Abstract
Purpose
Intracranial hypertension (IH) frequently complicates cerebral venous thrombosis (CVT). Distinct neuroimaging findings are associated with IH, yet their discriminative power, reversibility and factors favoring normalization in prospective CVT patients are unknown. We determined test performance measures of neuroimaging signs in acute CVT patients, their longitudinal change under anticoagulation, association with IH at baseline and with recanalization at follow-up.
Methods
We included 26 consecutive acute CVT patients and 26 healthy controls. Patients were classified as having IH based on CSF pressure > 25 cmH2O and/or papilledema on ophthalmological examination or ocular MRI. We assessed optic nerve sheath diameter (ONSD), optic nerve tortuousity, bulbar flattening, lateral and IVth ventricle size, pituitary configuration at baseline and follow-up, and their association with IH and venous recanalization.
Results
46% of CVT patients had IH. ONSD enlargement > 5.8 mm, optic nerve tortuousity and pituitary grade ≥ III had highest sensitivity, ocular bulb flattening and pituitary grade ≥ III highest specificity for IH. Only ONSD reliably discriminated IH at baseline. Recanalization was significantly associated with regressive ONSD and pituitary grade. Other neuroimaging signs tended to regress with recanalization. After treatment, 184.9 ± 44.7 days after diagnosis, bulbar flattening resolved, whereas compared with controls ONSD enlargement (p < 0.001) and partially empty sella (p = 0.017), among other indicators, persisted.
Conclusion
ONSD and pituitary grading have a high diagnostic value in diagnosing and monitoring CVT-associated IH. Given their limited sensitivity during early CVT and potentially persistent alterations following IH, neuroimaging indicators can neither replace CSF pressure measurement in diagnosing IH, nor determine the duration of anticoagulation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Intracranial hypertension (IH) frequently complicates cerebral venous thrombosis (CVT). It occurrs early in around 40% [1,2,3] and as a long-term complication in about 10% of patients [4]. IH is associated with visual loss [5], long-term morbidity and mortality [6]. Even in regressive thrombosis delayed IH may occur [3, 5, 7]. Obvious reasons for elevated intracranial pressure comprise space occupying hemorrhage, edema, or venous infarction. Risk factors for IH in patients without intracranial mass lesions include thrombosis of dominant and bilateral transverse sinus [3, 8, 9], superficial venous thrombosis [3, 10], and collateralization connecting dural sinus with deep intracranial veins [11].
IH, both symptomatic and subclinical, threatens vision and the extent of visual impairment is associated with cerebrospinal fluid (CSF) pressure [5]. Diagnosing CVT-related IH requires invasive CSF pressure measurement [12]. Yet, anticoagulation must be paused to perform a spinal tap, potentially causing recurrent and progressive thrombosis. Papilledema is a useful 95–100% specific surrogate for IH [13, 14], applicable for non-invasive screening. But even without papilledema CVT frequently causes retinal damage [15].
In addition to elevated CSF pressure and papilledema, several MR imaging signs are associated with IH (see Fig. 1, supplementary Figs. 1–4). Ocular signs include increased optic nerve sheath diameter (ONSD), optic disc protrusion, posterior scleral flattening, and vertical optic nerve tortuosity. Parenchymal signs include cerebral ventricle size changes and decreased pituitary height [14, 16,17,18]. Most are assessable using standard MRI sequences or by easily implementable non-routine sequences, such as ONSD, which is also readily examinable using bedside transbulbar sonography [19]. A strong association of these neuroimaging findings with IH was retrospectively determined in selected CVT cohorts with elevated CSF pressure [14, 16].
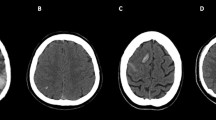
Reduction of the optic nerve sheath diameter between baseline (upper row) and follow-up (lower row) of patient P7, who presented with intracranial hypertension at diagnosis. The yellow bars in the upper central axial image show the position of 2D cross-sections 3 mm behind the optic nerve head, transsecting the right and left optic nerve perpendicular to its longitudinal orientation. The adjacent coronal images depict the cerebro-spinal fluid around the optic nerve in its sheath within the orbit, abating between baseline and follow-up imaging after 6 months. Also note the optic nerve tortuousity (upper and lower axial images)
The discriminative power of these neuromaging findings, yet, has not been established in prospective, unselected acute CVT patients. In addition, we have little information about the reversibility of neuroimaging signs during treatment and factors favoring their regression. Thus, IH neuroimaging indicators persisting after CVT may cause uncertainty regarding the duration of oral anticoagulation and the necessity of invasive diagnostics, such as lumbar puncture (LP).
We assessed test performance measures (sensitivity, specificity, positive and negative predictive values) of IH-associated neuroimaging surrogates during acute CVT. We compared patients with IH versus patients without IH to controls. IH was defined by a compound classifier consisting of CSF pressure > 25 cmH2O [12], papilledema on ophthalmological examination and/or optic disc protrusion on MRI [3]. In addition, we analyzed the reversibility of neuroimaging findings under anticoagulation, their association with IH at baseline and with venous recanalization at follow-up.
Methods
Cohort
Between January 2012 and December 2017, we prospectively registered 70 patients presenting with acute CVT to our institution. Inclusion criteria were age > 18 years and CVT diagnosed by neuroimaging (CCT and CT-Angiography or MRI and MR-Angiography). Of these, 26 patients who completed the MRI study protocol were included in the cohort (supplementary Fig. 5). 26 age- and sex-matched healthy volunteers without neurological disease underwent the study MRI to serve as controls.
