Abstract
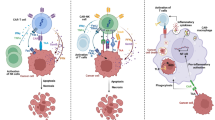
Renal cell carcinoma (RCC) is known to respond to immune checkpoint blockade (ICB) therapy, whereas there has been limited analysis of T-cell responses to RCC. In this study, we utilized human carbonic anhydrase 9 (hCA9) as a model neoantigen of mouse RENCA RCC. hCA9-expressing RENCA RCC (RENCA/hCA9) cells were rejected in young mice but grew in aged mice. CD8+ T cells were the primary effector cells involved in rejection in young mice, whereas CD4+ T cells participated at the early stage. Screening of a panel of hCA9-derived peptides revealed that mouse CD8+ T cells responded to hCA9288–296 peptide. Mouse CD4+ T cells responded to lysates of RENCA/hCA9, but not RENCA cells, and showed reactivity to hCA9 276–290, which shares three amino acids with hCA9 288–296 peptide. Immunohistochemistry analysis revealed that few T cells infiltrated RENCA/hCA9 tissues in aged mice. ICB therapy of anti-PD-1/anti-CTLA-4 antibodies promoted T-cell infiltration into tumor tissues, whereas no definite antitumor effect was observed. However, additional combination with cyclophosphamide or axitinib, a vascular endothelial growth factor receptor inhibitor, induced complete regression in half of the RENCA/hCA9-bearing aged mice with increased expression of PD-L1 in tumor tissues. These results indicate that hCA9 can be a useful model neoantigen to investigate antitumor T-cell responses in mice with RCC, and that RENCA/hCA9 in aged mice can serve as a non-inflamed ‘cold’ tumor model facilitating the development of effective combined immunotherapies for RCC.







Similar content being viewed by others
References
Pardoll DM (2012) The blockade of immune checkpoints in cancer immunotherapy. Nat Rev Cancer 12(4):252–264. https://doi.org/10.1038/nrc3239
Topalian S, Taube JM, Anders RA, Pardoll DM (2016) Mechanism-driven biomarkers to guide immune checkpoint blockade in cancer therapy. Nat Rev Cancer 16(5):275–287. https://doi.org/10.1038/nrc.2016.36
Ott PA, Hodi FS, Robert C (2013) CTLA-4 and PD-1/PD-L1 blockade: new immunotherapeutic modalities with durable clinical benefit in melanoma patients. Clin Cancer Res 19(19):5300–5309. https://doi.org/10.1158/1078-0432.CCR-13-0143
Postow MA, Callahan MK, Wolchok JD (2015) Immune checkpoint blockade in cancer therapy. J Clin Oncol 33(17):1974–1982. https://doi.org/10.1200/JCO.2014.59.4358
Gubin MM, Zhang X, Schuster H et al (2014) Checkpoint blockade cancer immunotherapy targets tumour-specific mutant antigens. Nature 515(7528):577–581. https://doi.org/10.1038/nature13988
Sharma P, Allison JP (2015) Immune checkpoint targeting in cancer therapy: toward combination strategies with curative potential. Cell 161(2):205–214. https://doi.org/10.1016/j.cell.2015.03.030
Van Allen EM, Miao D, Schilling B et al (2015) Genomic correlates of response to CTLA-4 blockade in metastatic melanoma. Science 350(6257):207–211. https://doi.org/10.1126/science.aad0095
Rizvi NA, Hellmann MD, Snyder A et al (2015) Cancer immunology. Mutational landscape determines sensitivity to PD-1 blockade in non-small cell lung cancer. Science 348(6230):124–128. https://doi.org/10.1126/science.aaa1348
Alexandrov LB, Nik-Zainal S, Wedge DC et al (2013) Signatures of mutational processes in human cancer. Nature 500(7463):415–421. https://doi.org/10.1038/nature12477
Turajlic S, Litchfield K, Xu H et al (2017) Insertion-and-deletion-derived tumour-specific neoantigens and the immunogenic phenotype: a pan-cancer analysis. Lancet Oncol 18(8):1009–1021. https://doi.org/10.1016/S1470-2045(17)30516-8
Hansen UK, Ramskov S, Bjerregaard AM et al (2020) Tumor-infiltrating T cells from clear cell renal cell carcinoma patients recognize neoepitopes derived from point and frameshift mutations. Front Immunol 11:373. https://doi.org/10.3389/fimmu.2020.00373
Kawagoe N, Shintaku I, Yutani S, Etoh H, Matsuoka K, Noda S, Itoh K (2000) Expression of the SART3 tumor rejection antigen in renal cell carcinoma. J Urol 164(6):2090–2095
Flad T, Spengler B, Kalbacher H et al (1998) Direct identification of major histocompatibility complex class I-bound tumor-associated peptide antigens of a renal carcinoma cell line by a novel mass spectrometric method. Cancer Res 58(24):5803–5811
