Abstract
Introduction
The use of tourniquet in total knee arthroplasty (TKA) has resulted in negligible intra-operative blood loss but notable post-operative blood loss, creating the ideal scenario for using topical haemostatic agents intra-operatively. Recently, medical adjuvants including tranexamic acid (TXA) and hydrogen peroxide (H2O2) have been introduced. The aim of this study was to evaluate the effectiveness of intra-articular TXA and H2O2 in reducing blood loss during TKA.
Materials and methods
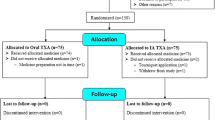
Fifty patients, who underwent a primary TKA with 1,500 mg of intra-articular TXA between May 2011 and December 2011, were compared with two matching cohorts of 50 patients each who underwent TKA with 100 ml of 3 % H2O2 wash and TKA without any TXA or H2O2. All surgeries were performed by two senior surgeons. The total blood loss was calculated by the hemoglobin balance method.
Results
The pre-operative serum hemoglobin levels were 13.1 ± 1.3, 13.1 ± 1.3 and 13.0 ± 1.2 g/dl (p > 0.05); while the drop in serum hemoglobin levels post-operatively was 2.0 ± 0.7, 2.4 ± 0.9 and 2.7 ± 0.8 g/dl for the TXA, H2O2 and Control groups, respectively (p < 0.001). The total amount of blood loss was 596 ± 449, 710 ± 279 and 760 ± 228 ml, respectively (p = 0.046). There was no difference in the duration of surgery between the three groups (p > 0.05).
Conclusions
This study showed that intra-articular TXA reduced blood loss during TKA without significantly increasing the duration of surgery. We cannot justify H2O2 wash as an alternative to intra-articular TXA to reduce blood loss during TKA.
Similar content being viewed by others
References
Abrishami A, Chung F, Wong J (2009) Topical application of antifibrinolytic drugs for on-pump cardiac surgery: a systematic review and meta-analysis. Can J Anaesth 56(3):202–212
Good L, Peterson E, Lisander B (2003) Tranexamic acid decreases external blood loss but not hidden blood loss in total knee replacement. Br J Anaesth 90(5):596–599
Hippala S, Strid L, Wennerstrand M, Arvela V, Mantyla S, Ylinen J, Niemelä H (1995) Tranexamic acid (Cyklokapron) reduces perioperative blood loss associated with total knee arthroplasty. Br J Anaesth 74(5):534–537
Kalairajah Y, Simpson D, Cossey AJ, Verrall GM, Spriggins AJ (2005) Blood loss after total knee replacement: effects of computer-assisted surgery. J Bone Joint Surg Br 87(11):1480–1482
Fiebig E (1998) Safety of the blood supply. Clin Orthop Relat Res 357:6–18
Parvizi J, Chaudhry S, Rasouli MR, Pulido L, Joshi A, Herman JH, Rothman RH (2011) Who needs autologous blood donation in joint replacement? J Knee Surg 24(1):25–31
Juelsgaard P, Larsen UT, Sorensen JV, Madsen F, Soballe K (2001) Hypotensive epidural anesthesia in total knee replacement without tourniquet: reduced blood loss and transfusion. Reg Anesth Pain Med 26(2):105–110
Levy O, Martinowitz U, Oran A, Tauber C, Horoszowski H (1999) The use of fibrin tissue adhesive to reduce blood loss and the need for blood transfusion after total knee arthroplasty. A prospective, randomized, multicenter study. J Bone Joint Surg Am 81(11):1580–1588
Onodera T, Majima T, Sawaguchi N, Kasahara Y, Ishigaki T, Minami A (2012) Risk of deep venous thrombosis in drain clamping with tranexamic acid and carbazochrome sodium sulfonate hydrate in total knee arthroplasty. J Arthroplast 27(1):105–108
