Abstract
Introduction
Patient-specific instrumentation (PSI) utilizes three-dimensional imaging to produce total knee arthroplasty cutting jigs which matches patient’s native anatomy. However, there are limited mid- to long-term studies examining its clinical efficacy. The aim of this study was to compare functional outcomes of PSI surgery versus conventional TKA surgery at 5-year follow-up.
Materials and methods
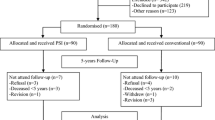
Sixty patients were prospectively recruited into either the MRI-based PSI or conventional TKA group. Functional outcomes were assessed using the Knee Society Function Score (KSFS), Knee Society Knee Score (KSKS) and Oxford Knee Score (OKS), while quality of life was evaluated with the Physical Component Score (PCS) and Mental Component Score (MCS) of Short-Form 36 and compared between the two groups at 5-year follow-up.
Results
Although the PCS was 7 ± 3 points better in the PSI group preoperatively (p = 0.017), it became 5 ± 2 points worse than the conventional group at 5-year follow-up (p = 0.025). As compared to the PSI group, the conventional group showed a significantly greater improvement in PCS at 5 years as compared to before surgery (p = 0.003). There were no significant differences in KSFS, KSKS, OKS or MCS between the two groups.
Conclusions
PSI TKA did not result in improved functional outcomes or better quality of life when compared to conventional TKA. The additional costs and waiting time associated with PSI are not justifiable and therefore not recommended as an alternative to conventional TKA.
Level of evidence
II.
Similar content being viewed by others
References
Kurtz S, Ong K, Lau E, Mowat F, Halpern M (2007) Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am 89(4):780–785
Rosenberger RE, Hoser C, Quirbach S, Attal R, Hennerbichler A, Fink C (2008) Improved accuracy of component alignment with the implementation of image-free navigation in total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 16(3):249–257
Kalairajah Y, Simpson D, Cossey AJ, Verrall GM, Spriggins AJ (2005) Blood loss after total knee replacement: effects of computer-assisted surgery. J Bone Joint Surg Br 87(11):1480–1482
Kalairajah Y, Cossey AJ, Verrall GM, Ludbrook G, Spriggins AJ (2006) Are systemic emboli reduced in computer-assisted knee surgery?: A prospective, randomised, clinical trial. J Bone Joint Surg Br 88(2):198–202
Ng VY, DeClaire JH, Berend KR, Gulick BC, Lombardi AV Jr. (2012) Improved accuracy of alignment with patient-specific positioning guides compared with manual instrumentation in TKA. Clin Orthop Relat Res 470(1):99–107
Noble JW Jr., Moore CA, Liu N (2012) The value of patient-matched instrumentation in total knee arthroplasty. J Arthroplasty 27(1):153–155
DeHaan AM, Adams JR, DeHart ML, Huff TW (2014) Patient-specific versus conventional instrumentation for total knee arthroplasty: peri-operative and cost differences. J Arthroplasty 29(11):2065–2069
Bali K, Walker P, Bruce W (2012) Custom-fit total knee arthroplasty: our initial experience in 32 knees. J Arthroplasty 27(6):1149–1154
Beal MD, Delagramaticas D, Fitz D (2016) Improving outcomes in total knee arthroplasty—do navigation or customized implants have a role? J Orthop Surg Res 11(1):60
Chauhan SK, Clark GW, Lloyd S, Scott RG, Breidahl W, Sikorski JM (2004) Computer-assisted total knee replacement. A controlled cadaver study using a multi-parameter quantitative CT assessment of alignment (the Perth CT protocol). J Bone Joint Surg Br 86(6):818–823
Kamat YD, Aurakzai KM, Adhikari AR, Matthews D, Kalairajah Y, Field RE (2009) Does computer navigation in total knee arthroplasty improve patient outcome at midterm follow-up? Int Orthop 33(6):1567–1570
