Abstract
Introduction
The objective of this study was to evaluate the temporal expression pattern of three different growth factors (VEGF, IL-1β, and TGF-1β) in a supraspinatus tendon lesion in an animal model. The hypothesis of this study is that there are variations in the expression of these factors in the first 8 weeks after injury.
Materials and methods
A full thickness defect was made in the supraspinatus tendon of 40 rat shoulders. The animal were sacrificed at 0, 3, 7, 14 and 56 days after injury and three tissue samples were obtained: bone from the tendon footprint; the supraspinatus tendon stump, and a fragment of the myotendinous junction. After mRNA extraction, quantitative PCR analysis was performed, and the expression of three different growth factors were evaluated in each zone.
Results
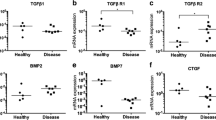
There was an increased expression of IL-1β during the first week after injury at all levels evaluated with a clear peak in the first day after injury. There was also a significant increase in TGF-1β expression levels all along the first week in the three zones. There were no variations in VEGF expression in the three zones along the 8 weeks.
Conclusion
IL-1β was expressed predominantly in the initial stages after injury; TGF initiated its expression after the initial phase since day three, whereas VEGF remained basically unchanged during the entire process.



Similar content being viewed by others
References
Yamaguchi K, Ditsios K, Middleton WD, Hildebolt CF, Galatz LM, Teefey SA (2006) The demographic and morphological features of rotator cuff disease. A comparison of asymptomatic and symptomatic shoulders. J Bone Jt Surg Am 88(8):1699–1704. doi:10.2106/JBJS.E.00835
Harryman DT 2nd, Hettrich CM, Smith KL, Campbell B, Sidles JA, Matsen FA 3rd (2003) A prospective multipractice investigation of patients with full-thickness rotator cuff tears: the importance of comorbidities, practice, and other covariables on self-assessed shoulder function and health status. J Bone Jt Surg Am 85-A(4):690–696
Park MC, ElAttrache NS, Tibone JE, Ahmad CS, Jun BJ, Lee TQ (2007) Part I: footprint contact characteristics for a transosseous-equivalent rotator cuff repair technique compared with a double-row repair technique. J Shoulder Elb Surg 16(4):461–468. doi:10.1016/j.jse.2006.09.010
Duquin TR, Buyea C, Bisson LJ (2010) Which method of rotator cuff repair leads to the highest rate of structural healing? A systematic review. Am J Sports Med 38(4):835–841. doi:10.1177/0363546509359679
Bishop J, Klepps S, Lo IK, Bird J, Gladstone JN, Flatow EL (2006) Cuff integrity after arthroscopic versus open rotator cuff repair: a prospective study. J Shoulder Elb Surg 15(3):290–299. doi:10.1016/j.jse.2005.09.017
Tashjian RZ, Hollins AM, Kim HM, Teefey SA, Middleton WD, Steger-May K, Galatz LM, Yamaguchi K (2010) Factors affecting healing rates after arthroscopic double-row rotator cuff repair. Am J Sports Med 38(12):2435–2442. doi:10.1177/0363546510382835
Kim HM, Caldwell JM, Buza JA, Fink LA, Ahmad CS, Bigliani LU, Levine WN (2014) Factors affecting satisfaction and shoulder function in patients with a recurrent rotator cuff tear. J Bone Jt Surg Am 96(2):106–112. doi:10.2106/JBJS.L.01649
Eljabu W, Klinger HM, von Knoch M (2015) The natural history of rotator cuff tears: a systematic review. Arch Orthop Trauma Surg 135(8):1055–1061. doi:10.1007/s00402-015-2239-1
Baums MH, Schminke B, Posmyk A, Miosge N, Klinger HM, Lakemeier S (2015) Effect of single- and double-row rotator cuff repair at the tendon-to-bone interface: preliminary results using an in vivo sheep model. Arch Orthop Trauma Surg 135(1):111–118. doi:10.1007/s00402-014-2118-1
Kovacevic D, Rodeo SA (2008) Biological augmentation of rotator cuff tendon repair. Clin Orthop Relat Res 466(3):622–633. doi:10.1007/s11999-007-0112-4
