Abstract
Purpose
Local infiltration analgesia (LIA) has been proven to be efficient in total knee arthroplasty (TKA). However, the effect of single-shot LIA is temporarily limited. The objective of this prospective trial was to investigate if the potential benefits resulting from LIA can be prolonged by a continuous intra-articular perfusion of LIA. The hypothesis of the present study was that the use of an additional continuous intra-articular perfusion delivering LIA would result in less pain and better function compared to single-shot LIA in the immediate post-operative period.
Methods
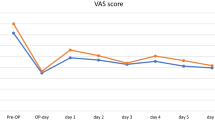
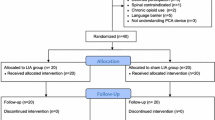
50 consecutively selected patients undergoing TKA received either a single-shot LIA (S-LIA group, 25 knees) or single-shot LIA combined with a continuous post-operative intra-articular perfusion for three post-operative days (CP-LIA group, 25 knees). VAS (visual analogue scale) for pain, pain medication consumption and flexion ability were recorded postoperatively for 6 days. All patients had the same implant, surgeon and intra- as well as post-operative setting.
Results
The VAS score was significantly better for CP-LIA 6 h after surgery and on post-operative day 1, 2 and 6. There was no significant difference with regard to additional opioid consumption or flexion ability of the knee. However, there was a trend of the CP-LIA group requiring less additional opioids over the complete post-operative period compared to the S-LIA group. There were no complications or revisions.
Conclusion
LIA combined with an additional intra-articular catheter provides better short-term pain control compared to single-shot LIA. However, no significant differences in terms of knee flexion were observed. This limited benefit should be balanced against the additional costs and the possible higher risk of infection.
Level of evidence
Level II.



Similar content being viewed by others
Abbreviations
- TKA:
-
Total knee arthroplasty
- LIA:
-
Local infiltration analgesia
- CP-LIA:
-
Continuous-perfusion local infiltration analgesia
- S-LIA:
-
Single-shot local infiltration analgesia
- ROM:
-
Range of motion
- VAS:
-
Visual analogue scale
- LMWH:
-
Low-molecular-weight heparins
References
Planckaert C, Larose G, Ranger P et al (2018) Total knee arthroplasty with unexplained pain: new insights from kinematics. Arch Orthop Trauma Surg 138:553–561. https://doi.org/10.1007/s00402-018-2873-5
Egloff C, Hügle T, Valderrabano V (2012) Biomechanics and pathomechanisms of osteoarthritis. Swiss Med Wkly 142:w13583. https://doi.org/10.4414/smw.2012.13583
Van Manen MD, Nace J, Mont MA (2012) Management of primary knee osteoarthritis and indications for total knee arthroplasty for general practitioners. J Am Osteopath Assoc 112:709–715
Michael JW-P, Schlüter-Brust KU, Eysel P (2010) The epidemiology, etiology, diagnosis, and treatment of osteoarthritis of the knee. Dtsch Arzteblatt Int 107:152–162. https://doi.org/10.3238/arztebl.2010.0152
Society KK (2012) Guidelines for the management of postoperative pain after total knee arthroplasty. Knee Surg Relat Res 24:201–207. https://doi.org/10.5792/ksrr.2012.24.4.201
Toftdahl K, Nikolajsen L, Haraldsted V et al (2007) Comparison of peri- and intraarticular analgesia with femoral nerve block after total knee arthroplasty: a randomized clinical trial. Acta Orthop 78:172–179. https://doi.org/10.1080/17453670710013645
Essving P, Axelsson K, Åberg E et al (2011) Local infiltration analgesia versus intrathecal morphine for postoperative pain management after total knee arthroplasty: a randomized controlled trial. Anesth Analg 113:926–933. https://doi.org/10.1213/ANE.0b013e3182288deb
Busch CA, Shore BJ, Bhandari R et al (2006) Efficacy of periarticular multimodal drug injection in total knee arthroplasty. A randomized trial. J Bone Joint Surg Am 88:959–963. https://doi.org/10.2106/JBJS.E.00344
Vendittoli P-A, Makinen P, Drolet P et al (2006) A multimodal analgesia protocol for total knee arthroplasty. A randomized, controlled study. J Bone Joint Surg Am 88:282–289. https://doi.org/10.2106/JBJS.E.00173
Ong JCA, Chin PL, Lin CP et al (2010) Continuous infiltration of local anaesthetic following total knee arthroplasty. J Orthop Surg Hong Kong 18:203–207. https://doi.org/10.1177/230949901001800214
Andersen KV, Bak M, Christensen BV et al (2010) A randomized, controlled trial comparing local infiltration analgesia with epidural infusion for total knee arthroplasty. Acta Orthop 81:606–610. https://doi.org/10.3109/17453674.2010.519165
Reinhardt KR, Duggal S, Umunna B-P et al (2014) Intraarticular analgesia versus epidural plus femoral nerve block after TKA: a randomized, double-blind trial. Clin Orthop 472:1400–1408. https://doi.org/10.1007/s11999-013-3351-6
Moghtadaei M, Farahini H, Faiz SH-R et al (2014) Pain management for total knee arthroplasty: single-injection femoral nerve block versus local infiltration analgesia. Iran Red Crescent Med J. https://doi.org/10.5812/ircmj.13247
Nakai T, Tamaki M, Nakamura T et al (2013) Controlling pain after total knee arthroplasty using a multimodal protocol with local periarticular injections. J Orthop 10:92–94. https://doi.org/10.1016/j.jor.2013.02.001
Carli F, Clemente A, Asenjo JF et al (2010) Analgesia and functional outcome after total knee arthroplasty: periarticular infiltration vs continuous femoral nerve block. Br J Anaesth 105:185–195. https://doi.org/10.1093/bja/aeq112
