Abstract
Aims
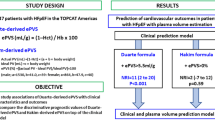
Estimated plasma volume status (ePVS) predicts prognosis in patients with heart failure (HF). It remains unclear whether admission, discharge or change ePVS best predicts post-discharge outcome in patients with acute decompensated heart failure (ADHF).
Methods
We retrospectively analyzed three cohort studies: 383 patients admitted at the Tokyo Medical University hospital, 165 patients admitted at the Centro Hospitalar do Porto and 164 patients admitted at the Nancy University Hospital (ICALOR study). ePVS at admission and at discharge as well as its change thereof were, respectively, calculated using the Duarte and Strauss formulas, both derived from hemoglobin and hematocrit ratios. Clinical variables including physical assessment, biological and echocardiographic parameters were recorded. The clinical outcome was a composite of re-hospitalization for worsening HF or all-cause mortality.
Results
The primary outcomes occurred in 27.2% at 1 year (in the Tokyo cohort), 45.3% at 6 months (in the Porto cohort) and 53.9% at median terms of 298.3 days (in the ICALOR study). After adjusting for potential confounders including natriuretic peptide, discharge ePVS remained significantly associated with increased rates of composite outcome in the Tokyo and Porto cohorts and ICALOR study [hazard ratio (HR) 1.21 (1.01–1.44), p = 0.04; HR 1.45 (1.16–1.81), p < 0.01; HR 1.45 (1.16–1.81), p < 0.01, respectively]. In addition, a pooled analysis yielded a significant improvement in reclassification with discharge ePVS [net reclassification index 13.6% (5.9–22.7), p = 0.004].
Conclusions
As validated in three independent ADHF cohorts, ePVS at discharge was independently associated with post-discharge clinical outcomes and improved the risk stratification of patients admitted for ADHF on top of well-established prognostic markers.



Similar content being viewed by others
References
Gheorghiade M, Follath F, Ponikowski P et al (2010) Assessing and grading congestion in acute heart failure: a scientific statement from the acute heart failure committee of the heart failure association of the European Society of Cardiology and endorsed by the European Society of Intensive Care Medicine. Eur J Heart Fail 12:423–433
Ambrosy AP, Pang PS, Khan S et al (2013) Clinical course and predictive value of congestion during hospitalization in patients admitted for worsening signs and symptoms of heart failure with reduced ejection fraction: findings from the EVEREST trial. Eur Heart J 34:835–843
Shiraishi Y, Nagai T, Kohsaka S et al (2018) Outcome of hospitalised heart failure in Japan and the United Kingdom stratified by plasma N-terminal pro-B-type natriuretic peptide. Clin Res Cardiol. https://doi.org/10.1007/s00392-018-1283-6
Coiro S, Rossignol P, Ambrosio G et al (2015) Prognostic value of residual pulmonary congestion at discharge assessed by lung ultrasound imaging in heart failure. Eur J Heart Fail 17:1172–1181
Palazzuoli A, Ruocco G, Beltrami M, Nuti R, Cleland JG (2018) Combined use of lung ultrasound, B-type natriuretic peptide, and echocardiography for outcome prediction in patients with acute HFrEF and HFpEF. Clin Res Cardiol 107:586–596
Yancy CW, Jessup M, Bozkurt B et al (2017) 2017 ACC/AHA/HFSA focused update of the 2013 ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Failure Society of America. J Card Fail 23:628–651
Ponikowski P, Voors AA, Anker SD et al (2016) 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur J Heart Fail 18:891–975
Girerd N, Seronde MF, Coiro S et al. Integrative assessment of congestion in heart failure throughout the patient journey. J Am Coll Cardiol 2017
Rossignol P, Menard J, Fay R, Gustafsson F, Pitt B, Zannad F (2011) Eplerenone survival benefits in heart failure patients post-myocardial infarction are independent from its diuretic and potassium-sparing effects. Insights from an EPHESUS (Eplerenone Post-Acute Myocardial Infarction Heart Failure Efficacy and Survival Study) substudy. J Am Coll Cardiol 58:1958–1966