Shen C, Tang ZH, Hu JZ, Zou GY, Xiao RC, Yan DX (2014) Does immobilization after arthroscopic rotator cuff repair increase tendon healing? A systematic review and meta-analysis. Arch Orthop Trauma Surg 134(9):1279–1285. doi:10.1007/s00402-014-2028-2
Bennett NT, Schultz GS (1993) Growth factors and wound healing: biochemical properties of growth factors and their receptors. Am J Surg 165(6):728–737
Molloy T, Wang Y, Murrell G (2003) The roles of growth factors in tendon and ligament healing. Sports Med 33(5):381–394. doi:10.2165/00007256-200333050-00004
Thomopoulos S, Williams GR, Gimbel JA, Favata M, Soslowsky LJ (2003) Variation of biomechanical, structural, and compositional properties along the tendon to bone insertion site. J Orthop Res 21(3):413–419. doi:10.1016/S0736-0266(03)00057-3
Pfaffl MW (2001) A new mathematical model for relative quantification in real-time RT-PCR. Nucleic Acids Res 29(9):e45
Hamada K, Fukuda H, Mikasa M, Kobayashi Y (1990) Roentgenographic findings in massive rotator cuff tears. A long-term observation. Clin Orthop Relat Res 254:92–96
Yamanaka K, Matsumoto T (1994) The joint side tear of the rotator cuff. A followup study by arthrography. Clin Orthop Relat Res 304:68–73
Deniz G, Kose O, Tugay A, Guler F, Turan A (2014) Fatty degeneration and atrophy of the rotator cuff muscles after arthroscopic repair: does it improve, halt or deteriorate? Arch Orthop Trauma Surg 134(7):985–990. doi:10.1007/s00402-014-2009-5
Lopez-Vidriero E, Goulding KA, Simon DA, Sanchez M, Johnson DH (2010) The use of platelet-rich plasma in arthroscopy and sports medicine: optimizing the healing environment. Arthroscopy 26(2):269–278. doi:10.1016/j.arthro.2009.11.015
Randelli P, Arrigoni P, Ragone V, Aliprandi A, Cabitza P (2011) Platelet rich plasma in arthroscopic rotator cuff repair: a prospective RCT study, 2-year follow-up. J Shoulder Elb Surg 20(4):518–528. doi:10.1016/j.jse.2011.02.008
Dolkart O, Chechik O, Zarfati Y, Brosh T, Alhajajra F, Maman E (2014) A single dose of platelet-rich plasma improves the organization and strength of a surgically repaired rotator cuff tendon in rats. Arch Orthop Trauma Surg 134(9):1271–1277. doi:10.1007/s00402-014-2026-4
Soslowsky LJ, Carpenter JE, DeBano CM, Banerji I, Moalli MR (1996) Development and use of an animal model for investigations on rotator cuff disease. J Shoulder Elbow Surg 5(5):383–392. doi:10.1016/S1058-2746(96)80070-X
Becker R, Pufe T, Kulow S, Giessmann N, Neumann W, Mentlein R, Petersen W (2004) Expression of vascular endothelial growth factor during healing of the meniscus in a rabbit model. J Bone Jt Surg Br 86(7):1082–1087
Lakemeier S, Reichelt JJ, Patzer T, Fuchs-Winkelmann S, Paletta JR, Schofer MD (2010) The association between retraction of the torn rotator cuff and increasing expression of hypoxia inducible factor 1alpha and vascular endothelial growth factor expression: an immunohistological study. BMC Musculoskelet Disord 11:230. doi:10.1186/1471-2474-11-230
Savitskaya YA, Izaguirre A, Sierra L, Perez F, Cruz F, Villalobos E, Almazan A, Ibarra C (2011) Effect of angiogenesis-related cytokines on rotator cuff disease: the search for sensitive biomarkers of early tendon degeneration. Clin Med Insights Arthritis Musculoskelet Disord 4:43–53. doi:10.4137/CMAMD.S7071
Yanagisawa K, Hamada K, Gotoh M, TokunagaT Oshika Y, Tomisawa M, Lee YH, Handa A, Kijima H, Yamazaki H, Nakamura M, Ueyama Y, Tamaoki N, Fukuda H (2001) Vascular endothelial growth factor (VEGF) expression in the subacromial bursa is increased in patients with impingement syndrome. J Orthop Res 19(3):448–455. doi:10.1016/S0736-0266(00)90021-4
Chan BP, Chan KM, Maffulli N, Webb S, Lee KK (1997) Effect of basic fibroblast growth factor. An in vitro study of tendon healing. Clin Orthop Relat Res 342:239–247
Klein MB, Yalamanchi N, Pham H, Longaker MT, Chang J (2002) Flexor tendon healing in vitro: effects of TGF-beta on tendon cell collagen production. J Hand Surg Am 27(4):615–620. doi:10.1053/jhsu.2002.34004
