Abstract
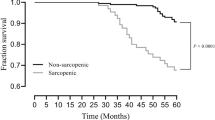
The number of patients on maintenance hemodialysis (HD) diagnosed with sarcopenia has been increasing through as individuals age. Recent focus is on the condition termed, “dynapenia,” which reduces only muscle function, as opposed to sarcopenia, which reduces both muscle mass and function. However, the association between dynapenia and cardio-cerebrovascular (CV) events in patients undergoing HD is largely unknown. The purpose of this study was to evaluate whether sarcopenia and dynapenia are associated with the onset of CV events in patients undergoing HD. We retrospectively analyzed 342 patients undergoing HD between January and December 2018. Patients who underwent HD thrice per week for > 3 months were included in the analysis. We adopted the Asian Working Group on Sarcopenia criteria for the diagnosis of sarcopenia and dynapenia. In this study, 244 patients undergoing HD were enrolled. The prevalence of sarcopenia was 38.5%. Sarcopenia was determined to be an independent contributor to CV events in patients undergoing HD. To investigate the clinical relevance of dynapenia in patients with HD, patients without sarcopenia were further divided into dynapenia and non-dynapenia groups. Among 150 patients without sarcopenia, 46 were diagnosed with dynapenia. In the Kaplan–Meier analysis, the rate of CV events was significantly different among the three groups in a stratified manner, with the highest rate in the sarcopenia group and the lowest rate in the non-sarco-dynapenia group. Both patients with sarcopenia and dynapenia had significantly increased CV events compared to those with non-sarco-dynapenia (HR 8.00; 95% CI 2.73–34.1; p < 0.0001 vs. HR 4.85; 95% CI 1.28–23.0; p < 0.02). Both sarcopenia and dynapenia resulted in significantly higher CV events than non-sarco-dynapenia in patients undergoing HD. Therefore, clinicians should evaluate muscle function in addition to muscle quantity to estimate CV events in patients undergoing HD.



Similar content being viewed by others
Abbreviations
- HD:
-
Hemodialysis
- AWGS:
-
The Asian Working Group on Sarcopenia
- CV:
-
Cardiovascular and cerebrovascular
- DEXA:
-
Dual-energy X-ray absorptiometry
- SMI:
-
Skeletal mass index
- MI:
-
Myocardial infarction
References
Cruz-Jentoft AJ, Sayer AA (2019) Sarcopenia. The Lancet 393(10191):2636–2646. https://doi.org/10.1016/s0140-6736(19)31138-9
Chen LK, Woo J, Assantachai P, Auyeung TW, Chou MY, Iijima K, Jang HC, Kang L, Kim M, Kim S, Kojima T, Kuzuya M, Lee JSW, Lee SY, Lee WJ, Lee Y, Liang CK, Lim JY, Lim WS, Peng LN, Sugimoto K, Tanaka T, Won CW, Yamada M, Zhang T, Akishita M, Arai H (2020) Asian Working Group for Sarcopenia: 2019 consensus update on sarcopenia diagnosis and treatment. J Am Med Dir Assoc 21(3):300–307. https://doi.org/10.1016/j.jamda.2019.12.012 (e302)
Kramer A (2020) An overview of the beneficial effects of exercise on health and performance. Adv Exp Med Biol 1228:3–22. https://doi.org/10.1007/978-981-15-1792-1_1
Visser M, Schaap LA (2011) Consequences of sarcopenia. Clin Geriatr Med 27(3):387–399. https://doi.org/10.1016/j.cger.2011.03.006
Yin J, Lu X, Qian Z, Xu W, Zhou X (2019) New insights into the pathogenesis and treatment of sarcopenia in chronic heart failure. Theranostics 9(14):4019–4029. https://doi.org/10.7150/thno.33000
Clark BC, Manini TM (2012) What is dynapenia? Nutrition 28(5):495–503. https://doi.org/10.1016/j.nut.2011.12.002
Manini TM, Clark BC (2012) Dynapenia and aging: an update. J Gerontol A Biol Sci Med Sci 67(1):28–40. https://doi.org/10.1093/gerona/glr010
Mori H, Kuroda A, Matsuhisa M (2019) Clinical impact of sarcopenia and dynapenia on diabetes. Diabetol Int 10(3):183–187. https://doi.org/10.1007/s13340-019-00400-1
