Abstract
Purpose
The rate of patients lost to follow-up may contribute to bias in randomized controlled trials (RCTs).
Methods
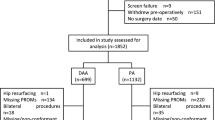
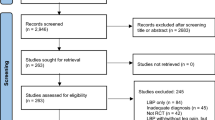
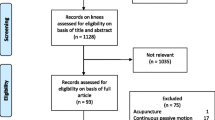
We systematically reviewed orthopaedic RCTs from 2008 to 2011, including 559 RCTs with 131,836 enrolled subjects. The loss to follow-up rates and minimum follow-up times were recorded for each trial. Orthopaedic subspecialty, country of origin, number of enrolled patients, patient age, follow-up strategy, and funding type were also recorded.
Results
Loss to follow-up was not reported in 111 of these studies (20 %). Mean loss to follow-up was 10.4 %. No orthopaedic subspecialty demonstrated significantly different follow-up rates. Remote follow-up strategies did not reduce the loss to follow-up rate. Studies with a minimum follow-up length of three years showed significantly higher loss to follow-up rates compared with studies with shorter minimum follow-up time (14.8 % versus 9.8 %, p = 0.01). Studies performed in the United States had a significantly higher rate of loss to follow-up compared with non-United States studies (13.8 % versus 9.4 %; p = 0.01).
Conclusions
Loss to follow-up rates in published orthopaedic randomized controlled trials is overall relatively low. A substantial portion of publications does not adequately report follow-up data. Studies performed in the United States and studies with longer follow-up periods seem to be at higher risk for loss to follow-up.


Similar content being viewed by others
References
Sprague S, Leece P, Bhandari M et al (2003) Limiting loss to follow-up in a multicenter randomized trial in orthopedic surgery. Control Clin Trials 24(6):719–725
Murray DW, Britton AR, Bulstrode CJ (1997) Loss to follow-up matters. J Bone Joint Surg (Br) 79(2):254–257
Norquist BM, Goldberg BA, Matsen FA (2000) Challenges in evaluating patients lost to follow-up in clinical studies of rotator cuff tears. J Bone Joint Surg 82(6):838–838
Bhandari M, Richards RR, Sprague S, Schemitsch EH (2002) The quality of reporting of randomized trials in the Journal of Bone and Joint Surgery from 1988 through 2000. J Bone Joint Surg Am 84(3):388–396
Begg C, Cho M, Eastwood S et al (1996) Improving the quality of reporting of randomized controlled trials. The CONSORT statement. JAMA 276(8):637–639
Chan S, Bhandari M (2007) The quality of reporting of orthopaedic randomized trials with use of a checklist for nonpharmacological therapies. J Bone Joint Surg 89(9):1970–1978. doi:10.2106/JBJS.F.01591
Sackett DL (2005) Evidence-based medicine. In: Armitage P, Colton T (eds) Encyclopedia of biostatistics. Wiley Online Library. doi:10.1002/0470011815.b2a08019
Zelle BA, Bhandari M, Sanchez AI, Probst C, Pape H-C (2013) Loss of follow-up in orthopaedic trauma: is 80% follow-up still acceptable? J Orthop Trauma 27(3):177–181. doi:10.1097/BOT.0b013e31825cf367
Kristman V, Manno M, Côté P (2004) Loss to follow-up in cohort studies: how much is too much? Eur J Epidemiol 219(8):751–760. doi:10.1023/B:EJEP.0000036568.02655.f8
Wright JG, Swiontkowski MF, Heckman JD (2003) Introducing levels of evidence to the journal. J Bone Joint Surg 85(1):1–3
Shea BJ, Grimshaw JM, Wells GA et al (2007) Development of AMSTAR: a measurement tool to assess the methodological quality of systematic reviews. BMC Med Res Methodol 7(1):10. doi:10.1186/1471-2288-7-10
Somerson JS, Bhandari M, Vaughan CT, Smith CS, Zelle BA (2014) Lack of diversity in orthopaedic trials conducted in the United States. J Bone Joint Surg Am 96(7), e56. doi:10.2106/JBJS.M.00531
Moher D, Hopewell S, Schulz KF et al (2010) CONSORT 2010 explanation and elaboration: updated guidelines for reporting parallel group randomised trials. BMJ 340:c869. doi:10.1136/bmj.c869
Solberg TK, Sørlie A, Sjaavik K, Nygaard ØP, Ingebrigtsen T (2011) Would loss to follow-up bias the outcome evaluation of patients operated for degenerative disorders of the lumbar spine? Acta Orthop 82(1):56–63. doi:10.3109/17453674.2010.548024
Imam MA, Barke S, Stafford GH, Parkin D, Field RE (2014) Loss to follow-up after total hip replacement: a source of bias in patient reported outcome measures and registry datasets? Hip Int 24(5):465–472. doi:10.5301/hipint.5000141
Pape H-C, Zelle B, Lohse R et al (2006) Evaluation and outcome of patients after polytrauma: can patients be recruited for long-term follow-up? Injury 37(12):1197–1203. doi:10.1016/j.injury.2006.07.032
Study to Prospectively Evaluate Reamed Intramedullary Nails in Patients with Tibial Fractures Investigators, Bhandari M, Guyatt G, Tornetta P 3rd, Schemitsch EH, Swiontkowski M, Sanders D, Walter SD (2008) Randomized trial of reamed and unreamed intramedullary nailing of tibial shaft fractures. J Bone Joint Surg Am 90(12):2567–2578. doi:10.2106/JBJS.G.01694
