Abstract
Introduction
External hydrocephalus (eHC) is commonly defined as a subtype of infant “hydrocephalus” consisting of macrocepahly associated with enlarged subarachnoid space and no or mild ventriculomegaly. This status is thought to be related to impaired CSF absorption because of arachnoid villi immaturity. However, other factors like the venous system might be involved in the development of the clinical picture.
Methods
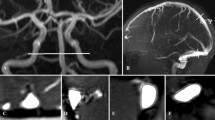
All patients diagnosed with eHC received prospectively contrast-enhanced 3D MR phlebography. Venous sis abnormalities were graded depending on the number of affected sinus segments and type. External CSF space volume was quantified planimetrically.
Results
Seventeen patients with the typical clinical feature of eHC were included. In 15, venous sinus abnormalities were found. There was a significant correlation between the volume of the widened cortical subarachnoid space (CSAS) and the number of venous sinus segments affected. Conversely, ventricular volume was not correlated.
Conclusion
These results support the hypothesis that impaired venous outflow plays a major role in external hydrocephalus development. Raised venous pressure increases intracranial pressure accelerating head growth, resulting in an enlargement of the cortical subarachnoid space. Increased venous pressure increases the capillary bed pressure and brain turgor preventing ventricular space to enlarge forcing displacement of ventricular CSF to the subarachnoid space. As a result, ventriculomegaly is rarely found. The descriptive term “external hydrocephalus” implying a primary etiology within the CSF system is misleading and this work supports the notion that venous hypertension is the leading cause of the clinical picture.





Similar content being viewed by others
References
Barlow CF (1984) CSF dynamics in hydrocephalus—with special attention to external hydrocephalus. Brain Dev 6:119–127
Bateman GA (2010) Hyperemic hydrocephalus: a new form of childhood hydrocephalus analogous to hyperemic intracranial hypertension in adults. J Neurosurg Pediatr 5(1):20–26
Bateman GA, Alber M, Schuhmann MU (2014) An association between external hydrocephalus in infants and reversible collapse of the venous sinuses. Neuropediatrics 45:183–187
Bateman GA, Brown KM (2011) The measurement of CSF flow through the aqueduct in normal and hydrocephalic children: from where does it come, to where does it go? Childs Nerv Syst 28:55–63
Bateman GA, Napier BD (2011) External hydrocephalus in infants: six cases with MR venogram and flow quantification correlation. Childs Nerv Syst 27:2087–2096
Brinker T, Stopa E, Morrison J, Klinge P (2014) A new look at cerebrospinal fluid circulation. Fluids Barriers CNS 11:10
De Bonis P, Pompucci A, Mangiola A, Rigante L, Anile C (2010) Post-traumatic hydrocephalus after decompressive craniectomy: an underestimated risk factor. J Neurotrauma 27:1965–1970
De Simone R, Ranieri A, Montella S, Bilo L, Cautiero F (2014) The role of dural sinus stenosis in idiopathic intracranial hypertension pathogenesis: the self-limiting venous collapse feedback-loop model. Panminerva Med 56(3):201–209
Dillon T, Berman W Jr, Yabek SM, Seigel R, Akl B, Wernly J (1986) Communicating hydrocephalus: a reversible complication of the mustard operation with serial hemodynamics and long-term follow-up. Ann Thorac Surg 41:146–149
Frydrychowski AF, Winklewski PJ, Guminski W (2012) Influence of acute jugular vein compression on the cerebral blood flow velocity, pial artery pulsation and width of subarachnoid space in humans. PLoS One 7(10):e48245
Hanlo PW, Gooskens RJ, van Schooneveld M, Tulleken CA, van der Knaap MS, Faber JA, Willemse J (1997) The effect of intracranial pressure on myelination and the relationship with neurodevelopment in infantile hydrocephalus. Dev Med Child Neurol 39:286–291
Hellbush LC (2007) Benign extracerebral fluid collections in infancy: clinical presentation and long-term follow-up. J Neurosurg 107(2 Suppl Pediatrics):119–125
Kapoor KG, Katz SE, Grzybowski DM, Lubow M (2008) Cerebrospinal fluid outflow: an evolving perspective. Brain Res Bull 77:327–334
Kumar R (2006) External hydrocephalus in small children. Childs Nerv Syst 22:1237–1241
Kendall B, Holland I (1981) Benign communicating hydrocephalus in children. Neuroradiology 21:93–96
Leliefeld PH, Gooskens RHJM, Vicken KL, Ramos LM, van der Grond J, Tulleken CAF et al (2008) Magnetic resonance imaging for quantitative flow measurement in infants with hydrocephalus: a prospective study. J Neurosurg Pediatrics 2:163–170
Libicher M, Tröger J (1992) US measurement of the subarachnoid space in infants: normal values. Radiology 184(3):749–751
Maki Y, Kokubo Y, Nose T, Yoshii Y (1976) Some characteristic findings of isotope cisternograms in children. J Neurosurg 45:56–59
Maytal J, Alvarez LA, Elkin CM, Shinnar S (1987) External hydrocephalus: radiologic spectrum and differentiation from cerebral atrophy. AJR Am J Roentgenol 148:1223–1230
Muenchberger H, Assaad N, Joy P, Brunsdon R, Shores EA (2006) Idiopathic macrocephaly in the infant: long-term neurological and neuropsychological outcome. Childs Nerv Syst 22(10):1242–1248
Norrell H, Wilson C, Howieson J et al (1969) Venous factors in infantile hydrocephalus. J Neurosurg 31:561–569
O’Hayon BB, Drake JM, Ossip MG, Tuli S, Clarke M (1998) Frontal and occipital horn ratio: a linear estimate of ventricular size for multiple imaging modalities in pediatric hydrocephalus. Pediatr Neurosurg 29(5):245–249
Oi S, Di Rocco C (2006) Proposal of “evolution theory in cerebrospinal fluid dynamics” and minor pathway hydrocephalus in developing immature brain. Childs Nerv Syst 22:662–669v
Rekate HL, Nadkarni TD, Wallace D (2008) The importance of the cortical subarachnoid space in understanding hydrocephalus. J Neurosurg Pediatr 2(1):1–11
Turner L (1961) The structure of arachnoid granulations with observations on their physiology and pathophysiological significance. Ann R Coll Surg Engl 29:237–264
Wiig US, Zahl SM, Egge A, Helseth E, Wester K (2017) Epidemiology of benign external hydrocephalus in Norway-a population-based study. Pediatr Neurol 73:36–41
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Sainz, L.V., Zipfel, J., Kerscher, S.R. et al. Cerebro-venous hypertension: a frequent cause of so-called “external hydrocephalus” in infants. Childs Nerv Syst 35, 251–256 (2019). https://doi.org/10.1007/s00381-018-4007-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-018-4007-3