Abstract
Objective
To investigate the prognostic value of deep learning (DL)–driven CT fibrosis quantification in idiopathic pulmonary fibrosis (IPF).
Methods
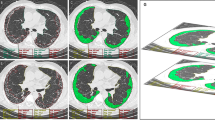
Patients diagnosed with IPF who underwent nonenhanced chest CT and spirometry between 2005 and 2009 were retrospectively collected. Proportions of normal (CT-Norm%) and fibrotic lung volume (CT-Fib%) were calculated on CT using the DL software. The correlations of CT-Norm% and CT-Fib% with forced vital capacity (FVC) and diffusion capacity of carbon monoxide (DLCO) were evaluated. The multivariable-adjusted hazard ratios (HRs) of CT-Norm% and CT-Fib% for overall survival were calculated with clinical and physiologic variables as covariates using Cox regression. The feasibility of substituting CT-Norm% for DLCO in the GAP index was investigated using time-dependent areas under the receiver operating characteristic curve (TD-AUCs) at 3 years.
Results
In total, 161 patients (median age [IQR], 68 [62–73] years; 104 men) were evaluated. CT-Norm% and CT-Fib% showed significant correlations with FVC (Pearson’s r, 0.40 for CT-Norm% and − 0.37 for CT-Fib%; both p < 0.001) and DLCO (0.52 for CT-Norm% and − 0.46 for CT-Fib%; both p < 0.001). On multivariable Cox regression, both CT-Norm% and CT-Fib% were independent prognostic factors when adjusted to age, sex, smoking status, comorbid chronic diseases, FVC, and DLCO (HRs, 0.98 [95% CI 0.97–0.99; p < 0.001] for CT-Norm% at 3 years and 1.03 [1.01–1.05; p = 0.01] for CT-Fib%). Substituting CT-Norm% for DLCO showed comparable discrimination to the original GAP index (TD-AUC, 0.82 [0.78–0.85] vs. 0.82 [0.79–0.86]; p = 0.75).
Conclusion
CT-Norm% and CT-Fib% calculated using chest CT–based deep learning software were independent prognostic factors for overall survival in IPF.
Key Points
• Normal and fibrotic lung volume proportions were automatically calculated using commercial deep learning software from chest CT taken from 161 patients diagnosed with idiopathic pulmonary fibrosis.
• CT-quantified volumetric parameters from commercial deep learning software were correlated with forced vital capacity (Pearson’s r, 0.40 for normal and − 0.37 for fibrotic lung volume proportions) and diffusion capacity of carbon monoxide (Pearson’s r, 0.52 and − 0.46, respectively).
• Normal and fibrotic lung volume proportions (hazard ratios, 0.98 and 1.04; both p < 0.001) independently predicted overall survival when adjusted for clinical and physiologic variables.






Similar content being viewed by others
Abbreviations
- ATS/ERS/JRS/ALAT:
-
American Thoracic Society/European Respiratory Society/Japanese Respiratory Society/Latin American Thoracic Association
- CT-Fib%:
-
Fibrotic lung volume proportion
- CT-Norm%:
-
Normal lung volume proportion
- DLCO :
-
Diffusion capacity of carbon monoxide
- DLCO%:
-
Diffusion capacity of carbon monoxide, expressed as a percentage of the predicted value
- FEV1%:
-
Forced expiratory volume in 1 s, expressed as a percentage of the predicted value
- FVC:
-
Forced vital capacity
- FVC%:
-
Forced vital capacity, expressed as a percentage of the predicted value
- GAP:
-
Gender, age, and physiology
- IPF:
-
Idiopathic pulmonary fibrosis
References
Lederer DJ, Martinez FJ (2018) Idiopathic pulmonary fibrosis. N Engl J Med 378:1811–1823
Raghu G, Chen S-Y, Yeh W-S et al (2014) Idiopathic pulmonary fibrosis in US Medicare beneficiaries aged 65 years and older: incidence, prevalence, and survival, 2001–11. Lancet Respir Med 2:566–572
Richeldi L, Du Bois RM, Raghu G et al (2014) Efficacy and safety of nintedanib in idiopathic pulmonary fibrosis. N Engl J Med 370:2071–2082
King TE Jr, Bradford WZ, Castro-Bernardini S et al (2014) A phase 3 trial of pirfenidone in patients with idiopathic pulmonary fibrosis. N Engl J Med 370:2083–2092
