Abstract
Objectives
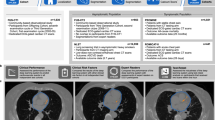
The size of the heart may predict major cardiovascular events (MACE) in patients with stable chest pain. We aimed to evaluate the prognostic value of 3D whole heart volume (WHV) derived from non-contrast cardiac computed tomography (CT).
Methods
Among participants randomized to the CT arm of the Prospective Multicenter Imaging Study for Evaluation of Chest Pain (PROMISE), we used deep learning to extract WHV, defined as the volume of the pericardial sac. We compared the WHV across categories of cardiovascular risk factors and coronary artery disease (CAD) characteristics and determined the association of WHV with MACE (all-cause death, myocardial infarction, unstable angina; median follow-up: 26 months).
Results
In the 3798 included patients (60.5 ± 8.2 years; 51.5% women), the WHV was 351.9 ± 57.6 cm3/m2. We found smaller WHV in no- or non-obstructive CAD, women, people with diabetes, sedentary lifestyle, and metabolic syndrome. Larger WHV was found in obstructive CAD, men, and increased atherosclerosis cardiovascular disease (ASCVD) risk score (p < 0.05). In a time-to-event analysis, small WHV was associated with over 4.4-fold risk of MACE (HR (per one standard deviation) = 0.221; 95% CI: 0.068–0.721; p = 0.012) independent of ASCVD risk score and CT-derived CAD characteristics. In patients with non-obstructive CAD, but not in those with no- or obstructive CAD, WHV increased the discriminatory capacity of ASCVD and CT-derived CAD characteristics significantly.
Conclusions
Small WHV may represent a novel imaging marker of MACE in stable chest pain. In particular, WHV may improve risk stratification in patients with non-obstructive CAD, a cohort with an unmet need for better risk stratification.
Key Points
• Heart volume is easily assessable from non-contrast cardiac computed tomography.
• Small heart volume may be an imaging marker of major adverse cardiac events independent and incremental to traditional cardiovascular risk factors and established CT measures of CAD.
• Heart volume may improve cardiovascular risk stratification in patients with non-obstructive CAD.






Similar content being viewed by others
Abbreviations
- ASCVD:
-
Atherosclerosis cardiovascular disease
- AUC:
-
Area under the curve
- BSA:
-
Body surface area
- CAC:
-
Coronary artery calcium
- CAD:
-
Coronary artery disease
- CI:
-
Confidence interval
- CT:
-
Computed tomography
- CTA:
-
Computed tomography angiography
- CV:
-
Cardiovascular
- DL:
-
Deep learning
- HR:
-
Hazard ratio
- HRPF:
-
High-risk plaque features
- IQR:
-
Interquartile range
- MACE:
-
Major adverse cardiac events
- MI:
-
Myocardial infarction
- ROC:
-
Receiver operator characteristic
- SD:
-
Standard deviation
- UA:
-
Unstable angina
- WHV:
-
Whole heart volume
References
Knuuti J, Wijns W, Saraste A et al (2019) ESC Guidelines for the diagnosis and management of chronic coronary syndromes The Task Force for the diagnosis and management of chronic coronary syndromes of the European Society of Cardiology (ESC). Eur Heart J. https://doi.org/10.1093/eurheartj/ehz425
Emami H, Takx RAP, Mayrhofer T et al (2017) Non-obstructive CAD by coronary CTA improves risk stratification and allocation of statin therapy. JACC Cardiovasc Imaging 10:1031–1038. https://doi.org/10.1016/j.jcmg.2016.10.022
Hoffmann U, Ferencik M, Udelson JE et al (2017) Prognostic value of noninvasive cardiovascular testing in patients with stable chest pain: insights from the PROMISE trial. Circulation. https://doi.org/10.1161/CIRCULATIONAHA.116.024360