General exclusion criteria were contraindications against MRI (ferro-magnetic implant, pregnancy, claustrophobia), critical illness (e.g. mechanical ventilation, severely altered consciousness), preexisting conditions causing intracranial hypertension (idiopathic intracranial hypertension, hydrocephalus) and denial to participate. We further excluded CVT patients showing space occupying hemorrhage, edema or venous infarction with midline-shift or lateral ventricle compression (see below) [3] and patients with symptoms suggestive of IH, in whom CSF pressure measurement, ophthalmological examination and/or ocular MRI were unavailable.
After diagnosing CVT, patients underwent cerebral and ocular MRI and, upon clinical suspicion of IH, CSF pressure measurement and additional ophthalmologic examination.
All 26 patients were part of a previous cross-sectional assessment of IH predictors in acute CVT [3].
Intracranial hypertension
We classified CVT patients as having intracranial hypertension based on the following predefined criteria [3]:
-
Symptoms of acute CVT (e.g. headache, seizure [20]) and
-
intracranial pressure > 25 cm H2O (according to ICHD-3 classification [12]) measured by CSF pressure in lateral decubitus position and/or
-
papilledema [13] on optical coherence tomography and/or optic disc protrusion on ocular MRI
As described before [3], we chose papilledema for its 95–100% specificity for IH [13, 14]. Given reports of unilateral papilledema in IH, we rated both uni- and bilateral optic nerve head protrusion as an indicator for IH [21]. Patients were defined as IH negative when they lacked criteria of the compound classifier.
MR-Imaging
CVT patients underwent baseline cerebral MRI at inclusion (3 Tesla MRI, Magnetom TRIO or 1.5 Tesla MRI, Magnetom Avanto, Siemens Healthcare, Erlangen, Germany) including 2D T1, 2D T2, 2D time-of-flight (TOF) venography, 3D fluid attenuated inversion recovery based on sampling perfection with application-optimized contrasts using different flip angle evolution (FLAIR SPACE), 2D susceptibility-weighted imaging (SWI), and 2D high-resolution T2-weighted half-Fourier acquisition single-shot turbo spin-echo (HASTE) sequences as previously described [19, 22, 23]. Supplementary Table 1 gives sequence details. We complemented dedicated orbital imaging and contrast-enhanced (ce-) vascular imaging at 3 T soon after CVT diagnosis, as described before [3]. Controls underwent the same MR protocol at 3 T as patients, yet without application of Gd contrast agent. CVT follow-up comprised the same MR protocol and neurological examination.
Venography
If not contraindicated, we acquired ce-T1W magnetization-prepared rapid acquisition with gradient echo (MPRAGE; supplementary Table 1) venography after acquision of the other sequences, approximately 4 min. after intravenous injection of 0.1 mmol/kg Gadoteridol (ProHance, Bracco Imaging, Milan, Italy), available in 24 patients. In two patients, we analyzed ce-CT-venography scans acquired after intravenous injection of 70 ml Iomeprol (Imeron 400, Bracco Imaging, Milan, Italy) at a flowrate of 3 ml/s, followed by 60 ml saline. CT-venography was started manually with inflow of contrast agent into the internal jugular vein using visual bolus tracking, as described before [3] using Siemens Somatom Definition AS and Definition Flash CT scanners (Siemens Healthcare, Erlangen, Germany); tube voltage 100 kV, exposure 140 mAs, collimation of 64 × 0.6 mm, helical mode, reconstruction of 0.75 mm isotropic datasets.
Blinded assessment
MRIs were rated by four experts with longstanding experience in neuroimaging analysis (blinded readers: TD and NL > 10 years, SM > 20 years in neuroradiology; FS > 10 years in cerebral MRI research) who interpreted anonymized data using standard imaging software (IMPAX EE R20 DeepUnity Diagnost, Dedalus HealthCare GmbH, Bonn, Germany). TD and SM analyzed venographies blinded to clinical characteristics, complementary morphological data and rating performed by NL and FS and vice versa.
Two Neuroophthalmologists with > 10 years (MR) and > 25 years (WL) experience in ophthalmology performed funduscopy, being unblinded to the CVT diagnosis but unaware of MRI and LP related data.
Physicians performing lumbar puncture were blinded to ophthalmologic and neuroimaging findings.
Presence of lesions
We identified CVT-associated cerebral edema in 3D FLAIR SPACE and hemorrhage using susceptibility-weighted imaging as described before [22]. In addition, on axial and coronal slices we searched for IH causes not attributable to thrombotic material, assessing any midline shift, lateral ventricle compression or dislocation of the temporal horns [3].
Thrombosis rating
TD systematically determined the location and number of thrombosed intracranial veins and sinus on all available time-of-flight (TOF) and ce-MPRAGE venographies [24] as described before [3]. One point was assigned to each thrombosed part of the following 18 predefined segments (1–18 points): rostral, mid and dorsal segments of the superior sagittal sinus (SSS), transverse and sigmoid sinus, basal veins of Rosenthal, great vein of Galen, straight sinus and cortical veins draining into the SSS including the superior and inferior collaterals of Trolard and Labbé.
