Abstract
Purpose
This study aims to assess the impact of endometrioma on patients who undergo ART treatment due to endometriosis.
Methods
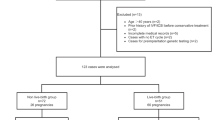
A retrospective study was conducted on women ≤ 40 years of age who underwent ART treatment at an academic medical center between January 2014 and December 2020. Two-hundred-and-eight women had received IVF/ICSI treatment due to endometriosis and there were 89 patients presence of endometrioma. Patients were further divided into primary endometrioma, recurrent endometrioma and those having received cystectomy for endometrioma prior to IVF/ICSI. The control group included 624 infertile women without endometriosis.
Results
In the endometrioma subgroup (B) the blastocyst formation rate was significantly lower when compared with the endometriosis (A) and control groups (C). The cumulative live birth rates (CLBRs) (60.5% versus 49.4% versus 56.9%, p = 0.194 in A versus B, p = 0.406 in A versus C, p = 0.878 in B versus C) were comparable. Multiple logistic regression analysis revealed that female age, total FSH dose and blastocyst formation rate were the significant variables in predicting CLBR (OR 0.89, CI 0.80–0.99, p < 0.025, OR 0.68 CI 0.53–0.88, p = 0.003 and OR 30.04, CI 9.93–90.9, p < 0.001, respectively). The CLBRs were comparable at 47.1%, 60% and 57.9% in the primary endometrioma, s/p cystectomy and recurrent endometrioma group.
Conclusion
Although the blastocyst formation rate was lower in the endometrioma group, CLBR was not worse than those who were in the endometriosis or control group. Cystectomy for endometrioma did not alter IVF/ICSI outcomes if the ovarian reserve was comparable. Recurrent endometrioma did not worsen IVF/ICSI outcomes than primary endometrioma.



Similar content being viewed by others
Availability of data and materials
All data generated and analyzed during this study are included in this published article and its supplementary information files.
Data availability
Data of the study are available and can be provided upon request.
References
Holoch KJ, Lessey BA (2010) Endometriosis and infertility. Clin Obstet Gynecol 53:429–438. https://doi.org/10.1097/GRF.0b013e3181db7d71
Macer ML, Taylor HS (2012) Endometriosis and infertility: a review of the pathogenesis and treatment of endometriosis-associated infertility. Obstet Gynecol Clin North Am 39:535–549. https://doi.org/10.1016/j.ogc.2012.10.002
Hughesdon PE (1957) The structure of endometrial cysts of the ovary. J Obstet Gynaecol Br Emp 64:481–487. https://doi.org/10.1111/j.1471-0528.1957.tb06276.x
Alborzi S, Keramati P, Younesi M, Samsami A, Dadras N (2014) The impact of laparoscopic cystectomy on ovarian reserve in patients with unilateral and bilateral endometriomas. Fertil Steril 101(2):427–434. https://doi.org/10.1016/j.fertnstert.2013.10.019
Young VJ, Brown JK, Saunders PT, Horne AW (2013) The role of the peritoneum in the pathogenesis of endometriosis. Hum Reprod Update 19:558–569. https://doi.org/10.1093/humupd/dmt024
Sanchez AM, Viganò P, Somigliana E, Panina-Bordignon P, Vercellini P, Candiani M (2014) The distinguishing cellular and molecular features of the endometriotic ovarian cyst: from pathophysiology to the potential endometrioma-mediated damage to the ovary. Hum Reprod Update 20:217–230. https://doi.org/10.1093/humupd/dmt053
