Abstract
Objectives
Multiple lung cancer screening studies reported the performance of Lung CT Screening Reporting and Data System (Lung-RADS), but none systematically evaluated its performance across different populations. This systematic review and meta-analysis aimed to evaluate the performance of Lung-RADS (versions 1.0 and 1.1) for detecting lung cancer in different populations.
Methods
We performed literature searches in PubMed, Web of Science, Cochrane Library, and Embase databases on October 21, 2022, for studies that evaluated the accuracy of Lung-RADS in lung cancer screening. A bivariate random-effects model was used to estimate pooled sensitivity and specificity, and heterogeneity was explored in stratified and meta-regression analyses.
Results
A total of 31 studies with 104,224 participants were included. For version 1.0 (27 studies, 95,413 individuals), pooled sensitivity was 0.96 (95% confidence interval [CI]: 0.90–0.99) and pooled specificity was 0.90 (95% CI: 0.87–0.92). Studies in high-risk populations showed higher sensitivity (0.98 [95% CI: 0.92–0.99] vs. 0.84 [95% CI: 0.50–0.96]) and lower specificity (0.87 [95% CI: 0.85–0.88] vs. 0.95 (95% CI: 0.92–0.97]) than studies in general populations. Non-Asian studies tended toward higher sensitivity (0.97 [95% CI: 0.91–0.99] vs. 0.91 [95% CI: 0.67–0.98]) and lower specificity (0.88 [95% CI: 0.85–0.90] vs. 0.93 [95% CI: 0.88–0.96]) than Asian studies. For version 1.1 (4 studies, 8811 individuals), pooled sensitivity was 0.91 (95% CI: 0.83–0.96) and specificity was 0.81 (95% CI: 0.67–0.90).
Conclusion
Among studies using Lung-RADS version 1.0, considerable heterogeneity in sensitivity and specificity was noted, explained by population type (high risk vs. general), population area (Asia vs. non-Asia), and cancer prevalence.
Clinical relevance statement
Meta-regression of lung cancer screening studies using Lung-RADS version 1.0 showed considerable heterogeneity in sensitivity and specificity, explained by the different target populations, including high-risk versus general populations, Asian versus non-Asian populations, and populations with different lung cancer prevalence.
Key Points
• High-risk population studies showed higher sensitivity and lower specificity compared with studies performed in general populations by using Lung-RADS version 1.0.
• In non-Asian studies, the diagnostic performance of Lung-RADS version 1.0 tended to be better than in Asian studies.
• There are limited studies on the performance of Lung-RADS version 1.1, and evidence is lacking for Asian populations.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lung cancer remains the leading cause of cancer-related death, with a 5-year survival of just 10–20% [1]. Results from large-scale multicenter studies offer hope, showing that screening by low-dose computed tomography (LDCT) can detect lung cancer at an early stage [2,3,4]. Apart from structural differences in screening approaches, false-positive rates can be decreased without substantially decreasing the sensitivity of cancer detection by optimizing the definition of a positive screen [5, 6], and cost-effectiveness can be improved by ensuring appropriate management algorithms for positive results [7].
Protocols to perform lung cancer screening have been developed in Western countries. The American College of Radiology released “Lung CT Screening Reporting and Data System (Lung-RADS)” version 1.0 in 2014 [8] based on published caption data from the United States National Lung Screening Trial (NLST), Dutch–Belgian Lung cancer screening trial (NELSON), and International Early Lung Cancer Action Program (I-ELCAP) [2, 3, 9, 10]. Lung-RADS has become one of the most widely used reporting and management aids for screen-detected nodules worldwide. Applied to the NLST population, version 1.0 effectively and considerably decreased the false-positive rate, at the cost of only a slight decrease in the false-negative rate, by increasing the size threshold for a positive baseline screen from 4 mm (greatest diameter) to 6 mm (average diameter) [11]. Whereafter, the Korean Lung Cancer Screening Project (K-LUCAS), the first Asian population-based, multicenter prospective lung cancer screening program, also adopted version 1.0 [12].
Lung-RADS version 1.1 was published in 2019 [8] and introduced three major changes based on rolling evidence. First, it increased the upper size limit for non-solid nodules in Lung-RADS category 3 from 20 to 30 mm based on evidence that these non-solid nodules follow an indolent course [13, 14] with little risk when continuing annual follow-up [15, 16]. Second, it down-classified perifissural nodules measuring < 10 mm to Lung-RADS category 2 to reduce false positives given that these are typically benign [17, 18]. Third, it added volumetric measurements to monitor the nodule growth rate and improve the ability to predict malignancy [19, 20]. This revision further decreased the false-positive rate for a subset of NLST participants with non-calcified nodules [21]. Lung-RADS version 2022 was recently released (November 2022), and thus far, no published studies have evaluated this newest version [22].
