Abstract
Purpose
Alcoholic liver disease (ALD) is a major health issue globally. In addition to pharmacotherapy, dietary support is also regarded as reliable strategy for ALD management. As a widely distributed natural constituent within edible plants, the present study aims to investigate the hepatoprotective effects of ursolic acid (UA) against ALD and also to deepen insights into the underlying targets and mechanisms comprehensively.
Methods
The hepatoprotective activity of UA against chronic alcohol-induced liver injury was investigated on Lieber–DeCarli liquid diet-based mouse model. In-depth RNA-seq transcriptomics and TMT-based proteomics analyses were conducted in parallel. Data integration as well as bioinformatics analysis were also performed to unravel the targets and mechanisms associated with the hepatoprotective activity of UA intake against alcoholic liver injury comprehensively.
Results
The serum biomarkers and pathological characteristics indicated the hepatoprotective effects of UA intake on alcoholic liver injury. 567 target genes and 377 target proteins related to the hepatoprotective activity of UA were identified in transcriptomics and proteomics analysis respectively, most of which were associated with function of cellular process, cell part and binding. After data integration, 56 co-regulated targets, including ADH4, CYP450 enzymes, NQO1, apolipoproteins, glutathione–S–transferase, etc. which were consistently modulated on both mRNA and protein levels were identified. These co-regulated targets were found to be correlated with 70 KEGG pathways led by carcinogenesis, retinol metabolism and CYP450 metabolism pathways.
Conclusion
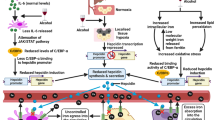
UA intake ameliorated chronic alcohol-induced liver injury. Given the role of the co-regulated targets in ALD and the bioinformatics analysis results, CYP450-, glutathione and redox homeostasis-dependent antioxidation, promotion of lipid transport, and restoration of ethanol metabolic capacity are the potentially underlying mechanisms. This information will further deepen our insights into the hepatoprotective effects of UA-rich edible plants, and provide us valuable instruction for ALD management.






Similar content being viewed by others
Abbreviations
- ALD:
-
Alcoholic liver disease
- UA:
-
Ursolic acid
- AST:
-
Aspartate aminotransferase
- ALT:
-
Alanine aminotransferase
- TG:
-
Triacylglycerol
- TC:
-
Total cholesterol
- TMT:
-
Transcriptomics and tandem mass tags
- RSEM:
-
RNA-seq by expectation maximization
- DEGs:
-
Differential expression genes
- FPKM:
-
Fragments per kilobase of exon per million mapped reads
- Edge R:
-
Empirical analysis of digital gene expression in R
- UPLC:
-
Ultra performance liquid chromatographer
- DEPs:
-
Differentially expressed proteins
- GO:
-
Gene ontology
- KEGG:
-
Kyoto encyclopedia of genes and genomes
- PPI:
-
Protein–protein interaction
- NQO1:
-
NAD(P)H dehydrogenase quinone 1
- GSTA2:
-
Glutathione S-transferase alpha 2
- BP:
-
Biological process
- CC:
-
Cellular component
- MF:
-
Molecular function
- OS:
-
Organismal systems
- CP:
-
Cellular processes
- M:
-
Metabolism
- HD:
-
Human diseases
- EIP:
-
Environmental information processing
- CYP450:
-
Cytochrome P450
- GST:
-
Glutathione S-transferase
- ROS:
-
Reactive oxygen species
- ADH:
-
Alcohol dehydrogenase
- RNS:
-
Reactive nitrogen species
References
Waszkiewicz N, Galinska-Skok B, Nestsiarovich A et al (2018) Neurobiological effects of binge drinking help in its detection and differential diagnosis from alcohol dependence. Dis Markers 2018:5623683. https://doi.org/10.1155/2018/5623683
Enoch MA, Albaugh BJ (2017) Review: genetic and environmental risk factors for alcohol use disorders in American Indians and Alaskan Natives. Am J Addict 26(5):461–468. https://doi.org/10.1111/ajad.12420
De Visser RO, Wheeler Z, Abraham C et al (2013) ‘Drinking is our modern way of bonding’: young people’s beliefs about interventions to encourage moderate drinking. Psychol Health 28(12):1460–1480. https://doi.org/10.1080/08870446.2013.828293
Axley PD, Richardson CT, Singal AK (2019) Epidemiology of alcohol consumption and societal burden of alcoholism and alcoholic liver disease. Clin Liver Dis 23(1):39–50. https://doi.org/10.1016/j.cld.2018.09.011
Crawford JM (2012) Histologic findings in alcoholic liver disease. Clin Liver Dis 16(4):699–716. https://doi.org/10.1016/j.cld.2012.08.004