Lange DR (1979) The mechanical bonding of methylmethacrylate to cancellous bone: effects of a hemostatic agent. J Bone Joint Surg Am 61(2):254–256
Benoni G, Fredin H (1996) Fibrinolytic inhibition with tranexamic acid reduces blood loss and blood transfusion after knee arthroplasty: a prospective, randomised, double-blind study of 86 patients. J Bone Joint Surg Br 78(3):434–440
Camarasa MA, Ollé G, Serra-Prat M, Martín A, Sánchez M, Ricós P, Pérez A, Opisso L (2006) Efficacy of aminocaproic, tranexamic acids in the control of bleeding during total knee replacement: a randomized clinical trial. Br J Anaesth 96(5):576–582
Maniar RN, Kumar G, Singhi T, Nayak RM, Maniar PR (2012) Most effective regimen of tranexamic acid in knee arthroplasty: a prospective randomized controlled study in 240 patients. Clin Orthop Relat Res 470(9):2605–2612
Sa-Ngasoongsong P, Channoom T, Kawinwonggowit V, Woratanarat P, Chanplakorn P, Wibulpolprasert B, Wongsak S, Udomsubpayakul U, Wechmongkolgorn S, Lekpittaya N (2011) Postoperative blood loss reduction in computer-assisted surgery total knee replacement by low dose intra-articular tranexamic acid injection together with 2-hour clamp drain: a prospective triple-blinded randomized controlled trial. Orthop Rev (Pavia) 3(2):e12
Roy SP, Tanki UF, Dutta A, Jain SK, Nagi ON (2012) Efficacy of intra-articular tranexamic acid in blood loss reduction following primary unilateral total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 20(12):2494–2501
Seo JG, Moon YW, Park SH, Kim SM, Ko KR (2013) The comparative efficacies of intra-articular and IV tranexamic acid for reducing blood loss during total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 21(8):1869–1874
Wong J, Abrishami A, El Beheiry H, Mahomed NN, Roderick Davey J, Gandhi R, Syed KA, Muhammad Ovais Hasan S, De Silva Y, Chung F (2010) Topical application of tranexamic acid reduces postoperative blood loss in total knee arthroplasty: a randomized, controlled trial. J Bone Joint Surg Am 92(15):2503–2513
Mongan PD, Brown RS, Thwaites BK (1998) Tranexamic acid and aprotinin reduce postoperative bleeding and transfusions during primary coronary revascularization. Anaesth Analg 87(2):258–265
Boylan JF, Klinck JR, Sandler AN, Arellano R, Greig PD, Nierenberg H, Roger SL, Glynn MF (1996) Tranexamic acid reduces blood loss, transfusion requirements, and coagulation factor use in primary orthotopic liver transplantation. Anesthesiology 85(5):1043–1048
Wellington K, Wagstaff AJ (2003) Tranexamic acid: a review of its use in the management of menorrhagia. Drugs 63(13):1417–1433
McCormack PL (2012) Tranexamic acid: a review of its use in the treatment of hyperfibrinolysis. Drugs 72(5):585–617
Bannister GC, Young SK, Baker AS, Mackinnon JG, Magnusson PA (1990) Control of bleeding in cemented arthroplasty. J Bone Joint Surg Br 72(3):444–446
Hankin FM, Campbell SE, Goldstein SA, Matthews LS (1984) Hydrogen peroxide as a topical hemostatic agent. Clin Orthop Relat Res 186:244–248
Howells RJ, Salmon JM, McCullough KG (1992) The effect of irrigating solutions on the strength of the cement-bone interface. Aust NZ J Surg 62(3):215–218
Lisander B, Ivarsson I, Jacobsson SA (1998) Intraoperative autotransfusion is associated with modest reduction of allogeneic transfusion in prosthetic hip surgery. Acta Anaesthesiol Scand 42(6):707–712
Nadler SB, Hidalgo JU, Bloch T (1962) Prediction of blood volume in normal human adults. Surgery 51(4):224–232