Clark BC, Manini TM (2008) Sarcopenia =/= dynapenia. J Gerontol A Biol Sci Med Sci 63(8):829–834. https://doi.org/10.1093/gerona/63.8.829
Yamada M, Kimura Y, Ishiyama D, Nishio N, Abe Y, Kakehi T, Fujimoto J, Tanaka T, Ohji S, Otobe Y, Koyama S, Okajima Y, Arai H (2017) Differential characteristics of skeletal muscle in community-dwelling older adults. J Am Med Dir Assoc 18(9):807. https://doi.org/10.1016/j.jamda.2017.05.011 (e809-807 e816)
Artero EG, Lee DC, Ruiz JR, Sui X, Ortega FB, Church TS, Lavie CJ, Castillo MJ, Blair SN (2011) A prospective study of muscular strength and all-cause mortality in men with hypertension. J Am Coll Cardiol 57(18):1831–1837. https://doi.org/10.1016/j.jacc.2010.12.025
Rantanen T, Guralnik JM, Foley D, Masaki K, Leveille S, Curb JD, White L (1999) Midlife hand grip strength as a predictor of old age disability. JAMA 281(6):558–560. https://doi.org/10.1001/jama.281.6.558
Takata Y, Ansai T, Soh I, Awano S, Yoshitake Y, Kimura Y, Nakamichi I, Goto K, Fujisawa R, Sonoki K, Yoshida A, Toyoshima K, Nishihara T (2012) Physical fitness and 6.5-year mortality in an 85-year-old community-dwelling population. Arch Gerontol Geriatr 54(1):28–33. https://doi.org/10.1016/j.archger.2011.04.014
Visser M, Goodpaster BH, Kritchevsky SB, Newman AB, Nevitt M, Rubin SM, Simonsick EM, Harris TB (2005) Muscle mass, muscle strength, and muscle fat infiltration as predictors of incident mobility limitations in well-functioning older persons. J Gerontol A Biol Sci Med Sci 60(3):324–333. https://doi.org/10.1093/gerona/60.3.324
Eckardt KU, Gillespie IA, Kronenberg F, Richards S, Stenvinkel P, Anker SD, Wheeler DC, de Francisco AL, Marcelli D, Froissart M, Floege J, Committee AROS (2015) High cardiovascular event rates occur within the first weeks of starting hemodialysis. Kidney Int 88(5):1117–1125. https://doi.org/10.1038/ki.2015.117
Mavrakanas TA, Charytan DM (2016) Cardiovascular complications in chronic dialysis patients. Curr Opin Nephrol Hypertens 25(6):536–544. https://doi.org/10.1097/MNH.0000000000000280
Usui T, Hanafusa N, Yasunaga H, Nangaku M (2019) Association of dialysis with in-hospital disability progression and mortality in community-onset stroke. Nephrology (Carlton) 24(7):737–743. https://doi.org/10.1111/nep.13242
Wheeler DC, London GM, Parfrey PS, Block GA, Correa-Rotter R, Dehmel B, Drueke TB, Floege J, Kubo Y, Mahaffey KW, Goodman WG, Moe SM, Trotman ML, Abdalla S, Chertow GM, Herzog CA, Investigators EVOCHTtLCET (2014) Effects of cinacalcet on atherosclerotic and nonatherosclerotic cardiovascular events in patients receiving hemodialysis: the evaluation of cinacalcet HCl therapy to lower cardiovascular events (EVOLVE) trial. J Am Heart Assoc 3(6):e001363. https://doi.org/10.1161/JAHA.114.001363
Lai S, Muscaritoli M, Andreozzi P, Sgreccia A, De Leo S, Mazzaferro S, Mitterhofer AP, Pasquali M, Protopapa P, Spagnoli A, Amabile MI, Molfino A (2019) Sarcopenia and cardiovascular risk indices in patients with chronic kidney disease on conservative and replacement therapy. Nutrition 62:108–114. https://doi.org/10.1016/j.nut.2018.12.005
Mori K, Nishide K, Okuno S, Shoji T, Emoto M, Tsuda A, Nakatani S, Imanishi Y, Ishimura E, Yamakawa T, Shoji S, Inaba M (2019) Impact of diabetes on sarcopenia and mortality in patients undergoing hemodialysis. BMC Nephrol 20(1):105. https://doi.org/10.1186/s12882-019-1271-8
Anderton N, Giri A, Wei G, Marcus RL, Chen X, Bjordahl T, Habib A, Herrera J, Beddhu S (2015) Sedentary behavior in individuals with diabetic chronic kidney disease and maintenance hemodialysis. J Ren Nutr 25(4):364–370. https://doi.org/10.1053/j.jrn.2015.01.018
Gomes EP, Reboredo MM, Carvalho EV, Teixeira DR, Carvalho LF, Filho GF, de Oliveira JC, Sanders-Pinheiro H, Chebli JM, de Paula RB, Pinheiro Bdo V (2015) Physical activity in hemodialysis patients measured by triaxial accelerometer. Biomed Res Int 2015:645645. https://doi.org/10.1155/2015/645645