Recanalization rating
TD and SM independently rated thrombus recanalization on follow-up ce-MRV as described before [3](supplementary Table 2), using the grading proposed by Aguiar de Sousa [25] and Qureshi [26]. Readers resolved disagreement by consensus. We analyzed the influence of recanalization extent (any degree, partial (i.e. Aguiar de Sousa grade ≥ 2A, see supplementary Table 3) and complete recanalization (Qureshi grade III, Aguiar de Sousa grade 3)).
Neuroimaging indicators of intracranial hypertension
NL rated the presence of optic disc protrusion [3], bulbar flattening and optic nerve tortuousity [17] depicting the bulbi and optic nerves (Fig. 1; supplementary Fig. 1), pituitary tissue was graded using 3-dimensional FLAIR SPACE [22] according to Yuh et al. (grade 1, normal appearance through grade 5, empty sella; grade 3 representing abnormal partially empty sella; supplementary Fig. 2)[16]. Lateral and fourth ventricle size (supplementary Figs. 3 and 4) was determined using standardized measurements on axial T1w images as previously described [14].
FS analyzed ONSD (Fig. 1) and frequency of enlargement > 5.8 mm [18, 19] using HASTE-sequence as described before [19, 23]. In short, we placed a circular region-of-interest marker 3 mm behind the eyeball, perpendicular to longitudinal extension of the optic nerve. ONSD was defined as the border of highest contrast of signal intensity change between CSF and the surrounding optic nerve sheath.
Statistics
Continuous data are given in mean ± standard deviation (SD). We assessed cross-sectional and longitudinal differences of continuous variables by simple and dependent t-test and categorical data by chi2 or Fishers’ test. We determined sensitivity and specificity, positive and negative predictive values (PPV, NPV) and odds ratios (OR) of neuroimaging signs. Ordinal variables were analyzed by Mann Whitney U (cross-sectional) or Wilcoxon rank sum tests (longitudinal). We determined associations of continuous, categorical and ordinal variables by Kendall’s tau.
All tests were two-sided if not stated otherwise, with an α-level of significance set at 5%. We considered missing data to occur at random and did not impute. P-values were not corrected for multiple testing and should be interpreted as hypothesis generating.
Results
Cohort
We included 26 CVT patients (21 female, 77.8%) and 26 age- and sex-matched controls. Patients’ demographics are presented in Table 1. Average time from CVT diagnosis to inclusion was 7.3 ± 8.7 days. 23 patients underwent follow-up ce-MRI after 184.9 ± 44.7 days, in the majority 5–7 months after CVT diagnosis. Later imaging was performed in three patients after 245 to 335 days. Of these, one patient (P7) was IH positive and two (P4 and P12) IH negative.
Classification of intracranial hypertension
12/26 patients (46.2%) had IH (supplementary Fig. 6). We classified 14 patients by CSF pressure measurement (11 patients had elevated (42.9 ± 10 cmH2O) and three normal CSF pressure (16.3 ± 1.5 cmH2O)). Among 9 patients undergoing neuroophthalmologic examination, we classified three patients by the lack of papilledema (6 were already classified by CSF pressure). We classified 9 out of 23 patients by ocular imaging (one showing, 8 lacking papilledema; the remaining 14 patients were already classified by CSF pressure and ophthalmologic examination).
In this cohort, no patient had unilateral papilledema. Controls did not show papilledema at repeated MRIs 26.2 ± 10.9 days apart.
Baseline imaging
Discriminative power of neuroimaging signs in CVT at baseline
For comparison with previously published retrospective data, Table 2 gives test performance metrics and odds ratios (OR) of neuroimaging findings. In patients with IH, ONSD enlargement > 5.8 mm, optic nerve tortuousity and partially empty sella (i.e. pituitary grade ≥ III) had highest sensitivity. Ocular bulb flattening, and pituitary grade ≥ III yielded highest specificity. NPV achieved at least 88.2%, whereas PPV were below 50%.
Compared with controls, all neuroimaging signs had higher OR in patients with versus without IH. Yet, OR were also elevated in patients without IH compared to controls (in decreasing order: bulbar flattening, pituitary grade ≥ III, ONSD enlargement > 5.8 mm).
Figure 2 shows the distribution of ONSD, lalteral and IVth ventricle size in CVT patients compared with controls. Among ocular findings, significantly larger ONSD discriminated patients with IH from both patients without IH and controls (see Fig. 2; ONSD in patients without IH and controls were comparable).
Boxplots show optic nerve sheath diameter (ONSD), lateral and IVth ventricle size in CVT patients at baseline, follow-up (FU) and in normal controls. Comparisons at baseline give the discriminative potential of neuroimaging findings. Longitudinal comparisons demonstrate the extent of reversibility, depending on the classifier IH and in relation to normal dimensions in controls. In conclusion, only ONSD discriminated IH in CVT patients, and differed significantly at follow-up in patients with versus without IH and healthy controls. To improve readability, we omitted p-values > 0.2 (n.s., not significant)
At baseline, none of the other ocular neuroimaging signs (ocular bulb flattening, optic nerve tortuousity) nor the parenchymal findings (lateral ventricle size, IVth ventricle size, and pituitary grade) discriminated CVT subgroups (Fig. 2, Table 2). Although at baseline IVth ventricle size was significantly wider in CVT patients without IH than in controls, IVth ventricle size in CVT patients with versus without IH were comparable. Pituitary grade discriminated controls from both patients with IH (p = 0.003) and patients without IH (p = 0.043). Yet, pituitary grade ≥ III did not discriminate between CVT subgroups (patients with versus without IH, p = 0.202; Mann–Whitney; one-sided comparisons in small sample), despite > 2.5-fold higher odds ratio in patients with IH (Table 2).