Chaumeron A, Audy D, Drolet P et al (2013) Periarticular injection in knee arthroplasty improves quadriceps function. Clin Orthop 471:2284–2295. https://doi.org/10.1007/s11999-013-2928-4
McCartney CJL, McLeod GA (2011) Local infiltration analgesia for total knee arthroplasty. Br J Anaesth 107:487–489. https://doi.org/10.1093/bja/aer255
Zhang S, Wang F, Lu ZD et al (2011) Effect of single-injection versus continuous local infiltration analgesia after total knee arthroplasty: a randomized, double-blind, placebo-controlled study. J Int Med Res 39:1369–1380. https://doi.org/10.1177/147323001103900423
Ali A, Sundberg M, Hansson U et al (2015) Doubtful effect of continuous intraarticular analgesia after total knee arthroplasty: a randomized double-blind study of 200 patients. Acta Orthop 86:373–377. https://doi.org/10.3109/17453674.2014.991629
Blendon RJ, Benson JM (2018) The public and the Opioid-abuse epidemic. N Engl J Med 378:407–411. https://doi.org/10.1056/NEJMp1714529
Iseki T, Tsukada S, Wakui M et al (2019) Percutaneous periarticular multi-drug injection at one day after total knee arthroplasty as a component of multimodal pain management: a randomized control trial. BMC Musculoskelet Disord. https://doi.org/10.1186/s12891-019-2451-1
Manchikanti L, Helm S, Fellows B et al (2012) Opioid epidemic in the United States. Pain Physician 15:ES9–38
Sabatino MJ, Kunkel ST, Ramkumar DB et al (2018) Excess opioid medication and variation in prescribing patterns following common orthopaedic procedures. J Bone Joint Surg Am 100:180–188. https://doi.org/10.2106/JBJS.17.00672
Wu L, Li M, Zeng Y et al (2020) Prevalence and risk factors for prolonged opioid use after total joint arthroplasty: a systematic review, meta-analysis, and meta-regression. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-020-03486-4
Mayr HO, Prall WC, Haasters F et al (2019) Pain relieve without impairing muscle function after local infiltration anaesthesia in primary knee arthroplasty: a prospective randomized study. Arch Orthop Trauma Surg 139:1007–1013. https://doi.org/10.1007/s00402-019-03194-8
Uesugi K, Kitano N, Kikuchi T et al (2014) Comparison of peripheral nerve block with periarticular injection analgesia after total knee arthroplasty: a randomized, controlled study. Knee 21:848–852. https://doi.org/10.1016/j.knee.2014.04.008
Spangehl MJ, Clarke HD, Hentz JG et al (2015) The Chitranjan Ranawat Award: Periarticular injections and femoral and sciatic blocks provide similar pain relief after TKA: a randomized clinical trial. Clin Orthop 473:45–53. https://doi.org/10.1007/s11999-014-3603-0
Goyal N, McKenzie J, Sharkey PF et al (2013) The 2012 Chitranjan Ranawat award: intraarticular analgesia after TKA reduces pain: a randomized, double-blinded, placebo-controlled, prospective study. Clin Orthop 471:64–75. https://doi.org/10.1007/s11999-012-2596-9
Niemeläinen M, Kalliovalkama J, Aho AJ et al (2014) Single periarticular local infiltration analgesia reduces opiate consumption until 48 hours after total knee arthroplasty. A randomized placebo-controlled trial involving 56 patients. Acta Orthop 85:614–619. https://doi.org/10.3109/17453674.2014.961399
Yuenyongviwat V, Pornrattanamaneewong C, Chinachoti T, Chareancholvanich K (2012) Periarticular injection with bupivacaine for postoperative pain control in total knee replacement: a prospective randomized double-blind controlled trial. Adv Orthop 2012:107309. https://doi.org/10.1155/2012/107309
Johnson SM, Saint John BE, Dine AP (2008) Local anesthetics as antimicrobial agents: a review. Surg Infect 9:205–213. https://doi.org/10.1089/sur.2007.036
Gómez-Cardero P, Rodríguez-Merchán EC (2010) Postoperative analgesia in TKA: ropivacaine continuous intraarticular infusion. Clin Orthop 468:1242–1247. https://doi.org/10.1007/s11999-009-1202-2
J N, V R, G C, T C (2005) Continuous Intra-Articular Infusion of Bupivacaine for Postoperative Pain Following Total Knee Arthroplasty. In: J. Knee Surg. https://pubmed.ncbi.nlm.nih.gov/16152868/. (Accessed 26 May 2020)
M M, P B, J H, et al (2020) Additional periarticular catheter shows no superiority over single-shot local infiltration analgesia alone in unicondylar knee replacement. Knee Surg Sports Traumatol Arthrosc Off J ESSKA. https://pubmed.ncbi.nlm.nih.gov/32303801/. (Accessed 26 May 2020)
Funding
No funding was received for the present study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors MM, SS, JH, CB declare that they have no conflict of interest. The author ET declares that he is providing consultancies for Convatec, KCI, LIMA, Medacta and Zimmer Biomet. He also declares that he receives royalties from LIMA, Medacta and Zimmer Biomet. He further declares that he is part of the euopean knee society board. The author JB declares that he has no conflict of interest, receives honoraria from DePuy, Conformis, Pajunk and Smith and Nephew.
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the ethic committee of the local state medical council (Approv.No. F-2017-024).
Informed consent
Informed consent was obtained from all individual participants included in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Meier, M., Sommer, S., Huth, J. et al. Local infiltration analgesia with additional intraarticular catheter provide better pain relief compared to single-shot local infiltration analgesia in TKA. Arch Orthop Trauma Surg 141, 105–111 (2021). https://doi.org/10.1007/s00402-020-03606-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-020-03606-0