Abstract
Accurate measurement of oxygen consumption (VO2) is important to precise calculation of blood flow using the Fick equation. This study aimed to validate the breath-by-breath method (BBBM) of measuring oxygen consumption VO2 compared with respiratory mass spectroscopy (MS) for intubated children during cardiac catheterization. The study used MS and BBBM to measure VO2 continuously and simultaneously for 10 min in consecutive anesthetized children undergoing cardiac catheterization who were intubated with a cuffed endotracheal tube, ventilated mechanically, and hemodynamically stable, with normal body temperature. From 26 patients, 520 data points were obtained. The mean VO2 was 94.5 ml/min (95 % confidence interval [CI] 65.7–123.3 ml/min) as measured by MS and 91.4 ml/min (95 % CI 64.9–117.9 ml/min) as measured by BBBM. The mean difference in VO2 measurements between MS and BBBM (3.1 ml/min; 95 % CI −1.7 to +7.9 ml/min) was not significant (p = 0.19). The MS and BBBM VO2 measurements were highly correlated (R 2 = 0.98; P < 0.0001). Bland–Altman analysis showed good correspondence between MS and BBBM, with a mean difference of −3.01 and 95 % limits of agreement ranging from −26.2 to +20.0. The mean VO2 indexed to body surface area did not differ significantly between MS and BBBM (3.4 ml/min m2; 95 % CI −1.4 to 8.2; p = 0.162). The mean difference and limits of agreement were −3.8 ml/min m2 (range, −19.9 to 26.7). Both MS and BBBM may be used to measure VO2 in anesthetized intubated children undergoing cardiac catheterization. The two methods demonstrated excellent agreement. However, BBBM may be more suited to clinical use with children.
Similar content being viewed by others
Accurate measurement of oxygen consumption (VO2) is essential to precise calculation of blood flow and cardiac output using the Fick equation:
Important clinical decisions are made for children with congenital heart disease based on the results of calculations using the Fick equation.
A number of investigators have shown the unreliability of assuming VO2 based on tables and formulas [8, 9, 12]. However, an assumed VO2 often is used because a suitable alternative readily adaptable to routine clinical practice is lacking, especially for intubated mechanically ventilated children. Respiratory mass spectroscopy (MS) measures VO2 accurately in ventilated subjects [8, 9, 12, 14].
Mass spectroscopy has many disadvantages in daily clinical practice due to the large size of the equipment, as well as its noise, high maintenance cost, need for constant technical monitoring, and specialized operator training requirements. In addition, the most widely used MS device in clinical research (AMIS 2000; Innovision, Odense, Denmark) is no longer manufactured.
The breath-by-breath method (BBBM) of expired gas analysis [4, 13] using the Innocor™ device (Innovision, Odense, Denmark) may be a useful alternative. We therefore sought to compare BBBM with MS in mechanically ventilated children undergoing cardiac catheterization.
Methods
The University of Alberta Research Ethics Review Board approved the study (Approval #Pro00018766). Informed written consent for participation in the study was obtained from the parents of all children and from the older children.
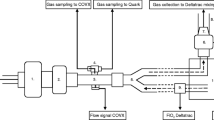
Measurement of VO2 (Fig. 1)
Breath-by-Breath Method
We used the Innocor™ inert gas rebreathing unit (Innovision, Odense, Denmark) based on gas analysis by BBBM. To use this method for intubated mechanically ventilated subjects, we added a flow meter (Hans Rudolph flow meter, 4500B and 8411B) between the endotracheal tube and the connection to the anesthetic device and the ventilator.
The flow meter was connected to the Innocor™ for gas analysis (Fig. 1). The Innocor™ estimates the difference in oxygen concentration between inspiration and expiration with each breath. This is achieved by integrating the product of oxygen concentration and flow in the respiratory gas during an interval, which covers a complete respiratory cycle.