Kwon SK, Kang YG, Chang CB, Sung SC, Kim TK (2010) Interpretations of the clinical outcomes of the nonresponders to mail surveys in patients after total knee arthroplasty. J Arthroplasty 25(1):133–137. doi:10.1016/j.arth.2008.11.004
Mihelic AH, Crimmins EM (1997) Loss to follow-up in a sample of Americans 70 years of age and older: the LSOA 1984–1990. J Gerontol B Psychol Sci Soc Sci 52B(1):S37–S48. doi:10.1093/geronb/52B.1.S37
Psaty BM, Cheadle A, Koepsell TD et al (1994) Race- and ethnicity-specific characteristics of participants lost to follow-up in a telephone cohort. Am J Epidemiol 140(2):161–171
Janson SL, Alioto ME, Boushey HA (2001) Attrition and retention of ethnically diverse subjects in a multicenter randomized controlled research trial. Control Clin Trials 22(6 Suppl):S236–S243. doi:10.1016/S0197-2456(01)00171-4
Becker SJE, Guitton TG, Ring D (2014) Predictors of missed research appointments in a randomized placebo-controlled trial. Arch Bone Joint Surg 2(3):192–198
Zelle BA, Buttacavoli FA, Shroff JB, Stirton JB (2015) Loss of follow-up in orthopaedic trauma: who is getting lost to follow-up? J Orthop Trauma 29(11):510–515. doi:10.1097/BOT.0000000000000346
Hopewell S, Clarke M, Lefebvre C, Scherer R (2007) Handsearching versus electronic searching to identify reports of randomized trials. Cochrane Database Syst Rev 2, MR000001. doi:10.1002/14651858.MR000001.pub2
Baghdadi YMK, Larson AN, Sierra RJ (2015) Long-term results of the uncemented acetabular component in a primary total hip arthroplasty performed for protrusio acetabuli: a fifteen year median follow-up. Int Orthop 39(5):839–845. doi:10.1007/s00264-014-2580-y
Maisongrosse P, Lepage B, Cavaignac E et al (2015) Obesity is no longer a risk factor for dislocation after total hip arthroplasty with a double-mobility cup. Int Orthop 39(7):1251–1258. doi:10.1007/s00264-014-2612-7
Pailhé R, Cavaignac E, Murgier J et al (2016) Triple osteotomy of the pelvis for Legg-Calve-Perthes disease: a mean fifteen year follow-up. Int Orthop 40(1):115–122. doi:10.1007/s00264-015-2687-9
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this study.
Conflicts of interest
Boris A. Zelle has received research grants from DePuySynthes and the Orthopaedic Trauma Association. Boris A. Zelle has received a speaker honorarium from AO Trauma North America. None of which is related to this study.
M. Bhandari reports funding received from Smith & Nephew, Stryker, Amgen, Zimmer, Moximed, Bioventus, Merck, Eli Lilly, Sanofi, Ferring, Conmed, DePuy and Bioventus. None of which is related to this article.
Jeremy S. Somerson, Katherine C. Bartush, and Jeffrey Shroff declare that they have no conflicts of interest.
Appendix
Appendix
Classification of studies to orthopaedic subspecialty categories was performed by consensus to the following groups: orthopaedic trauma, sports medicine, pediatric orthopaedic surgery, foot and ankle surgery, adult hip and knee reconstruction, shoulder and elbow surgery, hand surgery and orthopedic oncology. Studies evaluating fracture prevention and medical management were categorized as orthopaedic trauma. Pediatric foot conditions (e.g. clubfoot) were categorized as pediatric orthopaedics. Shoulder and elbow conditions were categorized to sports medicine if they related to instability, while reconstructive and arthroplasty procedures were categorized to shoulder and elbow surgery.
The following orthopaedic and general medical journals were included in the hand search: Acta Orthopaedica Scandinavica, American Journal of Sports Medicine, Arthroscopy, BMC Musculoskeletal Disorders, British Medical Journal, Canadian Medical Association Journal, Clinical Orthopaedics and Related Research, European Spine Journal, Foot Ankle International, Hip International, Indian Journal of Orthopaedics, Injury, International Orthopaedics, Journal of the American Medical Association, Journal of Arthroplasty, Journal of Bone and Joint Surgery, Journal of Bone and Joint Surgery British, Journal of Hand Surgery American, Journal of Neurosurgery: Spine, Journal of Orthopaedic Research, Journal of Orthopaedic Trauma, Journal of Pediatric Orthopaedics, Journal of Pediatric Orthopaedics B, Journal of Shoulder and Elbow Surgery, Journal of Trauma, The Knee, Lancet, New England Journal of Medicine, Osteoarthritis and Cartilage, Physical Therapy, Spine, and The Spine Journal.
Rights and permissions
About this article
Cite this article
Somerson, J.S., Bartush, K.C., Shroff, J.B. et al. Loss to follow-up in orthopaedic clinical trials: a systematic review. International Orthopaedics (SICOT) 40, 2213–2219 (2016). https://doi.org/10.1007/s00264-016-3212-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-016-3212-5