Several systematic reviews or meta-analyses assessed the performance of lung cancer screening by LDCT [23, 24], but the included studies adopted various definitions of positive screens and management algorithms. We found no prior systematic validation of the diagnostic performance of a standardized management protocol in LDCT lung cancer screening, and the performance across different target populations, such as high-risk versus general populations and Asian versus non-Asian populations. This systematic review and meta-analysis aimed to evaluate the diagnostic performance of Lung-RADS (versions 1.0 and 1.1) for detecting lung cancer in different target populations and explore which characteristics of target population can impact the performance.
Materials and methods
Study design
We followed the Preferred Reporting Items for Systematic Reviews of Diagnostic Test Accuracy (PRISMA-DTA) guidelines [25] and the Cochrane Handbook for Systematic Reviews of Diagnostic Test Accuracy (version 2.0, 2022) [26], and registered our study protocol in the international prospective register of systematic reviews, or PROSPERO (no. CRD42022311028). Two radiologists (3 and 5 years’ experience in lung cancer screening) independently screened the literature, selected studies, collected and extracted data, and assessed quality, resolving differences of opinion by consensus or discussion with a third radiologist (> 10 years’ experience in lung cancer screening).
Search strategy and literature screening
Literature searches of PubMed, Web of Science, Cochrane Library, and Embase were performed on 21 October 2022 using the strategies listed in Table 1, without language restrictions. Our search was based on the following keywords for lung cancer and Lung-RADS: (Lung Neoplasms OR lung OR pulmonary) AND (lung-RADS OR lungRADS OR lu-rads OR lurads OR RADS OR (reporting AND data-system)). And no filters were applied. Studies published before 2014 and duplicates were excluded using EndNote X8.
We screened titles, abstracts, and full texts of articles, and selected studies containing data for populations (a) screened for lung cancer, (b) screened by LDCT, (c) where a Lung-RADS protocol was applied for lung nodule management, (d) where the clinical or histopathological diagnosis of lung cancer was used as the reference standard, and (e) that included the diagnostic performance of Lung-RADS. Studies were excluded if they met any of the following criteria: (a) review, case reports, conference abstracts, editorials, or book chapters; (b) studies without sufficient data on 2 × 2 contingency tables; and (c) studies with data from the same cohort. When articles used data from the same cohort, we only included the article that included the largest population.
Data extraction and definitions
We used standardized data extraction forms to collect the following items from each included study: first author name, publication year, country, Lung-RADS version, study design (retrospective or prospective), baseline inclusion period, number of screened participants, number of positive screens, number of lung cancers, age (mean, median, and range), sex, smoking status, lung nodule number and type (solid, part solid, or ground glass), reference standard for lung cancer, and eligibility criteria. The reference standard for lung cancer was grouped as “pathology alone” (e.g., pathological proof only) or “pathology and other methods” (e.g., pathological proof or repeat CT, PET, multidisciplinary consensus). If some data were not available in the main text, supplementary files, or their references, we contacted the authors to resolve the missing data.
The Lung-RADS algorithm distinguishes baseline and follow-up screenings, with nodule categorization based on nodule type and size at baseline, and then also considering nodule pre-existence and growth rate at follow-up. Each Lung-RADS category has specific management recommendations: categories 1 and 2 indicate “negative screens” suitable for continued annual screening, while categories 3 and 4 indicate “positive screens” suitable for referral for additional screening or interventions before the next annual screening [8].
Finally, we recorded the population type, population area, and lung cancer prevalence from the extracted data, and studies were stratified based on these items. First, for population type, this was stratified into “high risk” and “general” based on smoking status. Studies with high-risk populations either used inclusion criteria based on smoking status (e.g., NLST selection criteria [2], NCCN high-risk criteria [27], USPSTF criteria [28], PLCOm2012 [29]) or only included participants who smoked. By contrast, studies with general populations either used inclusion criteria based on factors other than the smoking history or included both current, former, and never smokers. Second, studies were stratified by their geographic area into Asia and non-Asia groups. Third, regarding the prevalence of lung cancer, studies were stratified into two groups based on the median prevalence [30].
Quality assessment
The quality of included studies was evaluated with the Quality Assessment of Diagnostic Accuracy Studies (QUADAS-2) tool (Table S1) in Review Manager (RevMan, version 5.4. Copenhagen: The Cochrane Collaboration, 2020). QUADAS-2 is a structured checklist comprising four domains, namely patient selection, index test, reference standard, and flow and timing. The risk of bias was assessed using two or three signaling questions for each of the four domains, and concern about applicability was evaluated with one signaling question for the first three domains only. These seven items were then judged as “low,” “high,” or “unclear” [31].
Data synthesis and analysis
To calculate the sensitivity and specificity for lung cancer detection in the included studies, we constructed 2 × 2 contingency tables. A bivariate random-effects model was used to estimate the pooled sensitivity and specificity with their 95% CIs and represented in forest plots. Heterogeneity among studies was assessed using the Cochran Q test (p < 0.05 indicated heterogeneity) and Higgins inconsistency index (I2 ≥ 50% suggested substantial heterogeneity) [32, 33]. If heterogeneity was observed, we performed stratified and meta-regression analyses to explore the likely source. Stratified analyses were performed based on the following covariates: population type (high risk or general population), population area (Asia or non-Asia), study design (retrospective or prospective), reference standard (pathology alone, or pathology and other methods), and lung cancer prevalence (less or more than median). Publication bias was tested using Deeks’ funnel plot. For data analysis, the Midas module [34] in Stata 15.0 (StataCorp) was applied in the present study.
