Abstract
Background
Periprosthetic joint infection (PJI) is one of the most serious complications following total knee arthroplasty (TKA). However, the diagnosis remains a challenge for clinicians. In 2011, the muscoskeletal infection society (MSIS) criteria provided a consensus which has been updated in 2013, but these criteria are complex and contain tests that are time-consuming. The same is applicable to the pro-Implant guidelines. Therefore, a simpler diagnostic test is desirable.
Objectives
The value of neutrophil gelatinase-associated lipocalin (NGAL), leucocyte esterase (LE) levels, and the white blood cell (WBC) count in synovial fluid to diagnose PJI after TKA was evaluated.
Methods
In a retrospective cohort study, we analyzed 89 synovial fluid samples from 86 patients with suspected PJI after TKA. Thirteen and 23 of those samples were classified as PJI according to the MSIS and pro-Implant criteria, respectively. Subsequently, NGAL, LE levels, and the WBC count were determined, the former one using an immunoassay. Using either the MSIS or pro-Implant criteria as the golden standard for PJI, sensitivity and specificity of those markers were determined with ROC curves, and medians were compared with Mann–Whitney U and Pearson Chi-square tests.
Results
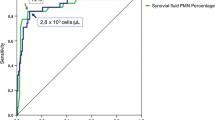
When applying the MSIS criteria, NGAL revealed 92% sensitivity and 83% specificity. WBC count showed similar sensitivity (92%) and specificity (84%), whereas sensitivity and specificity for LE were 39% and 88% respectively. When applying the pro-Implant criteria, sensitivity was 95% and specificity was 95% for NGAL. Sensitivity and specificity for WBC count were 100% and 97% and for LE 39% and 92% respectively.
Conclusion
NGAL and WBC count in synovial fluid has high accuracy in the diagnosis of PJI after TKA and should seriously be considered as part of PJI diagnostics. Leucocyte esterase can serve as rule-in criterion peroperatively. These conclusions are independent of which criteria set was used as golden standard.


Similar content being viewed by others
References
Perfetti DC, Boylan MR, Naziri Q et al (2017) Have periprosthetic hip infection rates plateaued? J Arthroplast 32:2244–2247. https://doi.org/10.1016/j.arth.2017.02.027
Boelch SP, Jakuscheit A, Doerries S et al (2018) Periprosthetic infection is the major indication for TKA revision: experiences from a university referral arthroplasty center. BMC Musculoskelet Disord 19:395. https://doi.org/10.1186/s12891-018-2314-1
Parvizi J, Zmistowski B, Berbari EF et al (2011) New definition for periprosthetic joint infection: from the workgroup of the musculoskeletal infection society. Clin Orthop Relat Res 469:2992–2994. https://doi.org/10.1007/s11999-011-2102-9
Parvizi J, Gehrke T, Chen AF (2013) Proceedings of the international consensus on periprosthetic joint infection. Bone Jt J 95-B:1450–1452. https://doi.org/10.1302/0301-620X.95B11.33135
Sigmund IK, Holinka J, Gamper J et al (2017) Qualitative ? α -defensin test (Synovasure) for the diagnosis of periprosthetic infection in revision total joint arthroplasty. Bone Jt J 99-B:66–72. https://doi.org/10.1302/0301-620X.99B1.BJJ-2016-0295.R1
Trampuz A (2018) Pocket guide to diagnosis & treatment of periprosthetic joint infection (PJI)
Renz N, Yermak K, Perka C, Trampuz A (2018) Alpha defensin lateral flow test for diagnosis of. J Bone Jt Surg Am 100:742–750. https://doi.org/10.2106/JBJS.17.01005
Fink B, Steurer M, Hofäcker S et al (2018) Preoperative PCR analysis of synovial fluid has limited value for the diagnosis of periprosthetic joint infections of total knee arthroplasties. Arch Orthop Trauma Surg 138:871–878. https://doi.org/10.1007/s00402-018-2924-y
