Abstract
Purpose
Excessive meat intake has been researched as a major cause of cardiovascular disease (CVD) among healthy adults, but data on this topic in Asian patients with diabetes are sparse. The quantity and variety of available meats vary widely between Asian and Western countries. As part of a nationwide cohort study we investigated the relationship between meat intake and incidence of CVD in Japanese patients with type 2 diabetes aged 40–70 years with HbA1c ≥ 6.5%.
Methods
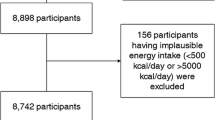
Analyzed were 1353 responders to a baseline dietary survey assessed by the Food Frequency Questionnaire based on food groups. Primary outcome was the 8-year risk of a CVD event, including coronary heart disease (CHD) and stroke. Cox regression analyses estimated hazard ratios (HRs) for dietary intake adjusted for age, gender, body mass index, HbA1c, smoking, energy intake, and other confounders.
Results
Mean meat intake in quartiles ranged from 9.9 to 97.7 g/day. After adjusting for confounders, HRs of CHD in the 2nd, 3rd, and 4th quartiles for meat intake compared with the 1st quartile were 2.84 (95% confidence interval 1.29–6.24, p = 0.01), 3.02 (1.36–6.70, p < 0.01), and 2.99 (1.35–6.65, p = 0.01), respectively. In two groups according to meat intake, patients consuming ≥ 20 g/day of meat had a 2.94-fold higher risk of CHD than those consuming < 20 g/day (p < 0.01). There was no significant association of stroke with meat intake.
Conclusions
An elevated incidence of CHD in Japanese patients with type 2 diabetes was associated with high meat intake.


Similar content being viewed by others
References
Aune D, Ursin G, Veierød MB (2009) Meat consumption and the risk of type 2 diabetes: a systematic review and meta-analysis of cohort studies. Diabetologia 52:2277–2287
Kontogianni MD, Panagiotakos DB, Pitsavos C et al (2008) Relationship between meat intake and the development of acute coronary syndromes: the CARDIO2000 case–control study. Eur J Clin Nutr 62:171–177
Kaluza J, Wolk A, Larsson SC (2012) Red meat consumption and risk of stroke: a meta-analysis of prospective studies. Stroke 43:2556–2560
Food and Agriculture Organization of the United Nations (2017) FAO Balance Sheet. http://faostat3.fao.org/download/FB/FBS/E Accessed 27 July 2017
Horikawa C, Yoshimura Y, Kamada C et al (2014) Dietary intake in Japanese patients with type 2 diabetes: analysis from Japan Diabetes Complications Study. J Diabetes Investig 5:176–187
Sone H, Ito H, Ohashi Y et al (2003) Obesity and type 2 diabetes in Japanese patients. Lancet 361:85
Inzucchi SE, Bergenstal RM, Buse JB et al (2012) Management of hyperglycemia in type 2 diabetes: a patient-centered approach: position statement of the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care 35:1364–1379
Karter AJ, Ferrara A, Liu JY et al (2002) Ethnic disparities in diabetic complications in an insured population. JAMA 287:2519–2527
Qi L, van Dam RM, Rexrode K et al (2007) Heme iron from diet as a risk factor for coronary heart disease in women with type 2 diabetes. Diabetes Care 30:101–106
Tanaka S, Tanaka S, Iimuro S et al (2014) Cohort Profile: the Japan Diabetes Complications Study: a long-term follow-up of a randomised lifestyle intervention study of type 2 diabetes. Int J Epidemiol 43:1054–1062
Sone H, Tanaka S, Iimuro S et al (2010) Long-term lifestyle intervention lowers the incidence of stroke in Japanese patients with type 2 diabetes: a nationwide multicentre randomised controlled trial (the Japan Diabetes Complications Study). Diabetologia 53:419–428
Ministry of Education C, Sports, Science, Technology J (2005) Standard tables of food composition in Japan 2005. http://www.mext.go.jp/b_menu/shingi/gijyutu/gijyutu3/toushin/05031802.htm Accessed 27 July 2017
Takahashi K, Yoshimura Y, Kaimoto T et al (2001) Validation of a Food Frequency Questionnaire based on food groups for estimating individual nutrient intake. Jpn J Nutr 59:221–232
Pan A, Sun Q, Bernstein AM et al (2011) Red meat consumption and risk of type 2 diabetes: 3 cohorts of US adults and an updated meta-analysis. Am J Clin Nutr 94:1088–1096
Micha R, Wallace SK, Mozaffarian D (2010) Red and processed meat consumption and risk of incident coronary heart disease, stroke, and diabetes mellitus: a systematic review and meta-analysis. Circulation 121:2271–2283
Peters SA, Huxley RR, Woodward M (2014) Diabetes as risk factor for incident coronary heart disease in women compared with men: a systematic review and meta-analysis of 64 cohorts including 858,507 individuals and 28,203 coronary events. Diabetologia 57:1542–1551
Subdivision on Resources, The Council for Science and Technology, Ministry of Education, Culture, Sports, Science, and Technology, Japan (2005) Standard Tables of Food Composition in Japan- Fifth Revised and Enlarged 2005. National Printing Bureau, Shiga
Brasitus TA, Davidson NO, Schachter D (1985) Variations in dietary triacylglycerol saturation alter the lipid composition and fluidity of rat intestinal plasma membranes. Biochim Biophys Acta 812:460–472