Results
Study selection and characteristics
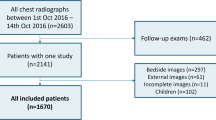
Figure 1 shows the literature search and study selection processes. The initial search yielded 2243 articles, from which we excluded 753 studies published before 2014 and a further 630 duplicates. We then excluded 733 articles by title and abstract screening and a further 96 by full-text screening. This left 31 eligible articles [11, 21, 35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63] comprising 104,224 participants for analysis.
Table 2 shows the study and patient characteristics for the included articles. Of the 31 studies, 27 only evaluated version 1.0, three only evaluated version 1.1, and one assessed both versions, but only the version 1.1 result was extracted. All included studies applied Lung-RADS at baseline screening, and only two (11, 57) separately evaluated it at baseline and follow-up. The studies were performed in nine countries, with the USA (54.8%, 17/31), China (9.7%, 3/31), South Korea (9.7%, 3/31), and Canada (6.5%, 2/31) as the most common. For the high-risk population, we identified 24 studies [11, 21, 35, 37,38,39, 43,44,45,46, 48,49,50, 52,53,54,55,56,57,58,59,60,61,62] that included only current or former smokers and one study that included 99.3% current or former smokers [36]. For the general population, we only identified five studies [40, 41, 47, 51, 63] that included both current, former, and never smokers and one study [42] that included only female never smokers. The median prevalence of lung cancer was 1.9% (range, 0.5–7.8%) for version 1.0 studies, including 14 with ≥ 1.9% prevalence, and 13 with < 1.9% prevalence, and was 2.4% (range, 2.0–3.9%) for version 1.1 studies.
Study quality
Overall, 13 studies satisfied all seven items of the QUADAS-2 checklist (Figure S1 and Table S2), 28 satisfied at least six items, and all 31 satisfied at least four items, suggesting a reasonable overall study quality (Figure S1). In the patient selection domain, two studies [21, 52] showed high risk of bias and high concern for applicability; these studies only included patients with non-calcified nodules, thereby excluding Lung-RADS category 1 (patients with calcified nodules and without nodules). Regarding flow and timing, nine studies showed an unclear risk of bias and six showed a high risk of bias. Eight studies [36, 43, 44, 46,47,48, 50, 55, 59] showed unclear risk of bias because they lacked sufficient information to determine the interval between Lung-RADS classification and lung cancer diagnosis. Among the studies with a high risk of bias, two [21, 35] included less than 90% of screened participants in the evaluation of Lung-RADS and six [35, 36, 45, 56, 60] applied different reference standards for lung cancer diagnosis. All included studies provided optimal scores for the index and reference standards.
Diagnostic performance of Lung-RADS version 1.0
The diagnostic performance of Lung-RADS version 1.0 at baseline was assessed in 27 studies with 95,413 participants [11, 35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53, 55,56,57,58,59, 62, 63]. These showed a pooled sensitivity of 0.96 (95% CI: 0.90–0.99) and a pooled specificity of 0.90 (95% CI: 0.87–0.92) (Fig. 2 and Table 3). We found substantial heterogeneity for both sensitivity (p < 0.001, I2 = 89.0%) and specificity (p < 0.001, I2 = 99.3%) across the studies. Meta-regression analysis showed that population type (p < 0.001), population area (p = 0.02), and lung cancer prevalence (p = 0.02) were significant covariates affecting heterogeneity among studies using version 1.0 (Table 3). Neither study design nor reference standard for lung cancer posed significant sources of heterogeneity (p > 0.05). Overall, the high-risk populations (n = 21; 54,384 individuals) showed higher sensitivity (0.98; 95% CI: 0.92–0.99) and lower specificity (0.87; 95% CI: 0.85–0.88) compared with general populations (n = 6; 41,029 individuals), where the corresponding values were 0.84 (95% CI: 0.50–0.96) and 0.95 (95% CI: 0.92–0.97), respectively (Table 3). The 95% CIs for both sensitivity and specificity overlapped when comparing Asia and non-Asia areas. However, studies outside Asia (n = 19; 49,102 individuals) tended to have a higher sensitivity (0.97; 95% CI: 0.91–0.99) and lower specificity (0.88; 95% CI: 0.85–0.90) compared with those performed in Asia (n = 8, 46,311 individuals), where the sensitivity was 0.91 (95% CI: 0.67–0.98) and the specificity was 0.93 (95% CI: 0.88–0.96) (Table 3). In addition, 95% CIs overlapped when comparing groups by a lung cancer prevalence < 1.9% (n = 13; 83,870 individuals; sensitivity, 0.97 [0.84–0.99]; specificity, 0.92 [0.88–0.94]) and ≥ 1.9% (n = 14; 11,543 individuals; sensitivity, 0.96 [0.86–0.99]; specificity, 0.87 [0.84–0.89]) (Table 3).
