Abstract
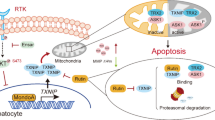
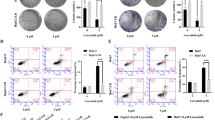
Metformin has been found to have inhibitory effects on a variety of tumors. However, its effects on non-small cell lung cancer (NSCLC) remain unclear. We demonstrated that metformin could inhibit the proliferation of A549 and H1299 cells. RNA transcriptome sequencing revealed that PDL1 was significantly downregulated in both cell types following treatment with metformin (P < 0.001). Jaspar analysis and chromatin immunoprecipitation showed that CEBPB could directly bind the promoter region of PDL1. Western blotting showed that protein expression of the isoforms CEBPB-LAP*, CEBPB-LAP, and CEBPB-LIP was significantly upregulated and the LIP/LAP ratio was increased. Gene chip analysis showed that PDL1 was significantly upregulated in A549-CEBPB-LAP cells and significantly downregulated in A549-CEBPB-LIP cells (P < 0.05) compared with CEBPB-NC cells. Dual-luciferase reporter gene assay showed that CEBPB-LAP overexpression could promote transcription of PDL1 and CEBPB-LIP overexpression could inhibit the process. Functional assays showed that the changes in CEBPB isoforms affected the function of NSCLC cells. Western blotting showed that metformin could regulate the function of NSCLC cells via AMPK–CEBPB–PDL1 signaling. Animal experiments showed that tumor growth was significantly inhibited by metformin, and atezolizumab and metformin had a synergistic effect on tumor growth. A total of 1247 patients were retrospectively analyzed, including 166 and 1081 patients in metformin and control groups, respectively. The positive rate of PDL1 was lower than that of the control group (HR = 0.338, 95% CI = 0.235–0.487; P < 0.001). In conclusion, metformin inhibited the proliferation of NSCLC cells and played an anti-tumor role in an AMPK–CEBPB–PDL1 signaling-dependent manner.





Similar content being viewed by others
Abbreviations
- AMPK:
-
AMP-activated protein kinase.
- ChIP:
-
Chromatin immunoprecipitation
- DEG:
-
Differential expressed genes
- EMT:
-
Epithelial interstitial transformation
- FC:
-
Fold change
- HR:
-
Hazard ratio
- NSCLC:
-
Non-small cell lung cancer
- OE:
-
Overexpressed
- PDL1:
-
Programmed cell death ligand-1
- qPCR:
-
Quantitative polymerase chain reaction
- SPF:
-
Specific pathogen-free
References
Yang P, Allen MS, Aubry MC et al (2005) Clinical features of 5,628 primary lung cancer patients: experience at mayo clinic from 1997 to 2003. Chest 128:452–462. https://doi.org/10.1378/chest.128.1.452
Wistuba II, Gelovani JG, Jacoby JJ, Davis SE, Herbst RS (2011) Methodological and practical challenges for personalized cancer therapies. Nat Rev Clin Oncol 8:135–141. https://doi.org/10.1038/nrclinonc.2011.2
Li JX, Huang JM, Jiang ZB, Li RZ, Sun A, Lai-Han Leung E, Yan PY (2019) Current clinical progress of PD-1/PD-L1 immunotherapy and potential combination treatment in non-small cell lung cancer. Integr Cancer Ther 18:1534735419890020. https://doi.org/10.1177/1534735419890020
Clark CA, Gupta HB, Sareddy G et al (2016) Tumor-intrinsic PD-L1 signals regulate cell growth, pathogenesis, and autophagy in ovarian cancer and melanoma. Cancer Res 76:6964–6974. https://doi.org/10.1158/0008-5472.CAN-16-0258
Zhang JJ, Zhang QS, Li ZQ, Zhou JW, Du J (2019) Metformin attenuates PD-L1 expression through activating hippo signaling pathway in colorectal cancer cells. Am J Trans Res 11:6965–6976
Xiong W, Hsieh CC, Kurtz AJ, Rabek JP, Papaconstantinou J (2001) Regulation of CCAAT/enhancer-binding protein-beta isoform synthesis by alternative translational initiation at multiple AUG start sites. Nucl Acids Res 29:3087–3098. https://doi.org/10.1093/nar/29.14.3087
Won C, Kim BH, Yi EH et al (2015) Signal transducer and activator of transcription 3-mediated CD133 up-regulation contributes to promotion of hepatocellular carcinoma. Hepatology 62:1160–1173. https://doi.org/10.1002/hep.27968
Akira S, Isshiki H, Sugita T, Tanabe O, Kinoshita S, Nishio Y, Nakajima T, Hirano T, Kishimoto T (1990) A nuclear factor for IL-6 expression (NF-IL6) is a member of a C/EBP family. EMBO J 9:1897–1906
Burgess-Beusse BL, Timchenko NA, Darlington GJ (1999) CCAAT/enhancer binding protein alpha (C/EBPalpha) is an important mediator of mouse C/EBPbeta protein isoform production. Hepatology 29:597–601. https://doi.org/10.1002/hep.510290245