More KM, Blanchard C, Theou O, Cranston A, Vinson AJ, Dipchand C, Kiberd B, Tennankore KK (2019) A location-based objective assessment of physical activity and sedentary behavior in ambulatory hemodialysis patients. Can J Kidney Health Dis 6:2054358119872967. https://doi.org/10.1177/2054358119872967
Hishii S, Miyatake N, Nishi H, Katayama A, Ujike K, Koumoto K, Suzuki H, Hashimoto H (2019) Relationship between sedentary behavior and all-cause mortality in Japanese chronic hemodialysis patients: a prospective cohort study. Acta Med Okayama 73(5):419–425. https://doi.org/10.18926/AMO/57372
O’Hare AM, Tawney K, Bacchetti P, Johansen KL (2003) Decreased survival among sedentary patients undergoing dialysis: results from the dialysis morbidity and mortality study wave 2. Am J Kidney Dis 41(2):447–454. https://doi.org/10.1053/ajkd.2003.50055
Kuki A, Tanaka K, Kushiyama A, Tanaka Y, Motonishi S, Sugano Y, Furuya T, Ozawa T (2019) Association of gait speed and grip strength with risk of cardiovascular events in patients on haemodialysis: a prospective study. BMC Nephrol 20(1):196. https://doi.org/10.1186/s12882-019-1370-6
Delmonico MJ, Harris TB, Visser M, Park SW, Conroy MB, Velasquez-Mieyer P, Boudreau R, Manini TM, Nevitt M, Newman AB, Goodpaster BH, Health A, Body (2009) Longitudinal study of muscle strength, quality, and adipose tissue infiltration. Am J Clin Nutr 90(6):1579–1585. https://doi.org/10.3945/ajcn.2009.28047
Correa-de-Araujo R, Harris-Love MO, Miljkovic I, Fragala MS, Anthony BW, Manini TM (2017) The need for standardized assessment of muscle quality in skeletal muscle function deficit and other aging-related muscle dysfunctions: a symposium report. Front Physiol 8:87. https://doi.org/10.3389/fphys.2017.00087
Goodpaster BH, Park SW, Harris TB, Kritchevsky SB, Nevitt M, Schwartz AV, Simonsick EM, Tylavsky FA, Visser M, Newman AB (2006) The loss of skeletal muscle strength, mass, and quality in older adults: the health, aging and body composition study. J Gerontol A Biol Sci Med Sci 61(10):1059–1064. https://doi.org/10.1093/gerona/61.10.1059
Moorthi RN, Avin KG (2017) Clinical relevance of sarcopenia in chronic kidney disease. Curr Opin Nephrol Hypertens 26(3):219–228. https://doi.org/10.1097/MNH.0000000000000318
Kim JK, Choi SR, Choi MJ, Kim SG, Lee YK, Noh JW, Kim HJ, Song YR (2014) Prevalence of and factors associated with sarcopenia in elderly patients with end-stage renal disease. Clin Nutr 33(1):64–68. https://doi.org/10.1016/j.clnu.2013.04.002
Nishi H, Takemura K, Higashihara T, Inagi R (2020) Uremic sarcopenia: clinical evidence and basic experimental approach. Nutrients. https://doi.org/10.3390/nu12061814
Delano MJ, Moldawer LL (2006) The origins of cachexia in acute and chronic inflammatory diseases. Nutr Clin Pract 21(1):68–81. https://doi.org/10.1177/011542650602100168
Stenvinkel P, Alvestrand A (2002) Inflammation in end-stage renal disease: sources, consequences, and therapy. Semin Dial 15(5):329–337. https://doi.org/10.1046/j.1525-139x.2002.00083.x
Kittiskulnam P, Chertow GM, Carrero JJ, Delgado C, Kaysen GA, Johansen KL (2017) Sarcopenia and its individual criteria are associated, in part, with mortality among patients on hemodialysis. Kidney Int 92(1):238–247. https://doi.org/10.1016/j.kint.2017.01.024
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hayashi, H., Izumiya, Y., Hayashi, O. et al. Dynapenia is an independent predictor of cardio-cerebrovascular events in patients undergoing hemodialysis. Heart Vessels 37, 1066–1074 (2022). https://doi.org/10.1007/s00380-021-02006-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00380-021-02006-7