Abstract
Objective
To quantify the distribution of cauda equina nerve roots in supine and upright positions using manual measurements and radiomics features both in normal subjects and in lumbar spinal canal stenosis (LSCS) patients.
Methods
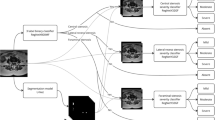
We retrospectively recruited patients who underwent weight-bearing MRI in supine and upright positions for back pain. 3D T2-weighted isotropic acquisition (3D-HYCE) sequences were used to develop a 3D convolutional neural network for identification and segmentation of lumbar vertebrae. Para-axial reformatted images perpendicular to the spinal canal and parallel to each vertebral endplate were automatically extracted. From each level, we computed the maximum antero-posterior (AP) and latero-lateral (LL) dispersion of nerve roots; further, radiomics features were extracted to quantify standardized metrics of nerve root distribution.
Results
We included 16 patients with LSCS and 20 normal subjects. In normal subjects, nerve root AP dispersion significantly increased from supine to upright position (p < 0.001, L2–L5 levels), and radiomics features showed an increase in non-uniformity. In LSCS subjects, in the upright position AP dispersion of nerve roots and entropy-related features increased caudally to the stenosis level (p < 0.001) and decreased cranially (p < 0.001). Moreover, entropy-related radiomics features negatively correlated with pre-operative Pain Numerical Rating Scale. Comparison between normal subjects and LSCS patients showed a difference in AP dispersion and increase of variance cranially to the stenosis level (p < 0.001) in the upright position.
Conclusions
Nerve root distribution inside the dural sac changed between supine and upright positions, and radiomics features were able to quantify the differences between normal and LSCS subjects.
Clinical relevance statement
The distribution of cauda equina nerve roots and the redundant nerve root sign significantly varies between supine and upright positions in normal subjects and spinal canal stenosis patients, respectively. Radiomics features quantify nerve root dispersion and correlates with pain severity.
Key Points
• Weight-bearing MRI depicts spatial distribution of the cauda equina in both supine and upright positions in normal subjects and spinal stenosis patients.
• Radiomics features can quantify the effects of spinal stenosis on the dispersion of the cauda equina in the dural sac.
• In the orthostatic position, dispersion of nerve roots is different in lumbar spinal stenosis patients compared to that in normal subjects; entropy-related features negatively correlated with pre-operative Pain Numerical Rating Scale.






Similar content being viewed by others
Abbreviations
- 3D-HYCE:
-
3D hybrid contrast-enhanced
- AP:
-
Antero-posterior
- CNN:
-
Convolutional neuronal network
- CSF:
-
Cerebrospinal fluid
- GLCM:
-
Gray-level cooccurrence matrix
- GLDM:
-
Gray-level dependence matrix
- GLRLM:
-
Gray-level run length matrix
- GLSZM:
-
Gray-level size zone matrix
- ICC:
-
Intraclass correlation coefficient
- LL:
-
Latero-lateral
- LSCS:
-
Lumbar spinal canal stenosis
- MPR:
-
Multi-planar reformatted
- NGTDM:
-
Neighboring gray tone difference matrix
- PNRS:
-
Pain Numerical Rating Scale
- RNR:
-
Redundant nerve roots
- wbMRI:
-
Weight-bearing magnetic resonance imaging
References
Lurie J, Tomkins-Lane C (2016) Management of lumbar spinal stenosis. BMJ h6234. https://doi.org/10.1136/bmj.h6234
Katz JN, Zimmerman ZE, Mass H, Makhni MC (2022) Diagnosis and management of lumbar spinal stenosis: a review. JAMA 327:1688–1699. https://doi.org/10.1001/jama.2022.5921
Ravindra VM, Senglaub SS, Rattani A et al (2018) Degenerative lumbar spine disease: estimating global incidence and worldwide volume. Global Spine J 8:784–794. https://doi.org/10.1177/2192568218770769