Khor YH, Ng Y, Barnes H, Goh NS, McDonald CF (2020) Holland AE (2020) Prognosis of idiopathic pulmonary fibrosis without anti-fibrotic therapy: a systematic review. Eur Respir Rev 29(157):190158
Raghu G, Collard HR, Egan JJ et al (2011) An official ATS/ERS/JRS/ALAT statement: idiopathic pulmonary fibrosis: evidence-based guidelines for diagnosis and management. Am J Respir Crit Care Med 183:788–824
National Institue for Health and Care Excellence: Idiopathic pulmonary fibrosis in adults: diagnosis and management. Available online: https://www.nice.org.uk/guidance/cg163. Accessed May 4, 2022
Raghu G, Remy-Jardin M, Myers JL et al (2018) Diagnosis of idiopathic pulmonary fibrosis. An official ATS/ERS/JRS/ALAT clinical practice guideline. Am J Respir Crit Care Med 198:e44–e68
Lynch DA, Sverzellati N, Travis WD et al (2018) Diagnostic criteria for idiopathic pulmonary fibrosis: a Fleischner Society White Paper. Lancet Respir Med 6:138–153
Ley B, Elicker BM, Hartman TE et al (2014) Idiopathic pulmonary fibrosis: CT and risk of death. Radiology 273:570–579
Ley B, Ryerson CJ, Vittinghoff E et al (2012) A multidimensional index and staging system for idiopathic pulmonary fibrosis. Ann Intern Med 156:684–691
Kim ES, Choi SM, Lee J et al (2015) Validation of the GAP score in Korean patients with idiopathic pulmonary fibrosis. Chest 147:430–437
Kim H, Jin KN, Yoo S-J et al (2022) Deep learning for estimating lung capacity on chest radiographs predicts survival in idiopathic pulmonary fibrosis. Radiology 306(3):e220292. https://doi.org/10.1148/radiol.220292
Graham BL, Steenbruggen I, Miller MR et al (2019) Standardization of spirometry 2019 update. An official American thoracic society and European respiratory society technical statement. Am J Respir Crit Care Med 200:e70–e88
Kang MJ, Won Y-J, Lee JJ et al (2022) Cancer statistics in Korea: incidence, mortality, survival, and prevalence in 2019. Cancer Res Treat 54:330–344
Kim MS, Choe J, Hwang HJ et al (2022) Interstitial lung abnormalities (ILA) on routine chest CT: comparison of radiologists’ visual evaluation and automated quantification. Eur J Radiol 157:110564
Kim GB, Jung K-H, Lee Y et al (2018) Comparison of shallow and deep learning methods on classifying the regional pattern of diffuse lung disease. J Digit Imaging 31:415–424
Park B, Park H, Lee SM, Seo JB, Kim N (2019) Lung segmentation on HRCT and volumetric CT for diffuse interstitial lung disease using deep convolutional neural networks. J Digit Imaging 32:1019–1026
Blanche P, Dartigues JF, Jacqmin-Gadda H (2013) Estimating and comparing time-dependent areas under receiver operating characteristic curves for censored event times with competing risks. Stat Med 32:5381–5397
Lynch DA, Godwin JD, Safrin S et al (2005) High-resolution computed tomography in idiopathic pulmonary fibrosis: diagnosis and prognosis. Am J Respir Crit Care Med 172:488–493
Best AC, Meng J, Lynch AM et al (2008) Idiopathic pulmonary fibrosis: physiologic tests, quantitative CT indexes, and CT visual scores as predictors of mortality. Radiology 246:935–940
Macintyre N, Crapo R, Viegi G et al (2005) Standardisation of the single-breath determination of carbon monoxide uptake in the lung. Eur Respir J 26:720–735
Desjardin A, Creveuil C, Bergot E, Normand H (2020) Assessment of concordance between diffusion of carbon monoxide through the lung using the 10 s breath-hold method, and the simultaneous NO/CO technique, in healthy participants. Respir Physiol Neurobiol 273:103319
Capaccione KM, Wang A, Lee SM et al (2021) Quantifying normal lung in pulmonary fibrosis: CT analysis and correlation with% DLCO. Clin Imaging 77:287–290
Calandriello L, Walsh SL (2022) The evolution of computer-based analysis of high-resolution CT of the chest in patients with IPF. Br J Radiol 95(1132):20200944
