Abstract
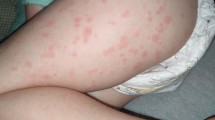
Juvenile idiopathic arthritis (JIA) is a heterogeneous group of arthritis of autoimmune aetiology. Systemic-onset juvenile idiopathic arthritis (soJIA) presents with fever, transient erythematous rash, hepatomegaly, splenomegaly, lymphadenopathy, and serositis. SoJIA presents multiple complications, and the most severe is the macrophage activation syndrome (MAS); the timely treatment of MAS must be established early and aggressively to avoid a fatal outcome. Therapeutic plasma exchange has anecdotally been used in refractory cases. A 66-month-old male with a 1-year illness characterized by evening-predominant, intermittent fever, adenomegalies, urticarial-like rash, arthralgia, and arthritis. Biochemical analysis revealed anaemia, leukocytosis, neutrophilia, hypertriglyceridemia, hyperferritinemia, and hypofibrinogenemia; bone marrow aspirate showed hemophagocytosis. He was diagnosed with SoJIA complicated with MAS. He received multiple treatments with IV human gammaglobulin, cyclosporine, dexamethasone, and tocilizumab without improvement. Plasma replacement treatment was performed. Afterwards, he presented significant improvement. After 3-year-follow-up, he remains in good general condition. We present a refractory case of soJIA complicated with MAS successfully treated with plasma exchange.


Similar content being viewed by others
References
Petty RE, Southwood TR, Manners P, Baum J, Glass DN, Goldenberg J, He X, Maldonado-Cocco J, Orozco-Alcala J, Prieur AM, Suarez-Almazor ME, Woo P (2004) International League of Associations for Rheumatology. International League of Associations for Rheumatology classification of juvenile idiopathic arthritis: second revision, Edmonton, 2001. J Rheumatol 31(2):390–392
Davì S, Consolaro A, Guseinova D, Pistorio A, Ruperto N, Martini A, Cron RQ, Ravelli A, MAS Study Group (2011) An international consensus survey of diagnostic criteria for macrophage activation syndrome in systemic juvenile idiopathic arthritis. J Rheumatol 38(4):764–768
Ravelli A, Grom AA, Behrens EM, Cron RQ (2012) Macrophage activation syndrome as part of systemic juvenile idiopathic arthritis: diagnosis, genetics, pathophysiology and treatment. Genes Immun 13(4):289–298
Minoia F, Davì S, Horne A, Demirkaya E, Bovis F, Li C, Lehmberg K, Weitzman S, Insalaco A, Wouters C, Shenoi S, Espada G, Ozen S, Anton J, Khubchandani R, Russo R, Pal P, Kasapcopur O, Miettunen P, Maritsi D, Merino R, Shakoory B, Alessio M, Chasnyk V, Sanner H, Gao YJ, Huasong Z, Kitoh T, Avcin T, Fischbach M, Frosch M, Grom A, Huber A, Jelusic M, Sawhney S, Uziel Y, Ruperto N, Martini A, Cron RQ, Raveli A, Pediatric Rheumatology International Trials Organization; Childhood Arthritis and Rheumatology Research Alliance; Pediatric Rheumatology Collaborative Study Group; Histiocyte Society (2014) Clinical features, treatment, and outcome of macrophage activation syndrome complicating systemic juvenile idiopathic arthritis: a multinational, multicenter study of 362 patients. Arthritis Rheumatol 66(11):3160–3169
Kimura Y, Weiss JE, Haroldson KL, Lee T, Punaro M, Oliveira S, Rabinovich E, Riebschleger M, Antón J, Blier PR, Gerloni V, Hazen MM, Kessler E, Onel K, Passo MH, Rennebohm RM, Wallace CA, Woo P, Wulffraat N, Childhood Arthritis Rheumatology Research Alliance Carra Net Investigators (2013) Pulmonary hypertension and other potentially fatal pulmonary complications in systemic juvenile idiopathic arthritis. Arthritis Care Res (Hoboken). 65(5):745–752
Rajasekaran S, Kruse K, Kovey K, Davis AT, Hassan NE, Ndika AN, Zuiderveen S, Birmingham J (2014) Therapeutic role of anakinra, an interleukin-1 receptor antagonist, in the management of secondary hemophagocytic lymphohistiocytosis/sepsis/multiple organ dysfunction/macrophage activating syndrome in critically ill children*. Pediatr Crit Care Med 15(5):401–408
Guzman J, Kerr T, Ward LM, Ma J, Oen K, Rosenberg AM, Feldman BM, Boire G, Houghton K, Dancey P, Scuccimarri R, Bruns A, Huber AM, Watanabe Duffy K, Shiff NJ, Berard RA, Levy DM, Stringer E, Morishita K, Johnson N, Cabral DA, Larché M, Petty RE, Laxer RM, Silverman E, Miettunen P, Chetaille AL, Haddad E, Spiegel L, Turvey SE, Schmeling H, Lang B, Ellsworth J, Ramsey SE, Roth J, Campillo S, Benseler S, Chédeville G, Schneider R, Tse SML, Bolaria R, Gross K, Feldman D, Cameron B, Jurencak R, Dorval J, LeBlanc C, St Cyr C, Gibbon M, Yeung RSM, Duffy CM, Tucker LB (2017) Growth and weight gain in children with juvenile idiopathic arthritis: results from the ReACCh-Out cohort. Pediatr Rheumatol Online J 15(1):68