Diagnostic performance of Lung-RADS version 1.1
Four studies with 8811 participants [21, 54, 60, 61], all comprising high-risk populations outside Asia, examined the diagnostic performance of Lung-RADS version 1.1 at baseline. The pooled sensitivity and specificity were 0.91 (95% CI: 0.83–0.96) and 0.81 (95% CI: 0.67–0.90), respectively (Fig. 3 and Table 3). We found substantial heterogeneity for both sensitivity (p < 0.001, I2 = 86.8%) and specificity (p < 0.001, I2 = 99.5%) among the studies.
Publication bias
Studies that assessed Lung-RADS version 1.0 showed no publication bias according to Deeks’ funnel plot (p = 0.44; Figure S2). However, publication bias could not be analyzed for Lung-RADS version 1.1 because of the limited number of studies.
Discussion
In this systematic review and meta-analysis, we assessed the diagnostic performances of Lung-RADS in lung cancer screening by LDCT. Our data showed that Lung-RADS version 1.0 had a pooled sensitivity of 96% (95% CI: 0.90–0.99) and specificity of 90% (95% CI: 0.87–0.92). Lung-RADS version 1.1 retained a similar pooled sensitivity (0.91; 95% CI: 0.83–0.96) but had suboptimal specificity (0.81; 95% CI: 0.67–0.90), which was based on a limited number of non-Asian studies.
For version 1.0, our results showed that studies in high-risk populations had higher sensitivity and somewhat lower specificity than studies in general populations. This suggests that Lung-RADS version 1.0 is more applicable to high-risk populations, consistent with the development of version 1.0 with published data from lung cancer screening trials that targeted high-risk populations [2, 3, 9, 10]. In addition, studies of version 1.0 outside Asia tended to show higher sensitivity and lower specificity compared with studies in Asia. Notably, all 19 studies outside Asia targeted high-risk populations, contrasting with only two out of eight in Asia [53, 59]. Nonetheless, compared with the studies outside Asia, both studies in high-risk Asian populations showed similar sensitivities and lower specificities. Studies in general Asian populations (n = 6) showed lower sensitivities and higher specificities than those studies, but due to the limited number in high-risk populations, we could not draw firm conclusions about either the most applicable population type for version 1.0 in Asia or where version 1.0 could have the greatest effect for those at high risk.
Lung-RADS was designed for the lung cancer screening, and as such, this meta-analysis only included screening studies. Most screening studies included high-risk populations, and in these studies, a high-risk population is mainly determined by smoking criteria. However, evidence has now shown that the proportion of lung cancer is higher in Asian than in Western never smokers, with about one-third of lung cancers in East Asia found in never smokers [64, 65]. Therefore, it may be reasonable that in the future, eligibility criteria for lung cancer screening will be extended, and screening will also be performed in never or less heavy smokers [66]. Nonetheless, our meta-analysis also indicates that targeting a general population using Lung-RADS version 1.0 in Asia will not necessarily result in the same high sensitivity found outside Asia in high-risk populations. This underscores the fact that the definition for “high risk” needs to be optimized and that the classification in Lung-RADS might need revising to improve its applicability in Asia. Other risk factors, such as emphysema, passive smoking, air pollution, fireplace fume exposure, and family history of lung cancer, may be included in the eligibility criteria [66, 67]. Moreover, in the latest 2021 USPSTF Criteria, the minimum age of eligibility criteria was lowered from 55 to 50 years, and other scientific societies may consider lowering the starting age as well [28].
Lung-RADS version 1.1 tended to show lower sensitivity and specificity compared with version 1.0, although the 95% CIs for both overlapped. We only identified four studies using Lung-RADS version 1.1. Among them, although the study by Kastner et al [21] evaluated both versions of Lung-RADS, we only extracted their results for version 1.1. Moreover, the study included participants with non-calcified nodules and excluded those with Lung-RADS category 1. This have undoubtedly led to an underestimation in the specificity of version 1.1 compared with the other studies. Thus, we cannot reach a reliable conclusion about the diagnostic performance of Lung-RADS version 1.1, or indeed, determine which version performs better for LDCT lung cancer screening in different areas. By contrast, Kastner et al [21] have reported conflicting results; Lung-RADS version 1.1 outperformed version 1.0, with the more recent version showing higher specificity at the cost of only a minimal decrease in sensitivity. It should be noted that their study population was at high risk (NLST population), whereas the current meta-analysis also included studies in general populations. Moreover, all four studies using version 1.1 were performed outside Asia. Therefore, more studies are needed to give more precise estimates of the diagnostic performance of Lung-RADS version 1.1 for lung cancer screening, especially in Asia.
Only one recently published meta-analysis on the performance of LDCT lung cancer screening reported the pooled sensitivity and specificity of Lung-RADS protocol in the stratified analysis, but without further discussion [24]. This recent meta-analysis included only nine studies using Lung-RADS version 1.0 and no studies using version 1.1. Additionally, only one study was performed in an Asian general population. Thus, our current study expands the evidence to Lung-RADS version 1.1 and Asian population.
