Abstract
Purpose
To evaluate the outcomes of intraperitoneal chemotherapy (IP) compared with those of intravenous chemotherapy (IV) in patients with advanced ovarian cancer after neoadjuvant chemotherapy (NACT) and interval debulking surgery (IDS) or primary debulking surgery (PDS).
Methods
Patients with advanced epithelial ovarian carcinoma treated with PDS or NACT and IDS from 2006 to 2015 were identified. Comparative statistics were used to evaluate covariates, and survival rates were calculated using the Kaplan–Meier method and compared with log-rank tests.
Results
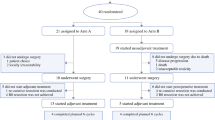
Sixty-six patients received NACT followed by IDS with residual disease of ≤ 1 cm; 42 of these patients (63.6%) received IP therapy; and 24 patients (36.3%) had IV therapy only after IDS. The median progression-free survival (PFS) was 16.0 months in the IP group and 13.5 months in the IV group (p = 0.13). The estimated median overall survival (OS) was 64.0 months with IP and 50.0 months with IV (p = 0.44). During the same study period, 149 patients underwent optimal PDS after which 93 patients (62.4%) received IP and 56 patients (37.6%) were given IV chemotherapy. Patients after IP demonstrated improved survival outcomes when compared to patients after IV therapy. The median PFS was 28.0 months after IP and 16.5 months after IV (p = 0.0006), and the median OS was not reached for IP and 50.0 months after IV (p < 0.0001).
Conclusions
Although IP chemotherapy after PDS is associated with improved survival, IP therapy after NACT and IDS, despite high rates of completion, may not have the same degree of survival advantage over IV therapy.


Similar content being viewed by others
References
Hoskins WJ, McGuire WP, Brady MF et al (1994) The effect of diameter of largest residual disease on survival after primary cytoreductive surgery in patients with suboptimal residual epithelial ovarian carcinoma. Am J Obstet Gynecol 170(4):974–980
Winter WE III, Maxwell GL, Tian C et al (2007) Prognostic factors for stage III epithelial ovarian cancer: a Gynecologic Oncology Group Study. J Clin Oncol 25(24):3621–3627
Vergote I, Trope CG, Amant F et al (2010) Neoadjuvant chemotherapy or primary surgery in stage IIIC or IV ovarian cancer. N Engl J Med 363(10):943–953
Kehoe S, Hook J, Nankivell M et al (2015) Primary chemotherapy versus primary surgery for newly diagnosed advanced ovarian cancer (CHORUS): an open-label, randomized, controlled, non-inferiority trial. Lancet 386:249–257
Hinchcliff EM, Melamed M, Clemmer JT et al (2016) Trends in the use of neoadjuvant chemotherapy for advanced-stage ovarian cancer: a National Cancer Data Base study. Gynecol Oncol 141(Suppl 1):28
Alberts DS, Liu PY, Hannigan EV et al (1996) Intraperitoneal cisplatin plus intravenous cyclophosphamide versus intravenous cisplatin plus intravenous cyclophosphamide for stage III ovarian cancer. N Engl J Med 335(26):1950–1955
Markman M, Bundy BN, Alberts DS et al (2001) Phase III trial of standard-dose intravenous cisplatin plus paclitaxel versus moderately high-dose carboplatin followed by intravenous paclitaxel and intraperitoneal cisplatin in small-volume stage III ovarian carcinoma: an intergroup study of the Gynecologic Oncology Group, Southwestern Oncology Group, and Eastern Cooperative Oncology Group. J Clin Oncol 19(4):1001–1007
Armstrong DK, Bundy B, Wenzel L et al (2006) Intraperitoneal cisplatin and paclitaxel in ovarian cancer. N Engl J Med 354(1):34–43
National Cancer Institute NCI issues clinical announcement for preferred method of treatment for advanced ovarian cancer (2006). http://ctep.cancer.gov/highlights/docs/clin_annc_010506.pdf. Accessed 2017
Walker J, Brady MF, DiSilvestro PA et al (2016) A phase III trial of bevacizumab with IV versus IP chemotherapy for ovarian, fallopian tube, and peritoneal carcinoma: an NRG Oncology Study. Gynecol Oncol 141(Suppl 1):208
Wright A, Cronin A, Milne DE et al (2015) Use and effectiveness of intraperitoneal chemotherapy for treatment of ovarian cancer. J Clin Oncol 33(26):2841–2847
Le T, Latifah H, Jolicoeur L et al (2011) Does intraperitoneal chemotherapy benefit optimally debulked epithelial ovarian cancer patients after neoadjuvant chemotherapy? Gynecol Oncol 121(3):451–454
Al Mutairi NJ, Le T (2014) Does modality of adjuvant chemotherapy after interval surgical debulking matter in epithelial ovarian cancer? Int J Gynecol Cancer 24(3):461–467
Mueller JJ, Kelly A, Zhou Q et al (2016) Intraperitoneal chemotherapy after interval debulking surgery for advanced-stage ovarian cancer: feasibility and outcomes at a comprehensive cancer center. Gynecol Oncol 143(3):496–503
Mackay HJ, Gallagher CJ, Parulekar WR et al (2016) OV21/PETROC: a randomized gynecologic cancer intergroup (GCIG) phase II study of intraperitoneal (IP) versus intravenous (IV) chemotherapy following neoadjuvant chemotherapy and optimal debulking surgery in epithelial ovarian cancer (EOC). In: Oral presentation presented at 2016 ASCO annual meeting, Chicago, IL
Matsuo K, Eno ML, Im DD et al (2010) Chemotherapy time interval and development of platinum and taxane resistance in ovarian, fallopian, and peritoneal carcinoma. Arch Gynecol Obstet 281(2):325–328
Tewari D, Java JJ, Salani R et al (2015) Long-term survival advantage and prognostic factors associated with intraperitoneal chemotherapy treatment in advanced ovarian cancer: a Gynecologic Oncology Group study. J Clin Oncol 33(13):1460–1466
Suidan RS, Zhou Q, Iasonos A et al (2015) Prognostic significance of the number of postoperative intraperitoneal chemotherapy cycles for patients with advanced epithelial ovarian cancer. Int J Gynecol Cancer 25(4):599–606
Katsumata N, Yasuda M, Takahashi F et al (2009) Dose-dense paclitaxel once a week in combination with carboplatin every 3 weeks for advanced ovarian cancer: a phase 3, open-label, randomised controlled trial. Lancet 374(9698):1331–1338
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to disclose.
Ethical approval
This study was approved by the ethics committee of each participating hospital and was performed in accordance with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was not required for this study.
Rights and permissions
About this article
Cite this article
Lee, J., Curtin, J.P., Muggia, F.M. et al. Timing is everything: intraperitoneal chemotherapy after primary or interval debulking surgery for advanced ovarian cancer. Cancer Chemother Pharmacol 82, 55–63 (2018). https://doi.org/10.1007/s00280-018-3591-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-018-3591-y