Duarte K, Monnez JM, Albuisson E, Pitt B, Zannad F, Rossignol P (2015) Prognostic value of estimated plasma volume in heart failure. JACC Heart Fail 3:886–893
Valle R, Aspromonte N, Milani L et al (2011) Optimizing fluid management in patients with acute decompensated heart failure (ADHF): the emerging role of combined measurement of body hydration status and brain natriuretic peptide (BNP) levels. Heart Fail Rev 16:519–529
Standard Techinique for the measurement of red-cell and plasma volume (1973) A report by the International Committe for Standardization in Hematology (ICSH): panel on diagnostic applications of radioisotopes in haematology. Br J Haematol 25:801–814
Kalra PR, Anagnostopoulos C, Bolger AP, Coats AJS, Anker SD (2002) The regulation and measurement of plasma volume in heart failure. J Am Coll Cardiol 39:1901–1908
Yoshihisa A, Abe S, Sato Y et al. Plasma volume status predicts prognosis in patients with acute heart failure syndromes. Eur Heart J Acute Cardiovasc Care 2017:2048872617690889
Ling HZ, Flint J, Damgaard M et al (2015) Calculated plasma volume status and prognosis in chronic heart failure. Eur J Heart Fail 17:35–43
Ferreira JP, Girerd N, Arrigo M et al (2016) Enlarging red blood cell distribution width during hospitalization identifies a very high-risk subset of acutely decompensated heart failure patients and adds valuable prognostic information on top of hemoconcentration. Medicine (Baltimore) 95:e3307
Agrinier N, Altieri C, Alla F et al (2013) Effectiveness of a multidimensional home nurse led heart failure disease management program–a French nationwide time-series comparison. Int J Cardiol 168:3652–3658
Levey AS, Bosch JP, Lewis JB, Greene T, Rogers N, Roth D (1999) A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation. Modification of Diet in Renal Disease Study Group. Ann Intern Med 130:461–470
Strauss MB, Davis RK, Rosenbaum JD, Rossmeisl EC (1951) Water diuresis produced during recumbency by the intravenous infusion of isotonic saline solution. J Clin Invest 30:862–868
Olson JM, Samad BA, Alam M (2008) Prognostic value of pulse-wave tissue Doppler parameters in patients with systolic heart failure. Am J Cardiol 102:722–725
Santas E, Garcia-Blas S, Minana G et al (2015) Prognostic implications of tissue Doppler imaging-derived e/ea ratio in acute heart failure patients. Echocardiography 32:213–220
Santarelli S, Russo V, Lalle I et al (2017) Prognostic value of decreased peripheral congestion detected by bioelectrical impedance vector analysis (BIVA) in patients hospitalized for acute heart failure: BIVA prognostic value in acute heart failure. Eur Heart J Acute Cardiovasc Care 6:339–347
Anker SD, Negassa A, Coats AJS et al (2003) Prognostic importance of weight loss in chronic heart failure and the effect of treatment with angiotensin-converting-enzyme inhibitors: an observational study. Lancet 361:1077–1083
Ferreira JP, Girerd N, Medeiros PB et al (2016) Spot urine sodium excretion as prognostic marker in acutely decompensated heart failure: the spironolactone effect. Clin Res Cardiol 105:489–507
De Vecchis R, Ariano C, Giandomenico G, Di Maio M, Baldi C (2016) Change of serum BNP between admission and discharge after acute decompensated heart failure is a better predictor of 6-month all-cause mortality than the single BNP value determined at admission. J Clin Med Res 8:737–742
Kociol RD, Horton JR, Fonarow GC et al (2011) Admission, discharge, or change in B-type natriuretic peptide and long-term outcomes: data from Organized Program to Initiate Lifesaving Treatment in Hospitalized Patients with Heart Failure (OPTIMIZE-HF) linked to Medicare claims. Circ Heart Fail 4:628–636
Testani JM, Chen J, McCauley BD, Kimmel SE, Shannon RP (2010) Potential effects of aggressive decongestion during the treatment of decompensated heart failure on renal function and survival. Circulation 122:265–272
van der Meer P, Postmus D, Ponikowski P et al (2013) The predictive value of short-term changes in hemoglobin concentration in patients presenting with acute decompensated heart failure. J Am Coll Cardiol 61:1973–1981