Ginsberg BH, Brown TJ, Simon I et al (1981) Effect of the membrane lipid environment on the properties of insulin receptors. Diabetes 30:773–780
Milanski M, Degasperi G, Coope A et al (2009) Saturated fatty acids produce an inflammatory response predominantly through the activation of TLR4 signaling in hypothalamus: implications for the pathogenesis of obesity. J Neurosci 29:359–370
Riccardi G, Giacco R, Rivellese AA (2004) Dietary fat, insulin sensitivity and the metabolic syndrome. Clin Nutr 23:447–456
Kanková K (2008) Diabetic threesome (hyperglycaemia, renal function and nutrition) and advanced glycation end products: evidence for the multiple-hit agent? Proc Nutr Soc 67:60–74
Uribarri J, Woodruff S, Goodman S et al (2010) Advanced glycation end products in foods and a practical guide to their reduction in the diet. J Am Diet Assoc 110:911–916
Zheng W, Lee SA (2009) Well-done meat intake, heterocyclic amine exposure, and cancer risk. Nutr Cancer 61:437–446
Uribarri J, Cai W, Ramdas M et al (2011) Restriction of advanced glycation end products improves insulin resistance in human type 2 diabetes: potential role of AGER1 and SIRT1. Diabetes Care 34:1610–1616
Vlassara H, Cai W, Goodman S et al (2009) Protection against loss of innate defenses in adulthood by low advanced glycation end products (AGE) intake: role of the antiinflammatory AGE receptor-1. J Clin Endocrinol Metab 94:4483–4491
Birlouez-Aragon I, Saavedra G, Tessier FJ et al (2010) A diet based on high-heat-treated foods promotes risk factors for diabetes mellitus and cardiovascular diseases. Am J Clin Nutr 91:1220–1226
Alexandersen P, Tankó LB, Bagger YZ et al (2006) The long-term impact of 2–3 years of hormone replacement therapy on cardiovascular mortality and atherosclerosis in healthy women. Climacteric 9:108–118
Miller VM, Duckles SP (2008) Vascular actions of estrogens: functional implications. Pharmacol Rev 60:210–241
Lobo RA (2017) Hormone-replacement therapy: current thinking. Nat Rev Endocrinol 13:220–231
Yusuf S, Hawken S, Ounpuu S et al (2004) Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case–control study. Lancet 364:937–952
Takii T, Yasuda S, Takahashi J et al (2010) Trends in acute myocardial infarction incidence and mortality over 30 years in Japan: report from the MIYAGI-AMI Registry Study. Circ J 74(1):93–100
Hanratty B, Lawlor DA, Robinson MB et al (2000) Sex differences in risk factors, treatment and mortality after acute myocardial infarction: an observational study. J Epidemiol Community Health 54:912–916
Poirier P, Giles TD, Bray GA et al (2006) Obesity and cardiovascular disease: pathophysiology, evaluation, and effect of weight loss: an update of the 1997 American Heart Association Scientific Statement on Obesity and Heart Disease from the Obesity Committee of the Council on Nutrition, Physical Activity, and Metabolism. Circulation 113:898–918
O’Donnell M, Mente A, Rangarajan S et al (2014) Urinary sodium and potassium excretion, mortality, and cardiovascular events. N Engl J Med 14 371:612–623
Horikawa C, Yoshimura Y, Kamada C et al (2014) Dietary sodium intake and incidence of diabetes complications in Japanese patients with type 2 diabetes: analysis of the Japan Diabetes Complications Study (JDCS). J Clin Endocrinol Metab 99:3635–3643
Kris-Etherton PM, Harris WS, Appel LJ,et al (2002) Fish consumption, fish oil, omega-3 fatty acids, and cardiovascular disease. Circulation 106:2747–2757
Wang X, Ouyang Y, Liu J et al (2014) Fruit and vegetable consumption and mortality from all causes, cardiovascular disease, and cancer: systematic review and dose–response meta-analysis of prospective cohort studies. BMJ 29:349:g4490
Johansson L, Solvoll K, Bjørneboe GE et al (1998) Under- and overreporting of energy intake related to weight status and lifestyle in a nationwide sample. Am J Clin Nutr 68:266–274
Martin GS, Tapsell LC, Batterham MJ et al (2002) Relative bias in diet history measurements: a quality control technique for dietary intervention trials. Public Health Nutr 5:537–545
Acknowledgements
We sincerely thank the late Professor Nobuhiro Yamada, who was a former director of the JDCS and always provided warm spiritual support to us all. We also thank Ms. Mami Haga and Ms. Natsuko Tada, Niigata University for their excellent secretarial assistance.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Disclosure statement
H.S. was support by a Grant-in-Aid for Scientific Research (#16H03260) from the Japan Society for the Promotion of Science (JSPS). This work is also financial support by the Ministry of Health, Labor and Welfare, Japan. The sponsors had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; or preparation, review, or approval of the manuscript.
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Horikawa, C., Kamada, C., Tanaka, S. et al. Meat intake and incidence of cardiovascular disease in Japanese patients with type 2 diabetes: analysis of the Japan Diabetes Complications Study (JDCS). Eur J Nutr 58, 281–290 (2019). https://doi.org/10.1007/s00394-017-1592-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-017-1592-y