Hanada K, Yewdell JW, Yang JC (2004) Immune recognition of a human renal cancer antigen through post-translational protein splicing. Nature 427(6971):252–256. https://doi.org/10.1038/nature02240
Takahashi Y, Harashima N, Kajigaya S et al (2008) Regression of human kidney cancer following allogeneic stem cell transplantation is associated with recognition of an HERV-E antigen by T cells. J Clin Invest 118(3):1099–1109. https://doi.org/10.1172/JCI34409
Minami T, Minami T, Shimizu N, Yamamoto Y, De Velasco M, Nozawa M, Yoshimura K, Harashima N, Harada M, Uemura H (2014) Identification of erythropoietin receptor-derived peptides having the potential to induce cancer-reactive cytotoxic T lymphocytes from HLA-A24+ patients with renal cell carcinoma. Int Immunopharm 20(1):59–65. https://doi.org/10.1016/j.intimp.2014.02.018
Minami T, Minami T, Shimizu N, Yamamoto Y, De Velasco M, Nozawa M, Yoshimura K, Harashima N, Harada M, Uemura H (2015) Identification of programmed death ligand 1-derived peptides capable of inducing cancer-reactive cytotoxic T lymphocytes from HLA-A24+ patients with renal cell carcinoma. J Immunother 38(7):285–291. https://doi.org/10.1097/CJI.0000000000000090
Minami T, Matsumura N, Sugimoto K, Shimizau N, De Velsasco Nozawa M, Yoshimura K, Harashima N, Harada M, Uemura H (2017) Hypoxia-inducing factor (HIF)-1a-derived peptide capable of inducing cancer-reactive cytotoxic T lymphocytes from HLA-A24+ patients with renal cell carcinoma. Int Immunopharm 44:197–202. https://doi.org/10.1016/j.intimp.2017.01.014
Komohara Y, Harada M, Ishihara Y, Suekane S, Nogichi M, Yamada A, Itoh K (2007) HLA-G as a target molecule in specific immunotherapy against renal cell carcinoma. Oncol Rep 18(6):1463–1468
Pantuck AJ, Zeng G, Belldegrun AS et al (2003) Pathobiology, prognosis, and targeted therapy for renal cell carcinoma: exploiting the hypoxia-induced pathway. Clin Cancer Res 9(13):4641–4652
Uemura H, Okajima E, Debruyne FM, Oosterwijk E (1994) Internal image anti-idiotype antibodies related to renal-cell carcinoma-associated antigen G250. Int J Cancer 56(4):609–614. https://doi.org/10.1002/ijc.2910560424
Uemura H, Fujimoto K, Tanaka M, Yoshikawa M, Hirao Y, Uejima S, Yoshikawa K, Itoh K (2006) A phase I trial of vaccination of CA9-derived peptides for HLA-A24-positive patients with cytokine-refractory metastatic renal cell carcinoma. Clin Cancer Res 12(6):1768–1775. https://doi.org/10.1158/1078-0432.CCR-05-2253
Shimizu K, Uemura H, Yoshikawa M, Yoshida K, Hirao Y, Iwashima K, Saga S, Yoshikawa K (2003) Induction of antigen specific cellular immunity by vaccination with peptides from MN/CA IX in renal cell carcinoma. Oncol Rep 10(5):1307–1311
Lustgarten J (2009) Cancer, aging and immunotherapy: lessons learned from animal models. Cancer Immunol Immunother 58(12):1979–1989. https://doi.org/10.1007/s00262-009-0677-8
Nakagawa T, Ohnishi K, Kosaki Y, Saito Y, Horlad H, Fujiwara Y, Takeya M, Komohara Y (2017) Optimum immunohistochemical procedures for analysis of macrophages in human and mouse formalin fixed paraffin-embedded tissue samples. J Clin Exp Hematop 57(1):31–36. https://doi.org/10.3960/jslrt.17017
Motzer RJ, Penkov K, Haanen J et al (2019) Avelumab plus axitinib versus sunitinib for advanced renal-cell carcinoma. New Engl J Med 380(12):1103–1115. https://doi.org/10.1056/NEJMoa1816047
Rini BI, Plimack ER, Stus V et al (2019) Pembrolizumab plus axitinib versus sunitinib for advanced renal-cell carcinoma. New Engl J Med 380(12):1116–1127. https://doi.org/10.1056/NEJMoa1816714
Youn JI, Nagaraj S, Collazo M, Gabrilovich (2008) Subsets of myeloid-derived suppressor cells in tumor-bearing mice. J Immunol 181(8):5791–5802. https://doi.org/10.4049/jimmunol.181.8.5791
Yang J, Yan J, Liu B (2018) Targeting VEGF/VEGFR to modulate antitumor immunity. Front Immunol 3(9):978. https://doi.org/10.3389/fimmu.2018.0097
Chai D, Shan H, Wang G et al (2019) Combining DNA vaccine and AIM2 in H1 nanoparticles exert anti-renal carcinoma effects via enhancing tumor-specific multi-functional CD8+ T-cell responses. Mol Cancer Ther 18(2):323–334. https://doi.org/10.1158/1535-7163.MCT-18-0832
