Abstract
Background
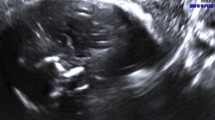
A relationship between Zika virus (ZikV) infection in pregnancy and the occurrence of microcephaly was established during the Zika outbreak in Brazil (2015–2016). Neuropathological findings in congenital Zika syndrome helped to understand its pathogenetic mechanisms.
Results
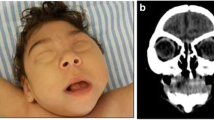
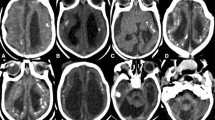
The most relevant postmortem findings in the central nervous system (CNS) of fetuses and neonates infected with ZikV early in gestation are microcephaly with ex-vacuo ventriculomegaly and large head circumference associated with obstructive hydrocephalus due to severe midbrain and aqueduct distortion. Babies with severe brain lesions are born with arthrogryposis. Histologically, there is extensive destruction of the hemispheric parenchyma, calcifications, various disturbances of neuronal migration, reactive gliosis, microglial hyperplasia and occasional perivascular cuffs of lymphocytes, also in the meninges. Hypoplastic lesions secondary to the lack of descending nerve fibers include small basis pontis, pyramids and spinal corticospinal tracts. Cerebellar hypoplasia is also common. Severe nerve motor nerve cell loss is observed in the anterior horn of the spinal cord.
Conclusion
A spectrum of neuropathological changes, from severe microcephaly to obstructive hydrocephalus was observed. The severity of the lesions is directly related to the gestational age, the most severe occurring when the mother is infected in the first trimester. Infection of progenitor cells at the germinal matrix was demonstrated. The lack of spinal motor neurons is responsible for fetal acynesia and consequent arthrogryposis.







Similar content being viewed by others
References
Oliveira Melo AS, Malinger G, Ximenes R, Szejnfeld PO, Alves Sampaio S, Bispo De Filippis AM (2016) Zika virus intrauterine infection causes fetal brain abnormality and microcephaly: tip of the iceberg? Ultrasound Obstet Gynecol 47:6–7. https://doi.org/10.1002/uog.15831
Soares de Oliveira-Szejnfeld P, Levine D, Melo ASO et al (2016) Congenital brain abnormalities and Zika virus: what the radiologist can expect to see? Radiology 281:203–218. https://doi.org/10.1148/radiol.2016161584
Lucia de Noronha L, Zanluca C, Azevedo MLV et al (2016) Zika virus damages the human placental barrier and presents marked fetal neurotropism. Mem Inst Oswaldo Cruz 111:287–293. https://doi.org/10.1590/0074-02760160085
Acosta-Reyes J, Navarro E, Herrera MJ et al (2017) Severe neurologic disorders in 2 fetuses with Zika virus infection, Colombia. Emerg Infect Dis 23:982–984. https://doi.org/10.3201/eid2306.161702
Sousa AQ, Cavalcante DIM, Franco LM et al (2017) Postmortem findings for 7 neonates with congenital Zika vírus infection. Emerg Infect Dis 23:1164–1167. https://doi.org/10.3201/eid2307.162019
Driggers RW, Ho C-Y, Korhonen EM et al (2016) Zika virus infection with prolonged maternal viremia and fetal brain abnormalities. N Engl J Med 374:2142–2151. https://doi.org/10.1056/NEJMoa1601824
Martines RB, Bhatnagar J, de Oliveira Ramos AM et al (2016) Pathology of congenital Zika syndrome in Brazil: a case series. Lancet 388:898–904. https://doi.org/10.1016/S0140-6736(16)30883-2
Mlakar J, Korva M, Tul N et al (2016) Zika virus associated with microcephaly. N Engl J Med 374:951–958. https://doi.org/10.1056/NEJMoa1600651
Chimelli L, Melo ASO, Avvad-Portari E et al (2017) The spectrum of neuropathological changes associated with congenital Zika virus infection. Acta Neuropathol 133:983–999. https://doi.org/10.1007/s00401-017-1699-5
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
I would also like to inform that neither Dr. Avvad Portari nor myself have any conflict of interest concerning the publication of this manuscript.
Rights and permissions
About this article
Cite this article
Chimelli, L., Avvad-Portari, E. Congenital Zika virus infection: a neuropathological review. Childs Nerv Syst 34, 95–99 (2018). https://doi.org/10.1007/s00381-017-3651-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-017-3651-3