Lee MJ, Cassinelli EH, Riew KD (2007) Prevalence of cervical spine stenosis. Anatomic study in cadavers. J Bone Joint Surg Am 89:376–380. https://doi.org/10.2106/JBJS.F.00437
Lee S, Lee JW, Yeom JS et al (2010) A practical MRI grading system for lumbar foraminal stenosis. AJR Am J Roentgenol 194:1095–1098. https://doi.org/10.2214/AJR.09.2772
Schizas C, Theumann N, Burn A et al (2010) Qualitative grading of severity of lumbar spinal stenosis based on the morphology of the dural sac on magnetic resonance images. Spine (Phila Pa 1976) 35:1919–1924. https://doi.org/10.1097/BRS.0b013e3181d359bd
Huang C-C, Jaw F-S, Young Y-H (2022) Radiological and functional assessment in patients with lumbar spinal stenosis. BMC Musculoskelet Disord 23:137. https://doi.org/10.1186/s12891-022-05053-x
Xu J, Hu Y (2021) Clinical features and efficacy analysis of redundant nerve roots. Front Surg. https://doi.org/10.3389/fsurg.2021.628928
Hansen BB, Nordberg CL, Hansen P et al (2019) Weight-bearing MRI of the lumbar spine: spinal stenosis and spondylolisthesis. Semin Musculoskelet Radiol 23:621–633. https://doi.org/10.1055/s-0039-1697937
Lau YYO, Lee RKL, Griffith JF, Chan CLY, Law SW, Kwok KO (2017) Changes in dural sac caliber with standing MRI improve correlation with symptoms of lumbar spinal stenosis. Eur Spine J 26:2666–2675. https://doi.org/10.1007/s00586-017-5211-7
Isensee F, Jaeger PF, Kohl SAA, Petersen J, Maier-Hein KH (2021) nnU-Net: a self-configuring method for deep learning-based biomedical image segmentation. Nat Methods 18:203–211. https://doi.org/10.1038/s41592-020-01008-z
van Griethuysen JJM, Fedorov A, Parmar C et al (2017) Computational radiomics system to decode the radiographic phenotype. Cancer Res 77:e104–e107. https://doi.org/10.1158/0008-5472.CAN-17-0339
Zwanenburg A, Vallières M, Abdalah MA et al (2020) The image biomarker standardization initiative: standardized quantitative radiomics for high-throughput image-based phenotyping. Radiology 295:328–338. https://doi.org/10.1148/radiol.2020191145
Minetama M, Kawakami M, Teraguchi M et al (2022) MRI grading of spinal stenosis is not associated with the severity of low back pain in patients with lumbar spinal stenosis. BMC Musculoskelet Disord 23:e857. https://doi.org/10.1186/s12891-022-05810-y
Acknowledgements
We acknowledge ESAOTE s.p.a for the technical support. We also acknowledge Luca Carbone and Elisa Fabbri for the assistance during the MRI acquisitions.
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is prof. Letterio S. Politi.
Conflict of interest
The authors of this manuscript declare relationships with the following companies: R. Levi received funding for Ph.D. fellowship by ESAOTE s.p.a. The other authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
R. Levi is a member of the European Radiology Editorial Board. He has not taken part in the review or selection process of this article.
Statistics and biometry
One of the authors has significant statistical expertise.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
The IRB was waived by the institutional Ethics Committee of the IRCCS Humanitas Clinical Research Hospital (Milan, Italy), due to the retrospective nature of the study. All the participants signed a general informed consent for MRI and for providing anonymized information for scientific studies.
Study subjects or cohorts overlap
Not applicable.
Methodology
• Retrospective
• Cross-sectional study
• Performed at one institution
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Levi, R., Battaglia, M., Garoli, F. et al. Quantification of cauda equina nerve root dispersion through radiomics features in weight-bearing MRI in normal subjects and spinal canal stenosis patients. Eur Radiol (2023). https://doi.org/10.1007/s00330-023-10467-9
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00330-023-10467-9