Abstract
Objective
To investigate the clinical features and surgical outcomes of pediatric congenital first branchial cleft anomalies (CFBCAs).
Methods
We conducted a retrospective analysis of 100 children who were referred to Shanghai Children’s Hospital from March 2014 to March 2022 for the treatment of CFBCAs.
Results
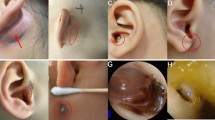
This study included 100 patients (33 males, 67 females) with an average age of 4.0 ± 2.7 years. 64 cases were type I FBCAs and 36 were type II. The main clinical manifestations included having a skin pit or discharge from it (62%), painless masses (5%), mucopurulent otorrhea (8%) and recurrent swelling with pain (90%) in the Pochet’s triangle area. 92% had infection histories, 84% had incision and drainage histories, and 18% had surgical histories. 6 cases of tympanic membranous attachment were found by auricular endoscopy. Ultrasonography (US) was 55.6% (30/54) accurate and enhanced CT was 75% (75/100) accurate in diagnosing CFBCAs. We dissected the facial nerve (FN) in 46% cases. Lesions ended in the external auditory canal (EAC) wall in 86 cases. 69 exhibited close relationship with the parotid. The patients were followed up 0.25–8.2 years. 11 had postoperative temporary facial paralysis and all improved within 6 months. 3 had recurrence and they were secondarily successfully retreated. No EAC stenosis were found.
Conclusions
CFBCAs often presented with repeated swelling and purulence in Pochet’s triangle. CT, US and auricular endoscopy can assist in diagnosis and planning the surgical strategy. Complete excision in non-infection stage as soon as possible is the first choice for the treatment of CFBCAs.


Similar content being viewed by others
References
Brown LA, Johnston DR, Rastatter J et al (2019) Differences in management outcome for first branchial cleft anomalies: a comparison of infants and toddlers to older children. Int J Pediatr Otorhinolaryngol 122:161–164
Liu W, Chen M, Hao J et al (2017) The treatment for the first branchial cleft anomalies in children. Eur Arch Otorhinolaryngol 274(9):3465–3470
Yang R, Dong C, Chen Y et al (2022) Analysis of the clinical features and surgical outcomes of first branchial cleft anomalies. Laryngoscope 132(5):1008–1014
Johnson JM, Moonis G, Green GE et al (2011) Syndromes of the first and second branchial arches, part 2: syndromes. AJNR Am J Neuroradiol 32(2):230–237
Shehan JN, Levi JR (2021) An unexpected cyst of the ear lobule. Am J Otolaryngol 42(4):102976
Work WP (1972) Newer concepts of first branchial cleft defects. Laryngoscope 82(9):1581–1593
Olsen KD, Maragos NE, Weiland LH (1980) First branchial cleft anomalies. Laryngoscope 90(3):423–436
Shinn JR, Purcell PL, Horn DL et al (2015) First branchial cleft anomalies: otologic manifestations and treatment outcomes. Otolaryngol Head Neck Surg 152(3):506–512
Li W, Zhao L, Xu H et al (2017) First branchial cleft anomalies in children: experience with 30 cases. Exp Ther Med 14(1):333–337
D’Souza AR, Uppal HS, De R et al (2002) Updating concepts of first branchial cleft defects: a literature review. Int J Pediatr Otorhinolaryngol 62(2):103–109
Chalard F, Hermann AL, Elmaleh-Berges M et al (2022) Correction: Imaging of parotid anomalies in infants and children. Insights Imaging 13(1):86
Chavan S, Deshmukh R, Karande P et al (2014) Branchial cleft cyst: a case report and review of literature. J Oral Maxillofac Pathol 18(1):150
Liu W, Liu B, Chen M et al (2018) Clinical analysis of first branchial cleft anomalies in children. Pediatr Investig 2(3):149–153
Liu W, Chen M, Liu B et al (2021) Clinical analysis of type II first branchial cleft anomalies in children. Laryngoscope 131(4):916–920
Ash J, Sanders OH, Abed T et al (2021) First branchial cleft anomalies: awareness is key. Cureus 13(12):e20655
Triglia JM, Nicollas R, Ducroz V et al (1998) First branchial cleft anomalies: a study of 39 cases and a review of the literature. Arch Otolaryngol Head Neck Surg 124(3):291–295
Jang M, Dai C (2017) An effective surgical approach for the management of recurrent first branchial cleft fistula with cysts: a case report. J Int Adv Otol 13(3):419–421
Liu H, Cheng A, Ward BB et al (2020) Clinical manifestations, diagnosis, and management of first branchial cleft fistula/sinus: a case series and literature review. J Oral Maxillofac Surg 78(5):749–761
Quintanilla-Dieck L, Virgin F, Wootten C et al (2016) Surgical approaches to first branchial cleft anomaly excision: a case series. Case Rep Otolaryngol 2016:3902974
Ebelhar AJ, Potts K (2012) An unusual otoscopic finding associated with a type II first branchial cleft anomaly. J Laryngol Otol 126(3):316–318
Ertas B, Gunaydin RO, Unal OF (2015) The relationship between the fistula tract and the facial nerve in type II first branchial cleft anomalies. Auris Nasus Larynx 42(2):119–122
Solares CA, Chan J, Koltai PJ (2003) Anatomical variations of the facial nerve in first branchial cleft anomalies. Arch Otolaryngol Head Neck Surg 129(3):351–355
Stulner C, Chambers PA, Telfer MR et al (2001) Management of first branchial cleft anomalies: report of two cases. Br J Oral Maxillofac Surg 39(1):30–33
Chang PH, Wu CM (2005) An insidious preauricular sinus presenting as an infected postauricular cyst. Int J Clin Pract 59(3):370–372
Martinez Del Pero M, Majumdar S, Bateman N et al (2007) Presentation of first branchial cleft anomalies: the Sheffield experience. J Laryngol Otol 121(5):455–459
Liu Y, Li T, Xue J et al (2012) First branchial cleft fistula presenting with internal opening on the Eustachian tube: illustrated cases and literature review. Int J Pediatr Otorhinolaryngol 76(5):642–645
Guo YX, Guo CB (2012) Relation between a first branchial cleft anomaly and the facial nerve. Brit J Oral Max Surg 50(3):259–263
Maithani T, Pandey A, Dey D et al (2014) First branchial cleft anomaly: clinical insight into its relevance in otolaryngology with pediatric considerations. Indian J Otolaryngol 66:S271–S276
Funding
Shanghai Shenkang hospital development center municipal hospital clinical research cultivation project (SHDC12019X21).
Author information
Authors and Affiliations
Contributions
Each of the authors has contributed to read and approved this manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interests regarding the publication of this paper.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, W., Xu, M., Wang, Q. et al. Congenital first branchial cleft anomalies in children: a study of 100 surgical cases and a review of the literature. Eur Arch Otorhinolaryngol 280, 425–433 (2023). https://doi.org/10.1007/s00405-022-07607-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-022-07607-0