Abstract
Purpose
The fibrogenic process in cholangiopathic diseases such as biliary atresia (BA) involves bile duct injury and apoptosis of cholangiocytes, which leads to the progression of liver fibrosis into liver cirrhosis and can result in end-staged liver disease. Recent advances in the development of organoids or mini-organ structures have allowed us to create an ex vivo injury model of the bile duct that mimics bile duct injury in BA. The aim of this experimental study was to develop a novel model of injured intrahepatic cholangiocytes as this can be relevant to BA. Our new model is important for studying the pathophysiological response of bile ducts to injury and the role of cholangiocytes in initiating the fibrogenic cascade. In addition, it has the potential to be used as a tool for developing new treatment strategies for BA.
Methods
Liver ductal organoids were generated from the liver of healthy neonatal mouse pups. Intrahepatic bile duct fragments were isolated and cultured in Matrigel dome. Injury was induced in the organoids by administration of acetaminophen in culture medium. The organoids were then evaluated for fibrogenic cytokines expression, cell apoptosis marker and cell proliferation marker.
Results
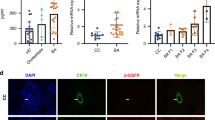
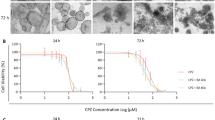
Organoids generated from intrahepatic bile duct fragments organized themselves into single-layer epithelial spheroids with lumen on the inside mimicking in vivo bile ducts. After 24-h exposure to acetaminophen, cholangiocytes in the organoids responded to the injury by increasing expression of fibrogenic cytokines, transforming growth factor beta-1 (TGF-β1) and platelet-derived growth factor-BB (PDGF-BB). This fibrogenic response of injured organoids was associated with increased cholangiocyte apoptosis and decreased cholangiocyte proliferation.
Conclusion
To our knowledge this is the first description of cholangiocyte injury in the organoids derived from intrahepatic bile ducts. Our injury model demonstrated that cholangiocyte apoptosis and its fibrogenic response may play a role in initiation of the fibrogenic process in cholangiopathic diseases such as BA. These findings are important for the development of novel therapy to reduce cholangiocyte apoptosis and to halt the early fibrogenic cascade in liver fibrogenesis. This novel injury model can prove very valuable for future research in biliary atresia.




Similar content being viewed by others
References
Friedman SL (2008) Mechanisms of hepatic fibrogenesis. Gastroenterology 134:1655–1669. https://doi.org/10.1053/j.gastro.2008.03.003
Ellis EL, Mann DA (2012) Clinical evidence for the regression of liver fibrosis. J Hepatol 56(5):1171–1180. https://doi.org/10.1016/j.jhep.2011.09.024
Nakanuma Y, Sasaki M, Harada K (2015) Autophagy and senescence in fibrosing cholangiopathies. J Hepatol 62:934–945. https://doi.org/10.1016/j.jhep.2014.11.027
Salas-Silva S, Simoni-Nieves A, Lopez-Ramirez J et al (2019) Cholangiocyte death in ductopenic cholestatic cholangiopathies: mechanistic basis and emerging therapeutic strategies. Life Sci 218:324–339. https://doi.org/10.1016/j.lfs.2018.12.044
Banales JM, Huebert RC, Karlsen T et al (2019) Cholangiocyte pathobiology. Nat Rev Gastroenterol Hepatol 16:269–281. https://doi.org/10.1038/s41575-019-0125-y
Shen W-J, Chen G, Wang M, Zheng S (2019) Liver fibrosis in biliary atresia. World J Pediatr 15:117–123. https://doi.org/10.1007/s12519-018-0203-1
Asai A, Miethke A, Bezerra JA (2015) Pathogenesis of biliary atresia: defining biology to understand clinical phenotypes. Nat Rev Gastroenterol Hepatol 12:342–352. https://doi.org/10.1038/nrgastro.2015.74
Harada K (2017) Sclerosing and obstructive cholangiopathy in biliary atresia: mechanisms and association with biliary innate immunity. Pediatr Surg Int 33:1243–1248. https://doi.org/10.1007/s00383-017-4154-8
Mack CL, Feldman AG, Sokol RJ (2012) Clues to the etiology of bile duct injury in biliary atresia. Semin Liver Dis 32:307–316. https://doi.org/10.1055/s-0032-1329899
Funaki N, Sasano H, Shizawa S et al (1998) Apoptosis and cell proliferation in biliary atresia. J Pathol 186:429–433. https://doi.org/10.1002/(SICI)1096-9896(199812)186:4%3c429::AID-PATH195%3e3.0.CO;2-6
Sasaki H, Nio M, Iwami D et al (2001) E-cadherin, alpha-catenin and beta-catenin in biliary atresia: correlation with apoptosis and cell cycle. Pathol Int 51:923–932. https://doi.org/10.1046/j.1440-1827.2001.01304.x
Erickson N, Mohanty SK, Shivakumar P et al (2008) Temporal-spatial activation of apoptosis and epithelial injury in murine experimental biliary atresia. Hepatol Baltim Md 47:1567–1577. https://doi.org/10.1002/hep.22229
Petersen C, Madadi-Sanjani O (2018) Role of viruses in biliary atresia: news from mice and men. Innov Surg Sci 3:101–106. https://doi.org/10.1515/iss-2018-0009
Milani S, Herbst H, Schuppan D et al (1991) Transforming growth factors beta 1 and beta 2 are differentially expressed in fibrotic liver disease. Am J Pathol 139:1221–1229