Fahmy NR, Patel DG (1981) Hemostatic changes and postoperative deep-vein thrombosis associated with use of a pneumatic tourniquet. J Bone Joint Surg Am 63(3):461–465
Langdown AJ, Field J, Grote J, Himayat H (2000) Aprotinin (Trasylol) does not reduce bleeding in primary total hip arthroplasty. J Arthroplast 15(8):1009–1012
Ishida K, Tsumura N, Kitagawa A, Hamamura S, Fukuda K, Dogaki Y, Kubo S, Matsumoto T, Matsushita T, Chin T, Iguchi T, Kurosaka M, Kuroda R (2011) Intra-articular injection of tranexamic acid reduces not only blood loss but also knee joint swelling after total knee arthroplasty. Int Orthop 35(11):1639–1645
Hiippala ST, Strid LJ, Wennerstrand MI, Arvela JV, Niemela HM, Mantyla SK, Kuisma RP, Ylinen JE (1997) Tranexamic acid radically decreases blood loss and transfusions associated with total knee arthroplasty. Anesth Analg 84(4):839–844
Krohn CD, Sorensen R, Lange JE, Riise R, Bjornsen S, Brosstad F (2003) Tranexamic acid given into the wound reduces post-operative blood loss by half in major orthopaedic surgery. Eur J Surg 588:57–61
Molloy DO, Archbold HA, Ogonda L, McConway J, Wilson RK, Beverland DE (2007) Comparison of topical fibrin spray and tranexamic acid on blood loss after total knee replacement: a prospective, randomised controlled trial. J Bone Joint Surg Br 89(3):306–309
Kagoma YK, Crowther MA, Douketis J, Bhandari M, Eikelboom J, Lim W (2009) Use of antifibrinolytic therapy to reduce transfusion in patients undergoing orthopedic surgery: a systematic review of randomized trials. Thromb Res 123(5):687–696
Cid J, Lozano M (2005) Tranexamic acid reduces allogeneic red cell transfusions in patients undergoing total knee arthroplasty: results of a meta-analysis of randomized controlled trials. Transfusion 45(8):1302–1307
Watt BE, Proudfoot AT, Vale JA (2004) Hydrogen peroxide poisoning. Toxicol Rev 23(1):51–57
Ramp WK, Arnold RR, Russell JE, Yancey JM (1987) Hydrogen peroxide inhibits glucose metabolism and collagen synthesis in bone. J Periodontol 58(5):340–344
Kaysinger KK, Nicholson NC, Ramp WK, Kellam JF (1995) Toxic effects of wound irrigation solutions on cultured tibiae and osteoblasts. J Orthop Trauma 9(4):303–311
Nicholson NC, Ramp WK, Kneisl JS, Kaysinger KK (1998) Hydrogen peroxide inhibits giant cell tumor and osteoblast metabolism in vitro. Clin Orthop Relat Res 347:250–260
Shida K, Yasumoto K, Yokoyama T, Maeda T, Ohtsuka N, Hosoyamada A (2002) Oxygen embolism after intraoperative use of hydrogen peroxide. Masui 51(12):1368–1370
Timperley AJ, Bracey DJ (1989) Cardiac arrest following the use of hydrogen peroxide during arthroplasty. J Arthroplast 4(4):369–370
Eipe NP, Ponniah M (2006) Perioperative blood loss assessment—how accurate? Indian J Anaesth 50(1):35–38
Acknowledgments
The authors thank Yanni Xu for her technical support.
Conflict of interest
The authors did not receive any outside funding or Grants in support of their research for or preparation of this work. Neither they nor a member of their immediate families received payments or other benefits or a commitment or agreement to provide such benefits from a commercial entity.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chen, J.Y., Rikhraj, I.S., Zhou, Z. et al. Can tranexamic acid and hydrogen peroxide reduce blood loss in cemented total knee arthroplasty?. Arch Orthop Trauma Surg 134, 997–1002 (2014). https://doi.org/10.1007/s00402-014-1958-z
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-014-1958-z