Abstract
Introduction and aim of study
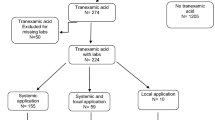
Tranexamic acid has been found to be effective in reducing peri-operative blood loss and is widely used across surgical specialties including orthopaedic surgery. However, there is still no consensus on the most appropriate and effective dose regimen. This study therefore compared the efficacy of single versus double dose regimens in patients that had interlocking intramedullary nailing by assessing the volume of drain output with the objective of determining the more effective regimen.
Methods
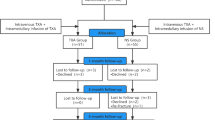
The study was a multicenter prospective study amongst adult patients who had interlocking intramedullary nailing for femoral nonunions. Following ethical approval, consent was obtained from eligible patients who were randomly assigned into two study groups. Group A patients had single pre-incision tranexamic acid bolus of one gram while group B patients had a second (repeat) one gram bolus (at the completion of wound closure). The volume of drain output at 48 h postop was the primary outcome measure and data collection was via an online data collection form linked to the google drive of the principal investigator. The mean of the drain output of the two groups was compared for statistical significance.
Results
A total of 61 patients participated in the study with 30 patients in group A and 31 patients in group B. The demographic data and duration of fracture were comparable in the two groups. Group A had a mean drain volume of 274.80 ml (± 103.93 ml) while group B had a mean of 187.94 ml (± 41.95 ml) and the difference was found to be statistically significant. (P, 0.000).
Conclusion
The findings suggest that double dose perioperative tranexamic acid regimen is superior to single-dose peri-operative tranexamic acid regimen in reducing post-operative blood loss in patients undergoing interlocking intramedullary nailing for femoral nonunions.
Similar content being viewed by others
Data availability
Relevant data and materials can be obtained at reasonable request from the corresponding author.
References
Simmons J, Sikorski RA, Pittet JF (2015) Tranexamic acid: from trauma to routine perioperative use. Curr Opin Anaesthiesiol 28(2):191–200
Poeran J, Rasul R, Suzuki S, Danninger T, Opperer M et al (2014) Tranexamic acid use and postoperative outcomes in patients undergoing total hip or knee arthroplasty in the United States; a retrospective analysis of effectiveness and safety. BMJ 349:g4829. https://doi.org/10.1136/bmj.g4829
Kinyanjui CK (2010) Factors affecting blood loss during open reduction and internal fixation (ORIF) of isolated closed femoral fractures at Mulago Hospital. East Afr Orthop J 4(2):48–51. https://doi.org/10.4314/eaoj.v4i2.63688
Madu K, Nnyagu H, Ede O (2018) Nonunion treatment outcomes in South East Nigeria. Niger J Orthop Trauma 17(2):77–80. https://doi.org/10.4103/njot.njot_23-18
Dada AA, Yinusa W, Giwa SO (2011) Review of the practice of traditional bone setting in Nigeria. Afr Health Sci 11(2):262–265
OlaOlorun DA, Oladiran IO, Adeniran A (2001) Complications of fracture treatment by traditional bone setters in South West Nigeria. Fam Pract 18(2):635–637. https://doi.org/10.1093/fampra/18.6.635
Prassad R, Patki A, Padhy S, Ramchandran G (2018) Single intravenous bolus versus perioperative continous infusion of tranexamic acid to reduce blood loss in abdominal oncosurgical procedures: a prospective randomized double blind clinical study. J Anaesthesio Clin Pharmacol 34(4):529–534. https://doi.org/10.4103/JOACP12217
Huang F, Wu D, Ma G, Yin Z, Wag Q (2014) The use of tranexamic acid to reduce blood loss and transfusion in major orthopaedic surgery: a meta-analysis. J Surg Res 186(1):318–327. https://doi.org/10.1016/j.jss.2013.08.020
Rjesparan K, Braut LC, Ahmad M, Field RE (2009) The effect of an intravenous bolus of tranexamic acid on blood loss in total hip replacement. J Bone Joint Surg Br 91(6):776–783. https://doi.org/10.1302/0301-620X.91B6.22393
Claeys MA, Vermeersch N, Haentjens P (2007) Reduction of blood loss with tranexamic acid in primary total hip replacement surgery. Acta Chir Belg 107(4):397–401. https://doi.org/10.1080/00015458.2007.11680081
Ferreira N, Marais LC, Aldous C (2014) Challenges and controversies in defining and classifying tibial nonunions. SA Orthop J 13(2):52–56
Thipparampall A, Gurajala I, Gopinath R (2017) The effect of different dose regimens of tranexamic acid in reducing blood loss during hip surgery. Indian J Anaesth 61(3):235–239. https://doi.org/10.4103/ija.IJA_495_16
Melvin JS, Stryker S, Sierra RJ (2015) Tranexamic acid in hip and knee arthroplasty. J Am Acad Orthop Surg 23(12):732–740. https://doi.org/10.5435/JAAOS-D-14-00223
Maniar RN, Kumer G, Singhi T, Nayak RM, Maniar PR (2012) Most effective regimen of tranexamic acid in knee arthroplasty; a prospective randomized controlled study in 240 patients. Clin Orthop Relat Res 470(9):2605–2612. https://doi.org/10.1007/s11999-012-2301-y
Benoni G, Bjorkman S, Fredin H (1995) Application of pharmacokinetic data from healthy volunteers for prediction of plasma concentrations of the tranexamic acid in surgical patients. Clin Drug Investig 10:280–287. https://doi.org/10.2165/00044011-199510050-00005
Steinhaus ME, Buksbaum J, Eisenmen A, Kohli M, Fragomen AT, Rozbruch RS (2020) Tranexamic acid reduces postoperative blood loss in distal femoral osteotomy. J Knee Surg 33(5):440–444. https://doi.org/10.1055/6s-0039-1678540
Motififard M, Tahririan MA, Saneie M, Badiei S, Nemati A (2015) Low dose perioperative intravenous tranexamic acid in patients undergoing total knee arthroplasty: a double blind randomized placebo controlled clinical trial. J Blood Transfus. https://doi.org/10.1155/2015/948304
Lin PC, Hsu CH, Huang CC, Chen WS, Wang JW (2012) The blood saving effect of tranexamic acid in minimally invasive total knee replacement; is an additional pre-operative injection effective? J Bone Joint Surg Br 94(7):932–936. https://doi.org/10.1202/0301-620X.94B7.28386
Pan WM, Li XG, Tang TS, Qian ZL, Zhang Q, Zhang CM (2010) Mini-subvastus versus a standard approach in total knee arthroplasty: a prospective, randomized, controlled study. J Int Med Res 38(3):890–900. https://doi.org/10.1177/147323001003800315
Author information
Authors and Affiliations
Contributions
All authors whose names appear in this submission: (1) made substantial contributions to the study conception, design, data acquisition and analysis; (2) were involved in manuscript preparation; (3) approved the version submitted for publication; and (4) agreed to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Ethical approval
Ethical approval was obtained from the Health Research and Ethics Committee (FMCB/HCS/HREC/APPR/VOL 2/10/2020).
Consent to participate
Informed consent for participation was obtained from all participating patients.
Consent to publish
Informed consent for publication was obtained from all study participants.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shodipo, O.M., Jatto, H.I., Ramat, A.M. et al. Comparison of single versus double tranexamic acid dose regimens in reducing post-operative blood loss following intramedullary nailing of femoral fracture nonunions. International Orthopaedics (SICOT) 46, 97–101 (2022). https://doi.org/10.1007/s00264-021-05220-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-021-05220-0