Abstract
Objectives
A drug-coated balloon (DCB) has potential applications in the treatment of intracranial atherosclerotic disease (ICAD). We aimed to evaluate changes of vessel wall features of ICAD lesions after DCB treatment by using vessel wall MRI (VWMRI).
Methods
We retrospectively included patients with symptomatic ICAD who underwent DCB angioplasty alone. The incidences of stenosis of the lumen area, vessel wall thickening, hyperintense plaques, and prominent wall enhancement were compared between the baseline and follow-up VWMRI.
Results
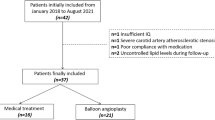
There were 29 ICAD lesions from 29 patients, of which 22 were stenosis and 7 were occlusion. The median interval between DCB treatment and follow-up VWMRI was 4.1 [3.3, 6.7] months. After DCB treatment, follow-up VWMRI showed a significant decrease in the stenosis degree of the lumen area (83% [71%, 96%] vs 15% [3%, 41%], p < 0.001). Thirty-eight percent (11/29) of the patients observed normal appearance of the target vessel wall on follow-up VWMRI. In the stenosis group, the prevalence of hyperintense plaques decreased from 66.7% (14/21) at baseline to 23.8% (5/21) at follow-up, and prominent wall enhancement decreased from 66.7% (14/21) at baseline to 19.0%(4/21) at follow-up. The incidence of hyperintense plaques (p = 0.028) and vessel wall thickening (p = 0.018) tended to decrease with follow-up time. Although not significant (p = 0.106), a similar trend was observed between the incidence of prominent wall enhancement and follow-up time.
Conclusion
Vascular healing with plaque modification and stabilization occurred following DCB treatment of ICAD lesions.
Key Points
• A drug-coated balloon (DCB) has potential applications in the treatment of intracranial atherosclerotic disease (ICAD).
• Vascular healing with plaque modification and stabilization occurred following DCB treatment of ICAD lesions.


Similar content being viewed by others
Abbreviations
- 3D:
-
Three-dimensional
- BA:
-
Basilar artery
- DCB:
-
Drug-coated balloon
- ICA:
-
Intracranial internal carotid artery
- ICAD:
-
Intracranial atherosclerotic disease
- MCA:
-
Middle cerebral arteries
- MRA:
-
MR angiography
- MSI:
-
Mean signal intensity
- TIA:
-
Transient ischemic attack
- TIMI:
-
Thrombolysis in myocardial infarction
- VA:
-
Vertebral arteries
- VWMRI:
-
Vessel wall MRI
References
Fukushima T, Ashikaga T, Yoshikawa S et al (2018) Effect of drug-coated balloon on stent restenosis, neointimal proliferation, and coronary dissection: an optical coherence tomography analysis. Coron Artery Dis 29:39–45
Ang H, Koppara TR, Cassese S, Ng J, Joner M, Foin N (2020) Drug-coated balloons: technical and clinical progress. Vasc Med 25:577–587
Zhang J, Zhang X, Zhang J et al (2020) Drug-coated balloon dilation compared with conventional stenting angioplasty for intracranial atherosclerotic disease. Neurosurgery 87:992–998
Han J, Zhang J, Zhang X et al (2019) Drug-coated balloons for the treatment of symptomatic intracranial atherosclerosis: initial experience and follow-up outcome. J Neurointerv Surg 11:569–573
Mossa-Basha M, Alexander M, Gaddikeri S, Yuan C, Gandhi D (2016) Vessel wall imaging for intracranial vascular disease evaluation. J Neurointerv Surg 8:1154–1159
Her AY, Shin ES, Chung JH et al (2019) Plaque modification and stabilization after paclitaxel-coated balloon treatment for de novo coronary lesions. Heart Vessels 34:1113–1121
Chowdhury MM, Singh K, Albaghdadi MS et al (2020) Paclitaxel drug-coated balloon angioplasty suppresses progression and inflammation of experimental atherosclerosis in rabbits. JACC Basic Transl Sci 5:685–695
Akutsu N, Ogaku A, Koyama Y et al (2019) Effect of drug-coated balloon angioplasty on in-stent restenotic coronary lesions analyzed with optical coherence tomography and serial coronary artery angioscopy. Heart Vessels 34:1925–1935
Bodle JD, Feldmann E, Swartz RH, Rumboldt Z, Brown T, Turan TN (2013) High-resolution magnetic resonance imaging: an emerging tool for evaluating intracranial arterial disease. Stroke 44:287–292
Mandell DM, Mossa-Basha M, Qiao Y et al (2017) Intracranial vessel wall MRI: principles and expert consensus recommendations of the American Society of Neuroradiology. AJNR Am J Neuroradiol 38:218–229
