Abstract
Objective
Extrauterine tumor spread is one of the essential determinants of disease outcome in endometrial cancer. However; more than 30% of patients still undergo incomplete surgery at the initial attempt. Strategies regarding the management of patients with incompletely staged early-stage disease or patients with undebulked advanced-stage disease remain controversial. Depending on postoperative uterine features and findings on imaging, patients may be put on observation or receive adjuvant therapy or undergo re-staging or debulking surgery followed by adjuvant therapy. To identify patients who would most benefit from a completion surgery, either for restaging or for cytoreduction, we developed a nomogram for estimation of extrauterine disease based on findings of final hysterectomy specimen.
Methods
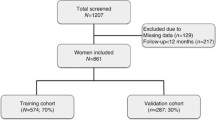
Data of 336 patients whose extrauterine disease status was known were analyzed. A nomogram was constructed using patient characteristics including age, grade, myometrial invasion, lymphovascular space involvement, cervical involvement, and peritoneal cytology. The nomogram was internally validated in terms of discrimination, calibration and overall performance.
Results
The nomogram showed good performance accuracy with an area under the receiver operating characteristic curve of 0.870, a specificity of 95.5%, and a positive predictive value of 73.9%. Decision curve analysis revealed that the use of the nomogram in decision-making for completion surgery leads to the equivalent of a net 18 true-positive results per 100 patients without an increase in the number of false-positive results.
Conclusions
Estimation of extrauterine disease from final hysterectomy specimen is possible with high predictive performance using the nomogram developed. The nomogram may help clinicians in decision-making for management of incomplete surgeries.


Similar content being viewed by others
References
Benedetti Panici P, Basile S, Maneschi F, Alberto Lissoni A, Signorelli M, Scambia G, Angioli R, Tateo S, Mangili G, Katsaros D, Garozzo G, Campagnutta E, Donadello N, Greggi S, Melpignano M, Raspagliesi F, Ragni N, Cormio G, Grassi R, Franchi M, Giannarelli D, Fossati R, Torri V, Amoroso M, Crocè C, Mangioni C (2008) Systematic pelvic lymphadenectomy vs. no lymphadenectomy in early-stage endometrial carcinoma: randomized clinical trial. J Natl Cancer Inst 100:1707–1716
ASTEC study group, Kitchener H, Swart AM, Qian Q, Amos C, Parmar MK, (2009) Efficacy of systematic pelvic lymphadenectomy in endometrial cancer (MRC ASTEC trial): a randomised study. Lancet 373:125–136
Havrilesky LJ, Cragun JM, Calingaert B, Synan I, Secord AA, Soper JT, Clarke-Pearson DL, Berchuck A (2005) Resection of lymph node metastases influences survival in stage IIIC endometrial cancer. Gynecol Oncol 99:689–695
Fujimoto T, Nanjyo H, Nakamura A, Yokoyama Y, Takano T, Shoji T, Nakahara K, Yamada H, Mizunuma H, Yaegashi N, Sugiyama T, Kurachi H, Sato A, Tanaka T (2007) Para-aortic lymphadenectomy may improve disease-related survival in patients with multipositive pelvic lymph node stage IIIc endometrial cancer. Gynecol Oncol 107:253–259
Barlin JN, Puri I, Bristow RE (2010) Cytoreductive surgery for advanced or recurrent endometrial cancer: a meta-analysis. Gynecol Oncol 118:14–18
Cripe J, Handorf E, Brown J, Jain A, Rubin S, Mantia-Smaldone G (2017) National Cancer Database Report of Lymphadenectomy Trends in Endometrial Cancer. Int J Gynecol Cancer 27:1408–1415
Mariani A, Dowdy SC, Cliby WA, Gostout BS, Jones MB, Wilson TO, Podratz KC (2008) Prospective assessment of lymphatic dissemination in endometrial cancer: a paradigm shift in surgical staging. Gynecol Oncol 109:11–18
Frumovitz M, Singh DK, Meyer L, Smith DH, Wertheim I, Resnik E, Bodurka DC (2004) Predictors of final histology in patients with endometrial cancer. Gynecol Oncol 95:463–468
NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines). Uterine Neoplasms, Version 1.2018. https://www.nccn.org. Accessed 20 September 2018.
Colombo N, Creutzberg C, Amant F, Bosse T, González-Martín A, Ledermann J, Marth C, Nout R, Querleu D, Mirza MR, Sessa C; ESMO-ESGO-ESTRO Endometrial Consensus Conference Working Group (2016) ESMO-ESGO-ESTRO Consensus Conference on Endometrial Cancer: diagnosis, treatment and follow-up. Ann Oncol 27: 16-41.