Greene SJ, Gheorghiade M, Vaduganathan M et al (2013) Haemoconcentration, renal function, and post-discharge outcomes among patients hospitalized for heart failure with reduced ejection fraction: insights from the EVEREST trial. Eur J Heart Fail 15:1401–1411
Testani JM, Brisco MA, Chen J, McCauley BD, Parikh CR, Tang WH (2013) Timing of hemoconcentration during treatment of acute decompensated heart failure and subsequent survival: importance of sustained decongestion. J Am Coll Cardiol 62:516–524
Khan H, Greene SJ, Fonarow GC et al (2015) Length of hospital stay and 30-day readmission following heart failure hospitalization: insights from the EVEREST trial. Eur J Heart Fail 17:1022–1031
Davison BA, Metra M, Senger S et al (2016) Patient journey after admission for acute heart failure: length of stay, 30-day readmission and 90-day mortality. Eur J Heart Fail 18:1041–1050
Ambrosy AP, Bhatt AS, Gallup D et al (2017) Trajectory of congestion metrics by ejection fraction in patients with acute heart failure (from the heart failure network). Am J Cardiol 120:98–105
Farmakis D, Simitsis P, Bistola V et al (2017) Acute heart failure with mid-range left ventricular ejection fraction: clinical profile, in-hospital management, and short-term outcome. Clin Res Cardiol 106:359–368
Ishihara S, Gayat E, Sato N et al (2016) Similar hemodynamic decongestion with vasodilators and inotropes: systematic review, meta-analysis, and meta-regression of 35 studies on acute heart failure. Clin Res Cardiol 105:971–980
Borlaug BA, Paulus WJ (2011) Heart failure with preserved ejection fraction: pathophysiology, diagnosis, and treatment. European heart journal 32:670–679
Costanzo MR, Ronco C, Abraham WT et al (2017) Extracorporeal ultrafiltration for fluid overload in heart failure: current status and prospects for further research. J Am Coll Cardiol 69:2428–2445
Fudim M, Miller WL (2018) Calculated estimates of plasma volume in patients with chronic heart failure-comparison with measured volumes. J Card Fail. https://doi.org/10.1016/j.cardfail.2018.07.462
Acknowledgements
We thank all the patients who participated in this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
PR, JF, FZ and NG are supported by a public grant overseen by the French National Research Agency (ANR) as part of the second “Investissements d’Avenir” program FIGHT-HF (reference: ANR-15-RHU-0004). F.Z. has received consulting fees from Actelion, Amgen, AstraZeneca, Bayer, Boehringer, Boston Science, CEVA, CVRx, Vifor-Fresenius, GE Healthcare, J&J, KBP BioSciences, Livanova, Novartis, NovoNordisk, Pfizer, Quantum Genomics, Relypsa, Resmed, Roche, Takeda and ZS pharma. P.R. has received fees from Honoraria, research grants and/or travel grants from AstraZeneca, Bayer, BG Medicine, BMS, CVRx, Daichii-Sankyo, Fresenius, Gambro, HAC-Pharma, Novartis, Relypsa, Roche, Sanofi, Servier, Stealth Peptides, CTMA and Vifor Fresenius Medical Care Renal Pharma. N.G. has received Board and consulting Fees (Honoraria) for Novartis and consulting fees (Honoraria) for Servier. M.F. received a grant from the American Heart Association and consulting fees from Coridea, Axon Therapies, Galvani and GE Healthcare. M.W. has received consulting fees from Medtronic and Philips, and Y.I. has received consulting fees from Medtronic. All other authors have no conflict of interest to declare.
Additional information
The original version of this article was revised: Modifications have been made to the Abstract. Full information regarding the corrections made can be found in the correction for this article.
Rights and permissions
About this article
Cite this article
Kobayashi, M., Rossignol, P., Ferreira, J.P. et al. Prognostic value of estimated plasma volume in acute heart failure in three cohort studies. Clin Res Cardiol 108, 549–561 (2019). https://doi.org/10.1007/s00392-018-1385-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-018-1385-1