Follow-up imaging
Until follow-up, IH symptoms resolved in most patients under treatment and greatly improved in P15 and P22 (Table 1). Patient P13 developed delayed IH, despite recanalization under anticoagulation (Aguiar de Sousa Grade 2B).
Reversibility of optic disc protrusion
Optic disc protrusion at follow-up was less frequent in patients with IH compared to baseline, without reaching statistical significance (baseline, 5/10 (50%); follow-up, 1/8 (12.5%), p = 0.152). No patient without IH developed optic disc protrusion until follow-up.
Reversibility of neuroimaging changes in CVT
Patients with IH showed a significant ONSD reduction between baseline and follow-up (Fig. 3), whereas ONSD remained stable in patients without IH.
Longitudinal changes of the other neuroimaging findings including pituitary grade (patients with IH, p = 0.414; without IH, p = 0.317) did not reach significance (Fig. 3, Table 3), although bulbar flattening frequency halved in patients with IH and patients without IH showed a trend towards lower frequency.
Normalization of neuroimaging indicators of intracranial hypertension
Among ocular neuroimaging signs, ONSD size in patients with IH remained significantly larger at follow-up compared to patients without IH and controls (Fig. 2). In line, ONSD enlargement > 5.8 mm at follow-up remained significantly more frequent in patients with IH compared with controls, whereas frequency in patients without IH versus controls was comparable (Table 3). Bulbar flattening and optic nerve tortuousity were as frequent in patients with and without IH at follow-up as in controls.
Among parenchymal neuroimaging sings partially empty sella remained significantly more frequent in patients with IH compared to controls (pituitary grades, one-sided p = 0.017), contrasting comparable pituitary grades in patients without IH versus controls (one-sided p = 0.434). At follow-up, patients with IH showed non-significantly less visible pituitary tissue (i.e. higher pituitary grade) compared to patients without IH (Mann–Whitney, p = 0.091). Between-group differences of lateral ventricle size at follow-up, although larger in patients with IH than without IH, were comparable to controls (Fig. 2). Longitudinally, the IVth ventricle showed stable dimensions in patients without IH, remaining larger than in controls (p = 0.033).
Taken together, in patients with IH, both absolute ONSD size, the frequency of ONSD enlargment > 5.8 mm and pituitary aspect did not normalize until follow-up, referring to controls. In IH negative patients, only the size of the IVth ventricle (already significantly larger at baseline) remained larger at follow-up, compared to controls.
Association of neuroimaging findings ‘ reversibility with recanalization
Supplementary Table 2 shows aggregated frequencies of recanalization grades. Figure 3 shows longitudinal size differences of the individual imaging signs and supplementary Fig. 7 changes of ONSD of individual eyes by Aguiar de Sousa grade ≥ 2A (at least partial recanalization of all previously thrombosed vessel segments).
The neuroimaging findings yielding a significant correlation with at least partial recanalization of all thrombosed segments (Aguiar de Sousa grade ≥ 2A) in our cohort were ONSD size reduction (Kendall’s tau; 0.406, p = 0.01) and pituitary grade (2.2 ± 1 in those with lower versus 3.7 ± 0.5 with higher recanalization grades; Mann–Whitney, p = 0.05). In addition, longitudinal changes of ONSD and lateral ventricle size (Fig. 3) showed a non-significant correlation with different recanalization grades (supplementary Table 3). In contrast, CVT patients showing complete recanalization had comparable pituitary grade at baseline and follow-up (p = 0.317).
Further analyses regarding recanalization grade and IH did not reveal significant correlations.
Discussion
In this prospective cohort including 26 patients with acute cerebral venous thrombosis (CVT), 12 (46%) had intracranial hypertension (IH), identified by CSF pressure > 25cmH2O and/or papilledema.
At baseline, ONSD was significantly larger and enlargement > 5.8 mm more frequent in CVT patients with versus without IH. Ocular bulb flattening and partially empty sella (pituitary grade ≥ III) had highest specificity, i.e. indicating low probability of IH when absent. Of high clinical value, negative predictive values of > 85% gave unremarkable findings in CVT patients classified not having IH. ONSD enlargement > 5.8 mm, optic nerve tortuousity and pituitary grade ≥ III showed highest sensitivity, supporting the diagnosis of IH. Neuroimaging indicators achieved positive predictive values below 50%, i.e. identified less than half of the patients classified having IH.
At follow-up, 70% of patients showed at least partial recanalization of previously thrombosed vessels, including 33% achieving complete recanalization. Reduction of ONSD and pituitary grade until follow-up were significantly associated with recanalization (at least partial recanalization of all previously thrombosed vessel segments; Aguiar de Sousa grade ≥ 2A). Despite significant regression, ONSD in patients with IH did not return to dimensions observed in patients without IH and controls. At follow-up, partially empty sella remained more frequent in patients with IH compared to controls, too, although all patients except for P13 showed marked improvement or resolution of IH symtoms.
Causes of intracranial hypertension
Several often intertwined mechanisms increase the IH risk in CVT: First, the amount and localization of thrombus predispose to IH [3, 8, 9, 27]. Second, depending on collateralization, even local thrombosis may increase endovenous pressure. Third, the pressure dependend CSF resorption via glymphatic pathways is reduced by lower trans-vessel pressure e.g. when thrombosis involves Pacchioni granulations [28]. Fourth, although rare, dural arterio-venous fistula causing or complicating CVT may increase intravenous and intracranial pressure [29,30,31]. Fifth, local space occupation due to edema, infarction and hemorrhage following venous stasis may cause rise of intracranial pressure [32].
