Abstract
Purpose
We have studied whether curcumin protects different pulmonary aspiration material-induced lung injury in rats.
Materials and methods
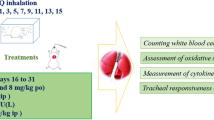
The experiments were designed in 60 Sprague–Dawley rats, randomly allotted into one of six groups (n = 10): normal saline (NS, control), enteral formula (Biosorb Energy Plus, BIO), hydrochloric acid (HCl), NS + curcumin-treated, BIO + curcumin-treated, and HCl + curcumin-treated. NS, BIO, HCl were injected in to the lungs. The rats received curcumin twice daily only for 7 days. Seven days later, both lungs in all groups were examined histopathologically, immunohistochemically, and biochemically. Histopathologic examination was performed according to the presence of peribronchial inflammatory cell infiltration, alveolar septal infiltration, alveolar edema, alveolar exudate, alveolar histiocytes, interstitial fibrosis, granuloma, and necrosis formation. Immunohistochemical assessments were examined for the activity of inducible nitric oxide synthase (iNOS) and the expression of surfactant protein D (SP-D). Malondialdehyde (MDA), hydroxyproline (HP), superoxide dismutase (SOD), and glutathione peroxidase (GSH-Px) activity were measured in the lung tissue.
Results
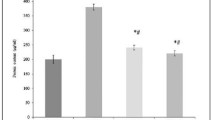
Our findings show that curcumin inhibits the inflammatory response reducing significantly (P < 0.05) all histopathological parameters in different pulmonary aspiration models. Pulmonary aspiration significantly increased the tissue HP content, MDA levels and decreased the antioxidant enzyme (SOD, GSH-Px) activities. Curcumin treatment significantly decreased the elevated tissue HP content, and MDA levels and prevented inhibition of SOD, and GSH-Px enzymes in the tissues. Furthermore, our data suggest that there is a significant reduction in the activity of iNOS and a rise in the expression of SP-D in lung tissue of different pulmonary aspiration models with curcumin therapy.
Conclusion
Our findings support the use of curcumin as a potential therapeutic agent in acute lung injury.



Similar content being viewed by others
References
Tasch MD, Stoelting RK (1996) Aspiration prevention, prophylaxis, and traetment. In: Benumoff JL (ed) Airway management. Mosby, St Louis, pp 183–201
Shepherd KE, Faulkner CS, Thal GD, Leiter JC (1995) Acute, subacute, and chronic histologic effects of simulated aspiration of a 0.7% sucralfate suspension in rats. Crit Care Med 23:532–536. doi:10.1097/00003246-199503000-00019
James CF, Modell JH, Gibbs CP, Kuck EJ, Ruiz BC (1984) Pulmonary aspiration: effects of volume and pH in the rat. Anesth Analg 63:665–668
Leth-Larsen R, Nordenback C, Tornoe I, Moeller V, Schlosser A, Koch C et al (2003) Surfactant protein D (SP-D) serum levels in patients with community-acquired pneumonia. Clin Immunol 108:29–37. doi:10.1016/S1521-6616(03)00042-1
Bhatia M, Moochhala S (2004) Role of inflammatory mediators in the pathophysiology of acute respiratory distress syndrome. J Pathol 202(2):145–156. doi:10.1002/path.1491
Tasaka S, Amaya F, Hashimoto S, Ishızaka A (2008) Roles of oxidants and redox signaling in the pathogenesis of acute respiratory distress syndrome. Antioxid Redox Signal 10(4):739–753. doi:10.1089/ars.2007.1940
Metnitz PG, Bartens C, Fischer M, Fridrich P, Steltzer H, Druml W (1999) Antioxidant status in patients with acute respiratory distress syndrome. Intensive Care Med 25(2):180–185. doi:10.1007/s001340050813
Cheng IW, Ware LB, Greene KE, Nuckton TJ, Eisner MD, Matthay MA (2003) Prognostic value of surfactant proteins A and D in patients with acute lung injury. Crit Care Med 31:20–27. doi:10.1097/00003246-200301000-00003
Herbein JF, Wright JR (2001) Enhanced clearance of surfactant protein D during LPS-induced acute inflammation in rat lung. Am J Physiol Lung Cell Mol Physiol 281:L268–L277
