Abstract
Background
Pediatric trauma patients sustaining blunt abdominal trauma (BAT) with intra-abdominal injury (IAI) are frequently admitted to the intensive care unit (ICU). This study was performed to identify predictors for ICU admission following BAT.
Methods
Prospective study of children (< 16 years) who presented to 14 Level-One Pediatric Trauma Centers following BAT over a 1-year period. Patients were categorized as ICU or non-ICU patients. Data collected included vitals, physical exam findings, laboratory results, imaging, and traumatic injuries. A multivariable hierarchical logistic regression model was used to identify predictors of ICU admission. Predictive ability of the model was assessed via tenfold cross-validated area under the receiver operating characteristic curves (cvAUC).
Results
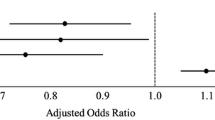
Included were 2,182 children with 21% (n = 463) admitted to the ICU. On univariate analysis, ICU patients were associated with abnormal age-adjusted shock index, increased injury severity scores (ISS), lower Glasgow coma scores (GCS), traumatic brain injury (TBI), and severe solid organ injury (SOI). With multivariable logistic regression, factors associated with ICU admission were severe trauma (ISS > 15), anemia (hematocrit < 30), severe TBI (GCS < 8), cervical spine injury, skull fracture, and severe solid organ injury. The cvAUC for the multivariable model was 0.91 (95% CI 0.88–0.92).
Conclusion
Severe solid organ injury and traumatic brain injury, in association with multisystem trauma, appear to drive ICU admission in pediatric patients with BAT. These results may inform the design of a trauma bay prediction rule to assist in optimizing ICU resource utilization after BAT.
Study design
Prognosis study.
Level of evidence
1.


Similar content being viewed by others
Abbreviations
- IAI:
-
Intra-abdominal injury
- MVC:
-
Motor vehicle collision
- BAT:
-
Blunt abdominal trauma
- SOI:
-
Solid organ injury
- ICU:
-
Intensive care unit
- CT:
-
Computed tomography
- SI:
-
Shock index
- GCS:
-
Glascow coma scale
- TBI:
-
Traumatic brain injury
- LOS:
-
Length of stay
- IQR:
-
Interquartile range
- ISS:
-
Injury severity score
- cvAUC:
-
Cross-validated area under the curve
- ROC:
-
Receiver operating characteristic curve
- AOR:
-
Adjusted odds ratio
- CI:
-
Confidence interval
References
Cooper A et al (1994) Mortality and truncal injury: the pediatric perspective. J Pediatr Surg 29(1):33–38
Holmes JF et al (2013) Identifying children at very low risk of clinically important blunt abdominal injuries. Ann Emerg Med 62(2):107–116 (e2)
Streck CJ et al (2017) Identifying children at very low risk for blunt intra-abdominal injury in whom CT of the abdomen can be avoided safely. J Am Coll Surg 224(4):449–458 (e3)
Wisner DH et al (2015) Management of children with solid organ injuries after blunt torso trauma. J Trauma Acute Care Surg 79(2):206–214 (quiz 332)
Leinwand MJ, Atkinson CC, Mooney DP (2004) Application of the APSA evidence-based guidelines for isolated liver or spleen injuries: a single institution experience. J Pediatr Surg 39(3):487–490 (discussion 487-90)
Fremgen HE et al (2014) Pediatric liver lacerations and intensive care: evaluation of ICU triage strategies. Pediatr Crit Care Med 15(4):e183–e191
Krieger AR et al (2012) Efficacy of anatomic and physiologic indicators versus mechanism of injury criteria for trauma activation in pediatric emergencies. J Trauma Acute Care Surg 73(6):1471–1477 (discussion 1477)
McVay MR et al (2008) Throwing out the “grade” book: management of isolated spleen and liver injury based on hemodynamic status. J Pediatr Surg 43(6):1072–1076
Mehall JR et al (2001) Prospective results of a standardized algorithm based on hemodynamic status for managing pediatric solid organ injury. J Am Coll Surg 193(4):347–353
Plumblee L et al (2020) Isolated low-grade solid organ injuries in children following blunt abdominal trauma: is it time to consider discharge from the emergency department? J Trauma Acute Care Surg 89(5):887–893
Narci A et al (2009) The prognostic importance of trauma scoring systems in pediatric patients. Pediatr Surg Int 25(1):25–30
Namasivayam A et al (2020) Predictors of modern contraceptive use among women and men in Uganda: a population-level analysis. BMJ Open 10(2):e034675
Luque-Fernandez MA, Redondo-Sánchez D, Maringe C (2019) cvauroc: Command to compute cross-validated area under the curve for ROC analysis after predictive modeling for binary outcomes. Stata J Promot Commun Stat Stata 19(3):615–625
Hosmer DW (2000) Applied logistic regression, 2nd edn. Wiley, New York
Hannan EL et al (2000) Predicting inpatient mortality for pediatric trauma patients with blunt injuries: a better alternative. J Pediatr Surg 35(2):155–159
Kong G et al (2015) Current state of trauma care in China, tools to predict death and ICU admission after arrival to hospital. Injury 46(9):1784–1789
Burd RS, Jang TS, Nair SS (2007) Evaluation of the relationship between mechanism of injury and outcome in pediatric trauma. J Trauma 62(4):1004–1014
Tepas JJ et al (1987) The pediatric trauma score as a predictor of injury severity in the injured child. J Pediatr Surg 22(1):14–18
Funding
No funding was used to conduct this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no potential conflicts of interest to disclose.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standard of the institutional research committees and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mehl, S.C., Cunningham, M.E., Streck, C.J. et al. Characteristics and predictors of intensive care unit admission in pediatric blunt abdominal trauma. Pediatr Surg Int 38, 589–597 (2022). https://doi.org/10.1007/s00383-022-05067-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-022-05067-5