Kaufman KM, Linghu B, Szustakowski JD, Husami A, Yang F, Zhang K, Filipovich AH, Fall N, Harley JB, Nirmala NR, Grom AA (2014) Whole-exome sequencing reveals overlap between macrophage activation syndrome in systemic juvenile idiopathic arthritis and familial hemophagocytic lymphohistiocytosis. Arthritis Rheumatol 66(12):3486–3495
Ravelli A, Minoia F, Davì S, Horne A, Bovis F, Pistorio A, Aricò M, Avcin T, Behrens EM, De Benedetti F, Filipovic L, Grom AA, Henter JI, Ilowite NT, Jordan MB, Khubchandani R, Kitoh T, Lehmberg K, Lovell DJ, Miettunen P, Nichols KE, Ozen S, Pachlopnik Schmid J, Ramanan AV, Russo R, Schneider R, Sterba G, Uziel Y, Wallace C, Wouters C, Wulffraat N, Demirkaya E, Brunner HI, Martini A, Ruperto N, Cron RQ, Paediatric Rheumatology International Trials Organisation; Childhood Arthritis and Rheumatology Research Alliance; Pediatric Rheumatology Collaborative Study Group; Histiocyte Society (2016) 2016 Classification Criteria for Macrophage Activation Syndrome Complicating Systemic Juvenile Idiopathic Arthritis: A European League Against Rheumatism/American College of Rheumatology/Paediatric Rheumatology International Trials Organisation Collaborative Initiative. Arthritis Rheumatol 68(3):566–576
Moradinejad MH, Ziaee V (2011) The incidence of macrophage activation syndrome in children with rheumatic disorders. Minerva Pediatr 63(6):459–466
Kinjo N, Hamada K, Hirayama C, Shimizu M (2018) Role of plasma exchange, leukocytapheresis, and plasma diafiltration in management of refractory macrophage activation syndrome. J Clin Apher 33(1):117–120
Shi L, Hu F, Xu C, Zhu H, Qie D, Yuan C, Tao Y, Liu H (2018) Plasma exchange successfully treated macrophage activation syndrome in rheumatoid factor-positive polyarticular juvenile idiopathic arthritis with co-existing pneumonia. Int J Rheum Dis 21(5):1142–1145
Miyazono A, Abe J, Ogura M, Sato M, Fujimaru T, Kamei K, Ito S (2014) Successful remission induced by plasma exchange combined with leukocytapheresis against refractory systemic juvenile idiopathic arthritis. Eur J Pediatr 173(12):1557–1560
Çakan M, Aktay-Ayaz N, Gemici H, Annayev A, Çıtak A, Akçay A, Öztürk G (2018) Sustained hyperferritinemia in a child with macrophage activation syndrome secondary to systemic juvenile idiopathic arthritis - perforinopathy: case based review. Turk J Pediatr 60(5):598–603
Nakakura H, Ashida A, Matsumura H, Murata T, Nagatoya K, Shibahara N, Inoue T, Tamai H (2009) A case report of successful treatment with plasma exchange for hemophagocytic syndrome associated with severe systemic juvenile idiopathic arthritis in an infant girl. Ther Apher Dial 13(1):71–76
Sato S, Hosokawa T, Kawashima H (2022) Successful treatment of plasma exchange for refractory systemic juvenile idiopathic arthritis complicated with macrophage activation syndrome and severe lung disease. Ann Rheum Dis 81(4):e61
Shi L, Yuan C, Tao Y (2015) A case report of plasmapheresis successfully treated macrophage activation syndrome in juvenile idiopathic arthritis. Zhonghua Er Ke Za Zhi 53(12):954–955
Yokota S, Itoh Y, Morio T, Sumitomo N, Daimaru K, Minota S (2015) Macrophage activation syndrome in patients with systemic juvenile idiopathic arthritis under treatment with Tocilizumab. J Rheumatol 42(4):712–722
Verweyen EL, Schulert GS (2022) Interfering with interferons: targeting the JAK-STAT pathway in complications of systemic juvenile idiopathic arthritis (SJIA). Rheumatology (Oxford) 61(3):926–935
Horne A, von Bahr GT, Chiang SCC, Meeths M, Björklund C, Ekelund M, Erensjö P, Berg S, Hagelberg S, Bryceson YT, Andersson U, Henter JI (2021) Efficacy of moderately dosed etoposide in macrophage activation syndrome-hemophagocytic lymphohistiocytosis. J Rheumatol 48(10):1596–1602
Funding
The work presented in this case report did not receive any funding. No funding was received for this work.
Author information
Authors and Affiliations
Contributions
All authors made substantial contributions to the conception, design of the work, analysis, and interpretation of data for the work; drafted and revised the work critically for important intellectual content; approved the final version to be published; and agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethics approval and consent to participate
All procedures were performed with the prior informed consent of the legal guardian.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liquidano-Perez, E., Maza-Ramos, G., Salazar-Bailón, J.L. et al. Therapeutic plasma exchange in refractory macrophage activation syndrome complicating systemic juvenile idiopathic arthritis: a case-based review. Rheumatol Int 43, 183–189 (2023). https://doi.org/10.1007/s00296-022-05231-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-022-05231-z