Guzel A, Başaran U, Aksu B, Kanter M, Yalcın O, Aktas C, Guzel A, Karasalıhoglu K (2008) Protective effects of S-methylisothiourea sulfate on different aspiration materials-induced lung injury in rats. Int J Pediatr Otorhinolaryngol 72(8):1241–1250. doi:10.1016/j.ijporl.2008.05.001
Strimpakos AS, Sharma RA (2008) Curcumin: preventive and therapeutic properties in laboratory studies and clinical trials. Antioxid Redox Signal 10(3):511–545. doi:10.1089/ars.2007.1769
Punithavathi D, Venkatesan N, Babu M (2000) Curcumin inhibition of bleomycin-induced pulmonary fibrosis in rats. Br J Pharmacol 131:169–172. doi:10.1038/sj.bjp.0703578
Kim KM, Pae HO, Zhung M, Ha HY, Ha YA, Chai KY et al (2008) Involvement of anti-inflammatory heme oxygenase-1 in the inhibitory effect of curcumin on the expression of pro-inflammatory inducible nitric oxide synthase in RAW264.7 macrophages. Biomed Pharmacother (Feb):20 (in press)
Mlsko TP, Moore WM, Kasten TP, Nlckols GA, Corbett JA, Tilton RG (1993) Selective inhibition of the inducible nitric oxide synthase by aminoguanidine. Eur J Pharmacol 233:119–125. doi:10.1016/0014-2999(93)90357-N
Jian MY, Koizumi T, Kubo K (2005) Effects of nitric oxide synthase inhibitor on acid aspiration-induced lung injury in rats. Pulm Pharmacol Ther 18:33–39. doi:10.1016/j.pupt.2004.07.007
Takil A, Umuroglu T, Gogus YF, Etı Z, Yildizeli B, Ahiskali R (2003) Histopathologic effects of lipid content of enteral solutions after pulmonary aspiration in rats. Nutrition 19:666–669. doi:10.1016/S0899-9007(03)00057-1
Hsu SM, Raine L, Fanger H (1981) Use of avidin-biotin-peroxidase complex (ABC) in immunperoxidase techniques: a comparison between ABC and unlabeled antibody (PAP) procedures. J Histochem Cytochem 29:577–580
Kivirikko KI, Laitinen O, Prockop DJ (1967) Modifications of a specific assay for hydroxyproline in urine. Anal Biochem 19:249–255. doi:10.1016/0003-2697(67)90160-1
Ohkawa H, Oshishi N, Yagi K (1979) Assay of lipid peroxidation in animal tissue by thiobarbituric acid reaction. Anal Biochem 95:351–358. doi:10.1016/0003-2697(79)90738-3
Lowry OH, Rosenbrough NJ, Farr AC, Randall RJ (1951) Protein measurement with the folin phenol regent. J Biol Chem 193:265–275
Sun Y, Oberley LW, Li Y (1988) A simple method for clinical assay of superoxide dismutase. Clin Chem 34:497–500
Paglia DE, Valentine WN (1967) Studies on the quantitative and qualitative characterisation of erythrocyte glutathione peroxidase. J Lab Clin Med 70:158–169
Pawlik MT, Schreyer AG, Ittner KP, Selig C, Gruber M, Feuerbach S et al (2005) Early treatment with pentoxifylline reduces lung injury induced by acid aspiration in rats. Chest 127:613–621. doi:10.1378/chest.127.2.613
Metheny NA, Clouse RE, Chang YH, Stewart BJ, Oliver DA, Kollef MH (2006) Tracheobronchial aspiration of gastric contents in critically ill tube-fed patients: frequency, outcomes, and risk factors. Crit Care Med 34:1007–1015. doi:10.1097/01.CCM.0000206106.65220.59
DeLegge MH (2002) Aspiration pneumonia: incidence, mortality and at-risk populations. JPEN J Parenter Enteral Nutr 26(6):S19–S24
Garzón Lorenzo P, Torrent Vernetta A, Server Salvà L, de Vicente CM, García-Cendón C, Gartner S (2008) Exogenous lipoid pneumonia. An Pediatr (Barc) 68(5):496–498. doi:10.1157/13120049
Ahrens P, Noll C, Kitz R, Willigens P, Zielen S, Hofmann D (1999) Lipid-laden alveolar macrophages: a useful marker of silent aspiration in children. Pediatr Pulmonol 28:8. doi:10.1002/(SICI)1099-0496(199909)28:19+<8::AID-PPUL1>3.0.CO;2-V
Hutson AD, Davidson BA, Raghavendran K, Chess PR, Tait AR, Holm BA et al (2006) Statistical prediction of the type of gastric aspiration lung injury based on early cytokine/chemokine profiles. Anesthesiology 104:73–79
Hyers TM (1993) Prediction of survival and mortality in patients with the adult respiratory distress syndrome. New Horiz 1:466–470
Jian MY, Koizumi T, Tsushima K, Kubo K (2004) JTE-607, a cytokine release blocker, attenuates acid aspiration-induced lung injury in rats. Eur J Pharmacol 488:231–238. doi:10.1016/j.ejphar.2004.02.026