Pérez-Prieto D, Portillo ME, Puig-Verdié L et al (2017) C-reactive protein may misdiagnose prosthetic joint infections particularly chronic and low-grade infections. Int Orthop 41:1315–1319. https://doi.org/10.1007/s00264-017-3430-5
Wang C, Li R, Wang Q, Wang C (2018) Synovial fluid leukocyte esterase in the diagnosis of peri-prosthetic joint infection: a systematic review and meta-analysis. Surg Infect (Larchmt) 19:245–253. https://doi.org/10.1089/sur.2017.192
Shahi A, Tan TL, Kheir MM et al (2017) Diagnosing periprosthetic joint infection: and the winner is? J Arthroplast 32:S232–S235. https://doi.org/10.1016/j.arth.2017.06.005
Deirmengian C, Kardos K, Kilmartin P et al (2014) Diagnosing periprosthetic joint infection: has the era of the biomarker arrived? Clin Orthop Relat Res 472:3254–3262. https://doi.org/10.1007/s11999-014-3543-8
Lee YS, Koo K-H, Kim HJ et al (2017) Synovial fluid biomarkers for the diagnosis of periprosthetic joint infection. J Bone Jt Surg 99:2077–2084. https://doi.org/10.2106/JBJS.17.00123
Gómez AV, Fernández-Pittol MJ, Muñoz-Mahamud E et al (2018) Evaluation of Lipocalin-2 as a biomarker of periprosthetic joint infection. J Arthroplast. https://doi.org/10.1016/j.arth.2018.09.047
Schmidt-Ott KM, Mori K, Li JY et al (2007) Dual action of neutrophil gelatinase-associated lipocalin. J Am Soc Nephrol 18:407–413. https://doi.org/10.1681/ASN.2006080882
Nairz M, Haschka D, Demetz E, Weiss G (2014) Iron at the interface of immunity and infection. Front Pharmacol 5:1–10. https://doi.org/10.3389/fphar.2014.00152
Salvagno GL, Ferrari A, Gelati M et al (2017) Analytical validation of Gentian NGAL particle-enhanced enhanced turbidimetric immunoassay (PETIA). Pract Lab Med 8:60–64. https://doi.org/10.1016/j.plabm.2017.04.006
Vergara A, Fernández-Pittol MJ, Muñoz-Mahamud E et al (2019) Evaluation of Lipocalin-2 as a biomarker of periprosthetic joint infection. J Arthroplast 34:123–125. https://doi.org/10.1016/j.arth.2018.09.047
Balato G, Franceschini V, Ascione T et al (2018) Diagnostic accuracy of synovial fluid, blood markers, and microbiological testing in chronic knee prosthetic infections. Arch Orthop Trauma Surg 138:165–171. https://doi.org/10.1007/s00402-017-2832-6
Sebastian S, Malhotra R, Sreenivas V et al (2018) Sonication of orthopaedic implants: a valuable technique for diagnosis of prosthetic joint infections. J Microbiol Methods 146:51–54. https://doi.org/10.1016/j.mimet.2018.01.015
Berbari E, Mabry T, Tsaras G et al (2010) Inflammatory blood laboratory levels as markers of prosthetic joint infection: a systematic review and meta-analysis. J Bone Jt Surg Ser A 92:2102–2109. https://doi.org/10.2106/JBJS.I.01199
Deirmengian C, Hallab N, Tarabishy A et al (2010) Synovial fluid biomarkers for periprosthetic infection. Clin Orthop Relat Res 468:2017–2023. https://doi.org/10.1007/s11999-010-1298-4
Funding
This study was financed by the Amphia hospital science funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This retrospective study does not contain any studies with human participants that require ethical approval in our country.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dijkman, C., Thomas, A.R., Koenraadt, K.L.M. et al. Synovial neutrophilic gelatinase-associated lipocalin in the diagnosis of periprosthetic joint infection after total knee arthroplasty. Arch Orthop Trauma Surg 140, 941–947 (2020). https://doi.org/10.1007/s00402-020-03427-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-020-03427-1