Abstract
Purpose
The palatal mucosa is a major donor site for connective tissue in the field of periodontal plastic surgery, since it satisfies both the esthetic and functional demands of patients. The purpose of this study was to use histomorphometric analysis to measure the thicknesses of the palatal mucosa and the lamina propria including the epithelium on cadavers.
Methods
Thirty-four hemimaxillae of cadavers were examined (13 male and 4 female, mean age 57.2 years). Each maxilla was processed for histological sectioning and subsequently for histomorphometric analysis. The thicknesses of the palatal mucosa and the lamina propria including the epithelium were measured at three points starting from the alveolar crest, at intervals of 4 mm, with the aid of Adobe Photoshop.
Results
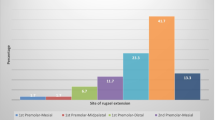
The thickness of the palatal mucosa at the alveolar crest and at 4 and 8 mm below the alveolar crest were 2.51 ± 0.83 (mean ± SD), 2.92 ± 0.80, and 3.62 ± 0.99 mm, respectively, and thus increasing from the alveolar crest toward the midpalatal suture. Conversely, the thicknesses of the lamina propria including the epithelium at these same positions were 2.06 ± 0.70, 1.54 ± 0.48, and 1.28 ± 0.46 mm, respectively, thus decreasing toward the midpalatal suture.
Conclusions
The present results indicate that clinicians need to be particularly careful when harvesting palatal mucosa that is destined to be used as autogenous donor material for connective tissue in periodontal plastic surgery.



Similar content being viewed by others
References
Barriviera M, Duarte WR, Januário AL, Faber J, Bezerra AC (2009) A new method to assess and measure palatal masticatory mucosa by cone-beam computerized tomography. J Clin Periodontol 36:564–568
Harris RJ (2003) Histologic evaluation of connective tissue grafts in humans. Int J Periodontics Restorative Dent 16:130–137
Karring T, Cumming BR, Oliver RC, Löe H (1975) The origin of granulation tissue and its impact on postoperative results of mucogingival surgery. J Periodontol 46:577–585
Khoury F, Happe A (2000) The palatal subepithelial connective tissue flap method for soft tissue management to cover maxillary defects: a clinical report. Int J Oral Maxillofac Implants 15:415–418
Klosek SK, Rungruang T (2009) Anatomical study of the greater palatine artery and related structures of the palatal vault: considerations for palate as the subepithelial connective tissue graft donor site. Surg Radiol Anat 31:245–250
Kobayashi K, Shimoda S, Nakagawa Y, Yamamoto A (2004) Accuracy in measurement of distance using limited cone-beam computerized tomography. Int J Oral Maxillofac Implants 19:228–231
Langer L, Langer B (1993) The subepithelial connective tissue graft for treatment of gingival recession. Dent Clin North Am 37:243–264
Lawson RB, Jones ML (1998) An evaluation of a noninvasive method of assessing alveolar bone levels in an experimental model of cleft lip and palate. Cleft Palate Craniofac J 35:1–8
Lee YJ, Kwon YH, Park JB, Herr Y, Shin SI, Heo SJ, Chung JH (2010) Epithelial thickness of the palatal mucosa: a histomorphometric study in Koreans. Anat Rec (Hoboken) 293:1966–1970
Methathrathip D, Apinhasmit W, Chompoopong S, Lertsirithong A, Ariyawatkul T, Sangvichien S (2005) Anatomy of greater palatine foramen and canal and pterygopalatine fossa in Thais: considerations for maxillary nerve block. Surg Radiol Anat 27:511–516
Mörmann W, Schaer F, Firestone AR (1981) The relationship between success of free gingival grafts and transplant thickness. Revascularization and shrinkage–a one year clinical study. J Periodontol 52:74–80
Müller HP, Schaller N, Eger T (1999) Ultrasonic determination of thickness of masticatory mucosa: a methodologic study. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 88:248–253
Nanci A (2005) Ten cate’s oral histology development, structure, and function. In: Oral Mucosa, 6th edn. Daehan Publishing Co, Seoul, pp 333–376 (in Korean)
Reiser GM, Bruno JF, Mahan PE, Larkin L (1996) The subepithelial connective tissue graft palatal donor site: anatomic considerations for surgeons. Int J Periodontics Restorative Dent 16:130–137
Sedon CL, Breault LG, Covington LL, Bishop BG (2005) The subepithelial connective tissue graft: part II. Histologic healing and clinical root coverage. J Contemp Dent Pract 6:139–150
Seibert JS, Salama H (1996) Alveolar ridge preservation and reconstruction. Periodontol 2000 11:69–84
Song JE, Um YJ, Kim CS, Choi SH, Cho KS, Kim CK, Chai JK, Jung UW (2008) Thickness of posterior palatal masticatory mucosa: the use of computerized tomography. J Periodontol 79:406–412
Stipetić J, Hrala Z, Celebić A (2005) Thickness of masticatory mucosa in the human hard palate and tuberosity dependent on gender and body mass index. Coll Antropol 29:243–247
Studer SP, Allen EP, Rees TC, Kouba A (1997) The thickness of masticatory mucosa in the human hard palate and tuberosity as potential donor sites for ridge augmentation procedures. J Periodontol 68:145–151
Sullivan HC, Atkins JH (1968) Free autogenous gingival grafts. Principles of successful grafting. Periodontics 6:121–129
Terakura T (1986) Non-invasive thickness measurement of the oral soft tissue. J Jpn Prosthodont Soc 30:1402–1411
Wara-aswapati N, Pitiphat W, Chandrapho N, Rattanayatikul C, Karimbux N (2001) Thickness of palatal masticatory mucosa associated with age. J Periodontol 72:1407–1412
Acknowledgments
This research was supported by Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education, Science and Technology (NRF-2011-0007227).
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Sun-Kyoung Yu and Baek-Hee Lee have contributed equally.
Rights and permissions
About this article
Cite this article
Yu, SK., Lee, BH., Lee, MH. et al. Histomorphometric analysis of the palatal mucosa associated with periodontal plastic surgery on cadavers. Surg Radiol Anat 35, 463–469 (2013). https://doi.org/10.1007/s00276-012-1066-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-012-1066-0