Abstract
Objective
In the present study, the efficacy and tolerability of the local acting antiseptic octenidine hydrochloride/phenoxyethanol (OHP) for the treatment of vaginal dysbiosis (VD) and/or bacterial vaginosis (BV) in pregnancy and its potential influence on preterm births and low-weight newborns were examined.
Methods
One-hundred nine pregnant women with increased pH values (>4.5) and BV characteristic symptoms were treated with OHP for 7 days and a second time in case of a recurrent pH increase. pH values were continuously controlled by women’s self-measurements.
Results
pH decreased to ≤4.5 in 67.9% of patients. Seven of 12 women (58.3%) treated again with OHP due to a recurrent pH increase finally reached the pH target (pH ≤ 4.5). No preterm birth occurred in the OHP group; no newborn had a birth weight <2,000 g. Rates of preterm births and low-weight newborns were comparable between OHP group and pregnant women without VD/BV.
Conclusions
OHP is effective and well tolerated in the treatment of VD/BV also in pregnancy without side effects and the occurrence of resistances. It could be an additional therapeutic option in the prevention of the multifactorial disease pattern ‘preterm birth’ with all their consequences.


Similar content being viewed by others
References
Raio L (2002) Screeninguntersuchungen auf eine drohende Frühgeburt. Gynäkologe 3:661–662
Saling E (2008) Strategien zur Frühgeburtsprävention. In: Hopp H (ed) Kontroversen in der Geburtsmedizin. Akademos Verlag, Hamburg
Nygren P, Fu R, Freeman M, Bougatsos C, Klebanoff M, Guise JM (2008) Evidence on the benefits and harms of screening and treating pregnant women who are asymptomatic for bacterial vaginosis: an update review for the US Preventive Service Task force. Ann Int Med 148:220–233
Usta IM, Nassar AH (2008) Advanced maternal age. Part I: obstetric complications. Am J Perinatol 25:521–534
Ryckman KK, Simhan HN, Krohn MA, Williams SM (2009) Cervical cytokine network patterns during pregnancy: the role of bacterial vaginosis and geographic ancestry. J Reprod Immunol 79(2):174–182
Xu J, Holzman CB, Arvidson CG, Chung H, Goepfert AR (2008) Midpregnancy vaginal fluid defensins, bacterial vaginosis, and risk of preterm delivery. Obstet Gynecol 112:524–531
Simhan HN, Krohn MA (2009) First-trimester cervical inflammatory milieu and subsequent early preterm birth. Am J Obstet Gynecol 200(4):377.e1–377.e4
Martius J, Hoyme UB; AG Infektiologie der DGGG (2006) Bakterielle Vaginose in Gynäkologie und Geburtshilfe. AWMF 015/028 guideline of the German Society of gynecology and obstetrics (Dt Ges f Gynäkologie und Geburtshilfe/DGGG), pp 1–6
Kekki M, Kurki T, Pelkonen J, Kurkinen-Räty M, Cacciatore B, Paavonen J (2001) Vaginal clindamycin in preventing preterm birth and peripartal infections in asymptomatic women with bacterial vaginosis: a randomized, controlled trial. Obstet Gynecol 97:643–648
Friese K, Neumann G, Siebert J, Harke HP, Kirschner W (2000) Vergleich zweier lokaler Antiseptika in der klinischen Anwendung bei bakteriell bedingten Vaginalinfektionen. Geburtsh Frauenheilk 60:308–313
Friese K, Neumann G, Siebert J (2002) Topical antiseptics as an alternative in the treatment of acute vulvovaginal candidosis. Arch Gynecol Obstet 268(3):194–197
Neumann G (2005) Infektionen und Infektionskrankheiten. In: Rath W, Friese K (eds) Erkrankungen in der Schwangerschaft. Georg Thieme, Stuttgart
Mendling W (2006) Vaginose, vaginitis, zervizitis und salpingitis, 2nd edn. Springer, Heidelberg
Petersen EE (2003) Infektionen in Gynäkologie und Geburtshilfe, 4th edn. Georg Thieme, Stuttgart
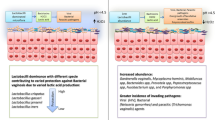
Saling E, Schreiber M (2005) Laktobazillen-Schutzsystem bei Schwangeren–effiziente Vermeidung von Frühgeburten durch Früherkennung von Störungen. Z Geburtshilfe Neonatol 209:119–127
Falagas ME, Betsi GI, Athanasiou S (2007) Probiotics for the treatment of women with bacterial vaginosis. Eur J Clin Mikrobiol Infect Dis 13:657–664
Saling E, Al-Taie T, Lüthje J (1999) Frühgeburtenvermeidungsprogramm, Zusammenarbeit zwischen Arzt, Hebamme und Patientin. Gynäkologe 32:39–45
Hoyme UB, Möller U, Saling E (2003) Aktuelle Aspekte der Thüringer Frühgeburtenvermeidungsaktion 2002. Zentralbl Gynakol 125:107–111
Msuya SE, Urivo J, Hussain A, Mbizvo EM, Jeausson S, Sam NE, Stray-Pedersen B (2009) Prevalence of sexually transmitted infections among pregnant women with known HIV status in northern Tanzania. Reprod Health 6(1):4
Bailey DM, DeGrazia CG, Hoff SJ, Schulenberg PL, O’Connor JR, Paris DA, Slee AM (1984) Bispyridinamines: a new class of topical antimicrobial agents as inhibitors of dental plaque. J Med Chem 27:1457–1464
Sedlock DM, Bailey DM (1985) Microbicidal activity of octenidine hydrochloride, a new alkanediylbis[pyridine] germicidal agent. Antimicrob Agents Chemother 28(6):786–790
Ghannoum MA, Elteen KA, Ellabib M, Whittaker PA (1990) Antimycotic effects of octenidine and pirtenidine. J Antimicrob Chemother 25(2):237–245
Neumann G (1998) Antiseptika in der therapeutischen Anwendung. Prakt Gynakol 3:223–226
Kramer A, Müller G (2008) Octenidine dihydrochloride. In: Kramer A, Assadian O (eds) Wallhäußers Praxis der Sterilisation, Desinfektion, Antiseptik und Konservierung. Thieme, Stuttgart
Goroncy-Bermes P (1998) Investigation into the efficacy of disinfectants against MRSA and VRE. Zentbl Hyg Umweltmed 201:297–309
Weissenbacher ER, Klemm A, Baumgartner L, Wachter I, Kassens E, Siebert J, Harke HP (1997) Octenisept®: study of transplacental passage in an in vitro perfusion model with human placenta (in german). Int J Exp Clin Chemother 10(4); suppl. 1
Acknowledgments
We thank Andrea Rathmann-Schmitz, Ph.D. (Bonn, Germany) for her assistance in preparing the manuscript for publication
Conflict of interest statement
The study was sponsored by the company Schuelke & Mayr. Data acquisition and statistical analysis were conducted independently.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Briese, V., Neumann, G., Waldschläger, J. et al. Efficacy and tolerability of a local acting antiseptic agent in the treatment of vaginal dysbiosis during pregnancy. Arch Gynecol Obstet 283, 585–590 (2011). https://doi.org/10.1007/s00404-010-1414-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-010-1414-4