Abstract
Purpose
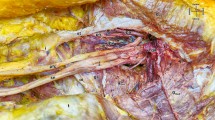
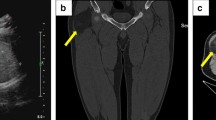
In this article, we report a case of an atypical inferior gluteal artery that passed through the piriformis muscle when it emerged from the pelvic cavity in an elderly Japanese female cadaver. We speculate that this atypical artery could be entrapped and compressed by the piriformis muscle and may therefore be associated with piriformis syndrome; however, the anatomical characteristics of such an atypical artery have not been previously reported. To assess this potential association, the atypical inferior gluteal artery was anatomically examined.
Methods
The cadaver examined in this report was a 97-year-old Japanese female who was donated to The Nippon Dental University for use in medical education and research. The atypical inferior gluteal artery and surrounding structures in half of the pelvis were examined macroscopically.
Results
The atypical inferior gluteal artery arose from the common arterial trunk, formed by itself and the superior gluteal artery, passed through the superior proximal part of the piriformis muscle, and left the pelvic cavity. It supplies branches to the lower half of the gluteus maximus and proximal part of the long head of the biceps femoris muscle. The piriformis muscle originates from the 2nd to 4th sacral vertebrae and attaches to the greater trochanter via a single short tendon.
Conclusion
According to our findings, when the atypical inferior gluteal artery is entrapped and compressed, ischemic signs and symptoms may emerge in the lower buttocks and proximal posterior thigh. These results provide a new perspective for the diagnosis and treatment of piriformis syndrome.


Similar content being viewed by others
Data availability
On reasonable requests, obtained data supporting the finding of the present study are available from the corresponding author.
References
Adachi B (1928) Das Arteriensystem Der Japaner, vol 2. Die Kaiserlich Japanische Universität zu Kyoto, Maruzen, Kyoto
Akita K, Sakamoto H, Sato T (1994) Arrangement and innervation of the glutei medius and minimus and the piriformis: a morphological analysis. Anat Rec 238:125–130. https://doi.org/10.1002/ar.1092380114
Arifoglu Y, Surucu HS, Sargon MF, Tanyeli E, Yazar F (1997) Double superior gemellus together with double piriformis and high division of the sciatic nerve. Surg Radiol Anat 19:407–408. https://doi.org/10.1007/BF01628510
Asmall T, Gunston G, Venter R, Henry B, Keet K (2020) Surgical anatomy of the sciatic nerve and its relationship to the piriformis muscle with a description of a rare variant. SA Orthop J 19:33–39
Bardeen CE (1901) A statistical study of variations in the formation andposition of the lumbosacral plexus in man. Anat Anz 19(124–143):209–238
Bardeen CR (1906) Development and variation of the nerves and the musculature of the inferior extremity and of the neighboring regions of the trunk in man. Am J Anat 6:259–390
Barton PM (1991) Piriformis syndrome: a rational approach to management. Pain 47:345–352. https://doi.org/10.1016/0304-3959(91)90227-O
Beaton L, Anson B (1938) The sciatic nerve and the piriformis muscle: their interrelation a possible cause of coccygodynia. J Bone Joint Surg 20:686–688
Beatty RA (1994) The piriformis muscle syndrome: a simple diagnostic maneuver. Neurosurgery 34:512–514. https://doi.org/10.1227/00006123-199403000-00018
Berihu BA, Debeb YG (2015) Anatomical variation in bifurcation and trifurcations of sciatic nerve and its clinical implications: in selected university in Ethiopia. BMC Res Notes 8:633. https://doi.org/10.1186/s13104-015-1626-6
Chiba S, Ishibashi Y, Kasai T (1994) Perforation of dorsal branches of the sacral nerve plexus through the piriformis muscle and its relation to changes of segmental arrangements of the vertebral column and others. Kaibogaku zasshi J Anat 69:281–305
Eisler P (1892) Der plexus lumbosacralis des menschen. Abhandlungen der Natur-forschenden Gesellschaft zu Halle Max Niemeyer 17:279–365
Fishman LM, Dombi GW, Michaelsen C, Ringel S, Rozbruch J, Rosner B, Weber C (2002) Piriformis syndrome: diagnosis, treatment, and outcome–a 10-year study. Arch Phys Med Rehabil 83:295–301. https://doi.org/10.1053/apmr.2002.30622
Gabrielli C, Olave E, Sarmento A, Mizusaki C, Prates JC (1997) Abnormal extrapelvic course of the inferior gluteal artery. Surg Radiol Anat 19:139–142. https://doi.org/10.1007/BF01627962
Gray H (1918) Anatomy of the human body, 20th edn. Lea & Febiger, Philadelphia and New Yoak
Güvençer M, Akyer P, Iyem C, Tetik S, Naderi S (2008) Anatomic considerations and the relationship between the piriformis muscle and the sciatic nerve. Surg Radiol Anat 30:467–474. https://doi.org/10.1007/s00276-008-0350-5