Classification of intracranial hypertension
To classify IH, we relied on elevated CSF pressure [12] and if unavailable, on papilledema on ophthalmological examination and/or optic disc protrusion on MRI. The number of positive neuroimaging findings correlates with CSF pressure [33]. In addition, the prevalence of papilledema correlates with the number of IH neuroimaging indicators, increasing from 2.8% in patients presenting at least one sign to 40% in patients with ≥ 4 IH indicators [34].
With nearly one in two patients (46%) developing IH during acute CVT, IH prevalence was comparable to previous reports [1, 2]. IH rarely developed delayed [4], affecting two patients with progressive thrombosis 6 and 38 days after CVT diagnosis.
Discriminative power
Our prospective CVT cohort appears closer to real-life in-hospital conditions than previous retrospective case–control cohorts selected by proven IH [14, 17], limiting their mutual comparability. Our results support the diagnostic value of ONSD enlargement regarding IH in acute CVT [18, 19]. In line with Dong et al. [14], pituitary grade differentiated CVT patients with IH and controls. The other neuroimaging indicators were less of avail. Although more common in patients with IH, optic nerve tortuousity had low sensitivity in identifying IH in acute CVT. Ocular bulb flattening frequency, pituitary grade, and—contrasting Dong et al. [14]—lateral and IVth ventricle size did not discriminate CVT patients with versus without IH at baseline.
Temporal course of morphological changes
Morphological changes may appear at different CVT stages and show a diverging dynamic. Given the 1–2 week latency from CVT diagnosis to inclusion in our cohort, we cannot exclude misclassification of patients who developed IH and associated morphological effects later. Despite elevated CSF pressure, five patients in our cohort did not show papilledema at inclusion. Papilledema in CVT mostly develops within one to two months [7]. The limited positive predictive value of neuroimaging findings might thus stem from the early CSF pressure measurement. In addition, the lack of papilledema in patients not undergoing CSF pressure measurement might have underestimated IH frequency.
Reversibility of neuroimaging findings in CVT
Little data is available on the usefulness of neuroimaging findings as monitoring parameters during the later CVT course, e.g. to guide the duration of anticoagulation in case of incomplete recanalization. Reversibility of neuroimaging indicators appeared heterogeneous, more frequently occurring in ocular findings in our cohort. The frequency of ONSD enlargement, bulbar flattening and pituitary grade decreased significantly, and reversibility was associated with IH classification. Yet, despite significant regredience, ONSD enlargement did not regress to baseline values in 8/8 IH patients compared to controls and patients without IH. Pituitary grade even increased in patients with IH.
As IH symptoms resolved in most patients, we estimate ongoing IH at follow-up is less probable. Patient P13 developed delayed IH despite advanced recanalization. Showing markedly improving IH symptoms but lacking follow-up LP, we cannot exclude ongoing IH causing slight residual blurred vision in P15 and intermittent tinnitus in P22.
Duration of IH, tissue elasticity and the time needed for normalization might affect the remission of IH neuroimaging signs. In idiopathic intracranial hypertension (IIH) patients showing papilledema, MRI findings suggestive of IH persisted after resolution of both symptoms and papilledema [35]. In CVT, papilledema was reversible on average after 6 months [7]. In vivo intrathecal infusion tests [36] and post mortem experiments [37] demonstrate the interrelation between ONSD enlargment and short-term CSF pressure elevation. ONSD reversiblility was incomplete after high pressure exposure [37]. In our cohort, we ascribe the persistent ONSD enlargment to prolonged IH during acute CVT.
At follow-up, partially empty sella in patients with IH remained significantly more frequent compared with controls, however not reaching significance compared with CVT patients without IH. Although IH treatment might reverse empty sella [38], pituitary compression may outlast due to structural changes of the sellar region, as in IIH [35].
Regredience of bulbar flattening frequency did not differ in patients with versus without IH, potentially due to the limited cohort size. Longitudinal changes of inner CSF spaces and IH at baseline were not significantly associated in our cohort. In line, the size of inner CSF spaces neither predicted IH nor differed before versus one month after treatment of CVT [39].
Association of reversibility of neuroimaging findings with recanalization
In the range of previous reports [40], depending on the grading used, 33% (Aguiar de Sousa) to 70% (Qureshi) showed complete and > 70% at least partial recanalization of all initially affected vessels. Several neuroimaging findings were non-significantly associated with partial recanalization of all previously thrombosed vessel segments (Aguiar de Sousa grade ≥ 2A). There was no correlation with presence or absence of complete recanalization alone.
Incomplete recanalization might predispose to longstanding IH, occurring in 10% after CVT [4]. In contrast, recanalization is associated with both normalization of hemodynamics, cerebral metabolism and positive outcome [25, 40,41,42,43]. Given variable collateralization networks, both the extent of recanalization necessary to prevent IH and the degree of venous flow restoration necessary for regredience of imaging alterations in CVT remain unclear.
Strengths and limitations
Strengths of our study include the prospective CVT cohort, reflecting real-life in-hospital conditions, which we analyzed by dedicated, systematic rating of thrombosis and recanalization. We internally validated test performance measures of neuroimaging signs by comparing IH subgroups versus their separate matched controls. Our results offer an orientation regarding the evolution of neuroimaging findings after CVT.