Xia Y, Zhang S, Zhang Q et al (2020) Insoluble dietary fibre intake is associated with lower prevalence of newly-diagnosed non-alcoholic fatty liver disease in Chinese men: a large population-based cross-sectional study. Nutr Metab 17:4. https://doi.org/10.1186/s12986-019-0420-1
Han Y, Glueck B, Shapiro D et al (2020) Dietary synbiotic supplementation protects barrier integrity of hepatocytes and liver sinusoidal endothelium in a mouse model of chronic-binge ethanol exposure. Nutrients 12(2):373. https://doi.org/10.3390/nu12020373
Caligiani A, Malavasi G, Palla G et al (2013) A simple GC-MS method for the screening of betulinic, corosolic, maslinic, oleanolic and ursolic acid contents in commercial botanicals used as food supplement ingredients. Food Chem 136(2):735–741. https://doi.org/10.1016/j.foodchem.2012.08.011
Lopez-Hortas L, Perez-Larran P, Gonzalez-Munoz MJ et al (2018) Recent developments on the extraction and application of ursolic acid. A review. Food Res Int 103:130–149. https://doi.org/10.1016/j.foodres.2017.10.028
Wozniak L, Skapska S, Marszalek K (2015) Ursolic acid-A pentacyclic triterpenoid with a wide spectrum of pharmacological activities. Molecules 20(11):20614–20641. https://doi.org/10.3390/molecules201119721
Lin YN, Wang CCN, Chang HY et al (2018) Ursolic acid, a novel liver X receptor α (LXRα) antagonist inhibiting ligand-induced nonalcoholic fatty liver and drug-induced lipogenesis. J Agric Food Chem 66(44):11647–11662. https://doi.org/10.1021/acs.jafc.8b04116
Ma JQ, Ding J, Zhang L et al (2014) Ursolic acid protects mouse liver against CCl4-induced oxidative stress and inflammation by the MAPK/NF-κB pathway. Environ Toxicol Pharmacol 37(3):975–983. https://doi.org/10.1016/j.etap.2014.03.011
Li D, Ren D, Luo Y et al (2016) Protective effects of ursolic acid against hepatotoxicity and endothelial dysfunction in mice with chronic high choline diet consumption. Chem Biol Interact 258:102–107. https://doi.org/10.1016/j.cbi.2016.08.019
Saraswat B, Visen PKS, Agarwal DP (2000) Ursolic acid isolated from Eucalyptus tereticornis protects against ethanol toxicity in isolated rat hepatocytes. Phytother Res 14(3):163–166. https://doi.org/10.1002/(sici)1099-1573(200005)14:3%3c163:aid-ptr588%3e3.0.co;2-d
Saravanan R, Viswanathan P, Pugalendi KV (2006) Protective effect of ursolic acid on ethanol-mediated experimental liver damage in rats. Life Sci 78(7):713–718. https://doi.org/10.1016/j.lfs.2005.05.060
Ainiwaer T, Refuhati, et al (2019) Multiomics analysis profile acute liver injury module clusters to compare the therapeutic efficacy of bifendate and muaddil sapra. Sci Rep 9(1):4335. https://doi.org/10.1038/s41598-019-40356-5
Barnett MPG, Cooney JM, Dommels YEM et al (2013) Modulation of colonic inflammation in Mdr1a (-/-) mice by green tea polyphenols and their effects on the colon transcriptome and proteome. J Nutr Biochem 24(10):1678–1690. https://doi.org/10.1016/j.jnutbio.2013.02.007
Wang X, Liu Q, Zhang B (2014) Leveraging the complementary nature of RNA-Seq and shotgun proteomics data. Proteomics 14(23–24):2676–2687. https://doi.org/10.1002/pmic.201400184
Lieber CS, DeCarli LM, Sorrell MF (1989) Experimental methods of ethanol administration. Hepatology 10(4):501–510. https://doi.org/10.1002/hep.1840100417
Lamas-Paz A, Hao F, Nelson LJ et al (2018) (2018) Alcoholic liver disease: utility of animal models. World J Gastroenterol 24(45):5063–5075. https://doi.org/10.3748/wjg.v24.i45.5063
Xu X, Zhu Q, Zhang R et al (2017) ITRAQ-based proteomics analysis of acute lung injury induced by oleic acid in mice. Cell Physiol Biochem 44(5):1949–1964. https://doi.org/10.1159/000485885
Liu Y, Beyer A, Aebersold R (2016) On the dependency of cellular protein levels on mRNA abundance. Cell 165(3):535–550. https://doi.org/10.1016/j.cell.2016.03.014
Staats S, Wagner AE, Lüersen K et al (2019) Dietary ursolic acid improves health span and life span in male drosophila melanogaster. BioFactors 45(2):169–186. https://doi.org/10.1002/biof.1467
Kwon EY, Shin SK, Choi MS (2018) Ursolic acid attenuates hepatic steatosis, fibrosis, and insulin resistance by modulating the circadian rhythm pathway in diet-induced obese mice. Nutrients 10(11):1719. https://doi.org/10.3390/nu10111719
Gong P, Cederbaum AI, Nieto N (2003) Increased expression of cytochrome P450 2E1 induces heme oxygenase-1 through ERK MAPK pathway. J Biol Chem 278(32):29693–29700. https://doi.org/10.1074/jbc.M304728200