Kinnman N, Francoz C, Barbu V et al (2003) The myofibroblastic conversion of peribiliary fibrogenic cells distinct from hepatic stellate cells is stimulated by platelet-derived growth factor during liver fibrogenesis. Lab Investig J Tech Methods Pathol 83:163–173. https://doi.org/10.1097/01.lab.0000054178.01162.e4
Mekala S, Tulimilli SV, Geesala R et al (2018) Cellular crosstalk mediated by platelet-derived growth factor BB and transforming growth factor β during hepatic injury activates hepatic stellate cells. Can J Physiol Pharmacol 96:728–741. https://doi.org/10.1139/cjpp-2017-0768
Tsuchida T, Friedman SL (2017) Mechanisms of hepatic stellate cell activation. Nat Rev Gastroenterol Hepatol 14:397–411. https://doi.org/10.1038/nrgastro.2017.38
Aimaiti Y, Jin X, Wang W et al (2018) TGF-β1 signaling regulates mouse hepatic stellate cell differentiation via the Jagged1/Notch pathway. Life Sci 192:221–230. https://doi.org/10.1016/j.lfs.2017.11.018
Huch M, Gehart H, van Boxtel R et al (2015) Long-term culture of genome-stable bipotent stem cells from adult human liver. Cell 160:299–312. https://doi.org/10.1016/j.cell.2014.11.050
Broutier L, Andersson-Rolf A, Hindley CJ et al (2016) Culture and establishment of self-renewing human and mouse adult liver and pancreas 3D organoids and their genetic manipulation. Nat Protoc 11:1724–1743. https://doi.org/10.1038/nprot.2016.097
Bai Q, Yan H, Sheng Y et al (2017) Long-term acetaminophen treatment induced liver fibrosis in mice and the involvement of Egr-1. Toxicology 382:47–58. https://doi.org/10.1016/j.tox.2017.03.008
Leite SB, Roosens T, El Taghdouini A et al (2016) Novel human hepatic organoid model enables testing of drug-induced liver fibrosis in vitro. Biomaterials 78:1–10. https://doi.org/10.1016/j.biomaterials.2015.11.026
Prior N, Inacio P, Huch M (2019) Liver organoids: from basic research to therapeutic applications. Gut 68:2228–2237. https://doi.org/10.1136/gutjnl-2019-319256
Jaeschke H, Duan L, Nguyen NT, Ramachandran A (2019) Mitochondrial damage and biogenesis in acetaminophen-induced liver injury. Liver Res 3:150–156. https://doi.org/10.1016/j.livres.2019.10.002
Ramachandran A, Jaeschke H (2019) Acetaminophen hepatotoxicity: A mitochondrial perspective. Adv Pharmacol 85:195–219. https://doi.org/10.1016/bs.apha.2019.01.007
Cho Y-E, Seo W, Kim D-K et al (2018) Exogenous exosomes from mice with acetaminophen-induced liver injury promote toxicity in the recipient hepatocytes and mice. Sci Rep 8:16070. https://doi.org/10.1038/s41598-018-34309-7
Mitchell DB, Acosta D, Bruckner JV (1985) Role of glutathione depletion in the cytotoxicity of acetaminophen in a primary culture system of rat hepatocytes. Toxicology 37:127–146. https://doi.org/10.1016/0300-483X(85)90119-2
Viña J, Romero FJ, Estrela JM, Viña JR (1980) Effect of acetaminophen (paracetamol) and its antagonists on glutathione (GSH) content in rat liver. Biochem Pharmacol 29:1968–1970. https://doi.org/10.1016/0006-2952(80)90113-6
Lorent K, Gong W, Koo KA et al (2015) Identification of a plant isoflavonoid that causes biliary atresia. Sci Transl Med 7:286ra67. https://doi.org/10.1126/scitranslmed.aaa1652
Waisbourd-Zinman O, Koh H, Tsai S et al (2016) The toxin biliatresone causes mouse extrahepatic cholangiocyte damage and fibrosis through decreased glutathione and SOX17. Hepatol Baltim Md 64:880–893. https://doi.org/10.1002/hep.28599
Yang Y, Wang J, Zhan Y et al (2020) The synthetic toxin biliatresone causes biliary atresia in mice. Lab Invest. https://doi.org/10.1038/s41374-020-0467-7
Zhao X, Lorent K, Wilkins BJ et al (2016) Glutathione antioxidant pathway activity and reserve determine toxicity and specificity of the biliary toxin biliatresone in zebrafish. Hepatol Baltim Md 64:894–907. https://doi.org/10.1002/hep.28603
Broide E, Klinowski E, Koukoulis G et al (2000) Superoxide dismutase activity in children with chronic liver diseases. J Hepatol 32:188–192. https://doi.org/10.1016/s0168-8278(00)80062-8
Tiao M-M, Lin T-K, Kuo F-Y et al (2007) Early stage of biliary atresia is associated with significant changes in 8-hydroxydeoxyguanosine and mitochondrial copy number. J Pediatr Gastroenterol Nutr 45:329–334. https://doi.org/10.1097/MPG.0b013e3180cc2c0f
Tiao M-M, Liou C-W, Huang L-T et al (2013) Associations of mitochondrial haplogroups B4 and E with biliary atresia and differential susceptibility to hydrophobic bile acid. PLOS Genet 9:e1003696. https://doi.org/10.1371/journal.pgen.1003696
Funding
This study was funded by the Naccarato Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
All animal experiments were approved by the Animal Care Committee at The Hospital for Sick Children (no. 42681), and all methods performed according to guidelines and regulations.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chusilp, S., Lee, C., Li, B. et al. A novel model of injured liver ductal organoids to investigate cholangiocyte apoptosis with relevance to biliary atresia. Pediatr Surg Int 36, 1471–1479 (2020). https://doi.org/10.1007/s00383-020-04765-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-020-04765-2