Descombes P, Chojkier M, Lichtsteiner S, Falvey E, Schibler U (1990) LAP, a novel member of the C/EBP gene family, encodes a liver-enriched transcriptional activator protein. Genes Dev 4:1541–1551. https://doi.org/10.1101/gad.4.9.1541
Maehara O, Ohnishi S, Asano A, Suda G, Natsuizaka M, Nakagawa K, Kobayashi M, Sakamoto N, Takeda H (2019) Metformin regulates the expression of CD133 Through the AMPK-CEBPbeta pathway in hepatocellular carcinoma cell lines. Neoplasia 21:545–556. https://doi.org/10.1016/j.neo.2019.03.007
Vallianou NG, Evangelopoulos A, Kazazis C (2013) Metformin and cancer. Rev Diabet Stud: RDS 10:228–235. https://doi.org/10.1900/RDS.2013.10.228
Lin CC, Yeh HH, Huang WL, Yan JJ, Lai WW, Su WP, Chen HH, Su WC (2013) Metformin enhances cisplatin cytotoxicity by suppressing signal transducer and activator of transcription-3 activity independently of the liver kinase B1-AMP-activated protein kinase pathway. Am J Respir Cell Mol Biol 49:241–250. https://doi.org/10.1165/rcmb.2012-0244OC
Queiroz EA, Puukila S, Eichler R et al (2014) Metformin induces apoptosis and cell cycle arrest mediated by oxidative stress, AMPK and FOXO3a in MCF-7 breast cancer cells. PLoS ONE 9:e98207. https://doi.org/10.1371/journal.pone.0098207
Vernieri C, Signorelli D, Galli G et al (2019) Exploiting fasting-mimicking diet and metformin to improve the efficacy of platinum-pemetrexed chemotherapy in advanced LKB1-inactivated lung adenocarcinoma: the FAME trial. Clin Lung Cancer 20:e413–e417. https://doi.org/10.1016/j.cllc.2018.12.011
Shackelford DB, Abt E, Gerken L et al (2013) LKB1 inactivation dictates therapeutic response of non-small cell lung cancer to the metabolism drug phenformin. Cancer Cell 23:143–158. https://doi.org/10.1016/j.ccr.2012.12.008
Graham GG, Punt J, Arora M et al (2011) Clinical pharmacokinetics of metformin. Clin Pharmacokinet 50:81–98. https://doi.org/10.2165/11534750-000000000-00000
Gravel SP, Hulea L, Toban N et al (2014) Serine deprivation enhances antineoplastic activity of biguanides. Cancer Res 74:7521–7533. https://doi.org/10.1158/0008-5472.CAN-14-2643-T
Chandel NS, Avizonis D, Reczek CR et al (2016) Are metformin doses used in murine cancer models clinically relevant? Cell Metab 23:569–570. https://doi.org/10.1016/j.cmet.2016.03.010
Zhou H, Liu J, Zhang Y, Zhang L (2019) Inflammatory bowel disease associated with the combination treatment of nivolumab and metformin: data from the FDA adverse event reporting system. Cancer Chemother Pharmacol 83:599–601. https://doi.org/10.1007/s00280-018-03763-5
Pardoll DM (2012) The blockade of immune checkpoints in cancer immunotherapy. Nat Rev Cancer 12:252–264. https://doi.org/10.1038/nrc3239
Kleffel S, Posch C, Barthel SR et al (2015) Melanoma cell-Intrinsic PD-1 receptor functions promote tumor growth. Cell 162:1242–1256. https://doi.org/10.1016/j.cell.2015.08.052
Chang CH, Qiu J, O’Sullivan D et al (2015) Metabolic competition in the tumor microenvironment is a driver of cancer progression. Cell 162:1229–1241. https://doi.org/10.1016/j.cell.2015.08.016
Zheng A, Li F, Chen F, Zuo J, Wang L, Wang Y, Chen S, Xiao B, Tao Z (2019) PDL1 promotes head and neck squamous cell carcinoma cell growth through mTOR signaling. Oncol Rep 41:2833–2843. https://doi.org/10.3892/or.2019.7053
Cao Y, Zhang L, Kamimura Y, Ritprajak P, Hashiguchi M, Hirose S, Azuma M (2011) B7–H1 overexpression regulates epithelial-mesenchymal transition and accelerates carcinogenesis in skin. Cancer Res 71:1235–1243. https://doi.org/10.1158/0008-5472.CAN-10-2217
Alsuliman A, Colak D, Al-Harazi O, Fitwi H, Tulbah A, Al-Tweigeri T, Al-Alwan M, Ghebeh H (2015) Bidirectional crosstalk between PD-L1 expression and epithelial to mesenchymal transition: significance in claudin-low breast cancer cells. Mol Cancer 14:149. https://doi.org/10.1186/s12943-015-0421-2
Ghebeh H, Tulbah A, Mohammed S, Elkum N, Bin Amer SM, Al-Tweigeri T, Dermime S (2007) Expression of B7–H1 in breast cancer patients is strongly associated with high proliferative Ki-67-expressing tumor cells. Int J Cancer 121:751–758. https://doi.org/10.1002/ijc.22703