Lou X, Ma N, Ma L, Jiang WJ (2013) Contrast-enhanced 3T high-resolution MR imaging in symptomatic atherosclerotic basilar artery stenosis. AJNR Am J Neuroradiol 34:513–517
Wang Y, Liu M, Pu C (2017) 2014 Chinese guidelines for secondary prevention of ischemic stroke and transient ischemic attack. Int J Stroke 12:302–320
Lou M, Chen Z, Wan J et al (2014) Susceptibility-diffusion mismatch predicts thrombolytic outcomes: a retrospective cohort study. AJNR Am J Neuroradiol 35:2061–2067
Wu F, Ma Q, Song H et al (2018) Differential features of culprit intracranial atherosclerotic lesions: a whole-brain vessel wall imaging study in patients with acute ischemic stroke. J Am Heart Assoc 7
Kwee RM, Qiao Y, Liu L, Zeiler SR, Wasserman BA (2019) Temporal course and implications of intracranial atherosclerotic plaque enhancement on high-resolution vessel wall MRI. Neuroradiology 61:651–657
Meng Y, Li M, Yu Y et al (2019) Quantitative score of the vessel morphology in middle cerebral artery atherosclerosis. J Neurol Sci 399:111–117
Norman G, Streiner D (2014) Biostatistics: the bare essentials, 4rd edn. B.C. Decker, PMPH: Shelton, USA
Wu F, Song H, Ma Q et al (2018) Hyperintense plaque on intracranial vessel wall magnetic resonance imaging as a predictor of artery-to-artery embolic infarction. Stroke 49:905–911
Levy AP, Moreno PR (2006) Intraplaque hemorrhage. Curr Mol Med 6:479–488
Portanova A, Hakakian N, Mikulis DJ, Virmani R, Abdalla WM, Wasserman BA (2013) Intracranial vasa vasorum: insights and implications for imaging. Radiology 267:667–679
Yang WJ, Wong KS, Chen XY (2017) Intracranial atherosclerosis: from microscopy to high-resolution magnetic resonance imaging. J Stroke 19:249–260
Talley JD, Hurst JW, King SB et al (1988) Clinical outcome 5 years after attempted percutaneous transluminal coronary angioplasty in 427 patients. Circulation 77:820–829
Scheller B, Fischer D, Clever YP et al (2013) Treatment of a coronary bifurcation lesion with drug-coated balloons: lumen enlargement and plaque modification after 6 months. Clin Res Cardiol 102:469–472
Poerner TC, Duderstadt C, Goebel B, Kretzschmar D, Figulla HR, Otto S (2017) Fractional flow reserve-guided coronary angioplasty using paclitaxel-coated balloons without stent implantation: feasibility, safety and 6-month results by angiography and optical coherence tomography. Clin Res Cardiol 106:18–27
Skarpathiotakis M, Mandell DM, Swartz RH, Tomlinson G, Mikulis DJ (2013) Intracranial atherosclerotic plaque enhancement in patients with ischemic stroke. Am J Neuroradiol 34:299–304
Sun J, Underhill HR, Hippe DS, Xue Y, Yuan C, Hatsukami TS (2012) Sustained acceleration in carotid atherosclerotic plaque progression with intraplaque hemorrhage: a long-term time course study. JACC Cardiovasc Imaging 5:798–804
Takaya N, Yuan C, Chu B et al (2005) Presence of intraplaque hemorrhage stimulates progression of carotid atherosclerotic plaques. Circulation 111:2768–2775
Chimowitz MI, Lynn MJ, Derdeyn CP et al (2011) Stenting versus aggressive medical therapy for intracranial arterial stenosis. N Engl J Med 365:993–1003
Feng X, Chan KL, Lan L et al (2019) Stroke mechanisms in symptomatic intracranial atherosclerotic disease: classification and clinical implications. Stroke 50:2692–2699
Arenillas JF, Molina CA, Montaner J, Sn A, González-Sánchez MA, Álvarez-Sabín J (2001) Progression and clinical recurrence of symptomatic middle cerebral artery stenosis. Stroke 32:2898–2904
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Prof. Dr. Ju Han.
Conflict of interest
The authors have no conflicts of interest to declare.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was not required due to the retrospective and observational nature of this study.
Ethical approval
Institutional Review Board approval was obtained with an ID of 2021S1060.
Methodology
• retrospective
• observational
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Meng, Y., Zhang, Y., Chu, X. et al. Plaque modification and stabilization after drug-coated balloon angioplasty for intracranial atherosclerotic lesions. Eur Radiol 33, 1112–1120 (2023). https://doi.org/10.1007/s00330-022-09129-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-022-09129-z