Considerable heterogeneity was noted among studies using both versions. Stratified and meta-regression analyses revealed that population type, population area, and lung cancer prevalence could explain part of heterogeneity among studies using Lung-RADS version 1.0. Generally, population type and area affect the population case mix (e.g., participants requiring additional tests or procedures) and disease prevalence, which could have caused the diagnostic accuracy of Lung-RADS to vary [68, 69]. Thus, these three factors are expected causes of study heterogeneity when using Lung-RADS.
This study has several limitations. First, we could not evaluate Lung-RADS management algorithms for follow-up screening, due to the limited number of studies that evaluated Lung-RADS at follow-up. Second, the proportion of lung cancers manifesting as subsolid nodules is much higher in Asia than in Western countries [70], which could result in the differences of Lung-RADS performance between Asia and non-Asia. In addition, to decrease the false-positive rates, version 1.1 added the identification and classification of perifissural nodules. However, only five included studies reported the proportion of subsolid nodules [21, 41, 47, 50, 61], and only one mentioned that of perifissural nodules [21]. Due to limited data, we could not evaluate the performance of Lung-RADS by nodule type, e.g., subsolid or perifissural nodules. Third, the included studies contained inadequate data about follow-up duration for lung cancer diagnosis, the experience of radiologists who read CT scans, and the quality of the CT images, so we cannot assess the impact of these factors on heterogeneity. Fourth, we identified only a few studies using version 1.1, likely because of its comparatively recent publication in 2019. The study by Kastner et al that accounted for a large proportion of the version 1.1 subset also showed a high risk of selection bias, preventing any firm conclusion about which version had the better diagnostic performance.
In conclusion, this systematic review and meta-analysis showed that there is a considerable heterogeneity in sensitivity and specificity among lung cancer screening studies using Lung-RADS version 1.0, explained by population type (high-risk versus general), population area (Asia versus non-Asia), and lung cancer prevalence. There are limited studies using Lung-RADS version 1.1 and data is lacking for Asian populations.
Abbreviations
- CI:
-
Confidence interval
- LDCT:
-
Low-dose computed tomography
- Lung-RADS:
-
Lung CT Screening Reporting and Data System
- NLST:
-
National Lung Screening Trial
- QUADAS:
-
Quality Assessment of Diagnostic Accuracy Studies
References
Sung H, Ferlay J, Siegel RL et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71:209–249. https://doi.org/10.3322/caac.21660
Team NLSTR (2011) Reduced lung-cancer mortality with low-dose computed tomographic screening. N Engl J Med 365:395–409. https://doi.org/10.1056/NEJMoa1102873
de Koning HJ, van der Aalst CM, de Jong PA et al (2020) Reduced lung-cancer mortality with volume CT screening in a randomized trial. N Engl J Med 382:503–513. https://doi.org/10.1056/NEJMoa1911793
Pastorino U, Silva M, Sestini S et al (2019) Prolonged lung cancer screening reduced 10-year mortality in the MILD trial: new confirmation of lung cancer screening efficacy. Ann Oncol 30:1162–1169. https://doi.org/10.1093/annonc/mdz117
Gierada DS, Pinsky P, Nath H et al (2014) Projected outcomes using different nodule sizes to define a positive CT lung cancer screening examination. J Natl Cancer Inst 106:dju284. https://doi.org/10.1093/jnci/dju284
Heuvelmans MA, Oudkerk M, de Bock GH et al (2013) Optimisation of volume-doubling time cutoff for fast-growing lung nodules in CT lung cancer screening reduces false-positive referrals. Eur Radiol 23:1836–1845. https://doi.org/10.1007/s00330-013-2799-9
Pinsky PF (2014) Assessing the benefits and harms of low-dose computed tomography screening for lung cancer. Lung Cancer Manag 3:491–498. https://doi.org/10.2217/lmt.14.41
American College of Radiology Committee on Lung-RADS® (2019) Lung-RADS assessment categories, version 1.1. Available via https://www.acr.org/Clinical-Resources/Reporting-and-Data-Systems/Lung-Rads. Accessed 1 May 2021
Horeweg N, Scholten ET, de Jong PA et al (2014) Detection of lung cancer through low-dose CT screening (NELSON): a prespecified analysis of screening test performance and interval cancers. Lancet Oncol 15:1342–1350. https://doi.org/10.1016/S1470-2045(14)70387-0