Decking R, Markmann Y, Fuchs J, Puhl W, Scharf HP (2005) Leg axis after computer-navigated total knee arthroplasty: a prospective randomized trial comparing computer-navigated and manual implantation. J Arthroplasty 20(3):282–288
Anderl W, Pauzenberger L, Kolblinger R, Kiesselbach G, Brandl G, Laky B et al (2016) Patient-specific instrumentation improved mechanical alignment, while early clinical outcome was comparable to conventional instrumentation in TKA. Knee Surg Sports Traumatol Arthrosc 24(1):102–111
Kotela A, Lorkowski J, Kucharzewski M, Wilk-Franczuk M, Sliwinski Z, Franczuk B et al (2015) Patient-specific CT-based instrumentation versus conventional instrumentation in total knee arthroplasty: a prospective randomized controlled study on clinical outcomes and in-hospital data. Biomed Res Int 2015:165908
Alcelik I, Blomfield M, Ozturk C, Soni A, Charity R, Acornley A (2017) A comparison of short term radiological alignment outcomes of the patient specific and standard instrumentation for primary total knee arthroplasty: a systematic review and meta-analysis. Acta Orthop Traumatol Turc 51(3):215–222
An VV, Sivakumar BS, Phan K, Levy YD, Bruce WJ (2017) Accuracy of MRI-based vs. CT-based patient-specific instrumentation in total knee arthroplasty: a meta-analysis. J Orthop Sci 22(1):116–120
Lee GC (2016) Patient-specific cutting blocks: of unproven value. Bone Joint J 98-B(1 Suppl A):78–80
Mannan A, Akinyooye D, Hossain F (2017) A meta-analysis of functional outcomes in patient-specific instrumented knee arthroplasty. J Knee Surg 30(7):668–674
Mannan A, Smith TO (2016) Favourable rotational alignment outcomes in PSI knee arthroplasty: a level 1 systematic review and meta-analysis. Knee 23(2):186–190
Kizaki K, Shanmugaraj A, Yamashita F, Simunovic N, Duong A, Khanna V et al (2019) Total knee arthroplasty using patient-specific instrumentation for osteoarthritis of the knee: a meta-analysis. BMC Musculoskelet Disord 20(1):561
Woon JTK, Zeng ISL, Calliess T, Windhagen H, Ettinger M, Waterson HB et al (2018) Outcome of kinematic alignment using patient-specific instrumentation versus mechanical alignment in TKA: a meta-analysis and subgroup analysis of randomised trials. Arch Orthop Trauma Surg 138(9):1293–1303
Thienpont E, Schwab PE, Fennema P (2017) Efficacy of patient-specific instruments in total knee arthroplasty: a systematic review and meta-analysis. J Bone Joint Surg Am 99(6):521–530
Abane L, Anract P, Boisgard S, Descamps S, Courpied JP, Hamadouche M (2015) A comparison of patient-specific and conventional instrumentation for total knee arthroplasty: a multicentre randomised controlled trial. Bone Joint J 97-B(1):56–63
Boonen B, Schotanus MG, Kerens B, van der Weegen W, Hoekstra HJ, Kort NP (2016) No difference in clinical outcome between patient-matched positioning guides and conventional instrumented total knee arthroplasty two years post-operatively: a multicentre, double-blind, randomised controlled trial. Bone Joint J 98-B(7):939–944
Nam D, Park A, Stambough JB, Johnson SR, Nunley RM, Barrack RL (2016) The Mark Coventry Award: custom cutting guides do not improve total knee arthroplasty clinical outcomes at 2 years followup. Clin Orthop Relat Res 474(1):40–46
Ollivier M, Parratte S, Lunebourg A, Viehweger E, Argenson JN (2016) The John Insall Award: no functional benefit after unicompartmental knee arthroplasty performed with patient-specific instrumentation: a randomized trial. Clin Orthop Relat Res 474(1):60–68
Schoenmakers DAL, Schotanus MGM, Boonen B, Kort NP (2018) Consistency in patient-reported outcome measures after total knee arthroplasty using patient-specific instrumentation: a 5-year follow-up of 200 consecutive cases. Knee Surg Sports Traumatol Arthrosc 26(6):1800–1804
