Abstract
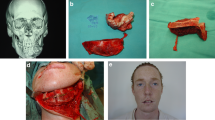
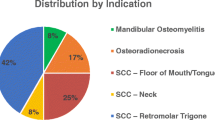
The objective of this investigation was to evaluate the indications for and the functional and cosmetic results of mandible reconstruction using free vascularized fibular flaps. It was also designed to assess the patients’ quality of life, daily activities, and self-esteem, with special emphasis on patient satisfaction. We conducted a retrospective chart review of all patients who underwent osseus or osteocutaneous free flap reconstruction of the mandible over a 10-year period (1992–2002). Those in whom a vascularized fibular flap was used were included in the study and invited for a follow-up comprehensive physical examination and x-ray evaluation. A questionnaire was also administered to evaluate patient satisfaction. Twenty-six patients were included in the study. Fourteen patients died after an average of 2 years and 9 months postoperatively due to their prognosis despite surgical intervention and adjuvant therapy. Of the remaining 12 patients, 6 appeared for the follow-up evaluation, 2 were unavailable for follow-up, and 4 denied participating. Of these 6 patients, all experienced a decrease in pain and were satisfied with their results. At the time of the latest follow-up, they experienced some difficulties swallowing, and in 3 patients, their articulation was impaired. All 6 patients would undergo the procedure again. Reconstruction of the mandible using a vascularized fibular graft produces satisfactory functional and cosmetic results. In benign lesions, the procedure is highly indicated. However, in the case of malignancy, most patients do not survive their primary tumor. Given the patients limited life expectancy, the improvement in their quality of life as a result of the improved appearance and function of the reconstructed mandible needs to be weighed against the potential morbidity of the operative intervention on an individual basis.



Similar content being viewed by others

References
Chen ZW, Yan W (1983) The study and clinical application of the osteocutaneous flap of fibula. Microsurgery 4:11–16
Cordeiro P, Disa J, Hidalgo D, Hu QY (1999) Reconstruction of the mandible with osseous free flaps: a 10-year experience with 150 consecutive patients. Plast Reconstr Surg 104:1314–1320
De Fries HO (1971) Reconstruction of the mandible: use of combined homologous mandible and autologous bone. Arch Otolaryngol 93:426–432
Guerra MM, Gias LNRodriguez Campo FJ, Diaz Gonzalez FJ (2001) Vascularized free fibular flap for mandibular reconstruction: a report of 26 cases. J Oral Maxillofac Surg 59:140–144
Hellem S, Olofsson J (1988) Titanium-coated hollow screw and reconstruction plate system (THORP) in mandibular reconstruction. J Craniomaxillofac Surg 16:173–183
Hidalgo DA (1989) Fibula free flap: a new method of mandible reconstruction. Plast Reconstr Surg 84:71–79
Holmes RE, Hagler HK (1987) Porous hydroxylapatite as a bone graft substitute in mandibular contour augmentation: a histometric study. J Oral Maxillofac Surg 45:421–429
Klotch DW, Billger JR (1985) Plate fixation for open mandibular fractures. Laryngoscope 95:1374–1377
Klotch DW, Prein J (1987) Mandibular reconstruction using AO plates. Am J Surg 154:384–388
McCullough DW, Fredrickson JM (1972) Composite neovascularized rib grafts for mandibular reconstruction. Surg Forum 23:492–494
Moscoso JF, Keller J, Genden E, Weinberg H, Biller HF, Buchbinder D, Urken MF (1994) Vascularized bone flaps in oromandibular reconstruction. A comparative anatomic study of bone stock from various donor sites to assess suitability for endosseous dental implants. Arch Otolaryngol Head Neck Surg 120:36–43
Nagamine T, Yakata H, Nakajima T (1987) Secondary reconstruction of the mandible with an aluminum oxide prosthesis. J Oral Maxillofac Surg 45:173–176
Ostrup LT, Fredrickson JM (1975) Reconstruction of mandibular defects after radiation, using a free, living bone graft transferred by microvascular anastomose. An experimental study. Plast Reconstr Surg 55:563–572
Peled M, El-Naaj IA, Lipin Y, Ardekian L (2005) The use of free fibular flap for functional mandibular reconstruction. J Oral Maxillofac Surg 63:220–224
Robertson GA (1986) A comparison between sternum and rib in osteomyocutaneous reconstruction of major mandibular defects. Ann Plast Surg 17:421–433
Serafin D, Villareal RA, Georgiade NG (1977) Rib-containing free flap to reconstruct mandibular defects. Br J Plast Surg 30:263–266
Shindo M et al. (2000)The fibula osteocutaneous flap in head and neck reconstruction: a critical evaluation of donor site morbidity. Arch Otolaryngol Head Neck Surg 126:1467–1472
Soutar DS, Scheker LR, Tanner NSB, McGregor IA (1983) The radial forearm flap: a versatile method for intraoral reconstruction. Br J Plast Surg 36:1–8
Takushima A, Harii K, Asato H, Momosawa A, Okazaki M, Nakatsuka T (2005) Choice of osseous and osteocutaneous flaps for mandibular reconstruction. Int J Clin Oncol 10:234–242
Taylor GI, Miller GD, Ham FJ (1975) The free vascularized bone graft. A clinical extension of microvascular techniques. Plast Reconstr Surg 55:533–544
Urken ML et al. (1998) Oromandibular reconstruction using microvascular composite flaps: report of 210 cases. Arch Otolaryngol Head Neck Surg 124:46–55
Vuillemin T, Raveh J, Sutter T (1988) Mandibular reconstruction with the titanium hollow screw reconstruction plate (THORP) system: evaluation of 62 cases. Plast Reconstr Surg 82(5):804–814
Wei FC, Chen HC, Chuang CC, Noordhoff FC (1986) Fibular osteoseptocutaneous flap: anatomic study and clinical application. Plast Reconstr Surg 78:191–200
Yoshimura M, Shimamura K, Iwai Y, Yamauchi S, Ueno T (1983) Free vascularized fibular transplant. A new method for monitoring circulation of the grafted fibula. J Bone Joint Surg Am 65:1295–1301
Author information
Authors and Affiliations
Corresponding author
Additional information
An erratum to this article can be found at http://dx.doi.org/10.1007/s00238-006-0105-7
Rights and permissions
About this article
Cite this article
Wedler, V., Farshad, M., Sen, M. et al. Retrospective analysis and clinical evaluation of mandible reconstruction with free fibula flap. Eur J Plast Surg 29, 285–291 (2007). https://doi.org/10.1007/s00238-006-0081-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00238-006-0081-y