Henschke CI, Yip R, Yankelevitz DF, Smith JP (2013) Definition of a positive test result in computed tomography screening for lung cancer. Ann Intern Med 158:246–252. https://doi.org/10.7326/0003-4819-158-4-201302190-00004
Pinsky PF, Gierada DS, Black W et al (2015) Performance of Lung-RADS in the national lung screening trial: a retrospective assessment. Ann Intern Med 162:485–491. https://doi.org/10.7326/M14-2086
Lee J, Lim J, Kim Y et al (2019) Development of protocol for Korean Lung Cancer Screening Project (K-LUCAS) to evaluate effectiveness and feasibility to implement national cancer screening program. Cancer Res Treat 51:1285–1294. https://doi.org/10.4143/crt.2018.464
Matsuguma H, Mori K, Nakahara R et al (2013) Characteristics of subsolid pulmonary nodules showing growth during follow-up with CT scanning. Chest 143:436–443. https://doi.org/10.1378/chest.11-3306
Chang B, Hwang JH, Choi Y-H et al (2013) Natural history of pure ground-glass opacity lung nodules detected by low-dose CT scan. Chest 143:172–178. https://doi.org/10.1378/chest.11-2501
Gulati CM, Schreiner AM, Libby DM et al (2014) Outcomes of unresected ground-glass nodules with cytology suspicious for adenocarcinoma. J Thorac Oncol 9:685–691. https://doi.org/10.1097/JTO.0000000000000143
Heuvelmans MA, Walter JE, Oudkerk M (2018) Management of baseline and new sub-solid nodules in CT lung cancer screening. Expert Rev Respir Med 12:1–3. https://doi.org/10.1080/17476348.2018.1398087
de Hoop B, van Ginneken B, Gietema H, Prokop M (2012) Pulmonary perifissural nodules on CT scans: rapid growth is not a predictor of malignancy. Radiology 265:611–616. https://doi.org/10.1148/radiol.12112351
Ahn MI, Gleeson TG, Chan IH et al (2010) Perifissural nodules seen at CT screening for lung cancer. Radiology 254:949–956. https://doi.org/10.1148/radiol.09090031
Korst RJ, Lee BE, Krinsky GA, Rutledge JR (2011) The utility of automated volumetric growth analysis in a dedicated pulmonary nodule clinic. J Thorac Cardiovasc Surg 142:372–377. https://doi.org/10.1016/j.jtcvs.2011.04.015
Mehta HJ, Ravenel JG, Shaftman SR et al (2014) The utility of nodule volume in the context of malignancy prediction for small pulmonary nodules. Chest 145:464–472. https://doi.org/10.1378/chest.13-0708
Kastner J, Hossain R, Jeudy J et al (2021) Lung-RADS version 1.0 versus Lung-RADS version 1.1: comparison of categories using nodules from the National Lung Screening Trial. Radiology 300:199–206. https://doi.org/10.1148/radiol.2021203704
American College of Radiology Committee on Lung-RADS® (2022) Lung-RADS assessment categories 2022. Available via https://www.acr.org/-/media/ACR/Files/RADS/Lung-RADS/Lung-RADS-2022.pdf. Accessed 1 Jan 2023
Jonas DE, Reuland DS, Reddy SM et al (2021) Screening for lung cancer with low-dose computed tomography: updated evidence report and systematic review for the US Preventive Services Task Force. JAMA 325:971. https://doi.org/10.1001/jama.2021.0377
Guo L, Yu Y, Yang F et al (2023) Accuracy of baseline low-dose computed tomography lung cancer screening: a systematic review and meta-analysis. Chin Med J Publish. https://doi.org/10.1097/CM9.0000000000002353
McInnes MDF, Moher D, Thombs BD et al (2018) Preferred reporting items for a systematic review and meta-analysis of diagnostic test accuracy studies: the PRISMA-DTA statement. JAMA 319:388. https://doi.org/10.1001/jama.2017.19163
Cochrane Screening and Diagnostic Test Methods Group (2022) Cochrane handbook for systematic reviews of diagnostic test accuracy, version 2.0. Available via https://training-cochrane-org.proxy-ub.rug.nl/handbook-diagnostic-test-accuracy. Accessed 1 Jan 2023
Ettinger DS, Wood DE, Aisner DL et al (2021) NCCN guidelines insights: non-small cell lung cancer, version 2.2021. J Natl Compr Canc Netw 19:254–266. https://doi.org/10.6004/jnccn.2021.0013
US Preventive Services Task Force, Krist AH, Davidson KW et al (2021) Screening for lung cancer: US preventive services task force recommendation statement. JAMA 325:962–970. https://doi.org/10.1001/jama.2021.1117
Tammemägi MC, Katki HA, Hocking WG et al (2013) Selection criteria for lung-cancer screening. N Engl J Med 368:728–736. https://doi.org/10.1056/NEJMoa1211776
DeCoster J, Gallucci M, Iselin A-MR (2011) Best practices for using median splits, artificial categorization, and their continuous alternatives. J Exp Psychopathol 2:197–209. https://doi.org/10.5127/jep.008310
Whiting PF, Rutjes AWS, Westwood ME et al (2011) QUADAS-2: a revised tool for the quality assessment of diagnostic accuracy studies. Ann Intern Med 155:529–536. https://doi.org/10.7326/0003-4819-155-8-201110180-00009
Higgins JPT, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21:1539–1558. https://doi.org/10.1002/sim.1186