The current purchase price of the Innocor™ is US$ 48,253, and the costs for its maintenance are approximately US$1,900 per year. The setup time, including calibration for each use, with practice, is 15–20 min. Between uses, the Innocor™ is turned off and may be stored remotely from the location of use. The warm-up time for each use is 100 s.
Mass Spectroscopy
We used the AMIS 2000 MS device for mass spectroscopy [9]. All expired gas was collected in a mixing chamber. An indicator gas, Argon, was added to the input port of the chamber. The oxygen consumption was determined by the differences in the measured O2 and argon concentrations between the inspired and expired gas.
The mass spectrometer (AMIS 2000) is no longer available for purchase. The last listed price by the manufacturer was approximately US$100,000, with maintenance costs of approximately US$12,000 per year. Between uses, the AMIS 2000 needs to remain turned on and running. It functions better if it remains at the location in which measurements are made. If it is stored remote from the location of use, it then requires a warm-up time of 8–12 h in the location of use for the best results. The setup time and the calibration for each use of the AMIS 2000 is 60 min if it is not stored in the location of use.
We calibrated both devices before each use according to the manufacturer’s instructions. Height and weight were measured the day before cardiac catheterization, and body surface area was calculated.
All the subjects were anesthetized with continuous intravenous infusions of remifentanyl and muscle-relaxed with rocuronium. They were intubated with a cuffed endotracheal tube (Mallinckrodt Medical, Northampton, UK) and mechanically ventilated with normal body temperature during VO2 measurements. We checked for a gas leak in the circuit using the anesthetic device measurement of inspired and expired gas volumes. Both the AMIS 2000 and the Innocor™ were connected to the ventilator circuit so simultaneous VO2 measurements could be obtained. Once a stable baseline was reached, the VO2 of each subject was measured continuously for 10 min.
Statistical Analysis
All statistical analyses were performed using the Statistical Package for the Social Sciences (SPSS), version 13 (SPSS Inc., Chicago, IL, USA), and the results were presented as mean values ± standard deviations unless otherwise stated. We compared mean VO2 (ml/min) and indexed VO2 (ml/min m2) using a paired Student’s t test. Bland–Altman plots were used to assess agreements between the two methods of measuring VO2 [2]. Linear regression analysis was performed to examine the correlation between the two methods of measuring VO2.
Results
Between June 2011 and April 2012, the study enrolled 26 consecutive patients with congenital heart disease who underwent routine cardiac catheterization under general anesthesia. The congenital heart diseases included patent ductus arteriosus (n = 2), atrial septal defect (n = 3) ventricular septal defect (n = 3), pulmonary valve stenosis (n = 4), coarctation of the aorta (n = 1), pulmonary artery hypertension (n = 6), post-cardiac transplantation (n = 1), post-arterial switch operation for transposition of the great arteries (n = 1); post-tetralogy of Fallot repair (n = 2), and hypoplastic left heart syndrome after completion of Fontan (n = 3).
The ages of the 14 male and 12 male subjects ranged from 0.4 to 20 years (median, 4.5 years; interquartile range [IQR] 1.9–7.0 years). Their body weights ranged from 4.4 to 73.3 kg (median 20 kg; IQR 10.0–24.6 kg), and their heights ranged from 0.55 to 1.75 m (median 1.1 m; IQR 0.8–1.2 m). Their body surface areas ranged from 0.26 to 1.88 m2 (median 0.78 m2; IQR 0.5–0.9 m2).
We analyzed all the VO2 measurements recorded at 1-min intervals during 10 min with both methods. Consequently, 520 data points were obtained from 26 patients. The mean value of VO2 was 94.5 ml/min (95 % confidence interval [CI], 65.7–123.3 ml/min) measured by MS compared with 91.4 ml/min (95 % CI 64.9–117.9 ml/min) measured by BBBM.