Our study is limited by its size and monocentric design, and also by exclusion of patients lacking both CSF pressure measurement and ophthalmologic examination or ocular MRI. Second, our cohort possibly overrepresents patients with visual symptoms and, excluding critically ill patients, our results might not apply to severe CVT. Third, for ethical reasons, we renounced follow-up CSF pressure measurement to confirm IH reversibility. We think this is negligible as IH symptoms resoved in all patients. Only one patient (P9) showed asymptomatic optic disc protrusion on follow-up MRI. Our results need replication, ideally in a larger prospective cohort.
Clinical consequences
The suspicion of CVT indicates emergent brain imaging work-up. Complementing ce-MR-venography, IH neuroimaging sings offer high specificity classifying IH. Unfortunately, the temporal course of IH and neuroimaging findings in CVT are highly variable and symptoms may precede morphological effects of IH. This carries the risk of misclassification and explains the limited positive predictive value of IH neuroimaging indicators. Thus, neuroimaging surrogates may support estimating the IH risk in CVT but appear insufficient to replace CSF pressure measurement.
Pausing anticoagulation for spinal tap carries the risk of progressive thrombosis. This requires evaluating the clinical presentation in synopsis with IH risk factors, e.g. thrombus location, extension and collateralization [3, 9, 11, 27]. Consequently, individual IH pretest probability should guide the decision to perform LP. Longitudinal ONSD assessment may be a helpful alternative, given the ease of sonographic bedside assessment.
Further, IH neuroimaging findings persisting after CVT or appearing delayed in asymptomatic patients may cause uncertainty regarding the need and duration of anticoagulation, clinical follow-up frequency and invasive CSF pressure measurement. In asymptomatic CVT patients, persisting IH indicators should promote non-invasive diagnostic steps before-hand, such as ophthalmological examination (e.g. optical coherence tomography, fundoscopy, ONSD sonography) [7, 13, 15]. In patients with a sustained suspicion of IH, we suggest determining CSF pressure to guide further therapy, e.g. continued anticoagulation or acetazolamide [44].
The optimal duration of anticoagulation is currently elusive [44] as 3/4 of patients recanalized within 3 months [40], but recanalization may occur as late as 800 days after CVT [42]. Therefore, patients showing incomplete recanalization need individualized counseling regarding anticoagulation duration, weighing the chances of further recanalization versus bleeding risk.
Conclusion
Intracranial hypertension complicates acute CVT in nearly every second patient and may develop with delay. Therefore, the appearance of clinical signs or neuroimaging findings of IH and their reversibility warrant further investigation. In patients with acute CVT, neuroimaging features with high sensitivity for IH were ONSD enlargement, optic nerve tortuousity, and pituitary grade ≥ III (“partially empty sella”), supporting the diagnosis of IH. Lack of ocular bulb flattening and pituitary grade ≥ III had high specificity, indicating low IH probability. Finally, ONSD enlargement discriminated presence of IH.
Non-invasive ONSD measurement might guide the clinician in diagnosing and following up on CVT-related IH. In our study, ONSD and pituitary grade improved significantly, yet, did not reach dimensions observed in controls.
Taken together, neuroimagig indicators in synopsis with clinical presentation and IH risk factors should guide clinical reasoning and diagnostic procedures in CVT.
Data Availability
The data that support the findings of this study are available from the corresponding author on reasonable request.
References
Saposnik G, Barinagarrementeria F, Brown RD et al (2011) Diagnosis and management of cerebral venous thrombosis: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 42:1158–1192. https://doi.org/10.1161/STR.0b013e31820a8364
Duman T, Uluduz D, Midi I et al (2017) A multicenter study of 1144 patients with cerebral venous thrombosis: the VENOST study. J Stroke Cerebrovasc Dis 26:1848–1857. https://doi.org/10.1016/j.jstrokecerebrovasdis.2017.04.020
Schuchardt F, Demerath T, Lützen N et al (2022) Risk factors for the development of secondary intracranial hypertension in acute cerebral venous thrombosis. Neuroradiology. https://doi.org/10.1007/s00234-022-03091-9
Geisbüsch C, Herweh C, Gumbinger C et al (2021) Chronic intracranial hypertension after cerebral venous and sinus thrombosis – frequency and risk factors. Neurol Res Pract 3:28. https://doi.org/10.1186/s42466-021-00127-y
Ding J, Zhou D, Geng T et al (2018) To predict visual deterioration according to the degree of intracranial hypertension in patients with cerebral venous sinus thrombosis. Eur Neurol 80:28–33. https://doi.org/10.1159/000492184
Ferro JM, Canhao P, Stam J et al (2009) Delay in the diagnosis of cerebral vein and dural sinus thrombosis: influence on outcome. Stroke 40:3133–3138. https://doi.org/10.1161/STROKEAHA.109.553891