Aziz ZA, Wells AU, Hansell DM et al (2004) HRCT diagnosis of diffuse parenchymal lung disease: inter-observer variation. Thorax 59:506–511
Ash SY, Harmouche R, Vallejo DLL et al (2017) Densitometric and local histogram based analysis of computed tomography images in patients with idiopathic pulmonary fibrosis. Respir Res 18:1–11
Loeh B, Brylski LT, von der Beck D et al (2019) Lung CT densitometry in idiopathic pulmonary fibrosis for the prediction of natural course, severity, and mortality. Chest 155:972–981
Kim HJ, Brown MS, Chong D et al (2015) Comparison of the quantitative CT imaging biomarkers of idiopathic pulmonary fibrosis at baseline and early change with an interval of 7 months. Acad Radiol 22:70–80
Siddique N, Paheding S, Elkin CP, Devabhaktuni V (2021) U-net and its variants for medical image segmentation: a review of theory and applications. IEEE Access 9:82031–82057
Humphries SM, Swigris JJ, Brown KK et al (2018) Quantitative high-resolution computed tomography fibrosis score: performance characteristics in idiopathic pulmonary fibrosis. Eur Resp J 52(3):1801384
Humphries SM, Mackintosh JA, Jo HE et al (2022) Quantitative computed tomography predicts outcomes in idiopathic pulmonary fibrosis. Respirology 27:1045–1053. https://doi.org/10.1111/resp.14333
Handa T, Tanizawa K, Oguma T et al (2022) Novel artificial intelligence-based technology for chest computed tomography analysis of idiopathic pulmonary fibrosis. Ann Am Thorac Soc 19:399–406
Ley B, Collard HR, King TE Jr (2011) Clinical course and prediction of survival in idiopathic pulmonary fibrosis. Am J Respir Crit Care Med 183:431–440
Lamas DJ, Kawut SM, Bagiella E, Philip N, Arcasoy SM, Lederer DJ (2011) Delayed access and survival in idiopathic pulmonary fibrosis: a cohort study. Am J Respir Crit Care Med 184(7):842–847
Funding
This study has received funding by the Research Program 2020 funded by Seoul National University College of Medicine Research Foundation (800-20200313), the Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Science and ICT (NRF-2020R1C1C1003684), and the grant from the Seoul National University Hospital Research Fund (04-2020-2040). However, the funders had no role in the study design; in the collection, analysis, and interpretation of the data; in the writing of the report; and in the decision to submit the article for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Hyungjin Kim.
Conflict of interest
Author Hyungjin Kim is a member of European Radiology Scientific Editorial board. He has not taken part in review or selection process for this manuscript. The remaining authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
Statistical analyses were performed by a statistician with 15 years of experience (Yunhee Choi). She is one of the co-authors.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
Institutional Review Board approval was obtained.
Study subjects or cohorts overlap
The patients in our study have been reported in previous publications on validation of the GAP score and lung volume estimation using chest radiographs.
Kim ES, Choi SM, Lee J, et al Validation of the GAP score in Korean patients with idiopathic pulmonary fibrosis. Chest. 2015;147(2):430–437. https://doi.org/10.1378/chest.14-0453; and in submitted: Deep Learning for Estimating Lung Capacity on Chest Radiographs to Predict Survival in Idiopathic Pulmonary Fibrosis as PDF in file inventory.
Methodology
-
retrospective
-
observational
-
performed at one institution
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nam, J.G., Choi, Y., Lee, SM. et al. Prognostic value of deep learning–based fibrosis quantification on chest CT in idiopathic pulmonary fibrosis. Eur Radiol 33, 3144–3155 (2023). https://doi.org/10.1007/s00330-023-09534-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-023-09534-y