Kudoh L, Miyazaki H, Ohara M, Fukushima J, Tazawa T, Yamada H (2001) Activation of alveolar macrophages in acid-injured lung in rats: different effect of pentoxifylline on tumor necrosis factor-alpha and nitric oxide production. Crit Care Med 29:1621–1625. doi:10.1097/00003246-200108000-00020
Mıtsushima H, Oishi K, Ngao T, Ichinose A, Senba M, Iwasaki T et al (2002) Acid aspiration induces bacterial pneumonia by enhanced bacterial adherence in mice. Microb Pathog 33:203–210. doi:10.1006/mpat.2002.0529
Goldman G, Welbourn R, Kobzik L, Valeri CR, Shepro D, Hechtman HB (1992) Reactive oxygen species and elastase mediate lung permeability after acid aspiration. J Appl Physiol 73(2):571–575
Aksu B, İnan M, Kanter M, Ozpuyan F, Uzun H, Durmuş G et al (2007) The effects of methylene blue on renal scarring due to pyelonepritis in rats. Pediatr Nephrol 22(7):992–1001. doi:10.1007/s00467-007-0464-8
Downey GP, Dong Q, Kruger J, Dedhar S, Cherapanov V (1999) Regulation of neutrophil activation in acute lung injury. Chest 116:46S–54S. doi:10.1378/chest.116.suppl_1.46S-a
Davidson BA, Knight PR, Helinski JD, Nader ND, Shanley TP, Johnson KJ (1999) The role of tumor necrosis factor-alpha in the pathogenesis of aspiration pneumonitis in rats. Anesthesiology 91:486–499. doi:10.1097/00000542-199908000-00024
Folkesson HG, Matthay MA, Hebert CA, Broaddus VC (1995) Acid aspiration-induced lung injury in rabbits is mediated by interleukin-8-dependent mechanisms. J Clin Invest 96:107–116. doi:10.1172/JCI118009
Moncada S (1992) The l-arginine:nitric oxide pathway. Acta Physiol Scand 145:201–227
Nathan C, Xie QW (1994) Nitric oxide synthases: roles, tolls and controls. Cell 78:915–918. doi:10.1016/0092-8674(94)90266-6
Gaston B, Drazen JM, Loscalzo J, Stamler JS (1994) The biology of nitrogen oxides in the airways. Am J Respir Crit Care Med 149:538–551
Speyer CL, Neff TA, Warner RL, Guo RF, Sarma JV, Riedemann NC et al (2003) Regulatory effects of iNOS on acute lung inflammatory responses in mice. Am J Pathol 163:2319–2328
Bogdan C (2001) Nitric oxide and immune response. Nat Immunol 2:907–916. doi:10.1038/ni1001-907
Lee KH, Rico P, Billiar TR, Pinsky MR (1998) Nitric oxide production after acute, unilateral hydrochloric acid-induced lung injury in a canine model. Crit Care Med 26:2042–2047. doi:10.1097/00003246-199812000-00038
Harkin DW, Rubin BB, Romaschin A, Lindsay TF (2004) Selective inducible nitric oxide synthase (iNOS) inhibition attenuates remote acute lung injury in a model of ruptured abdominal aortic aneurysm. J Surg Res 120:230–241. doi:10.1016/j.jss.2004.03.011
Miyakawa H, Sato K, Shinbori T, Okamoto T, Gushima Y, Fujiki M et al (2002) Effects of inducible nitric oxide synthase and xanthine oxidase inhibitors on SEB-induced interstitial pneumonia in mice. Eur Respir J 19:447–457. doi:10.1183/09031936.02.00265902
Bachofen M, Weibel ER (1982) Structural alterations of lung parenchyma in the adult respiratory distress syndrome. Clin Chest Med 3:35–56
Botas C, Poulain F, Akiyama J, Brown C, Allen L, Goerke J et al (1998) Altered surfactant homeostasis and alveolar type II cell morphology in mice lacking surfactant protein D. Proc Natl Acad Sci USA 95:11869–11874. doi:10.1073/pnas.95.20.11869
Crouch EC (1998) Collectins and pulmonary host defense. Am J Respir Cell Mol Biol 19:177–201
Ikegami M, Scoville EA, Grant S, Korfhagen T, Brondyk W, Scheule RK et al (2007) Surfactant protein-D and surfactant inhibit endotoxin-induced pulmonary inflammation. Chest 132(5):1447–1454. doi:10.1378/chest.07-0864
Pan T, Nielsen LD, Allen MJ, Shannon KM, Shannon JM, Selman M et al (2002) Serum SP-D is a marker of lung injury in rats. Am J Physiol Lung Cell Mol Physiol 282:L824–L832
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Guzel, A., Kanter, M., Aksu, B. et al. Preventive effects of curcumin on different aspiration material-induced lung injury in rats. Pediatr Surg Int 25, 83–92 (2009). https://doi.org/10.1007/s00383-008-2282-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-008-2282-x