Liu KC, Bhatti MT, Chen JJ et al (2020) Presentation and progression of papilledema in cerebral venous sinus thrombosis. Am J Ophthalmol 213:1–8. https://doi.org/10.1016/j.ajo.2019.12.022
Glik A, Benkovich E, Kesler A et al (2016) Lateral sinus thrombosis: the importance of the unaffected sinus: the unaffected sinus in lateral sinus thrombosis. J Neuroimaging 26:599–604. https://doi.org/10.1111/jon.12336
Farias-Moeller R, Avery R, Diab Y et al (2016) Contralateral hypoplastic venous draining sinuses are associated with elevated intracranial pressure in unilateral cerebral sinovenous thrombosis. AJNR Am J Neuroradiol 37:2392–2395. https://doi.org/10.3174/ajnr.A4899
Kalita J, Singh VK, Jain N et al (2019) Cerebral venous sinus thrombosis score and its correlation with clinical and MRI findings. J Stroke Cerebrovasc Dis 28:104324. https://doi.org/10.1016/j.jstrokecerebrovasdis.2019.104324
Barboza MA, Mejias C, Colin-Luna J et al (2015) Intracranial venous collaterals in cerebral venous thrombosis: clinical and imaging impact. J Neurol Neurosurg Psychiatry 86:1314–1318. https://doi.org/10.1136/jnnp-2014-309717
(2018) Headache classification committee of the International Headache Society (IHS) the international classification of headache disorders, 3rd edition. Cephalalgia 38:1–211. https://doi.org/10.1177/0333102417738202
Sallam A, Abdelaal Ahmed Mahmoud M. Alkhatip A, Kamel MG et al (2021) The diagnostic accuracy of noninvasive methods to measure the intracranial pressure: a systematic review and meta-analysis. Anesth Analg 132:686–695. https://doi.org/10.1213/ANE.0000000000005189
Dong C, Zheng Y, Li X et al (2016) Morphometric MRI changes in intracranial hypertension due to cerebral venous thrombosis: a retrospective imaging study. Clin Radiol 71:691–697. https://doi.org/10.1016/j.crad.2016.04.011
Koban Y, Ozlece H, Karayol S, Huseyinoglu N (2019) Decreased retinal nerve fiber layer thickness in patients with cerebral venous thrombosis. BMC Ophthalmol 19:57. https://doi.org/10.1186/s12886-019-1046-9
Yuh WT, Zhu M, Taoka T et al (2000) MR imaging of pituitary morphology in idiopathic intracranial hypertension. J Magn Reson Imaging 12:808–813
Ridha MA, Saindane AM, Bruce BB et al (2013) Magnetic resonance imaging findings of elevated intracranial pressure in cerebral venous thrombosis versus idiopathic intracranial hypertension with transverse sinus stenosis. Neuro-Ophthalmol 37:1–6. https://doi.org/10.3109/01658107.2012.738759
Geeraerts T, Newcombe VF, Coles JP et al (2008) Use of T2-weighted magnetic resonance imaging of the optic nerve sheath to detect raised intracranial pressure. Crit Care 12:R114. https://doi.org/10.1186/cc7006
Bäuerle J, Schuchardt F, Schroeder L et al (2013) Reproducibility and accuracy of optic nerve sheath diameter assessment using ultrasound compared to magnetic resonance imaging. BMC Neurol 13. https://doi.org/10.1186/1471-2377-13-187
Ferro JM, Aguiar de Sousa D (2019) Cerebral venous thrombosis: an update. Curr Neurol Neurosci Rep 19:74. https://doi.org/10.1007/s11910-019-0988-x
Banerjee M, Aalok SP, Vibha D (2020) Unilateral papilledema in idiopathic intracranial hypertension: a rare entity. Eur J Ophthalmol:1120672120969041. https://doi.org/10.1177/1120672120969041
Schuchardt F, Hennemuth A, Schroeder L et al (2017) Acute cerebral venous thrombosis: three-dimensional visualization and quantification of hemodynamic alterations using 4-dimensional flow magnetic resonance imaging. Stroke 48:671–677. https://doi.org/10.1161/STROKEAHA.116.015102
Weigel M, Lagreze WA, Lazzaro A et al (2006) Fast and quantitative high-resolution magnetic resonance imaging of the optic nerve at 3.0 tesla. Invest Radiol 41:83–86
Sadigh G, Mullins ME, Saindane AM (2016) Diagnostic performance of mri sequences for evaluation of dural venous sinus thrombosis. AJR Am J Roentgenol 206:1298–1306. https://doi.org/10.2214/AJR.15.15719
Aguiar de Sousa D, Lucas Neto L, Arauz A et al (2020) Early recanalization in patients with cerebral venous thrombosis treated with anticoagulation. Stroke 51:1174–1181. https://doi.org/10.1161/STROKEAHA.119.028532
Qureshi AI (2010) A classification scheme for assessing recanalization and collateral formation following cerebral venous thrombosis. J Vasc Interv Neurol 3:1–2
Aguiar de Sousa D, Lucas Neto L, Jung S et al (2019) Brush sign is associated with increased severity in cerebral venous thrombosis. Stroke 50:1574–1577. https://doi.org/10.1161/STROKEAHA.119.025342
McKnight CD, Rouleau RM, Donahue MJ, Claassen DO (2020) The regulation of cerebral spinal fluid flow and its relevance to the glymphatic system. Curr Neurol Neurosci Rep 20:58. https://doi.org/10.1007/s11910-020-01077-9
Cognard C, Casasco A, Toevi M et al (1998) Dural arteriovenous fistulas as a cause of intracranial hypertension due to impairment of cranial venous outflow. J Neurol Neurosurg Psychiatry 65:308–316. https://doi.org/10.1136/jnnp.65.3.308
Schuchardt FF, Demerath T, Elsheikh S et al (2021) Dural arteriovenous fistula formation secondary to cerebral venous thrombosis: longitudinal magnetic resonance imaging assessment using 4D-Combo-MR-Venography. Thromb Haemost:s-0041–1723991. https://doi.org/10.1055/s-0041-1723991