Lin FY, Shaw LJ, Dunning AM et al (2011) Mortality risk in symptomatic patients with nonobstructive coronary artery disease: a prospective 2-center study of 2,583 patients undergoing 64-detector row coronary computed tomographic angiography. J Am Coll Cardiol 58:510–519. https://doi.org/10.1016/j.jacc.2010.11.078
Ferencik M, Mayrhofer T, Bittner DO et al (2018) Use of high-risk coronary atherosclerotic plaque detection for risk stratification of patients with stable chest pain: a secondary analysis of the PROMISE randomized clinical trial. JAMA Cardiol. https://doi.org/10.1001/jamacardio.2017.4973
Budoff MJ, Thomas M, Maros F et al (2017) Prognostic value of coronary artery calcium in the PROMISE study (Prospective Multicenter Imaging Study for Evaluation of Chest Pain). Circulation 136:1993–2005. https://doi.org/10.1161/CIRCULATIONAHA.117.030578
Lu MT, Park J, Ghemigian K et al (2016) Epicardial and paracardial adipose tissue volume and attenuation – association with high-risk coronary plaque on computed tomographic angiography in the ROMICAT II trial. Atherosclerosis 251:47–54. https://doi.org/10.1016/j.atherosclerosis.2016.05.033
Goeller M, Achenbach S, Marwan M et al (2018) Epicardial adipose tissue density and volume are related to subclinical atherosclerosis, inflammation and major adverse cardiac events in asymptomatic subjects. J Cardiovasc Comput Tomogr 12:67–73. https://doi.org/10.1016/j.jcct.2017.11.007
Kizer JR, Bella JN, Palmieri V et al (2006) Left atrial diameter as an independent predictor of first clinical cardiovascular events in middle-aged and elderly adults: the Strong Heart Study (SHS). Am Heart J 151:412–418
Bittencourt MS, Blankstein R, Mao S et al (2016) Left ventricular area on non-contrast cardiac computed tomography as a predictor of incident heart failure – The Multi-Ethnic Study of Atherosclerosis. J Cardiovasc Comput Tomogr 10:500–506. https://doi.org/10.1016/j.jcct.2016.07.009
Dimopoulos K, Giannakoulas G, Bendayan I et al (2013) Cardiothoracic ratio from postero-anterior chest radiographs: a simple, reproducible and independent marker of disease severity and outcome in adults with congenital heart disease. Int J Cardiol 166:453–457. https://doi.org/10.1016/j.ijcard.2011.10.125
Giamouzis G, Sui X, Love TE, Butler J, Young JB, Ahmed A (2008) A propensity-matched study of the association of cardiothoracic ratio with morbidity and mortality in chronic heart failure††The Digitalis Investigation Group (DIG) study was conducted and supported by the NHLBI in collaboration with the DIG investigators. This report was prepared using a limited-access data set obtained by the NHLBI and does not necessarily reflect the opinions or views of the DIG study or the NHLBI. Am J Cardiol 101:343–347. https://doi.org/10.1016/j.amjcard.2007.08.039
Hemingway H, Shipley M, Christie D, Marmot M (1998) Cardiothoracic ratio and relative heart volume as predictors of coronary heart disease mortality The Whitehall study 25 year follow-up. Eur Heart J 19:859–869. https://doi.org/10.1053/euhj.1997.0862
Zaman MJS, Sanders J, Crook AM et al (2007) Cardiothoracic ratio within the “normal” range independently predicts mortality in patients undergoing coronary angiography. Heart 93:491–494. https://doi.org/10.1136/hrt.2006.101238
Douglas PS, Hoffmann U, Lee KL et al (2014) PROspective multicenter imaging study for evaluation of chest pain: rationale and design of the PROMISE trial. Am Heart J 167:796–803.e1. https://doi.org/10.1016/j.ahj.2014.03.003
Mosteller RD (1987) Simplified calculation of body-surface area. N Engl J Med 317:1098. https://doi.org/10.1056/NEJM198710223171717