Insall JN, Dorr LD, Scott RD, Scott WN (1989) Rationale of the knee society clinical rating system. Clin Orthop Relat Res 248:13–14
Dawson J, Fitzpatrick R, Murray D, Carr A (1998) Questionnaire on the perceptions of patients about total knee replacement. J Bone Joint Surg Br 80(1):63–69
Ware JE Jr., Sherbourne CD (1992) The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care 30(6):473–483
Ware JE, Kosinski M, Keller SD (1994) SF-36 physical and mental summary scales: a user’s manual. Health Institute, New England Medical Center, Boston
Jenkinson C (1998) The SF-36 physical and mental health summary measures: an example of how to interpret scores. J Health Serv Res Policy 3(2):92–96
Laucis NC, Hays RD, Bhattacharyya T (2015) Scoring the SF-36 in orthopaedics: a brief guide. J Bone Joint Surg Am 97(19):1628–1634
Lee WC, Kwan YH, Chong HC, Yeo SJ (2017) The minimal clinically important difference for Knee Society Clinical Rating System after total knee arthroplasty for primary osteoarthritis. Knee Surg Sports Traumatol Arthrosc 25(11):3354–3359
Harvie P, Sloan K, Beaver RJ (2012) Computer navigation vs conventional total knee arthroplasty: five-year functional results of a prospective randomized trial. J Arthroplasty 27(5):667–72e1
Hossain FS, Konan S, Patel S, Rodriguez-Merchan EC, Haddad FS (2015) The assessment of outcome after total knee arthroplasty: are we there yet? Bone Joint J 97-B(1):3–9
Mizner RL, Petterson SC, Clements KE, Zeni JA Jr., Irrgang JJ, Snyder-Mackler L (2011) Measuring functional improvement after total knee arthroplasty requires both performance-based and patient-report assessments: a longitudinal analysis of outcomes. J Arthroplasty 26(5):728–737
Leon-Munoz VJ, Martinez-Martinez F, Lopez-Lopez M, Santonja-Medina F (2019) Patient-specific instrumentation in total knee arthroplasty. Expert Rev Med Devices 16(7):555–567
Chen JY, Yeo SJ, Yew AK, Tay DK, Chia SL, Lo NN et al (2014) The radiological outcomes of patient-specific instrumentation versus conventional total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 22(3):630–635
Wu XD, Xiang BY, Schotanus MGM, Liu ZH, Chen Y, Huang W (2017) CT- versus MRI-based patient-specific instrumentation for total knee arthroplasty: a systematic review and meta-analysis. Surgeon 15(6):336–348
Abdel MP, Parratte S, Blanc G, Ollivier M, Pomero V, Viehweger E et al (2014) No benefit of patient-specific instrumentation in TKA on functional and gait outcomes: a randomized clinical trial. Clin Orthop Relat Res 472(8):2468–2476
Pietsch M, Djahani O, Zweiger C, Plattner F, Radl R, Tschauner C et al (2013) Custom-fit minimally invasive total knee arthroplasty: effect on blood loss and early clinical outcomes. Knee Surg Sports Traumatol Arthrosc 21(10):2234–2240
Zhu M, Chen JY, Chong HC, Yew AKS, Foo LSS, Chia SL et al (2017) Outcomes following total knee arthroplasty with CT-based patient-specific instrumentation. Knee Surg Sports Traumatol Arthrosc 25(8):2567–2572
Funding
This work was supported by the FY2017 SingHealth DUKE-NUS Musculoskeletal Sciences Academic Clinical Programme Research Support Programme Grant [Project No.: 13/FY2017/P1/16-A30].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Human and animal rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by the Centralised Institutional Review Board (CIRB) (No. 2011/517/D).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Moorthy, V., Chen, J.Y., Liow, M.H.L. et al. Mid-term functional outcomes of patient-specific versus conventional instrumentation total knee arthroplasty: a prospective study. Arch Orthop Trauma Surg 141, 669–674 (2021). https://doi.org/10.1007/s00402-020-03729-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-020-03729-4