Kuroda M, Kuroda K, Arakawa A, Fukumura Y, Kitade M, Kikuchi I, Kumakiri J, Matsuoka S, Brosens IA, Brosens JJ, Takeda S, Yao T (2012) Histological assessment of impact of ovarian endometrioma and laparoscopic cystectomy on ovarian reserve. J Obstet Gynaecol Res 38:1187–1193. https://doi.org/10.1111/j.1447-0756.2012.01845.x
Matsuzaki S, Schubert B (2010) Oxidative stress status in normal ovarian cortex surrounding ovarian endometriosis. Fertil Steril 93:2431–2432. https://doi.org/10.1016/j.fertnstert.2009.08.068
Muzii L, Di Tucci C, Di Feliciantonio M, Galati G, Di Donato V, Musella A, Palaia I, Panici PB (2018) Antimüllerian hormone is reduced in the presence of ovarian endometriomas: a systematic review and meta-analysis. Fertil Steril 110:932–940. https://doi.org/10.1016/j.fertnstert.2018.06.025
Hamdan M, Dunselman G, Li TC, Cheong Y (2015) The impact of endometrioma on IVF/ICSI outcomes: a systematic review and meta-analysis. Hum Reprod Update 21:809–825. https://doi.org/10.1093/humupd/dmv035
Sanchez AM, Vanni VS, Bartiromo L, Papaleo E, Zilberberg E, Candiani M, Orvieto R, Viganò P (2017) Is the oocyte quality affected by endometriosis? A review of the literature. J Ovarian Res 10:43. https://doi.org/10.1186/s13048-017-0341-4
Becker CM, Bokor A, Heikinheimo O, Horne A, Jansen F, Kiesel L, King K, Kvaskoff M, Nap A, Petersen K, Saridogan E, Tomassetti C, van Hanegem N, Vulliemoz N, Vermeulen N (2022) ESHRE Endometriosis Guideline Group. ESHRE guideline: endometriosis. Hum Reprod Open. https://doi.org/10.1093/hropen/hoac009
Vercellini P, Somigliana E, Daguati R, Barbara G, Abbiati A, Fedele L (2009) The second time around: reproductive performance after repetitive versus primary surgery for endometriosis. Fertil Steril 92:1253–1255. https://doi.org/10.1016/j.fertnstert.2009.04.037
Benaglia L, Somigliana E, Iemmello R, Colpi E, Nicolosi AE, Ragni G (2008) Endometrioma and oocyte retrieval-induced pelvic abscess: a clinical concern or an exceptional complication? Fertil Steril 89:1263–1266. https://doi.org/10.1016/j.fertnstert.2007.05.038
Nieweglowska D, Hajdyla-Banas I, Pitynski K, Banas T, Grabowska O, Juszczyk G, Ludwin A, Jach R (2015) Age-related trends in anti-Mullerian hormone serum level in women with unilateral and bilateral ovarian endometriomas prior to surgery. Reprod Biol Endocrinol 13:128. https://doi.org/10.1186/s12958-015-0125-x
Somigliana E, Benaglia L, Paffoni A, Busnelli A, Vigano P, Vercellini P (2015) Risks of conservative management in women with ovarian endometriomas undergoing IVF. Hum Reprod Update 21:486–499. https://doi.org/10.1093/humupd/dmv012
Younis JS, Shapso N, Fleming R, Ben-Shlomo I, Izhaki I (2019) Impact of unilateral versus bilateral ovarian endometriotic cystectomy on ovarian reserve: a systematic review and meta-analysis. Hum Reprod Update 25:375–391. https://doi.org/10.1093/humupd/dmy049
Ergun B, Ozsurmeli M, Dundar O, Comba C, Kuru O, Bodur S (2015) Changes in markers of ovarian reserve after laparoscopic ovarian cystectomy. J Minim Invasive Gynecol 22:997–1003. https://doi.org/10.1016/j.jmig.2015.05.001
Benschop L, Farquhar C, van der Poel N, Heineman MJ (2010) Interventions for women with endometrioma prior to assisted reproductive technology. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD008571
Exacoustos C, Manganaro L, Zupi E (2014) Imaging for the evaluation of endometriosis and adenomyosis. Best Pract Res Clin Obstet Gynaecol 28:655–681. https://doi.org/10.1016/j.bpobgyn.2014.04.010