Bristow RE, Zerbe MJ, Rosenshein NB, Grumbine FC, Montz FJ (2000) Stage IVB endometrial carcinoma: the role of cytoreductive surgery and determinants of survival. Gynecol Oncol 78:85–91
Ayhan A, Taskiran C, Celik C, Yuce K, Kucukali T (2002) The influence of cytoreductive surgery on survival and morbidity in stage IVB endometrial cancer. Int J Gynecol Cancer 12:448–453
Cook NR (2010) Methods for evaluating novel biomarkers - a new paradigm. Int J Clin Pract 64:1723–1727
Steyerberg EW, Harrell FE Jr, Borsboom GJ, Eijkemans MJ, Vergouwe Y, Habbema JD (2001) Internal validation of predictive models: efficiency of some procedures for logistic regression analysis. J Clin Epidemiol 54:774–781
Gerds TA, Cai T, Schumacher M (2008) The performance of risk prediction models. Biom J 50:457–479
Vickers AJ (2008) Decision analysis for the evaluation of diagnostic tests, prediction models and molecular markers. Am Stat 62:314–320
Chan JK, Wu H, Cheung MK, Shin JY, Osann K, Kapp DS (2007) The outcomes of 27,063 women with unstaged endometrioid uterine cancer. Gynecol Oncol 106:282–288
Creutzberg CL, van Putten WL, Koper PC, Lybeert ML, Jobsen JJ, Wárlám-Rodenhuis CC, De Winter KA, Lutgens LC, van den Bergh AC, van de Steen-Banasik E, Beerman H, van Lent M (2000) Surgery and postoperative radiotherapy versus surgery alone for patients with stage-1 endometrial carcinoma: multicentre randomised trial. PORTEC Study Group. Post Operative Radiation Therapy in Endometrial Carcinoma. Lancet 355:1404–1411
Nout RA, Smit VT, Putter H, Jürgenliemk-Schulz IM, Jobsen JJ, Lutgens LC, van der Steen-Banasik EM, Mens JW, Slot A, Kroese MC, van Bunningen BN, Ansink AC, van Putten WL, Creutzberg CL; PORTEC Study Group (2010) Vaginal brachytherapy versus pelvic external beam radiotherapy for patients with endometrial cancer of high-intermediate risk (PORTEC-2): an open-label, non-inferiority, randomised trial. Lancet 375:816–823
de Boer SM, Powell ME, Mileshkin L, Katsaros D, Bessette P, Haie-Meder C, Ottevanger PB, Ledermann JA, Khaw P, Colombo A, Fyles A, Baron MH, Jürgenliemk-Schulz IM, Kitchener HC, Nijman HW, Wilson G, Brooks S, Carinelli S, Provencher D, Hanzen C, Lutgens LCHW, Smit VTHBM, Singh N, Do V, D'Amico R, Nout RA, Feeney A, Verhoeven-Adema KW, Putter H, Creutzberg CL, PORTEC study group. (2018) Adjuvant chemoradiotherapy versus radiotherapy alone for women with high-risk endometrial cancer (PORTEC-3): final results of an international, open-label, multicentre, randomised, phase 3 trial. Lancet Oncol 9:295–309
Matei D, Filiaci VL, Randall M (2017) A randomized phase III trial of cisplatin and tumor volume directed irradiation followed by carboplatin and paclitaxel vs carboplatin and paclitaxel for optimally debulked, advanced endometrial carcinoma. Proc Am Soc Clin Oncol 35(suppl 15):5505
Ayhan A, Kart C, Guven S, Boynukalin K, Kucukali T (2006) The role of reoperation in the management of endometrial carcinoma found in simple hysterectomy. J Surg Oncol 93:373–378
Rauch GM, Kaur H, Choi H, Kaur H, Choi H, Ernst RD, Klopp AH, Boonsirikamchai P, Westin SN, Marcal LP (2014) Optimization of MR imaging for pretreatment evaluation of patients with endometrial and cervical cancer. Radiographics 34:1082–1098
Kitajima K, Murakami K, Yamasaki E, Kaji Y, Sugimura K (2009) Accuracy of integrated FDG-PET/contrast-enhanced CT in detecting pelvic and paraaortic lymph node metastasis in patients with uterine cancer. Eur Radiol 19:1529–1536
Lin MY, Dobrotwir A, McNally O, Abu-Rustum NR, Narayan K (2018) Role of imaging in the routine management of endometrial cancer. Int J Gynaecol Obstet 143(Suppl 2):109–117
Van Calster B, Wynants L, Verbeek JFM, Verbakel JY, Christodoulou E, Vickers AJ, Roobol MJ, Steyerberg EW (2018) Reporting and interpreting decision curve analysis: a guide for investigators. Eur Urol 74:796–804
Acknowledgements
This study was funded by Akdeniz University Research Foundation, Antalya, Turkey (Grant number: TSA-2017–2712). The abstract of this work was presented in the 20th International Meeting of the European Society of Gynaecological Oncology (ESGO 2017), 04–07 November 2017, Vienna, Austria.
Author information
Authors and Affiliations
Contributions
SB: protocol/project development, data collection or management, data analysis, manuscript writing. TT: protocol/project development, data collection or management, data analysis, manuscript writing. HAA: data collection or management, manuscript editing. TS: manuscript editing, supervision. YY: protocol/project development, methodology, manuscript editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest and nothing to disclose.
Ethical approval
This study has been approved by the Ethics Committee of the Akdeniz University School of Medicine. This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Informed consent of patients was not obtained due to the nature of study and the obtained data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bozkurt, S., Toptas, T., Aydin, H.A. et al. A nomogram for decision-making of completion surgery in endometrial cancer diagnosed after hysterectomy. Arch Gynecol Obstet 300, 693–701 (2019). https://doi.org/10.1007/s00404-019-05223-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-019-05223-8