Abstract
Background
The ideal treatment for juvenile osteochondritis dissecans of the talus (ODT) is still unclear. To determine predictors of failure of conservative treatment, children admitted for ODT were retrospectively analyzed.
Methods
Patient files were analyzed to search for children treated for an ODT between 2000 and 2011. X-rays and MRI at baseline were evaluated for grading of lesions and the patient history was obtained. Final follow-up evaluation was performed via questionnaire and complementary telephone interview. Outcome was measured using the AOFAS and the Olerud/Molander scores. Conservative treatment consisted of out of sports and modification of activity under full weight-bearing. In case of persisting pain, full load removal on crutches was initiated. For further analysis, two groups were formed: (1) successful conservative treatment; (2) converted to surgical therapy. A logistic regression was used to determine potential predictors of conservative treatment failure.
Results
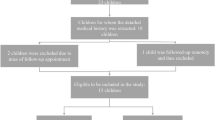
Seventy-seven lesions in 67 children with a mean age of 11.4 years (range 4–15 years) at the time of diagnosis were identified. Every patient received conservative treatment as a first-line treatment after diagnosis of ODT except for one single patient with a grade IV lesion at time of diagnosis who received operative treatment directly after diagnosis. Sixty-one percent of the lesions failed conservative treatment. A higher age as well as a grade III lesion at time of diagnosis was predictive for failure of the conservative treatment (p = 0.03 and p = 0.02, respectively). Regarding the functional outcome, a higher grade lesion in general was predictive for an inferior outcome as measured by clinical score.
Conclusion
Grade III ODT especially in older children leads significantly more often to treatment failure when treated non-surgically. No other predictors for treatment failure could be identified.
Level of evidence
Level III (retrospective comparative study).

Similar content being viewed by others
References
Higuera J, Laguna R, Peral M, Aranda E, Soleto J (1998) Osteochondritis dissecans of the talus during childhood and adolescence. J Pediatr Orthop 18:328–332
Letts M, Davidson D, Ahmer A (2003) Osteochondritis dissecans of the talus in children. J Pediatr Orthop 23:617–625
Perumal V, Wall E, Babekir N (2007) Juvenile osteochondritis dissecans of the talus. J Pediatr Orthop 27:821–825. doi:10.1097/BPO.0b013e3181558961
Flick AB, Gould N (1985) Osteochondritis dissecans of the talus (transchondral fractures of the talus): review of the literature and new surgical approach for medial dome lesions. Foot Ankle. 5:165–185
Verhagen RA, Struijs PA, Bossuyt PM, van Dijk CN (2003) Systematic review of treatment strategies for osteochondral defects of the talar dome. Foot Ankle Clin 8:233–242, viii–ix
Berndt AL, Harty M (1959) Transchondral fractures (osteochondritis dissecans) of the talus. J Bone Joint Surg Am. 41-A:988–1020
Canale ST, Belding RH (1980) Osteochondral lesions of the talus. J Bone Joint Surg Am 62:97–102
Mubarak SJ, Carroll NC (1979) Familial osteochondritis dissecans of the knee. Clin Orthop Relat Res. 140:131–136
Woods K, Harris I (1995) Osteochondritis dissecans of the talus in identical twins. J Bone Joint Surg Br 77:331
Lam KY, Siow HM (2012) Conservative treatment for juvenile osteochondritis dissecans of the talus. J Orthop Surg (Hong Kong). 20:176–180
Kramer J, Stiglbauer R, Engel A, Prayer L, Imhof H (1992) MR contrast arthrography (MRA) in osteochondrosis dissecans. J Comput Assist Tomogr 16:254–260
Olerud C, Molander H (1984) A scoring scale for symptom evaluation after ankle fracture. Arch Orthop Trauma Surg 103:190–194
Kitaoka HB, Alexander IJ, Adelaar RS, Nunley JA, Myerson MS, Sanders M (1994) Clinical rating systems for the ankle-hindfoot, midfoot, hallux, and lesser toes. Foot Ankle Int 15:349–353
Yonetani Y, Nakamura N, Natsuume T, Shiozaki Y, Tanaka Y, Horibe S (2010) Histological evaluation of juvenile osteochondritis dissecans of the knee: a case series. Knee Surg Sports Traumatol Arthrosc 18:723–730. doi:10.1007/s00167-009-0898-6
Kramer DE, Glotzbecker MP, Shore BJ, Zurakowski D, Yen YM, Kocher MS et al (2014) Results of surgical management of osteochondritis dissecans of the ankle in the pediatric and adolescent population. J Pediatr Orthop. doi:10.1097/BPO.0000000000000352
Rosenfeld SB, Herring JA, Chao JC (2007) Legg-calve-perthes disease: a review of cases with onset before six years of age. J Bone Joint Surg Am 89:2712–2722. doi:10.2106/JBJS.G.00191
Salter RB, Thompson GH (1984) Legg-Calve-Perthes disease. The prognostic significance of the subchondral fracture and a two-group classification of the femoral head involvement. J Bone Joint Surg Am 66:479–489
Ippolito E, Tudisco C, Farsetti P (1987) The long-term prognosis of unilateral Perthes’ disease. J Bone Joint Surg Br 69:243–250
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Heyse, T.J., Schüttler, K.F., Schweitzer, A. et al. Juvenile osteochondritis dissecans of the talus: predictors of conservative treatment failure. Arch Orthop Trauma Surg 135, 1337–1341 (2015). https://doi.org/10.1007/s00402-015-2260-4
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-015-2260-4