Lindgren E, Rentzos A, Hiltunen S et al (2022) Dural arteriovenous fistulas in cerebral venous thrombosis: data from the International Cerebral Venous Thrombosis Consortium: data from the International Cerebral Venous Thrombosis Consortium. Eur J Neurol 29:761–770. https://doi.org/10.1111/ene.15192
Coutinho JM, van den Berg R, Zuurbier SM et al (2014) Small juxtacortical hemorrhages in cerebral venous thrombosis: JCHs in cerebral thrombosis. Ann Neurol 75:908–916. https://doi.org/10.1002/ana.24180
Rohr AC, Riedel C, Fruehauf M-C et al (2011) MR imaging findings in patients with secondary intracranial hypertension. Am J Neuroradiol 32:1021–1029. https://doi.org/10.3174/ajnr.A2463
Chen BS, Meyer BI, Saindane AM et al (2021) Prevalence of incidentally detected signs of intracranial hypertension on magnetic resonance imaging and their association with papilledema. JAMA Neurol 78:718. https://doi.org/10.1001/jamaneurol.2021.0710
Chang RO, Marshall BK, Yahyavi N et al (2016) Neuroimaging features of idiopathic intracranial hypertension persist after resolution of papilloedema. Neuroophthalmology 40:165–170. https://doi.org/10.1080/01658107.2016.1179767
Hansen H-C, Helmke K (1997) Validation of the optic nerve sheath response to changing cerebrospinal fluid pressure: ultrasound findings during intrathecal infusion tests. J Neurosurg 87:34–40. https://doi.org/10.3171/jns.1997.87.1.0034
Hansen H-C, Lagrèze W, Krueger O, Helmke K (2011) Dependence of the optic nerve sheath diameter on acutely applied subarachnoidal pressure - an experimental ultrasound study. Acta Ophthalmol 89:e528-532. https://doi.org/10.1111/j.1755-3768.2011.02159.x
Zagardo MT, Cail WS, Kelman SE, Rothman MI (1996) Reversible empty sella in idiopathic intracranial hypertension: an indicator of successful therapy? AJNR Am J Neuroradiol 17:1953–1956
Zheng Y, Chen J, Yuan M et al (2019) Does a change in ventricular size predict a diagnosis of cerebral venous thrombosis-related acute intracranial hypertension? Results of a retrospective imaging study. Acta Radiol 60:1308–1313. https://doi.org/10.1177/0284185118823346
Aguiar de Sousa D, Lucas Neto L, Canhão P, Ferro JM (2018) Recanalization in cerebral venous thrombosis: a systematic review and meta-analysis. Stroke 49:1828–1835. https://doi.org/10.1161/STROKEAHA.118.022129
Kawai N, Shindou A, Masada T et al (2005) Hemodynamic and metabolic changes in a patient with cerebral venous sinus thrombosis: evaluation using O-15 positron emission tomography. Clin Nucl Med 30:391–394
Stolz E, Gerriets T, Bödeker RH et al (2002) Intracranial venous hemodynamics is a factor related to a favorable outcome in cerebral venous thrombosis. Stroke 33:1645–1650
Rezoagli E, Martinelli I, Poli D et al (2018) The effect of recanalization on long-term neurological outcome after cerebral venous thrombosis. J Thromb Haemost. https://doi.org/10.1111/jth.13954
Ferro JM, Bousser M-G, Canhão P et al (2017) European Stroke Organization guideline for the diagnosis and treatment of cerebral venous thrombosis - endorsed by the European Academy of Neurology. Eur J Neurol 24:1203–1213. https://doi.org/10.1111/ene.13381
Acknowledgements
We thank D. Hazard, Institute of Medical Biometry and Statistics, Faculty of Medicine, Medical Center-University of Freiburg, for statistical advice.
Funding
Open Access funding enabled and organized by Projekt DEAL. None related to the submitted work.
FS: previous work on dural arterio-venous fistula in cerebral venous thrombosis was partially supported by Forschungskommission, Medical Faculty, Albert-Ludwigs-University, Freiburg (SCHU 1097/16); Grant 01VSF19053 by the Innovations Committee of the Federal Joint Committee (gemeinsamer Bundesausschuss, gBA).
MW: received funding from Biogen for developing spinal cord MRI.
SM: received grants from the federal Ministry of Education and Research, receives consulting fees from Acandis, Balt, Medtronic and Novartis (member of study imaging core lab), honoraria for lectures fromBalt, Medtronic, and Stryker.
HU: receives honoraria for lectures from Biogen, Eisai, Lilly, Mbits.
CW: receives funding from the Deutsche Forschungsgemeinschaft.
AH: receives funding from Berta-Ottenstein programme for Advanced Clinician Scientists, Medical Faculty, University of Freiburg, Germany and from Deutsche Forschungsgemeinschaft grant HA 5399/6–1.
TD: received travel grants from Balt, Stryker.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
HU is on the board of directors of Neuroradiology.
The other authors do not report financial or non-financial conflicts of interest related to the submitted work.
Ethics
The study protocol was approved by our institutional ethics committee (protocol number 306/10) and all participants gave written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Schuchardt, F.F., Lützen, N., Küchlin, S. et al. Clinical value of neuroimaging indicators of intracranial hypertension in patients with cerebral venous thrombosis. Neuroradiology (2024). https://doi.org/10.1007/s00234-024-03363-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00234-024-03363-6