Jackson C (1914) Morris’s treatise on anatomy: a complete systematic treatise by English and American authors, 5th edn. P. Blakiston’s Son, Philadelphia
Jacomo AL, Martinez CAR, Saleh SO, Andrade M, Akamatsu FE (2014) Unusual relationship between the piriform muscle and sciatic, inferior gluteal and posterior femoral cutaneous nerves. Int J Morphol 32:432–434. https://doi.org/10.4067/S0717-95022014000200008
Jankovic D, Peng P, van Zundert A (2013) Brief review: piriformis syndrome: etiology, diagnosis, and management. Can J Anaesth 60:1003–1012. https://doi.org/10.1007/s12630-013-0009-5
Kosukegawa I, Yoshimoto M, Isogai S, Nonaka S, Yamashita T (1976) (2006) Piriformis syndrome resulting from a rare anatomic variation. Spine (Phila Pa) 31:E664-666. https://doi.org/10.1097/01.brs.0000231877.34800.71
Larionov A, Yotovski P, Filgueira L (2022) Novel anatomical findings with implications on the etiology of the piriformis syndrome. Surg Radiol Anat 44:1397–1407. https://doi.org/10.1007/s00276-022-03023-5
Martin HD, Kivlan BR, Palmer IJ, Martin RL (2014) Diagnostic accuracy of clinical tests for sciatic nerve entrapment in the gluteal region. Knee Surg Sports Traumatol Arthrosc 22:882–888. https://doi.org/10.1007/s00167-013-2758-7
Natsis K, Totlis T, Konstantinidis GA, Paraskevas G, Piagkou M, Koebke J (2014) Anatomical variations between the sciatic nerve and the piriformis muscle: a contribution to surgical anatomy in piriformis syndrome. Surg Radiol Anat 36:273–280. https://doi.org/10.1007/s00276-013-1180-7
Pace JB, Nagle D (1976) Piriform syndrome. West J Med 124:435–439
Papadopoulos EC, Khan SN (2004) Piriformis syndrome and low back pain: a new classification and review of the literature. Orthop Clin North Am 35:65–71. https://doi.org/10.1016/S0030-5898(03)00105-6
Pecina HI, Boric I, Smoljanovic T, Duvancic D, Pecina M (2008) Surgical evaluation of magnetic resonance imaging findings in piriformis muscle syndrome. Skeletal Radiol 37:1019–1023. https://doi.org/10.1007/s00256-008-0538-0
Pecina M (1979) Contribution to the etiological explanation of the piriformis syndrome. Acta Anat (Basel) 105:181–187
Piersol G (1919) Human Anatomy, 7th edn. J. B. Lippincott & Co., Philadelphia and London
Probst D, Stout A, Hunt D (2019) Piriformis syndrome: a narrative review of the anatomy, diagnosis, and treatment. PM R 11:54–63. https://doi.org/10.1002/pmrj.12189
Reynoso JP, De Jesus Encarnacion M, Nurmukhametov R, Melchenko D, Efe IE, Goncharov E, Taveras AA, Ramirez Pena IJ, Montemurro N (2022) Anatomical variations of the sciatic nerve exit from the pelvis and its relationship with the piriformis muscle: a cadaveric study. Neurol Int 14:894–902. https://doi.org/10.3390/neurolint14040072
Song WC, Bae SM, Han SH, Koh KS (2006) Anatomical and radiological study of the superior and inferior gluteal arteries in the gluteus maximus muscle for musculocutaneous flap in Koreans. J Plast Reconstr Aesthet Surg 59:935–941. https://doi.org/10.1016/j.bjps.2005.11.028
Sulak O, Sakalli B, Ozguner G, Kastamoni Y (2014) Anatomical relation between sciatic nerve and piriformis muscle and its bifurcation level during fetal period in human. Surg Radiol Anat 36:265–272. https://doi.org/10.1007/s00276-013-1179-0
Tan J, Bialowas C, Lowry N, Fahl J, Smith MP, Khan AS (2023) Variations in the vasculature of the gluteal region: a case report and clinical implications. Transl Res Anat. https://doi.org/10.1016/j.tria.2023.100248
Yan J, Takechi M, Hitomi J (2013) Variations in the course of the Inferior gluteal nerve and artery: a case report and literature review. Surg Sci 4:429–432. https://doi.org/10.4236/ss.2013.410084
Acknowledgements
The authors sincerely thank individual who donated her body to science so that anatomical research could be performed. Results from such research can potentially increase mankind’s overall knowledge that can then improve patient care. Therefore, the donor and her families deserve our highest gratitude.
Funding
The authors did not receive support from any organization for the present work.
Author information
Authors and Affiliations
Contributions
HA: conceptualization, methodology, data curation, manuscript writing. KT: methodology, data curation. RK: supervision. TT: resource. IK and KK: resource, supervision.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Ethical approval
This is an case report. We confirmed that no ethical approval is required based on the guidelines of The Japanese Association of Anatomists.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Anetai, H., Tokita, K., Kojima, R. et al. An atypical inferior gluteal artery passing through the piriformis muscle. Surg Radiol Anat 46, 59–64 (2024). https://doi.org/10.1007/s00276-023-03256-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-023-03256-y