Chang J-C, Chen M-J, Guu H-F, Chen Y-F, Yi Y-C, Kung H-F, Chen L-Y (2017) Min-Min Chou Does the “freeze-all” policy allow for a better outcome in assisted reproductive techniques than the use of fresh embryo transfers? A retrospective study. Taiwan J Obstet Gynecol 56(6):775–780. https://doi.org/10.1016/j.tjog.2017.10.013
Senapati S, Sammel MD, Morse C, Barnhart KT (2016) Impact of endometriosis on in vitro fertilization outcomes: an evaluation of the Society for Assisted Reproductive Technologies Database. Fertil Steril 106:164–171. https://doi.org/10.1016/j.fertnstert.2016.03.037
Prefumo F, Rossi AC (2018) Endometriosis, endometrioma, and ART results: Current understanding and recommended practices. Best Pract Res Clin Obstet Gynaecol 51:34–40. https://doi.org/10.1016/j.bpobgyn.2018.01.019
Rossi AC, Prefumo F (2016) The effects of surgery for endometriosis on pregnancy outcomes following in vitro fertilization and embryo transfer: a systematic review and meta-analysis. Arch Gynecol Obstet 294:647–655. https://doi.org/10.1007/s00404-016-4136-4
Alshehre SM, Narice BF, Fenwick MA, Metwally M (2021) The impact of endometrioma on in vitro fertilisation/intra-cytoplasmic injection IVF/ICSI reproductive outcomes: a systematic review and meta-analysis. Arch Gynecol Obstet 303(1):3–16. https://doi.org/10.1007/s00404-020-05796-9
Kuroda K, Kitade M, Kikuchi I, Kumakiri J, Matsuoka S, Kuroda M, Takeda S (2009) The impact of endometriosis, endometrioma and ovarian cystectomy on assisted reproductive technology. Reprod Med Biol 8:113–118. https://doi.org/10.1007/s12522-009-0021-1
Suzuki T, Izumi S, Matsubayashi H, Awaji H, Yoshikata K, Makino T (2005) Impact of ovarian endometrioma on oocytes and pregnancy outcome in in vitro fertilization. Fertil Steril 83:908–913. https://doi.org/10.1016/j.fertnstert.2004.11.028
Leonardi M, Gibbons T, Armour M, Wang R, Glanville E, Hodgson R, Cave AE, Ong J, Tong YYF, Jacobson TZ, Mol BW, Johnson NP, Condous G (2020) When to do surgery and when not to do surgery for endometriosis: a systematic review and meta-analysis. J Minim Invasive Gynecol 27:390–407. https://doi.org/10.1016/j.jmig.2019.10.014
Wu CQ, Albert A, Alfaraj S, Taskin O, Alkusayer GM, Havelock J, Yong P, Allaire C, Bedaiwy MA (2019) Live Birth Rate after Surgical and Expectant Management of Endometriomas after In Vitro Fertilization: A Systematic Review, Meta-Analysis, and Critical Appraisal of Current Guidelines and Previous Meta-Analyses. J Minim Invasive Gynecol 26:299–311. https://doi.org/10.1016/j.jmig.2018.08.029
Maignien C, Santulli P, Gayet V, Lafay-Pillet MC, Korb D, Bourdon M, Marcellin L, de Ziegler D, Chapron C (2017) Prognostic factors for assisted reproductive technology in women with endometriosis-related infertility. Am J Obstet Gynecol 216(280):e1-280.e9. https://doi.org/10.1016/j.ajog.2016.11.1042
Roustan A, Perrin J, Debals-Gonthier M, Paulmyer-Lacroix O, Agostini A, Courbiere B (2015) Surgical diminished ovarian reserve after endometrioma cystectomy versus idiopathic DOR: comparison of in vitro fertilization outcome. Hum Reprod 30:840–847. https://doi.org/10.1093/humrep/dev029
Ata B, Mumusoglu S, Aslan K, Seyhan A, Kasapoglu I, Avci B, Urman B, Bozdag G, Uncu G (2017) Which is worse? Comparison of ART outcome between women with primary or recurrent endometriomas. Hum Reprod 32:1427–1431. https://doi.org/10.1093/humrep/dex099