Qorraj M, Bruns H, Bottcher M, Weigand L, Saul D, Mackensen A, Jitschin R, Mougiakakos D (2017) The PD-1/PD-L1 axis contributes to immune metabolic dysfunctions of monocytes in chronic lymphocytic leukemia. Leukemia 31:470–478. https://doi.org/10.1038/leu.2016.214
Mariathasan S, Turley SJ, Nickles D et al (2018) TGFbeta attenuates tumour response to PD-L1 blockade by contributing to exclusion of T cells. Nature 554:544–548. https://doi.org/10.1038/nature25501
Russell A, Boone B, Jiang A, Sealy L (2010) Genomic profiling of C/EBPbeta2 transformed mammary epithelial cells: a role for nuclear interleukin-1beta. Cancer Biol Ther 10:509–519. https://doi.org/10.4161/cbt.10.5.12725
Regalo G, Forster S, Resende C et al (2016) C/EBPbeta regulates homeostatic and oncogenic gastric cell proliferation. J Mol Med 94:1385–1395. https://doi.org/10.1007/s00109-016-1447-7
Sundfeldt K, Ivarsson K, Carlsson M, Enerback S, Janson PO, Brannstrom M, Hedin L (1999) The expression of CCAAT/enhancer binding protein (C/EBP) in the human ovary in vivo: specific increase in C/EBPbeta during epithelial tumour progression. Br J Cancer 79:1240–1248. https://doi.org/10.1038/sj.bjc.6690199
Rask K, Thorn M, Ponten F, Kraaz W, Sundfeldt K, Hedin L, Enerback S (2000) Increased expression of the transcription factors CCAAT-enhancer binding protein-beta (C/EBBeta) and C/EBzeta (CHOP) correlate with invasiveness of human colorectal cancer. Int J Cancer 86:337–343. https://doi.org/10.1002/(sici)1097-0215(20000501)86:3%3c337::aid-ijc6%3e3.0.co;2-3
Li Y, Bevilacqua E, Chiribau CB, Majumder M, Wang C, Croniger CM, Snider MD, Johnson PF, Hatzoglou M (2008) Differential control of the CCAAT/enhancer-binding protein beta (C/EBPbeta) products liver-enriched transcriptional activating protein (LAP) and liver-enriched transcriptional inhibitory protein (LIP) and the regulation of gene expression during the response to endoplasmic reticulum stress. J Biol Chem 283:22443–22456. https://doi.org/10.1074/jbc.M801046200
Wethmar K, Begay V, Smink JJ, Zaragoza K, Wiesenthal V, Dorken B, Calkhoven CF, Leutz A (2010) C/EBPbetaDeltauORF mice–a genetic model for uORF-mediated translational control in mammals. Genes Dev 24:15–20. https://doi.org/10.1101/gad.557910
Smink JJ, Begay V, Schoenmaker T, Sterneck E, de Vries TJ, Leutz A (2009) Transcription factor C/EBPbeta isoform ratio regulates osteoclastogenesis through MafB. EMBO J 28:1769–1781. https://doi.org/10.1038/emboj.2009.127
Buck M, Poli V, Hunter T, Chojkier M (2001) C/EBPbeta phosphorylation by RSK creates a functional XEXD caspase inhibitory box critical for cell survival. Mol Cell 8:807–816. https://doi.org/10.1016/s1097-2765(01)00374-4
Tang QQ, Gronborg M, Huang H, Kim JW, Otto TC, Pandey A, Lane MD (2005) Sequential phosphorylation of CCAAT enhancer-binding protein beta by MAPK and glycogen synthase kinase 3beta is required for adipogenesis. Proc Natl Acad Sci USA 102:9766–9771. https://doi.org/10.1073/pnas.0503891102
Li X, Kim JW, Gronborg M, Urlaub H, Lane MD, Tang QQ (2007) Role of cdk2 in the sequential phosphorylation/activation of C/EBPbeta during adipocyte differentiation. Proc Natl Acad Sci USA 104:11597–11602. https://doi.org/10.1073/pnas.0703771104
Acknowledgements
This work was supported by grants from National Natural Science Foundation of China (No. 81401875) and the Research Program of Shanghai Health Commission (Grant No. 20204Y022). We have asked the International Science Editing Corporation for editing the language.
Author information
Authors and Affiliations
Contributions
CZ and WJ take responsibility for the integrity of the work as a whole. CZ, WJ, and TL conceived the study. TL, ML, and MNZ performed most of the bioinformatics analysis and wrote the manuscript. GSB, YWH, JQL, ZCC, and YSZ collected the tumor samples and analyzed the data of clinical characteristics. JJX, ZWL, and QW helped project design and manuscript editing. LLT supervised this study.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflict of interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lu, T., Li, M., Zhao, M. et al. Metformin inhibits human non-small cell lung cancer by regulating AMPK–CEBPB–PDL1 signaling pathway. Cancer Immunol Immunother 71, 1733–1746 (2022). https://doi.org/10.1007/s00262-021-03116-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-021-03116-x