Gupta S, Pandey R, Katyal R et al (2005) Lipid peroxide levels and antioxidant status in alcoholic liver disease. Indian J Clin Biochem 20(1):67–71. https://doi.org/10.1007/BF02893045
Owuor ED, Kong AN (2002) Antioxidants and oxidants regulated signal transduction pathways. Biochem Pharmacol 64(5–6):765–770. https://doi.org/10.1016/s0006-2952(02)01137-1
Yeligar SM, Machida K, Kalra VK (2010) Ethanol-induced HO-1 and NQO1 are differentially regulated by HIF-1alpha and Nrf2 to attenuate inflammatory cytokine expression. J Biol Chem 285(46):35359–35373. https://doi.org/10.1074/jbc.M110.138636
Rushmore TH, Pickett CB (1993) Glutathione S-transferases, structure, regulation, and therapeutic implications. J Biol Chem 268(16):11475–11478. https://doi.org/10.1016/0005-2736(93)90149-T
Chen J, Schenker S, Henderson GI (2002) 4-Hydroxynonenal detoxification by mitochondrial glutathione S-transferase is compromised by short-term ethanol consumption in rats. Alcohol Clin Exp Res 26(8):1252–1258. https://doi.org/10.1111/j.1530-0277.2002.tb02664.x
Probyn ME, Zanini S, Ward LC et al (2012) A rodent model of low- to moderate-dose ethanol consumption during pregnancy: patterns of ethanol consumption and effects on fetal and offspring growth. Reprod Fertil Dev 24(6):859. https://doi.org/10.1071/RD11200
Nuutinen H, Lindros KO, Salaspuro M (1983) Determinants of blood acetaldehyde level during ethanol oxidation in chronic alcoholics. Alcohol Clin Exp Res 7(2):163–168. https://doi.org/10.1111/j.1530-0277.1983.tb05432.x
Srinivasan MP, Bhopale KK, Amer SM et al (2019) Linking dysregulated AMPK signaling and ER stress in ethanol-induced liver injury in hepatic alcohol dehydrogenase deficient deer mice. Biomolecules 9(10):560. https://doi.org/10.3390/biom9100560
Getz GS, Reardon CA (2009) Apoprotein E as a lipid transport and signaling protein in the blood, liver, and artery wall. J Lipid Res 50(Suppl):S156–S161. https://doi.org/10.1194/jlr.R800058-JLR200
Gong M, Castillo L, Redman RS et al (2008) Down-regulation of liver Galbeta 1, 4GlcNAc alpha2, 6-sialyltransferase gene by ethanol significantly correlates with alcoholic steatosis in humans. Metabolism 57(12):1663–1668. https://doi.org/10.1016/j.metabol.2008.07.021
Tahara M, Matsumoto K, Nukiwa T et al (1999) Hepatocyte growth factor leads to recovery from alcohol-induced fatty liver in rats. J Clin Invest 103(3):313–320. https://doi.org/10.1172/JCI4433
Tomita K, Azuma T, Kitamura N et al (2004) Pioglitazone prevents alcohol-induced fatty liver in rats through up-regulation of c-Met. Gastroenterology 126(3):873–885. https://doi.org/10.1053/j.gastro.2003.12.008
Teschke R (2018) Alcoholic liver disease: alcohol metabolism, cascade of molecular mechanisms, cellular targets, and clinical aspects. Biomedicines 6(4):106. https://doi.org/10.3390/biomedicines6040106
Lu Y, Zhuge J, Wu D et al (2011) Ethanol induction of CYP2A5: permissive role for CYP2E1. Drug Metab Dispos 39(2):330. https://doi.org/10.1124/dmd.110.035691
Lu Y, Cederbaum AI (2015) Cytochrome P450s and alcoholic liver disease. Curr Pharm Des 24(14):1502–1517. https://doi.org/10.2174/1381612824666180410091511
de Waziers I, Bouguet J, Beaune PH et al (1992) Effects of ethanol, dexamethasone and RU 486 on expression of cytochromes P450 2B, 2E, 3A and glutathione transferase pi in a rat hepatoma cell line (Fao). Pharmacogenetics 2(1):12–18. https://doi.org/10.1097/00008571-199202000-00003
Derikvandy A, Pourkhabbaz HR, Banaee M et al (2020) Genotoxicity and oxidative damage in zebrafish (Danio rerio) after exposure to effluent from ethyl alcohol industry. Chemosphere 251:126609. https://doi.org/10.1016/j.chemosphere.2020.126609
Acknowledgements
The authors gratefully acknowledge the financial support of National Natural Science Foundation of China (No. 81760769), the Ningxia Hui Autonomous Region key research and development program (2020BFG03007), and the Fundamental Research Funds for the Central Universities (2018-JYBZZ-JS017).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yan, X., Liu, X., Wang, Y. et al. Multi-omics integration reveals the hepatoprotective mechanisms of ursolic acid intake against chronic alcohol consumption. Eur J Nutr 61, 115–126 (2022). https://doi.org/10.1007/s00394-021-02632-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-021-02632-x