Higgins JPT, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560. https://doi.org/10.1136/bmj.327.7414.557
Dwamena B (2009) MIDAS: Stata module for meta-analytical integration of diagnostic test accuracy studies. Available via https://ideas.repec.org/c/boc/bocode/s456880.html. Accessed 1 May 2021
McKee BJ, Regis SM, McKee AB et al (2016) Performance of ACR Lung-RADS in a clinical CT lung screening program. J Am Coll Radiol 13:R25–R29. https://doi.org/10.1016/j.jacr.2015.12.009
Halpenny DF, Cunningham JD, Long NM et al (2016) Patients with a previous history of malignancy undergoing lung cancer screening: clinical characteristics and radiologic findings. J Thorac Oncol 11:1447–1452. https://doi.org/10.1016/j.jtho.2016.05.006
Guichet PL, Liu BY, Desai B et al (2018) Preliminary results of lung cancer screening in a socioeconomically disadvantaged population. AJR Am J Roentgenol 210:489–496. https://doi.org/10.2214/AJR.17.18853
Jacobs CD, Jafari ME (2017) Early results of lung cancer screening and radiation dose assessment by low-dose CT at a community hospital. Clin Lung Cancer 18:e327–e331. https://doi.org/10.1016/j.cllc.2017.01.011
Marshall HM, Zhao H, Bowman RV et al (2017) The effect of different radiological models on diagnostic accuracy and lung cancer screening performance. Thorax 72:1147–1150. https://doi.org/10.1136/thoraxjnl-2016-209624
Hsu H-T, Tang E-K, Wu M-T et al (2018) Modified Lung-RADS improves performance of screening LDCT in a population with high prevalence of non–smoking-related lung cancer. Acad Radiol 25:1240–1251. https://doi.org/10.1016/j.acra.2018.01.012
Kang H-R, Cho JY, Lee SH et al (2019) Role of low-dose computerized tomography in lung cancer screening among never-smokers. J Thorac Oncol 14:436–444. https://doi.org/10.1016/j.jtho.2018.11.002
Kim HY, Jung K-W, Lim KY et al (2018) Lung cancer screening with low-dose CT in female never smokers: retrospective cohort study with long-term national data follow-up. Cancer Res Treat 50:748–756. https://doi.org/10.4143/crt.2017.312
Bhandari S, Tripathi P, Pham D et al (2019) Performance of community-based lung cancer screening program in a Histoplasma endemic region. Lung Cancer 136:102–104. https://doi.org/10.1016/j.lungcan.2019.08.026
Healey TT, Singer T, Baird GL, Agarwal S (2019) Implementation of lung imaging reporting and data systems in a community private radiology practice: it can be done. J Am Coll Radiol 16:1688–1690. https://doi.org/10.1016/j.jacr.2019.05.046
Kaminetzky M, Milch HS, Shmukler A et al (2019) Effectiveness of Lung-RADS in reducing false-positive results in a diverse, underserved, urban lung cancer screening cohort. J Am Coll Radiol 16:419–426. https://doi.org/10.1016/j.jacr.2018.07.011
Meier-Schroers M, Homsi R, Gieseke J et al (2019) Lung cancer screening with MRI: evaluation of MRI for lung cancer screening by comparison of LDCT- and MRI-derived Lung-RADS categories in the first two screening rounds. Eur Radiol 29:898–905. https://doi.org/10.1007/s00330-018-5607-8
Ouyang B, Guo J, Zhou W et al (2019) Lung cancer screening with low-dose spiral CT in a unit staff: results of the baseline screening. Zhong Nan Da Xue Xue Bao Yi Xue Ban 44:1252–1257. https://doi.org/10.11817/j.issn.1672-7347.2019.190235
da S Teles GB, Macedo ACS, Chate RC et al (2020) LDCT lung cancer screening in populations at different risk for lung cancer. BMJ Open Resp Res 7:e000455. https://doi.org/10.1136/bmjresp-2019-000455
Tremblay A, Taghizadeh N, MacGregor J-H et al (2019) Application of lung-screening reporting and data system versus pan-Canadian early detection of lung cancer nodule risk calculation in the Alberta Lung Cancer Screening Study. J Am Coll Radiol 16:1425–1432. https://doi.org/10.1016/j.jacr.2019.03.006
BarbosaJr EJM, Yang R, Hershman M (2021) Real world lung cancer CT screening performance, smoking behavior, and adherence to recommendations: Lung-RADS category and smoking status predict adherence. AJR Am J Roentgenol 216:919–926. https://doi.org/10.2214/AJR.20.23637
Hsu Y-C, Tsai Y-H, Weng H-H et al (2020) Artificial neural networks improve LDCT lung cancer screening: a comparative validation study. BMC Cancer 20:1023. https://doi.org/10.1186/s12885-020-07465-1
Kessler A, Peng R, Mardakhaev E et al (2020) Performance of the Vancouver risk calculator compared with Lung-RADS in an urban, diverse clinical lung cancer screening cohort. Radiol Imaging Cancer 2:e190021. https://doi.org/10.1148/rycan.2020190021
Kim H, Kim HY, Goo JM, Kim Y (2020) Lung cancer CT screening and Lung-RADS in a tuberculosis-endemic country: the Korean Lung Cancer Screening Project (K-LUCAS). Radiology 296:181–188. https://doi.org/10.1148/radiol.2020192283