Welcome to Python.org. In: Python.org. https://www.python.org/. Accessed 2 Dec 2020
TensorFlow. In: TensorFlow. https://www.tensorflow.org/. Accessed 2 Dec 2020
Keras: the Python deep learning API. https://keras.io/. Accessed 2 Dec 2020
(2017) CUDA Zone. In: NVIDIA Dev. https://developer.nvidia.com/cuda-zone. Accessed 2 Dec 2020
3D Slicer. https://www.slicer.org/. Accessed 2 Dec 2020
Agatston AS, Janowitz WR, Hildner FJ, Zusmer NR, Viamonte M Jr, Detrano R (1990) Quantification of coronary artery calcium using ultrafast computed tomography. J Am Coll Cardiol 15:827–832
de Araújo Gonçalves P, Garcia-Garcia HM, Dores H et al (2013) Coronary computed tomography angiography-adapted Leaman score as a tool to noninvasively quantify total coronary atherosclerotic burden. Int J Cardiovasc Imaging 29:1575–1584. https://doi.org/10.1007/s10554-013-0232-8
Paulus WJ, Tschöpe C (2013) A novel paradigm for heart failure with preserved ejection fraction: comorbidities drive myocardial dysfunction and remodeling through coronary microvascular endothelial inflammation. J Am Coll Cardiol 62:263–271. https://doi.org/10.1016/j.jacc.2013.02.092
ter Maaten JM, Damman K, Verhaar MC et al (2016) Connecting heart failure with preserved ejection fraction and renal dysfunction: the role of endothelial dysfunction and inflammation. Eur J Heart Fail 18:588–598. https://doi.org/10.1002/ejhf.497
Kalogeropoulos A, Georgiopoulou V, Psaty BM et al (2010) Inflammatory markers and incident heart failure risk in older adults: the health ABC (Health, Aging, and Body Composition) Study. J Am Coll Cardiol 55:2129–2137. https://doi.org/10.1016/j.jacc.2009.12.045
Velagaleti RS, Gona P, Pencina MJ et al (2014) Left ventricular hypertrophy patterns and incidence of heart failure with preserved versus reduced ejection fraction. Am J Cardiol 113:117–122. https://doi.org/10.1016/j.amjcard.2013.09.028
Shah RV, Abbasi SA, Heydari B et al (2013) Insulin resistance, subclinical left ventricular remodeling, and the obesity paradox: MESA (Multi-Ethnic Study of Atherosclerosis). J Am Coll Cardiol 61:1698–1706. https://doi.org/10.1016/j.jacc.2013.01.053
Pierdomenico SD, Lapenna D, Bucci A, Manente BM, Cuccurullo F, Mezzetti A (2004) Prognostic value of left ventricular concentric remodeling in uncomplicated mild hypertension. Am J Hypertens 17:1035–1039. https://doi.org/10.1016/j.amjhyper.2004.06.016
Fuchs A, Mejdahl MR, Kühl JT et al (2016) Normal values of left ventricular mass and cardiac chamber volumes assessed by 320-detector computed tomography angiography in the Copenhagen General Population Study. Eur Heart J Cardiovasc Imaging 17:1009–1017. https://doi.org/10.1093/ehjci/jev337
Shah SJ, Lam CSP, Svedlund S et al (2018) Prevalence and correlates of coronary microvascular dysfunction in heart failure with preserved ejection fraction: PROMIS-HFpEF. Eur Heart J 39:3439–3450. https://doi.org/10.1093/eurheartj/ehy531
Camici PG, Crea F (2007) Coronary microvascular dysfunction. N Engl J Med 356:830–840. https://doi.org/10.1056/NEJMra061889
Tona F, Serra R, Di Ascenzo L et al (2014) Systemic inflammation is related to coronary microvascular dysfunction in obese patients without obstructive coronary disease. Nutr Metab Cardiovasc Dis 24:447–453. https://doi.org/10.1016/j.numecd.2013.09.021
Crea F, Bairey Merz CN, Beltrame JF et al (2017) The parallel tales of microvascular angina and heart failure with preserved ejection fraction: a paradigm shift. Eur Heart J 38:473–477. https://doi.org/10.1093/eurheartj/ehw461