No significant difference was found between the MS and BBBM measurements of VO2 (3.1 ml/min; 95 % CI −1.7 to +7.9 ml/min; p = 0.191). Linear regression analysis showed a high coefficient of correlation (R 2 = 0.98; p < 0.0001) between the MS and BBBM measurements of VO2 (Fig. 2). Bland–Altman plots demonstrated excellent correspondence between MS and BBBM, with a mean difference of −3.01 ml/min. The 95 % limits of agreement were −26.2 to +20.0 (Fig. 3).
Similar results were obtained if VO2 was indexed to body surface area (BSA) (Table 1). The mean difference between the indexed VO2 was 3.4 ml/min m2 (95 % CI −1.4 to 8.2 ml/min m2; p = 0.16). Figure 3 demonstrates the linear regression of indexed VO2 values obtained with the two methods. The mean difference and limits of agreement of indexed VO2 demonstrated by Bland–Altman analysis were −3.84 ml/min m2 (range −19.85 to 26.70 ml/min m2) (Figs. 4, 5).
Discussion
The main finding of our study was that the two methods (MS and BBBM) for measuring VO2 in anesthetized ventilated children (with BSAs ranging from 0.26 to 1.88 m2) showed good agreement. The two methods measured VO2 by analyzing the difference in oxygen concentration between inspired and expired gas.
Accurate measurement of the cardiac output and the pulmonary blood flow in patients with congenital heart disease requires precise measurement of VO2 for meaningful results to be obtained from the Fick equation. Numerous studies have demonstrated the discordance between assumed and measured VO2 [1, 11, 14]. However, the practice of using assumed VO2 persists in part due to the difficulty and expense of direct measurement in the real-life clinical setting.
We have demonstrated that BBBM using the Innocor™ yields results for VO2 that have good agreement with MS. However, BBBM (Innocor™) is simpler to use and less expensive than MS. MS incurs reduced maintenance costs and is readily available. But the AMIS 2000 device for MS currently is not available for purchase from the manufacturer. Our study suggests that BBBM using the Innocor™ is a useful alternative for intubated children.
Mass spectroscopy using the AMIS 2000 device yields results that correlate and agree well with thermodilution [7]. This method has been used extensively to measure VO2 in ventilated children [5, 8, 14]. Cardiac output often is measured by thermodilution rather than by use of the Fick equation in patients without systemic to pulmonary shunt lesions, partly because of the difficulty measuring VO2. General good agreement exists in cardiac output measurement between Fick and thermodilution [6]. Although the data are conflicting, thermodilution is thought to be inaccurate if the cardiac output is low or if there is tricuspid or pulmonary valve regurgitation [3, 7, 10].
The aforementioned limitations may make use of BBBM together with Fick’s equation particularly appealing during cardiac catheterization of patients with pulmonary hypertension or after repair of congenital heart disease in patients with right ventricle-to-pulmonary artery conduits, who often have varying degrees or tricuspid and pulmonary insufficiency. Moreover, mechanical ventilation may affect the accuracy of thermodilution measurements of cardiac output [10]. This is particularly germane to pediatric practice because anesthesia with mechanical ventilation often is used to facilitate cardiac catheterization, especially for those undergoing interventional procedures.
The Innocor™ is smaller and lighter than the AMIS 2000 used for MS and takes up considerably less space, which is of importance in the cramped quarters of many cardiac catheterization laboratories, with the Innocor™ less likely to impinge on the anesthetic platform. Another disadvantage of MS is the noise from the pump, which works best if running continuously and may be distracting.
However, use of BBBM and the Innocor™ device has certain potential drawbacks. Both the flow meter and sampling tube are sensitive to moisture, which limits their accuracy over long continuous periods. Use of a heated flow meter or intermittent rather than continuous measurements of VO2 may mitigate this disadvantage.