Maller B, Simmons VN, Byrne MM, Tanvetyanon T (2021) Characteristics and outcomes of lung cancer screening among individuals with or without cancer history. Clin Lung Cancer 22:e629–e636. https://doi.org/10.1016/j.cllc.2020.12.006
O’Dwyer E, Halpenny DF, Ginsberg MS (2021) Lung cancer screening in patients with previous malignancy: is this cohort at increased risk for malignancy? Eur Radiol 31:458–467. https://doi.org/10.1007/s00330-020-07026-x
White LJ, Kaur A, Lapel RT et al (2020) Lung cancer screening at a military treatment facility: a retrospective review. Mil Med 185:e864–e869. https://doi.org/10.1093/milmed/usz386
Darling GE, Tammemägi MC, Schmidt H et al (2021) Organized lung cancer screening pilot: informing a province-wide program in Ontario, Canada. Ann Thorac Surg 111:1805–1811. https://doi.org/10.1016/j.athoracsur.2020.07.051
Erkmen CP, Dako F, Moore R et al (2021) Adherence to annual lung cancer screening with low-dose CT scan in a diverse population. Cancer Causes Control 32:291–298. https://doi.org/10.1007/s10552-020-01383-0
Parang S, Bhavin J (2021) LDCT Screening in smokers in India—a pilot, proof-of-concept study. Indian J Radiol Imaging 31:318–322. https://doi.org/10.1055/s-0041-1734227
Regis SM, Borondy-Kitts A, McKee AB et al (2022) Outcomes of positive and suspicious findings in clinical computed tomography lung cancer screening and the road ahead. Ann Am Thorac Soc 19:1371–1378. https://doi.org/10.1513/AnnalsATS.202106-733OC
Silva M, Milanese G, Sestini S et al (2021) Lung cancer screening by nodule volume in Lung-RADS v1.1: negative baseline CT yields potential for increased screening interval. Eur Radiol 31:1956–1968. https://doi.org/10.1007/s00330-020-07275-w
Oshiro CES, Frankland TB, Mor J et al (2022) Lung cancer screening by race and ethnicity in an integrated health system in Hawaii. JAMA Netw Open 5:e2144381. https://doi.org/10.1001/jamanetworkopen.2021.44381
Panina A, Kaidarova D, Zholdybay Z et al (2022) Lung cancer screening with low-dose chest computed tomography: experience from radon-contaminated regions in Kazakhstan. J Prev Med Public Health 55:273–279. https://doi.org/10.3961/jpmph.21.600
Lam S (2019) Lung Cancer Screening in Never-Smokers. J Thorac Oncol 14:336–337. https://doi.org/10.1016/j.jtho.2018.12.019
Zhou F, Zhou C (2018) Lung cancer in never smokers-the East Asian experience. Transl Lung Cancer Res 7:450–463. https://doi.org/10.21037/tlcr.2018.05.14
Kerpel-Fronius A, Tammemägi M, Cavic M et al (2022) Screening for lung cancer in individuals who never smoked: an International Association for the Study of Lung Cancer Early Detection and Screening Committee Report. J Thorac Oncol 17:56–66. https://doi.org/10.1016/j.jtho.2021.07.031
Yang X, Wisselink HJ, Vliegenthart R et al (2022) Association between chest CT–defined emphysema and lung cancer: a systematic review and meta-analysis. Radiology 304:322–330. https://doi.org/10.1148/radiol.212904
Leeflang MMG, Rutjes AWS, Reitsma JB et al (2013) Variation of a test’s sensitivity and specificity with disease prevalence. CMAJ 185:E537-544. https://doi.org/10.1503/cmaj.121286
van Stralen KJ, Stel VS, Reitsma JB et al (2009) Diagnostic methods I: sensitivity, specificity, and other measures of accuracy. Kidney Int 75:1257–1263. https://doi.org/10.1038/ki.2009.92
Infante MV, Cardillo G (2020) Lung cancer screening in never-smokers: facts and remaining issues. Eur Respir J 56:2002949. https://doi.org/10.1183/13993003.02949-2020
Funding
This study has received funding by the Royal Netherlands Academy of Arts and Sciences (Grant No. PSA_SA_BD_01). Yifei Mao is funded by the Chinese Scholarship Council (CSC No. 202008440409).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Prof. Geertruida H. de Bock.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
One of the authors has significant statistical expertise.
Informed consent
Written informed consent was not required for this study because this was a systematic review and meta-analysis.
Ethical approval
Institutional review board approval was not required because this was a systematic review and meta-analysis.
Methodology
• Retrospective.
• Diagnostic study.
• Multicenter study.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mao, Y., Cai, J., Heuvelmans, M.A. et al. Performance of Lung-RADS in different target populations: a systematic review and meta-analysis. Eur Radiol 34, 1877–1892 (2024). https://doi.org/10.1007/s00330-023-10049-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-023-10049-9