Shvarts O1, Janzen N, Lam JS, Leppert JT, Caliliw R, Figlin RA, Belldegrun AS, Zeng G (2006) RENCA/carbonic anhydrase-IX: a murine model of a carbonic-IX-expressing renal cell carcinoma. Urology 68(5):1132–1138. https://doi.org/10.1016/j.urology.2006.08.1073
Kim BR, Yang EK, Kim DY, Kim SH, Moon DC, Lee JH, Kim HJ, Lee JC (2012) Generation of anti-tumour immune response using dendritic cells pulsed with carbonic anhydrase IX-Acinetobacter baumannil outer membrane protein A fusion proteins against renal cell carcinoma. Clin Exp Immunol 167(1):73–83. https://doi.org/10.1111/j.1365-2249.2011.04489.x
Herbert N, Haferkamp A, Schmitz-Winnenthal HF, Zöller M (2010) Concomitant tumor and autoantigen vaccination supports renal cell carcinoma rejection. J Immunol 185(2):902–916. https://doi.org/10.4049/jimmunol.0902683
Birkhäuser FD, Koya RC, Neufeld C et al (2013) Dendritic cell-based immunotherapy in prevention and treatment of renal cell carcinoma: efficacy, safety, and activity of Ad-GM·CAIX in immunocompetent mouse models. J Immunother 36(2):102–111. https://doi.org/10.1097/CJI.0b013e31827bec97
Ishikawa S, Matsui Y, Wachi S, Yamaguchi H, Harashima N, Harada M (2016) Age-associated impairment of antitumor immunity in carcinoma-bearing mice and restoration by oral administration of Lentinula edodes mycelia extract. Cancer Immunol Immunotherapy 65(8):961–972. https://doi.org/10.1007/s00262-016-1857-y
Rammensee HG (1995) Chemistry of peptides associated with MHC class I and class II molecules. Curr Opin Immunol 7(1):85–96. https://doi.org/10.1016/0952-7915(95)80033-6
Albert ML, Jegathesan M, Darnell RB (2001) Dendritic cell maturation is required for the cross-tolerization of CD8+ T cells. Nat Immunol 2(11):1010–1017. https://doi.org/10.1038/ni722
Kreiter S, Vormehr, van de Romer N et al (2015) Mutant MHC class II epitopes drive therapeutic immune responses to cancer. Nature 520(7780):692–696. https://doi.org/10.1038/nature14426
Alspach E, Lussier DM, Miceli AP et al (2019) MHC-II neoantigens shape tumour immunity and response to immunotherapy. Nature 574:696–701. https://doi.org/10.1038/s41586-019-1671-8
Tumeh PC, Harview CL, Yearley JH et al (2014) PD-1 blockade induces responses by inhibiting adaptive immune resistance. Nature 515(7528):568–571. https://doi.org/10.1038/nature13954
Bonaventura P, Shekarian T, Alcazer V et al (2019) Cold tumors: a therapeutic challenge for immunotherapy. Front Immunol 10:168. https://doi.org/10.3389/fimmu.2019.00168
Galon J, Bruni D (2019) Approaches to treat immune hot, altered and cold tumours with combination immunotherapies. Nat Rev Drug Discov 18(3):197–218. https://doi.org/10.1038/s41573-018-0007-y
Iida Y, Harashima N, Motoshima T et al (2017) Contrasting effects of cyclophosphamide on anti-CTLA-4 blockade therapy in two tumor mouse models. Cancer Sci 108(10):1974–1984. https://doi.org/10.1111/cas.13337
Chen DS, Mellman I (2017) Elements of cancer immunity and the cancer-immune set point. Nature 541(7637):321–330. https://doi.org/10.1038/nature21349
Kroemer G, Galluzzi L, Kepp O, Zitvogel L (2013) Immunogenic cell death in cancer therapy. Annu Rev Immunol 31:51–72. https://doi.org/10.1146/annurev-immunol-032712-100008
Sistigu A, Viaud S, Chaput N, Bracci L, Proietti E, Zitvogel L (2011) Immunomodulatory effects of cyclophosphamide and implementations for vaccine design. Semin Immunopathol 33(4):369–368. https://doi.org/10.1007/s00281-011-0245-0
Four SD, Maenhout SK, Pierre KD, Renmans D, Niclou SP, Thielemans K, Neyns B, Aerts JL (2015) Axitinib increases the infiltration of immune cells and reduces the suppressive capacity of monocytic MDSCs in an intracranial mouse melanoma model. Oncoimmunol 22(4):e998107. https://doi.org/10.1080/2162402X.2014.998107
Acknowledgements
This study was supported in part by JSPS KAKENHI Grants (No. 17K07217 to M Harada, No. 17K11301 to K Yoshikawa, and No. 19H03794 for H Uemura), Suzuken Memorial Foundation to Y Iida, and SHIMANE “SUIGAN” Project to M Harada.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Harada, M., Iida, Y., Kotani, H. et al. T-cell responses and combined immunotherapy against human carbonic anhydrase 9-expressing mouse renal cell carcinoma. Cancer Immunol Immunother 71, 339–352 (2022). https://doi.org/10.1007/s00262-021-02992-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-021-02992-7