RG, Pollack IP, Stark WJ (1986) Surgical vitrectomy for pseudophakic malignant glaucoma. Am J Ophthalmol 102:149–153. https://doi.org/10.1016/0002-9394(86)90135-2
Prata TS, Dorairaj S, De Moraes CG, Mehta S, Sbeity Z, Tello C, Liebmann J, Ritch R (2013) Is preoperative ciliary body and iris anatomical configuration a predictor of malignant glaucoma development? Clin Experiment Ophthalmol 41:541–545. https://doi.org/10.1111/ceo.12057
Shaffer RN, Hoskins HD Jr (1978) Ciliary block (malignant) glaucoma. Ophthalmology 85:215–221. https://doi.org/10.1016/s0161-6420(78)35669-4
Quigley HA, Friedman DS, Congdon NG (2003) Possible mechanisms of primary angle-closure and malignant glaucoma. J Glaucoma 12:167–180. https://doi.org/10.1097/00061198-200304000-00013
Chandler PA (1951) Malignant glaucoma. Am J Ophthalmol 34:993–1000. https://doi.org/10.1016/0002-9394(51)91168-3
Epstein DL, Hashimoto JM, Anderson PJ, Grant WM (1979) Experimental perfusions through the anterior and vitreous chambers with possible relationships to malignant glaucoma. Am J Ophthalmol 88:1078–1086. https://doi.org/10.1016/0002-9394(79)90420-3
Brown RH, Lynch MG, Tearse JE, Nunn RD (1986) Neodymium-YAG vitreous surgery for phakic and pseudophakic malignant glaucoma. Arch Ophthalmol (Chicago, Ill : 1960) 104:1464–1466. https://doi.org/10.1001/archopht.1986.01050220058026
Epstein DL, Steinert RF, Puliafito CA (1984) Neodymium-YAG laser therapy to the anterior hyaloid in aphakic malignant (ciliovitreal block) glaucoma. Am J Ophthalmol 98:137–143. https://doi.org/10.1016/0002-9394(87)90347-3
Shahid H, Salmon JF (2012) Malignant glaucoma: a review of the modern literature. J Ophthalmol 2012:852659. https://doi.org/10.1155/2012/852659
Thompson AC, Vu DM, Postel EA, Challa P (2020) Factors impacting outcomes and the time to recovery from malignant glaucoma. Am J Ophthalmol 209:141–150. https://doi.org/10.1016/j.ajo.2019.07.023
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700. https://doi.org/10.1136/bmj.b2700
Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M, Henry D, Altman DG, Ansari MT, Boutron I, Carpenter JR, Chan AW, Churchill R, Deeks JJ, Hróbjartsson A, Kirkham J, Jüni P, Loke YK, Pigott TD, Ramsay CR, Regidor D, Rothstein HR, Sandhu L, Santaguida PL, Schünemann HJ, Shea B, Shrier I, Tugwell P, Turner L, Valentine JC, Waddington H, Waters E, Wells GA, Whiting PF, Higgins JP (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919. https://doi.org/10.1136/bmj.i4919
Bravata DM, Olkin I (2001) Simple pooling versus combining in meta-analysis. Eval Health Prof 24:218–230. https://doi.org/10.1177/01632780122034885
Dave P, Senthil S, Rao HL, Garudadri CS (2013) Treatment outcomes in malignant glaucoma. Ophthalmology 120:984–990. https://doi.org/10.1016/j.ophtha.2012.10.024
Tomey KF, Senft SH, Antonios SR, Shammas IV, Shihab ZM, Traverso CE (1987) Aqueous misdirection and flat chamber after posterior chamber implants with and without trabeculectomy. Arch Ophthalmol (Chicago, Ill : 1960) 105:770–773. https://doi.org/10.1001/archopht.1987.01060060056032
Melamed S, Ashkenazi I, Blumenthal M (1991) Nd-YAG laser hyaloidotomy for malignant glaucoma following one-piece 7 mm intraocular lens implantation. Br J Ophthalmol 75:501–503. https://doi.org/10.1136/bjo.75.8.501
Wu ZH, Wang YH, Liu Y (2016) Management strategies in malignant glaucoma secondary to antiglaucoma surgery. Int J Ophthalmol 9:63–68. https://doi.org/10.18240/ijo.2016.01.11
Wang J, Du E, Tang J (2018) The treatment of malignant glaucoma in nanophthalmos: a case report. BMC Ophthalmol 18:54. https://doi.org/10.1186/s12886-018-0714-5
Delaney YM, Oyinloye A, Benjamin L (2002) Nd:YAG vitreolysis and pars plana vitrectomy: surgical treatment for vitreous floaters. Eye (Lond) 16:21–26. https://doi.org/10.1038/sj.eye.6700026
Shah CP, Heier JS (2017) YAG laser vitreolysis vs sham YAG vitreolysis for symptomatic vitreous floaters: a randomized clinical trial. JAMA Ophthalmol 135:918–923. https://doi.org/10.1001/jamaophthalmol.2017.2388
Little BC, Hitchings RA (1993) Pseudophakic malignant glaucoma: Nd:YAG capsulotomy as a primary treatment. Eye (Lond) 7(Pt 1):102–104. https://doi.org/10.1038/eye.1993.21
Shah CP, Heier JS (2020) Long-term follow-up of efficacy and safety of YAG vitreolysis for symptomatic Weiss ring floaters. Ophthalmic Surg Lasers Imaging Retina 51:85–88. https://doi.org/10.3928/23258160-20200129-04
Liu X, Wang Q, Zhao J (2020) Acute retinal detachment after Nd:YAG treatment for vitreous floaters and postertior capsule opacification: a case report. BMC Ophthalmol 20:157. https://doi.org/10.1186/s12886-020-01428-7
Ozyol E, Ozyol P, DoğanayErdoğan B, Onen M (2014) The role of anterior hyaloid face integrity on retinal complications during Nd: YAG laser capsulotomy. Graefes Arch Clin Exp Ophthalmol 252:71–75. https://doi.org/10.1007/s00417-013-2526-x
Bhargava R, Kumar P, Phogat H, Chaudhary KP (2015) Neodymium-yttrium aluminium garnet laser capsulotomy energy levels for posterior capsule opacification. J Ophthalmic Vis Res 10:37–42. https://doi.org/10.4103/2008-322x.156101
Author information
Authors and Affiliations
Contributions
M. S. collected the data and wrote the manuscript. I. D. performed the statistical analysis and critically revised the manuscript. T. S. and A. E. L. contributed to the discussion and critically revised the manuscript. A. B. contributed to the discussion, critically revised the manuscript, and directed the project.
Corresponding author
Ethics declarations
Ethics approval
This is a review and meta-analysis article. The Shamir Medical Center Research Ethics Committee has confirmed that no ethical approval is required.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Safir, M., Hecht, I., Sharon, T. et al. Application of Nd:YAG laser to the anterior vitreous in malignant glaucoma — a systemic review and meta-analysis. Graefes Arch Clin Exp Ophthalmol 260, 2981–2990 (2022). https://doi.org/10.1007/s00417-022-05640-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-022-05640-7