Muzii L, Achilli C, Lecce F, Bianchi A, Franceschetti S, Marchetti C, Perniola G, Panici PB (2015) Second surgery for recurrent endometriomas is more harmful to healthy ovarian tissue and ovarian reserve than first surgery. Fertil Steril 103:738–743. https://doi.org/10.1016/j.fertnstert.2014.12.101
Park H, Kim CH, Kim EY, Moon JW, Kim SH, Chae HD, Kang BM (2015) Effect of second-line surgery on in vitro fertilization outcome in infertile women with ovarian endometrioma recurrence after primary conservative surgery for moderate to severe endometriosis. Obstet Gynecol Sci 58:481–486. https://doi.org/10.5468/ogs.2015.58.6.481
Vercellini P, Somigliana E, Viganò P, Abbiati A, Barbara G, Crosignani PG (2009) Surgery for endometriosis-associated infertility: a pragmatic approach. Hum Reprod 24:254–269. https://doi.org/10.1093/humrep/den379
Corachán A, Pellicer N, Pellicer A, Ferrero H (2021) Novel therapeutic targets to improve IVF outcomes in endometriosis patients: a review and future prospects. Hum Reprod Update 27:923–972. https://doi.org/10.1093/humupd/dmab014
Ferrero H, Corachan A, Aguilar A, Quinonero A, Carbajo-Garcia MC, Alama P, Tejera A, Taboas E, Munoz E, Pellicer A (2019) Single-cell RNA sequencing of oocytes from ovarian endometriosis patients reveals a differential transcriptomic profile associated with lower quality. Hum Reprod 34:1302–1312. https://doi.org/10.1093/humrep/dez053
Tang H, Yan Y, Wang T, Zhang T, Shi W, Fan R, Yao Y (2015) Suodi Zhai Effect of follicle-stimulating hormone receptor Asn680Ser polymorphism on the outcomes of controlled ovarian hyperstimulation: an updated meta-analysis of 16 cohort studies. J Assist Reprod Genet 32:1801–1810. https://doi.org/10.1007/s10815-015-0600-5
Garrido N, Bellver J, Remohí J, Simón C, Pellicer A (2011) Cumulative live-birth rates per total number of embryos needed to reach newborn in consecutive in vitro fertilization (IVF) cycles: a new approach to measuring the likelihood of IVF success. Fertil Steril 96:40–46. https://doi.org/10.1016/j.fertnstert.2011.05.008
Exacoustos C, Zupi E, Piccione E (2017) Ultrasound imaging for ovarian and deep infiltrating endometriosis. Semin Reprod Med 35:5–24. https://doi.org/10.1055/s-0036-1597127
Funding
No funding was received for conducting this study.
Author information
Authors and Affiliations
Contributions
J-CC: Protocol/project development, Data Collection, Manuscript writing. M-JC: Protocol/project development, manuscript revision. H-FK: prepared the figures and tables. Y-CY: prepared the figures and tables. H-FG: Data collection or management. L-YC: Data collection or management. Y-FC: Data analysis. S-TC: Data analysis. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval and consent to participate
Institutional Review Board, TCVGH, No. CE21306B. Date of approval: August 30, 2021.
Informed consent statement
Not applicable
Consent to publish
Authors are responsible for the correctness of the statements provided in the manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chang, JC., Yi, YC., Chen, YF. et al. Presence of endometrioma decreased blastocyst formation rate but not impair Assisted Reproductive Technology (ART) outcome. Arch Gynecol Obstet 307, 2011–2020 (2023). https://doi.org/10.1007/s00404-023-07036-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-023-07036-2