Functional residual capacity (FRC) varies from one breath to the next. The BBBM assumes a constant end-tidal oxygen concentration from breath to breath. Thus, the accuracy of VO2 measured by BBBM could be less reliable at a higher fraction of inspired oxygen concentration (FiO2). All methods for measuring VO2 become less reliable as the FiO2 is increased above 0.4–0.6, so neither of the two methods offers an advantage over the other for children receiving high concentrations of inspired oxygen. We did not study children weighing less than 4 kg, and further measurements of VO2 in smaller children and infants are required. In contrast, MS has proved to be reliable for children weighing less than 4 kg [5].
In conclusion, this study demonstrated that VO2 can be measured accurately in children undergoing cardiac catheterization by BBBM using the Innocor™. These measurements are repeatable and have excellent agreement with respiratory MS using the AMIS 2000 device. We suggest that BBBM may be a useful alternative to MS for the routine measurement of VO2 in mechanically ventilated children undergoing cardiac catheterization.
Abbreviations
- BBBM:
-
Breath-by-breath method (InnocorTM)
- CI:
-
Confidence interval
- FiO2 :
-
Fraction of inspired oxygen concentration
- IQR:
-
Interquartile range
- MS:
-
Respiratory mass spectroscopy
- SPSS:
-
Statistical package for the social sciences
- VO2 :
-
Oxygen consumption
- ml:
-
Milliliters
References
Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1:307–310
Carter J, Jeukendrup AE (2002) Validity and reliability of three commercially available breath-by-breath respiratory systems. Eur J Appl Physiol 86:435–441
Cigarroa RG, Lange RA, Williams RH et al (1989) Underestimation of cardiac output by thermodilution in patients with tricuspid regurgitation. Am J Med 86:417–420
Davies NJ, Denison DM (1979) The measurement of metabolic gas exchange and minute volume by mass spectrometry alone. Respir Physiol 36:261–267
Hammarlund K (1984) Measurement of oxygen consumption in preterm infants: assessment of a method using a mass spectrometer. Clin Physiol 4:519–531
Hillis LD, Firth BG, Winniford MD (1985) Analysis of factors affecting the variability of Fick versus indicator dilution measurements of cardiac output. Am J Cardiol 56:764–768
Hoeper MM, Maier R, Tongers J et al (1999) Determination of cardiac output by the Fick method, thermodilution, and acetylene rebreathing in pulmonary hypertension. Am J Respir Crit Care Med 160:535–541
Li J, Bush A, Schulze-Neick I et al (2003) Measured versus estimated oxygen consumption in ventilated patients with congenital heart disease: the validity of predictive equations. Crit Care Med 31:1235–1240
Lundell BP, Casas ML, Wallgren CG (1996) Oxygen consumption in infants and children during heart catheterization. Pediatr Cardiol 17:207–213
Nishikawa T, Dohi S (1993) Errors in the measurement of cardiac output by thermodilution. Can J Anaesth 40:142–153
Reybrouck T, Deroost F, Van der Hauwaert LG (1992) Evaluation of breath-by-breath measurement of respiratory gas exchange in pediatric exercise testing. Chest 102:147–152
Schmitz A, Kretschmar O, Knirsch W et al (2008) Comparison of calculated with measured oxygen consumption in children undergoing cardiac catheterization. Pediatr Cardiol 29:1054–1058
Shekerdemian L, Shore D, Lincoln C et al (1996) Negative-pressure ventilation improves cardiac output after right heart surgery. Circulation 94:II-49–II-55
Sodal IE (1989) The medical mass spectrometer. Biomed Instrum Technol 23:469–476
Acknowledgments
Funding for this study was provided by a Grant from the Women and Children’s Health Research Institute, Edmonton, Alberta.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Guo, L., Cui, Y., Pharis, S. et al. Measurement of Oxygen Consumption in Children Undergoing Cardiac Catheterization: Comparison Between Mass Spectrometry and the Breath-by-Breath Method. Pediatr Cardiol 35, 798–802 (2014). https://doi.org/10.1007/s00246-013-0855-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-013-0855-5