Lee JF, Barrett-O’Keefe Z, Garten RS et al (2016) Evidence of microvascular dysfunction in heart failure with preserved ejection fraction. Heart 102:278–284. https://doi.org/10.1136/heartjnl-2015-308403
Lavie CJ, McAuley PA, Church TS, Milani RV, Blair SN (2014) Obesity and cardiovascular diseases: implications regarding fitness, fatness, and severity in the obesity paradox. J Am Coll Cardiol 63:1345–1354. https://doi.org/10.1016/j.jacc.2014.01.022
Moller JE, Hillis GS, Oh JK et al (2003) Left atrial volume: a powerful predictor of survival after acute myocardial infarction. Circulation 107:2207–2212
Vasan RS, Larson MG, Benjamin EJ, Evans JC, Levy D (1997) Left ventricular dilatation and the risk of congestive heart failure in people without myocardial infarction. N Engl J Med 336:1350–1355. https://doi.org/10.1056/NEJM199705083361903
Lauer MS, Evans JC, Levy D (1992) Prognostic implications of subclinical left ventricular dilatation and systolic dysfunction in men free of overt cardiovascular disease (the framingham heart study). Am J Cardiol 70:1180–1184. https://doi.org/10.1016/0002-9149(92)90052-Z
Raymond RJ, Hinderliter AL, Willis PW et al (2002) Echocardiographic predictors of adverse outcomes in primary pulmonary hypertension. J Am Coll Cardiol 39:1214–1219. https://doi.org/10.1016/S0735-1097(02)01744-8
Sun JP, James KB, Sheng Yang X et al (1997) Comparison of mortality rates and progression of left ventricular dysfunction in patients with idiopathic dilated cardiomyopathy and dilated versus nondilated right ventricular cavities. Am J Cardiol 80:1583–1587. https://doi.org/10.1016/S0002-9149(97)00780-7
Acknowledgements
Dr. Hoffmann received Research Grants from the National Institutes of Health (U01HL092040, U01HL092022), and Siemens Medical Solutions, Heart Flow Inc., and served as a consultant for Heart Flow. Dr. Lu reports consulting fees with PQBypass and a research grant from the Nvidia Corporation Academic Program. Dr. Lu is supported by grants from the American Heart Association Precision Medicine Institute 18UNPG34030172 and the Harvard University Center For AIDS Research NIH/NIAID 5P30AI060354-14. Dr. Ferencik reports receiving a grant from the American Heart Association 13FTF16450001. The other authors have nothing to disclose.
Funding
The PROMISE trial was supported by grants from the National Heart, Lung, and Blood Institute (R01HL098237, R01HL098236, R01HL098305, and R01HL098235).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Dr. Borek Foldyna.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
One of the authors (Prof. Thomas Mayrhofer) has significant statistical expertise and no complex statistical methods were necessary for this paper.
Informed consent
Local and central institutional review boards approved the study, and all patients provided written informed consent.
Ethical approval
Local and central institutional review boards approved the study.
Study subjects or cohorts overlap
This investigation is a sub-study of the Prospective Multicenter Imaging Study for Evaluation of Chest Pain (PROMISE) trial.
Methodology
• Secondary analysis
• Multicenter randomized controlled trial
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(DOCX 1058 kb)
Rights and permissions
About this article
Cite this article
Foldyna, B., Zeleznik, R., Eslami, P. et al. Small whole heart volume predicts cardiovascular events in patients with stable chest pain: insights from the PROMISE trial. Eur Radiol 31, 6200–6210 (2021). https://doi.org/10.1007/s00330-021-07695-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-021-07695-2