Anaguchi Y, Yasuda K, Majima T, Tohyama H, Minami A, Hayashi K (2005) The effect of transforming growth factor-beta on mechanical properties of the fibrous tissue regenerated in the patellar tendon after resecting the central portion. Clin Biomech (Bristol, Avon) 20(9):959–965. doi:10.1016/j.clinbiomech.2005.05.012
Galatz LM, Sandell LJ, Rothermich SY, Das R, Mastny A, Havlioglu N, Silva MJ, Thomopoulos S (2006) Characteristics of the rat supraspinatus tendon during tendon-to-bone healing after acute injury. J Orthop Res 24(3):541–550. doi:10.1002/jor.20067
Lui P, Zhang P, Chan K, Qin L (2010) Biology and augmentation of tendon-bone insertion repair. J Orthop Surg Res 5:59. doi:10.1186/1749-799X-5-59
Tsubone T, Moran SL, Amadio PC, Zhao C, An KN (2004) Expression of growth factors in canine flexor tendon after laceration in vivo. Ann Plast Surg 53(4):393–397. doi:10.1097/01.sap.0000125501.72773.01
Kobayashi M, Itoi E, Minagawa H, Miyakoshi N, Takahashi S, Tuoheti Y, Okada K, Shimada Y (2006) Expression of growth factors in the early phase of supraspinatus tendon healing in rabbits. J Shoulder Elb Surg 15(3):371–377. doi:10.1016/j.jse.2005.09.003
Wurgler-Hauri CC, Dourte LM, Baradet TC, Williams GR, Soslowsky LJ (2007) Temporal expression of 8 growth factors in tendon-to-bone healing in a rat supraspinatus model. J Shoulder Elb Surg 16(5 Suppl):S198–S203. doi:10.1016/j.jse.2007.04.003
Kovacevic D, Fox AJ, Bedi A, Ying L, Deng XH, Warren RF, Rodeo SA (2011) Calcium-phosphate matrix with or without TGF-beta3 improves tendon-bone healing after rotator cuff repair. Am J Sports Med 39(4):811–819. doi:10.1177/0363546511399378
Manning CN, Kim HM, Sakiyama-Elbert S, Galatz LM, Havlioglu N, Thomopoulos S (2011) Sustained delivery of transforming growth factor beta three enhances tendon-to-bone healing in a rat model. J Orthop Res 29(7):1099–1105. doi:10.1002/jor.21301
Kim HM, Galatz LM, Das R, Havlioglu N, Rothermich SY, Thomopoulos S (2011) The role of transforming growth factor beta isoforms in tendon-to-bone healing. Connect Tissue Res 52(2):87–98. doi:10.3109/03008207.2010.483026
van de Loo AA, Arntz OJ, Bakker AC, van Lent PL, Jacobs MJ, van den Berg WB (1995) Role of interleukin 1 in antigen-induced exacerbations of murine arthritis. Am J Pathol 146(1):239–249
Wilusz RE, Weinberg JB, Guilak F, McNulty AL (2008) Inhibition of integrative repair of the meniscus following acute exposure to interleukin-1 in vitro. J Orthop Res 26(4):504–512. doi:10.1002/jor.20538
Gotoh M, Hamada K, Yamakawa H, Yanagisawa K, Nakamura M, Yamazaki H, Ueyama Y, Tamaoki N, Inoue A, Fukuda H (2001) Interleukin-1-induced subacromial synovitis and shoulder pain in rotator cuff diseases. Rheumatology (Oxford) 40(9):995–1001
Koshima H, Kondo S, Mishima S, Choi HR, Shimpo H, Sakai T, Ishiguro N (2007) Expression of interleukin-1beta, cyclooxygenase-2, and prostaglandin E2 in a rotator cuff tear in rabbits. J Orthop Res 25(1):92–97. doi:10.1002/jor.20241
Blaine TA, Cote MA, Proto A, Mulcahey M, Lee FY, Bigliani LU (2011) Interleukin-1beta stimulates stromal-derived factor-1alpha expression in human subacromial bursa. J Orthop Res 29(11):1695–1699. doi:10.1002/jor.21416
Acknowledgments
Approved by Dña Ana Isabel Ortiz Chercoles, Presidenta Comité Bienestar Animal (CEBA) Hospital Ramón y Cajal Madrid Spain.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We have no conflicts of interest to disclose.
Rights and permissions
About this article
Cite this article
Díaz Heredia, J., Ruiz Iban, M.A., Martínez-Botas, J. et al. Growth factor expression after supraspinatus tear: a quantitative polymerase chain reaction (PCR) study in rats. Arch Orthop Trauma Surg 136, 1563–1570 (2016). https://doi.org/10.1007/s00402-016-2518-5
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-016-2518-5